
The Research Gap (Literature Gap)
Everything you need to know to find a quality research gap
By: Ethar Al-Saraf (PhD) | Expert Reviewed By: Eunice Rautenbach (DTech) | November 2022
If you’re just starting out in research, chances are you’ve heard about the elusive research gap (also called a literature gap). In this post, we’ll explore the tricky topic of research gaps. We’ll explain what a research gap is, look at the four most common types of research gaps, and unpack how you can go about finding a suitable research gap for your dissertation, thesis or research project.
Overview: Research Gap 101
- What is a research gap
- Four common types of research gaps
- Practical examples
- How to find research gaps
- Recap & key takeaways
What (exactly) is a research gap?
Well, at the simplest level, a research gap is essentially an unanswered question or unresolved problem in a field, which reflects a lack of existing research in that space. Alternatively, a research gap can also exist when there’s already a fair deal of existing research, but where the findings of the studies pull in different directions , making it difficult to draw firm conclusions.
For example, let’s say your research aims to identify the cause (or causes) of a particular disease. Upon reviewing the literature, you may find that there’s a body of research that points toward cigarette smoking as a key factor – but at the same time, a large body of research that finds no link between smoking and the disease. In that case, you may have something of a research gap that warrants further investigation.
Now that we’ve defined what a research gap is – an unanswered question or unresolved problem – let’s look at a few different types of research gaps.

Types of research gaps
While there are many different types of research gaps, the four most common ones we encounter when helping students at Grad Coach are as follows:
- The classic literature gap
- The disagreement gap
- The contextual gap, and
- The methodological gap
Need a helping hand?
1. The Classic Literature Gap
First up is the classic literature gap. This type of research gap emerges when there’s a new concept or phenomenon that hasn’t been studied much, or at all. For example, when a social media platform is launched, there’s an opportunity to explore its impacts on users, how it could be leveraged for marketing, its impact on society, and so on. The same applies for new technologies, new modes of communication, transportation, etc.
Classic literature gaps can present exciting research opportunities , but a drawback you need to be aware of is that with this type of research gap, you’ll be exploring completely new territory . This means you’ll have to draw on adjacent literature (that is, research in adjacent fields) to build your literature review, as there naturally won’t be very many existing studies that directly relate to the topic. While this is manageable, it can be challenging for first-time researchers, so be careful not to bite off more than you can chew.

2. The Disagreement Gap
As the name suggests, the disagreement gap emerges when there are contrasting or contradictory findings in the existing research regarding a specific research question (or set of questions). The hypothetical example we looked at earlier regarding the causes of a disease reflects a disagreement gap.
Importantly, for this type of research gap, there needs to be a relatively balanced set of opposing findings . In other words, a situation where 95% of studies find one result and 5% find the opposite result wouldn’t quite constitute a disagreement in the literature. Of course, it’s hard to quantify exactly how much weight to give to each study, but you’ll need to at least show that the opposing findings aren’t simply a corner-case anomaly .

3. The Contextual Gap
The third type of research gap is the contextual gap. Simply put, a contextual gap exists when there’s already a decent body of existing research on a particular topic, but an absence of research in specific contexts .
For example, there could be a lack of research on:
- A specific population – perhaps a certain age group, gender or ethnicity
- A geographic area – for example, a city, country or region
- A certain time period – perhaps the bulk of the studies took place many years or even decades ago and the landscape has changed.
The contextual gap is a popular option for dissertations and theses, especially for first-time researchers, as it allows you to develop your research on a solid foundation of existing literature and potentially even use existing survey measures.
Importantly, if you’re gonna go this route, you need to ensure that there’s a plausible reason why you’d expect potential differences in the specific context you choose. If there’s no reason to expect different results between existing and new contexts, the research gap wouldn’t be well justified. So, make sure that you can clearly articulate why your chosen context is “different” from existing studies and why that might reasonably result in different findings.

4. The Methodological Gap
Last but not least, we have the methodological gap. As the name suggests, this type of research gap emerges as a result of the research methodology or design of existing studies. With this approach, you’d argue that the methodology of existing studies is lacking in some way , or that they’re missing a certain perspective.
For example, you might argue that the bulk of the existing research has taken a quantitative approach, and therefore there is a lack of rich insight and texture that a qualitative study could provide. Similarly, you might argue that existing studies have primarily taken a cross-sectional approach , and as a result, have only provided a snapshot view of the situation – whereas a longitudinal approach could help uncover how constructs or variables have evolved over time.

Practical Examples
Let’s take a look at some practical examples so that you can see how research gaps are typically expressed in written form. Keep in mind that these are just examples – not actual current gaps (we’ll show you how to find these a little later!).
Context: Healthcare
Despite extensive research on diabetes management, there’s a research gap in terms of understanding the effectiveness of digital health interventions in rural populations (compared to urban ones) within Eastern Europe.
Context: Environmental Science
While a wealth of research exists regarding plastic pollution in oceans, there is significantly less understanding of microplastic accumulation in freshwater ecosystems like rivers and lakes, particularly within Southern Africa.
Context: Education
While empirical research surrounding online learning has grown over the past five years, there remains a lack of comprehensive studies regarding the effectiveness of online learning for students with special educational needs.
As you can see in each of these examples, the author begins by clearly acknowledging the existing research and then proceeds to explain where the current area of lack (i.e., the research gap) exists.

How To Find A Research Gap
Now that you’ve got a clearer picture of the different types of research gaps, the next question is of course, “how do you find these research gaps?” .
Well, we cover the process of how to find original, high-value research gaps in a separate post . But, for now, I’ll share a basic two-step strategy here to help you find potential research gaps.
As a starting point, you should find as many literature reviews, systematic reviews and meta-analyses as you can, covering your area of interest. Additionally, you should dig into the most recent journal articles to wrap your head around the current state of knowledge. It’s also a good idea to look at recent dissertations and theses (especially doctoral-level ones). Dissertation databases such as ProQuest, EBSCO and Open Access are a goldmine for this sort of thing. Importantly, make sure that you’re looking at recent resources (ideally those published in the last year or two), or the gaps you find might have already been plugged by other researchers.
Once you’ve gathered a meaty collection of resources, the section that you really want to focus on is the one titled “ further research opportunities ” or “further research is needed”. In this section, the researchers will explicitly state where more studies are required – in other words, where potential research gaps may exist. You can also look at the “ limitations ” section of the studies, as this will often spur ideas for methodology-based research gaps.
By following this process, you’ll orient yourself with the current state of research , which will lay the foundation for you to identify potential research gaps. You can then start drawing up a shortlist of ideas and evaluating them as candidate topics . But remember, make sure you’re looking at recent articles – there’s no use going down a rabbit hole only to find that someone’s already filled the gap 🙂
Let’s Recap
We’ve covered a lot of ground in this post. Here are the key takeaways:
- A research gap is an unanswered question or unresolved problem in a field, which reflects a lack of existing research in that space.
- The four most common types of research gaps are the classic literature gap, the disagreement gap, the contextual gap and the methodological gap.
- To find potential research gaps, start by reviewing recent journal articles in your area of interest, paying particular attention to the FRIN section .
If you’re keen to learn more about research gaps and research topic ideation in general, be sure to check out the rest of the Grad Coach Blog . Alternatively, if you’re looking for 1-on-1 support with your dissertation, thesis or research project, be sure to check out our private coaching service .

Psst... there’s more!
This post was based on one of our popular Research Bootcamps . If you're working on a research project, you'll definitely want to check this out ...
You Might Also Like:

38 Comments
This post is REALLY more than useful, Thank you very very much
Very helpful specialy, for those who are new for writing a research! So thank you very much!!
I found it very helpful article. Thank you.
it very good but what need to be clear with the concept is when di we use research gap before we conduct aresearch or after we finished it ,or are we propose it to be solved or studied or to show that we are unable to cover so that we let it to be studied by other researchers ?
Just at the time when I needed it, really helpful.
Very helpful and well-explained. Thank you
VERY HELPFUL
We’re very grateful for your guidance, indeed we have been learning a lot from you , so thank you abundantly once again.
hello brother could you explain to me this question explain the gaps that researchers are coming up with ?
Am just starting to write my research paper. your publication is very helpful. Thanks so much
How to cite the author of this?
your explanation very help me for research paper. thank you
Very important presentation. Thanks.
Very helpful indeed
Best Ideas. Thank you.
I found it’s an excellent blog to get more insights about the Research Gap. I appreciate it!
Kindly explain to me how to generate good research objectives.
This is very helpful, thank you
How to tabulate research gap
Very helpful, thank you.
Thanks a lot for this great insight!
This is really helpful indeed!
This article is really helpfull in discussing how will we be able to define better a research problem of our interest. Thanks so much.
Reading this just in good time as i prepare the proposal for my PhD topic defense.
Very helpful Thanks a lot.
Thank you very much
This was very timely. Kudos
Great one! Thank you all.
Thank you very much.
This is so enlightening. Disagreement gap. Thanks for the insight.
How do I Cite this document please?
Research gap about career choice given me Example bro?
I found this information so relevant as I am embarking on a Masters Degree. Thank you for this eye opener. It make me feel I can work diligently and smart on my research proposal.
This is very helpful to beginners of research. You have good teaching strategy that use favorable language that limit everyone from being bored. Kudos!!!!!
This plat form is very useful under academic arena therefore im stil learning a lot of informations that will help to reduce the burden during development of my PhD thesis
This information is beneficial to me.
Insightful…
Submit a Comment Cancel reply
Your email address will not be published. Required fields are marked *
Save my name, email, and website in this browser for the next time I comment.
- Print Friendly
Have a language expert improve your writing
Run a free plagiarism check in 10 minutes, generate accurate citations for free.
- Knowledge Base
Methodology
- How to Write a Literature Review | Guide, Examples, & Templates
How to Write a Literature Review | Guide, Examples, & Templates
Published on January 2, 2023 by Shona McCombes . Revised on September 11, 2023.
What is a literature review? A literature review is a survey of scholarly sources on a specific topic. It provides an overview of current knowledge, allowing you to identify relevant theories, methods, and gaps in the existing research that you can later apply to your paper, thesis, or dissertation topic .
There are five key steps to writing a literature review:
- Search for relevant literature
- Evaluate sources
- Identify themes, debates, and gaps
- Outline the structure
- Write your literature review
A good literature review doesn’t just summarize sources—it analyzes, synthesizes , and critically evaluates to give a clear picture of the state of knowledge on the subject.
Instantly correct all language mistakes in your text
Upload your document to correct all your mistakes in minutes
Table of contents
What is the purpose of a literature review, examples of literature reviews, step 1 – search for relevant literature, step 2 – evaluate and select sources, step 3 – identify themes, debates, and gaps, step 4 – outline your literature review’s structure, step 5 – write your literature review, free lecture slides, other interesting articles, frequently asked questions, introduction.
- Quick Run-through
- Step 1 & 2
When you write a thesis , dissertation , or research paper , you will likely have to conduct a literature review to situate your research within existing knowledge. The literature review gives you a chance to:
- Demonstrate your familiarity with the topic and its scholarly context
- Develop a theoretical framework and methodology for your research
- Position your work in relation to other researchers and theorists
- Show how your research addresses a gap or contributes to a debate
- Evaluate the current state of research and demonstrate your knowledge of the scholarly debates around your topic.
Writing literature reviews is a particularly important skill if you want to apply for graduate school or pursue a career in research. We’ve written a step-by-step guide that you can follow below.
Here's why students love Scribbr's proofreading services
Discover proofreading & editing
Writing literature reviews can be quite challenging! A good starting point could be to look at some examples, depending on what kind of literature review you’d like to write.
- Example literature review #1: “Why Do People Migrate? A Review of the Theoretical Literature” ( Theoretical literature review about the development of economic migration theory from the 1950s to today.)
- Example literature review #2: “Literature review as a research methodology: An overview and guidelines” ( Methodological literature review about interdisciplinary knowledge acquisition and production.)
- Example literature review #3: “The Use of Technology in English Language Learning: A Literature Review” ( Thematic literature review about the effects of technology on language acquisition.)
- Example literature review #4: “Learners’ Listening Comprehension Difficulties in English Language Learning: A Literature Review” ( Chronological literature review about how the concept of listening skills has changed over time.)
You can also check out our templates with literature review examples and sample outlines at the links below.
Download Word doc Download Google doc
Before you begin searching for literature, you need a clearly defined topic .
If you are writing the literature review section of a dissertation or research paper, you will search for literature related to your research problem and questions .
Make a list of keywords
Start by creating a list of keywords related to your research question. Include each of the key concepts or variables you’re interested in, and list any synonyms and related terms. You can add to this list as you discover new keywords in the process of your literature search.
- Social media, Facebook, Instagram, Twitter, Snapchat, TikTok
- Body image, self-perception, self-esteem, mental health
- Generation Z, teenagers, adolescents, youth
Search for relevant sources
Use your keywords to begin searching for sources. Some useful databases to search for journals and articles include:
- Your university’s library catalogue
- Google Scholar
- Project Muse (humanities and social sciences)
- Medline (life sciences and biomedicine)
- EconLit (economics)
- Inspec (physics, engineering and computer science)
You can also use boolean operators to help narrow down your search.
Make sure to read the abstract to find out whether an article is relevant to your question. When you find a useful book or article, you can check the bibliography to find other relevant sources.
You likely won’t be able to read absolutely everything that has been written on your topic, so it will be necessary to evaluate which sources are most relevant to your research question.
For each publication, ask yourself:
- What question or problem is the author addressing?
- What are the key concepts and how are they defined?
- What are the key theories, models, and methods?
- Does the research use established frameworks or take an innovative approach?
- What are the results and conclusions of the study?
- How does the publication relate to other literature in the field? Does it confirm, add to, or challenge established knowledge?
- What are the strengths and weaknesses of the research?
Make sure the sources you use are credible , and make sure you read any landmark studies and major theories in your field of research.
You can use our template to summarize and evaluate sources you’re thinking about using. Click on either button below to download.
Take notes and cite your sources
As you read, you should also begin the writing process. Take notes that you can later incorporate into the text of your literature review.
It is important to keep track of your sources with citations to avoid plagiarism . It can be helpful to make an annotated bibliography , where you compile full citation information and write a paragraph of summary and analysis for each source. This helps you remember what you read and saves time later in the process.
To begin organizing your literature review’s argument and structure, be sure you understand the connections and relationships between the sources you’ve read. Based on your reading and notes, you can look for:
- Trends and patterns (in theory, method or results): do certain approaches become more or less popular over time?
- Themes: what questions or concepts recur across the literature?
- Debates, conflicts and contradictions: where do sources disagree?
- Pivotal publications: are there any influential theories or studies that changed the direction of the field?
- Gaps: what is missing from the literature? Are there weaknesses that need to be addressed?
This step will help you work out the structure of your literature review and (if applicable) show how your own research will contribute to existing knowledge.
- Most research has focused on young women.
- There is an increasing interest in the visual aspects of social media.
- But there is still a lack of robust research on highly visual platforms like Instagram and Snapchat—this is a gap that you could address in your own research.
There are various approaches to organizing the body of a literature review. Depending on the length of your literature review, you can combine several of these strategies (for example, your overall structure might be thematic, but each theme is discussed chronologically).
Chronological
The simplest approach is to trace the development of the topic over time. However, if you choose this strategy, be careful to avoid simply listing and summarizing sources in order.
Try to analyze patterns, turning points and key debates that have shaped the direction of the field. Give your interpretation of how and why certain developments occurred.
If you have found some recurring central themes, you can organize your literature review into subsections that address different aspects of the topic.
For example, if you are reviewing literature about inequalities in migrant health outcomes, key themes might include healthcare policy, language barriers, cultural attitudes, legal status, and economic access.
Methodological
If you draw your sources from different disciplines or fields that use a variety of research methods , you might want to compare the results and conclusions that emerge from different approaches. For example:
- Look at what results have emerged in qualitative versus quantitative research
- Discuss how the topic has been approached by empirical versus theoretical scholarship
- Divide the literature into sociological, historical, and cultural sources
Theoretical
A literature review is often the foundation for a theoretical framework . You can use it to discuss various theories, models, and definitions of key concepts.
You might argue for the relevance of a specific theoretical approach, or combine various theoretical concepts to create a framework for your research.
Like any other academic text , your literature review should have an introduction , a main body, and a conclusion . What you include in each depends on the objective of your literature review.
The introduction should clearly establish the focus and purpose of the literature review.
Depending on the length of your literature review, you might want to divide the body into subsections. You can use a subheading for each theme, time period, or methodological approach.
As you write, you can follow these tips:
- Summarize and synthesize: give an overview of the main points of each source and combine them into a coherent whole
- Analyze and interpret: don’t just paraphrase other researchers — add your own interpretations where possible, discussing the significance of findings in relation to the literature as a whole
- Critically evaluate: mention the strengths and weaknesses of your sources
- Write in well-structured paragraphs: use transition words and topic sentences to draw connections, comparisons and contrasts
In the conclusion, you should summarize the key findings you have taken from the literature and emphasize their significance.
When you’ve finished writing and revising your literature review, don’t forget to proofread thoroughly before submitting. Not a language expert? Check out Scribbr’s professional proofreading services !
This article has been adapted into lecture slides that you can use to teach your students about writing a literature review.
Scribbr slides are free to use, customize, and distribute for educational purposes.
Open Google Slides Download PowerPoint
If you want to know more about the research process , methodology , research bias , or statistics , make sure to check out some of our other articles with explanations and examples.
- Sampling methods
- Simple random sampling
- Stratified sampling
- Cluster sampling
- Likert scales
- Reproducibility
Statistics
- Null hypothesis
- Statistical power
- Probability distribution
- Effect size
- Poisson distribution
Research bias
- Optimism bias
- Cognitive bias
- Implicit bias
- Hawthorne effect
- Anchoring bias
- Explicit bias
A literature review is a survey of scholarly sources (such as books, journal articles, and theses) related to a specific topic or research question .
It is often written as part of a thesis, dissertation , or research paper , in order to situate your work in relation to existing knowledge.
There are several reasons to conduct a literature review at the beginning of a research project:
- To familiarize yourself with the current state of knowledge on your topic
- To ensure that you’re not just repeating what others have already done
- To identify gaps in knowledge and unresolved problems that your research can address
- To develop your theoretical framework and methodology
- To provide an overview of the key findings and debates on the topic
Writing the literature review shows your reader how your work relates to existing research and what new insights it will contribute.
The literature review usually comes near the beginning of your thesis or dissertation . After the introduction , it grounds your research in a scholarly field and leads directly to your theoretical framework or methodology .
A literature review is a survey of credible sources on a topic, often used in dissertations , theses, and research papers . Literature reviews give an overview of knowledge on a subject, helping you identify relevant theories and methods, as well as gaps in existing research. Literature reviews are set up similarly to other academic texts , with an introduction , a main body, and a conclusion .
An annotated bibliography is a list of source references that has a short description (called an annotation ) for each of the sources. It is often assigned as part of the research process for a paper .
Cite this Scribbr article
If you want to cite this source, you can copy and paste the citation or click the “Cite this Scribbr article” button to automatically add the citation to our free Citation Generator.
McCombes, S. (2023, September 11). How to Write a Literature Review | Guide, Examples, & Templates. Scribbr. Retrieved July 8, 2024, from https://www.scribbr.com/dissertation/literature-review/
Is this article helpful?
Shona McCombes
Other students also liked, what is a theoretical framework | guide to organizing, what is a research methodology | steps & tips, how to write a research proposal | examples & templates, get unlimited documents corrected.
✔ Free APA citation check included ✔ Unlimited document corrections ✔ Specialized in correcting academic texts
- Privacy Policy

Home » Research Gap – Types, Examples and How to Identify
Research Gap – Types, Examples and How to Identify
Table of Contents

Research Gap
Definition:
Research gap refers to an area or topic within a field of study that has not yet been extensively researched or is yet to be explored. It is a question, problem or issue that has not been addressed or resolved by previous research.
How to Identify Research Gap
Identifying a research gap is an essential step in conducting research that adds value and contributes to the existing body of knowledge. Research gap requires critical thinking, creativity, and a thorough understanding of the existing literature . It is an iterative process that may require revisiting and refining your research questions and ideas multiple times.
Here are some steps that can help you identify a research gap:
- Review existing literature: Conduct a thorough review of the existing literature in your research area. This will help you identify what has already been studied and what gaps still exist.
- Identify a research problem: Identify a specific research problem or question that you want to address.
- Analyze existing research: Analyze the existing research related to your research problem. This will help you identify areas that have not been studied, inconsistencies in the findings, or limitations of the previous research.
- Brainstorm potential research ideas : Based on your analysis, brainstorm potential research ideas that address the identified gaps.
- Consult with experts: Consult with experts in your research area to get their opinions on potential research ideas and to identify any additional gaps that you may have missed.
- Refine research questions: Refine your research questions and hypotheses based on the identified gaps and potential research ideas.
- Develop a research proposal: Develop a research proposal that outlines your research questions, objectives, and methods to address the identified research gap.
Types of Research Gap
There are different types of research gaps that can be identified, and each type is associated with a specific situation or problem. Here are the main types of research gaps and their explanations:
Theoretical Gap
This type of research gap refers to a lack of theoretical understanding or knowledge in a particular area. It can occur when there is a discrepancy between existing theories and empirical evidence or when there is no theory that can explain a particular phenomenon. Identifying theoretical gaps can lead to the development of new theories or the refinement of existing ones.
Empirical Gap
An empirical gap occurs when there is a lack of empirical evidence or data in a particular area. It can happen when there is a lack of research on a specific topic or when existing research is inadequate or inconclusive. Identifying empirical gaps can lead to the development of new research studies to collect data or the refinement of existing research methods to improve the quality of data collected.
Methodological Gap
This type of research gap refers to a lack of appropriate research methods or techniques to answer a research question. It can occur when existing methods are inadequate, outdated, or inappropriate for the research question. Identifying methodological gaps can lead to the development of new research methods or the modification of existing ones to better address the research question.
Practical Gap
A practical gap occurs when there is a lack of practical applications or implementation of research findings. It can occur when research findings are not implemented due to financial, political, or social constraints. Identifying practical gaps can lead to the development of strategies for the effective implementation of research findings in practice.
Knowledge Gap
This type of research gap occurs when there is a lack of knowledge or information on a particular topic. It can happen when a new area of research is emerging, or when research is conducted in a different context or population. Identifying knowledge gaps can lead to the development of new research studies or the extension of existing research to fill the gap.
Examples of Research Gap
Here are some examples of research gaps that researchers might identify:
- Theoretical Gap Example : In the field of psychology, there might be a theoretical gap related to the lack of understanding of the relationship between social media use and mental health. Although there is existing research on the topic, there might be a lack of consensus on the mechanisms that link social media use to mental health outcomes.
- Empirical Gap Example : In the field of environmental science, there might be an empirical gap related to the lack of data on the long-term effects of climate change on biodiversity in specific regions. Although there might be some studies on the topic, there might be a lack of data on the long-term effects of climate change on specific species or ecosystems.
- Methodological Gap Example : In the field of education, there might be a methodological gap related to the lack of appropriate research methods to assess the impact of online learning on student outcomes. Although there might be some studies on the topic, existing research methods might not be appropriate to assess the complex relationships between online learning and student outcomes.
- Practical Gap Example: In the field of healthcare, there might be a practical gap related to the lack of effective strategies to implement evidence-based practices in clinical settings. Although there might be existing research on the effectiveness of certain practices, they might not be implemented in practice due to various barriers, such as financial constraints or lack of resources.
- Knowledge Gap Example: In the field of anthropology, there might be a knowledge gap related to the lack of understanding of the cultural practices of indigenous communities in certain regions. Although there might be some research on the topic, there might be a lack of knowledge about specific cultural practices or beliefs that are unique to those communities.
Examples of Research Gap In Literature Review, Thesis, and Research Paper might be:
- Literature review : A literature review on the topic of machine learning and healthcare might identify a research gap in the lack of studies that investigate the use of machine learning for early detection of rare diseases.
- Thesis : A thesis on the topic of cybersecurity might identify a research gap in the lack of studies that investigate the effectiveness of artificial intelligence in detecting and preventing cyber attacks.
- Research paper : A research paper on the topic of natural language processing might identify a research gap in the lack of studies that investigate the use of natural language processing techniques for sentiment analysis in non-English languages.
How to Write Research Gap
By following these steps, you can effectively write about research gaps in your paper and clearly articulate the contribution that your study will make to the existing body of knowledge.
Here are some steps to follow when writing about research gaps in your paper:
- Identify the research question : Before writing about research gaps, you need to identify your research question or problem. This will help you to understand the scope of your research and identify areas where additional research is needed.
- Review the literature: Conduct a thorough review of the literature related to your research question. This will help you to identify the current state of knowledge in the field and the gaps that exist.
- Identify the research gap: Based on your review of the literature, identify the specific research gap that your study will address. This could be a theoretical, empirical, methodological, practical, or knowledge gap.
- Provide evidence: Provide evidence to support your claim that the research gap exists. This could include a summary of the existing literature, a discussion of the limitations of previous studies, or an analysis of the current state of knowledge in the field.
- Explain the importance: Explain why it is important to fill the research gap. This could include a discussion of the potential implications of filling the gap, the significance of the research for the field, or the potential benefits to society.
- State your research objectives: State your research objectives, which should be aligned with the research gap you have identified. This will help you to clearly articulate the purpose of your study and how it will address the research gap.
Importance of Research Gap
The importance of research gaps can be summarized as follows:
- Advancing knowledge: Identifying research gaps is crucial for advancing knowledge in a particular field. By identifying areas where additional research is needed, researchers can fill gaps in the existing body of knowledge and contribute to the development of new theories and practices.
- Guiding research: Research gaps can guide researchers in designing studies that fill those gaps. By identifying research gaps, researchers can develop research questions and objectives that are aligned with the needs of the field and contribute to the development of new knowledge.
- Enhancing research quality: By identifying research gaps, researchers can avoid duplicating previous research and instead focus on developing innovative research that fills gaps in the existing body of knowledge. This can lead to more impactful research and higher-quality research outputs.
- Informing policy and practice: Research gaps can inform policy and practice by highlighting areas where additional research is needed to inform decision-making. By filling research gaps, researchers can provide evidence-based recommendations that have the potential to improve policy and practice in a particular field.
Applications of Research Gap
Here are some potential applications of research gap:
- Informing research priorities: Research gaps can help guide research funding agencies and researchers to prioritize research areas that require more attention and resources.
- Identifying practical implications: Identifying gaps in knowledge can help identify practical applications of research that are still unexplored or underdeveloped.
- Stimulating innovation: Research gaps can encourage innovation and the development of new approaches or methodologies to address unexplored areas.
- Improving policy-making: Research gaps can inform policy-making decisions by highlighting areas where more research is needed to make informed policy decisions.
- Enhancing academic discourse: Research gaps can lead to new and constructive debates and discussions within academic communities, leading to more robust and comprehensive research.
Advantages of Research Gap
Here are some of the advantages of research gap:
- Identifies new research opportunities: Identifying research gaps can help researchers identify areas that require further exploration, which can lead to new research opportunities.
- Improves the quality of research: By identifying gaps in current research, researchers can focus their efforts on addressing unanswered questions, which can improve the overall quality of research.
- Enhances the relevance of research: Research that addresses existing gaps can have significant implications for the development of theories, policies, and practices, and can therefore increase the relevance and impact of research.
- Helps avoid duplication of effort: Identifying existing research can help researchers avoid duplicating efforts, saving time and resources.
- Helps to refine research questions: Research gaps can help researchers refine their research questions, making them more focused and relevant to the needs of the field.
- Promotes collaboration: By identifying areas of research that require further investigation, researchers can collaborate with others to conduct research that addresses these gaps, which can lead to more comprehensive and impactful research outcomes.
Disadvantages of Research Gap
While research gaps can be advantageous, there are also some potential disadvantages that should be considered:
- Difficulty in identifying gaps: Identifying gaps in existing research can be challenging, particularly in fields where there is a large volume of research or where research findings are scattered across different disciplines.
- Lack of funding: Addressing research gaps may require significant resources, and researchers may struggle to secure funding for their work if it is perceived as too risky or uncertain.
- Time-consuming: Conducting research to address gaps can be time-consuming, particularly if the research involves collecting new data or developing new methods.
- Risk of oversimplification: Addressing research gaps may require researchers to simplify complex problems, which can lead to oversimplification and a failure to capture the complexity of the issues.
- Bias : Identifying research gaps can be influenced by researchers’ personal biases or perspectives, which can lead to a skewed understanding of the field.
- Potential for disagreement: Identifying research gaps can be subjective, and different researchers may have different views on what constitutes a gap in the field, leading to disagreements and debate.
About the author
Muhammad Hassan
Researcher, Academic Writer, Web developer
You may also like

Purpose of Research – Objectives and Applications

Appendix in Research Paper – Examples and...

Research Project – Definition, Writing Guide and...

Research Objectives – Types, Examples and...

Research Contribution – Thesis Guide

APA Table of Contents – Format and Example

- Planning to Write
Q: How do I identify a research gap during the literature review?
When writing the literature review of a particular research topic, how do I know what the previous literature is missing and what needs to be addressed?
Asked on 29 Jan, 2021
Specifically in the context of doing and writing the literature review, you can identify a gap in any/all of the following ways:
- Look up papers that build on previous papers, be it by the same author/s or others. Find out what gaps the later papers have addressed, and if there are still any.
- On the same lines, you may also wish to go through papers cited by the present paper.
- Go through the Discussion/Conclusion section of the paper, where the author(s) talk(s) of the shortcomings of their research and suggest ways in which they think their research could be improved in the future. Also go through the implications and recommendations mentioned (if any) in case there are any ideas there.
- Finally, it also comes down to your knowledge of the topic you are studying and your research acumen, your astuteness in being able to identify a gap that could lead to a potential study of considerable significance/impact. This, as you can gauge, will come with time.
For now, here are some resources for further help with your question.
- How does a problem statement lend itself to further inquiry on confirming a gap in research?
- How can I describe the gap in literature when no previous research has been done on the problem?
- Would my work be considered addressing a research gap or making a contribution?
And here are some resources for help with writing a literature review .
- What a journal editor expects to see in a literature review
- How to write the literature review of your research paper
And in case you’re presently writing a review paper, all the best!
Answered by Editage Insights on 02 Feb, 2021
- Upvote this Answer

This content belongs to the Conducting Research Stage
Confirm that you would also like to sign up for free personalized email coaching for this stage.
Trending Searches
- Statement of the problem
- Background of study
- Scope of the study
- Types of qualitative research
- Rationale of the study
- Concept paper
- Literature review
- Introduction in research
- Under "Editor Evaluation"
- Ethics in research
Recent Searches
- Review paper
- Responding to reviewer comments
- Predatory publishers
- Scope and delimitations
- Open access
- Plagiarism in research
- Journal selection tips
- Editor assigned
- Types of articles
- "Reject and Resubmit" status
- Decision in process
- Conflict of interest
Research Methods
- Getting Started
- Literature Review Research
- Research Design
- Research Design By Discipline
- SAGE Research Methods
- Teaching with SAGE Research Methods
Literature Review
- What is a Literature Review?
- What is NOT a Literature Review?
- Purposes of a Literature Review
- Types of Literature Reviews
- Literature Reviews vs. Systematic Reviews
- Systematic vs. Meta-Analysis
Literature Review is a comprehensive survey of the works published in a particular field of study or line of research, usually over a specific period of time, in the form of an in-depth, critical bibliographic essay or annotated list in which attention is drawn to the most significant works.
Also, we can define a literature review as the collected body of scholarly works related to a topic:
- Summarizes and analyzes previous research relevant to a topic
- Includes scholarly books and articles published in academic journals
- Can be an specific scholarly paper or a section in a research paper
The objective of a Literature Review is to find previous published scholarly works relevant to an specific topic
- Help gather ideas or information
- Keep up to date in current trends and findings
- Help develop new questions
A literature review is important because it:
- Explains the background of research on a topic.
- Demonstrates why a topic is significant to a subject area.
- Helps focus your own research questions or problems
- Discovers relationships between research studies/ideas.
- Suggests unexplored ideas or populations
- Identifies major themes, concepts, and researchers on a topic.
- Tests assumptions; may help counter preconceived ideas and remove unconscious bias.
- Identifies critical gaps, points of disagreement, or potentially flawed methodology or theoretical approaches.
- Indicates potential directions for future research.
All content in this section is from Literature Review Research from Old Dominion University
Keep in mind the following, a literature review is NOT:
Not an essay
Not an annotated bibliography in which you summarize each article that you have reviewed. A literature review goes beyond basic summarizing to focus on the critical analysis of the reviewed works and their relationship to your research question.
Not a research paper where you select resources to support one side of an issue versus another. A lit review should explain and consider all sides of an argument in order to avoid bias, and areas of agreement and disagreement should be highlighted.
A literature review serves several purposes. For example, it
- provides thorough knowledge of previous studies; introduces seminal works.
- helps focus one’s own research topic.
- identifies a conceptual framework for one’s own research questions or problems; indicates potential directions for future research.
- suggests previously unused or underused methodologies, designs, quantitative and qualitative strategies.
- identifies gaps in previous studies; identifies flawed methodologies and/or theoretical approaches; avoids replication of mistakes.
- helps the researcher avoid repetition of earlier research.
- suggests unexplored populations.
- determines whether past studies agree or disagree; identifies controversy in the literature.
- tests assumptions; may help counter preconceived ideas and remove unconscious bias.
As Kennedy (2007) notes*, it is important to think of knowledge in a given field as consisting of three layers. First, there are the primary studies that researchers conduct and publish. Second are the reviews of those studies that summarize and offer new interpretations built from and often extending beyond the original studies. Third, there are the perceptions, conclusions, opinion, and interpretations that are shared informally that become part of the lore of field. In composing a literature review, it is important to note that it is often this third layer of knowledge that is cited as "true" even though it often has only a loose relationship to the primary studies and secondary literature reviews.
Given this, while literature reviews are designed to provide an overview and synthesis of pertinent sources you have explored, there are several approaches to how they can be done, depending upon the type of analysis underpinning your study. Listed below are definitions of types of literature reviews:
Argumentative Review This form examines literature selectively in order to support or refute an argument, deeply imbedded assumption, or philosophical problem already established in the literature. The purpose is to develop a body of literature that establishes a contrarian viewpoint. Given the value-laden nature of some social science research [e.g., educational reform; immigration control], argumentative approaches to analyzing the literature can be a legitimate and important form of discourse. However, note that they can also introduce problems of bias when they are used to to make summary claims of the sort found in systematic reviews.
Integrative Review Considered a form of research that reviews, critiques, and synthesizes representative literature on a topic in an integrated way such that new frameworks and perspectives on the topic are generated. The body of literature includes all studies that address related or identical hypotheses. A well-done integrative review meets the same standards as primary research in regard to clarity, rigor, and replication.
Historical Review Few things rest in isolation from historical precedent. Historical reviews are focused on examining research throughout a period of time, often starting with the first time an issue, concept, theory, phenomena emerged in the literature, then tracing its evolution within the scholarship of a discipline. The purpose is to place research in a historical context to show familiarity with state-of-the-art developments and to identify the likely directions for future research.
Methodological Review A review does not always focus on what someone said [content], but how they said it [method of analysis]. This approach provides a framework of understanding at different levels (i.e. those of theory, substantive fields, research approaches and data collection and analysis techniques), enables researchers to draw on a wide variety of knowledge ranging from the conceptual level to practical documents for use in fieldwork in the areas of ontological and epistemological consideration, quantitative and qualitative integration, sampling, interviewing, data collection and data analysis, and helps highlight many ethical issues which we should be aware of and consider as we go through our study.
Systematic Review This form consists of an overview of existing evidence pertinent to a clearly formulated research question, which uses pre-specified and standardized methods to identify and critically appraise relevant research, and to collect, report, and analyse data from the studies that are included in the review. Typically it focuses on a very specific empirical question, often posed in a cause-and-effect form, such as "To what extent does A contribute to B?"
Theoretical Review The purpose of this form is to concretely examine the corpus of theory that has accumulated in regard to an issue, concept, theory, phenomena. The theoretical literature review help establish what theories already exist, the relationships between them, to what degree the existing theories have been investigated, and to develop new hypotheses to be tested. Often this form is used to help establish a lack of appropriate theories or reveal that current theories are inadequate for explaining new or emerging research problems. The unit of analysis can focus on a theoretical concept or a whole theory or framework.
* Kennedy, Mary M. "Defining a Literature." Educational Researcher 36 (April 2007): 139-147.
All content in this section is from The Literature Review created by Dr. Robert Larabee USC
Robinson, P. and Lowe, J. (2015), Literature reviews vs systematic reviews. Australian and New Zealand Journal of Public Health, 39: 103-103. doi: 10.1111/1753-6405.12393

What's in the name? The difference between a Systematic Review and a Literature Review, and why it matters . By Lynn Kysh from University of Southern California

Systematic review or meta-analysis?
A systematic review answers a defined research question by collecting and summarizing all empirical evidence that fits pre-specified eligibility criteria.
A meta-analysis is the use of statistical methods to summarize the results of these studies.
Systematic reviews, just like other research articles, can be of varying quality. They are a significant piece of work (the Centre for Reviews and Dissemination at York estimates that a team will take 9-24 months), and to be useful to other researchers and practitioners they should have:
- clearly stated objectives with pre-defined eligibility criteria for studies
- explicit, reproducible methodology
- a systematic search that attempts to identify all studies
- assessment of the validity of the findings of the included studies (e.g. risk of bias)
- systematic presentation, and synthesis, of the characteristics and findings of the included studies
Not all systematic reviews contain meta-analysis.
Meta-analysis is the use of statistical methods to summarize the results of independent studies. By combining information from all relevant studies, meta-analysis can provide more precise estimates of the effects of health care than those derived from the individual studies included within a review. More information on meta-analyses can be found in Cochrane Handbook, Chapter 9 .
A meta-analysis goes beyond critique and integration and conducts secondary statistical analysis on the outcomes of similar studies. It is a systematic review that uses quantitative methods to synthesize and summarize the results.
An advantage of a meta-analysis is the ability to be completely objective in evaluating research findings. Not all topics, however, have sufficient research evidence to allow a meta-analysis to be conducted. In that case, an integrative review is an appropriate strategy.
Some of the content in this section is from Systematic reviews and meta-analyses: step by step guide created by Kate McAllister.
- << Previous: Getting Started
- Next: Research Design >>
- Last Updated: Aug 21, 2023 4:07 PM
- URL: https://guides.lib.udel.edu/researchmethods
Warning: The NCBI web site requires JavaScript to function. more...
An official website of the United States government
The .gov means it's official. Federal government websites often end in .gov or .mil. Before sharing sensitive information, make sure you're on a federal government site.
The site is secure. The https:// ensures that you are connecting to the official website and that any information you provide is encrypted and transmitted securely.
- Publications
- Account settings
- Browse Titles
NCBI Bookshelf. A service of the National Library of Medicine, National Institutes of Health.
Robinson KA, Akinyede O, Dutta T, et al. Framework for Determining Research Gaps During Systematic Review: Evaluation [Internet]. Rockville (MD): Agency for Healthcare Research and Quality (US); 2013 Feb.

Framework for Determining Research Gaps During Systematic Review: Evaluation [Internet].
Introduction.
The identification of gaps from systematic reviews is essential to the practice of “evidence-based research.” Health care research should begin and end with a systematic review. 1 - 3 A comprehensive and explicit consideration of the existing evidence is necessary for the identification and development of an unanswered and answerable question, for the design of a study most likely to answer that question, and for the interpretation of the results of the study. 4
In a systematic review, the consideration of existing evidence often highlights important areas where deficiencies in information limit our ability to make decisions. We define a research gap as a topic or area for which missing or inadequate information limits the ability of reviewers to reach a conclusion for a given question. A research gap may be further developed, such as through stakeholder engagement in prioritization, into research needs. Research needs are those areas where the gaps in the evidence limit decision making by patients, clinicians, and policy makers. A research gap may not be a research need if filling the gap would not be of use to stakeholders that make decisions in health care. The clear and explicit identification of research gaps is a necessary step in developing a research agenda. Evidence reports produced by Evidence-based Practice Centers (EPCs) have always included a future research section. However, in contrast to the explicit and transparent steps taken in the completion of a systematic review, there has not been a systematic process for the identification of research gaps.
In a prior methods project, our EPC set out to identify and pilot test a framework for the identification of research gaps. 5 , 6 We searched the literature, conducted an audit of EPC evidence reports, and sought information from other organizations which conduct evidence synthesis. Despite these efforts, we identified little detail or consistency in the frameworks used to determine research gaps within systematic reviews. In general, we found no widespread use or endorsement of a specific formal process or framework for identifying research gaps using systematic reviews.
We developed a framework to systematically identify research gaps from systematic reviews. This framework facilitates the classification of where the current evidence falls short and why the evidence falls short. The framework included two elements: (1) the characterization the gaps and (2) the identification and classification of the reason(s) for the research gap.
The PICOS structure (Population, Intervention, Comparison, Outcome and Setting) was used in this framework to describe questions or parts of questions inadequately addressed by the evidence synthesized in the systematic review. The issue of timing, sometimes included as PICOTS, was considered separately for Intervention, Comparison, and Outcome. The PICOS elements were the only sort of framework we had identified in an audit of existing methods for the identification of gaps used by EPCs and other related organizations (i.e., health technology assessment organizations). We chose to use this structure as it is one familiar to EPCs, and others, in developing questions.
It is not only important to identify research gaps but also to determine how the evidence falls short, in order to maximally inform researchers, policy makers, and funders on the types of questions that need to be addressed and the types of studies needed to address these questions. Thus, the second element of the framework was the classification of the reasons for the existence of a research gap. For each research gap, the reason(s) that most preclude conclusions from being made in the systematic review is chosen by the review team completing the framework. To leverage work already being completed by review teams, we mapped the reasons for research gaps to concepts from commonly used evidence grading systems. Briefly, these categories of reasons, explained in detail in the prior JHU EPC report 5 , are:
- Insufficient or imprecise information
- Biased information
- Inconsistent or unknown consistency results
- Not the right information
The framework facilitates a systematic approach to identifying research gaps and the reasons for those gaps. The identification of where the evidence falls short and how the evidence falls short is essential to the development of important research questions and in providing guidance in how to address these questions.
As part of the previous methods product, we developed a worksheet and instructions to facilitate the use of the framework when completing a systematic review (See Appendix A ). Preliminary evaluation of the framework and worksheet was completed by applying the framework to two completed EPC evidence reports. The framework was further refined through peer review. In this current project, we extend our work on this research gaps framework.
Our objective in this project was to complete two types of further evaluation: (1) application of the framework across a larger sample of existing systematic reviews in different topic areas, and (2) implementation of the framework by EPCs. These two objectives were used to evaluate the framework and instructions for usability and to evaluate the application of the framework by others, outside of our EPC, including as part of the process of completing an EPC report. Our overall goal was to produce a revised framework with guidance that could be used by EPCs to explicitly identify research gaps from systematic reviews.
- Cite this Page Robinson KA, Akinyede O, Dutta T, et al. Framework for Determining Research Gaps During Systematic Review: Evaluation [Internet]. Rockville (MD): Agency for Healthcare Research and Quality (US); 2013 Feb. Introduction.
- PDF version of this title (425K)
Other titles in these collections
- AHRQ Methods for Effective Health Care
- Health Services/Technology Assessment Texts (HSTAT)
Recent Activity
- Introduction - Framework for Determining Research Gaps During Systematic Review:... Introduction - Framework for Determining Research Gaps During Systematic Review: Evaluation
Your browsing activity is empty.
Activity recording is turned off.
Turn recording back on
Connect with NLM
National Library of Medicine 8600 Rockville Pike Bethesda, MD 20894
Web Policies FOIA HHS Vulnerability Disclosure
Help Accessibility Careers
info This is a space for the teal alert bar.
notifications This is a space for the yellow alert bar.

Research Process
- Brainstorming
- Explore Google This link opens in a new window
- Explore Web Resources
- Explore Background Information
- Explore Books
- Explore Scholarly Articles
- Narrowing a Topic
- Primary and Secondary Resources
- Academic, Popular & Trade Publications
- Scholarly and Peer-Reviewed Journals
- Grey Literature
- Clinical Trials
- Evidence Based Treatment
- Scholarly Research
- Database Research Log
- Search Limits
- Keyword Searching
- Boolean Operators
- Phrase Searching
- Truncation & Wildcard Symbols
- Proximity Searching
- Field Codes
- Subject Terms and Database Thesauri
- Reading a Scientific Article
- Website Evaluation
- Article Keywords and Subject Terms
- Cited References
- Citing Articles
- Related Results
- Search Within Publication
- Database Alerts & RSS Feeds
- Personal Database Accounts
- Persistent URLs
- Literature Gap and Future Research
- Web of Knowledge
- Annual Reviews
- Systematic Reviews & Meta-Analyses
- Finding Seminal Works
- Exhausting the Literature
- Finding Dissertations
- Researching Theoretical Frameworks
- Research Methodology & Design
- Tests and Measurements
- Organizing Research & Citations This link opens in a new window
- Scholarly Publication
- Learn the Library This link opens in a new window
Research Articles
These examples below illustrate how researchers from different disciplines identified gaps in existing literature. For additional examples, try a NavigatorSearch using this search string: ("Literature review") AND (gap*)
- Addressing the Recent Developments and Potential Gaps in the Literature of Corporate Sustainability
- Applications of Psychological Science to Teaching and Learning: Gaps in the Literature
- Attitudes, Risk Factors, and Behaviours of Gambling Among Adolescents and Young People: A Literature Review and Gap Analysis
- Do Psychological Diversity Climate, HRM Practices, and Personality Traits (Big Five) Influence Multicultural Workforce Job Satisfaction and Performance? Current Scenario, Literature Gap, and Future Research Directions
- Entrepreneurship Education: A Systematic Literature Review and Identification of an Existing Gap in the Field
- Evidence and Gaps in the Literature on HIV/STI Prevention Interventions Targeting Migrants in Receiving Countries: A Scoping Review
- Homeless Indigenous Veterans and the Current Gaps in Knowledge: The State of the Literature
- A Literature Review and Gap Analysis of Emerging Technologies and New Trends in Gambling
- A Review of Higher Education Image and Reputation Literature: Knowledge Gaps and a Research Agenda
- Trends and Gaps in Empirical Research on Open Educational Resources (OER): A Systematic Mapping of the Literature from 2015 to 2019
- Where Should We Go From Here? Identified Gaps in the Literature in Psychosocial Interventions for Youth With Autism Spectrum Disorder and Comorbid Anxiety
What is a ‘gap in the literature’?
The gap, also considered the missing piece or pieces in the research literature, is the area that has not yet been explored or is under-explored. This could be a population or sample (size, type, location, etc.), research method, data collection and/or analysis, or other research variables or conditions.
It is important to keep in mind, however, that just because you identify a gap in the research, it doesn't necessarily mean that your research question is worthy of exploration. You will want to make sure that your research will have valuable practical and/or theoretical implications. In other words, answering the research question could either improve existing practice and/or inform professional decision-making (Applied Degree), or it could revise, build upon, or create theoretical frameworks informing research design and practice (Ph.D Degree). See the Dissertation Center for additional information about dissertation criteria at NU.
For a additional information on gap statements, see the following:
- How to Find a Gap in the Literature
- Write Like a Scientist: Gap Statements
How do you identify the gaps?
Conducting an exhaustive literature review is your first step. As you search for journal articles, you will need to read critically across the breadth of the literature to identify these gaps. You goal should be to find a ‘space’ or opening for contributing new research. The first step is gathering a broad range of research articles on your topic. You may want to look for research that approaches the topic from a variety of methods – qualitative, quantitative, or mixed methods.
See the videos below for further instruction on identifying a gap in the literature.
Identifying a Gap in the Literature - Dr. Laurie Bedford
How Do You Identify Gaps in Literature? - SAGE Research Methods
Literature Gap & Future Research - Library Workshop
This workshop presents effective search techniques for identifying a gap in the literature and recommendations for future research.
Where can you locate research gaps?
As you begin to gather the literature, you will want to critically read for what has, and has not, been learned from the research. Use the Discussion and Future Research sections of the articles to understand what the researchers have found and where they point out future or additional research areas. This is similar to identifying a gap in the literature, however, future research statements come from a single study rather than an exhaustive search. You will want to check the literature to see if those research questions have already been answered.

Roadrunner Search
Identifying the gap in the research relies on an exhaustive review of the literature. Remember, researchers may not explicitly state that a gap in the literature exists; you may need to thoroughly review and assess the research to make that determination yourself.
However, there are techniques that you can use when searching in NavigatorSearch to help identify gaps in the literature. You may use search terms such as "literature gap " or "future research" "along with your subject keywords to pinpoint articles that include these types of statements.

Was this resource helpful?
- << Previous: Resources for a Literature Review
- Next: Web of Knowledge >>
- Last Updated: Jun 12, 2024 1:44 PM
- URL: https://resources.nu.edu/researchprocess

© Copyright 2024 National University. All Rights Reserved.
Privacy Policy | Consumer Information
Research to Action
The Global Guide to Research Impact
Social Media
Framing challenges
Gap analysis for literature reviews and advancing useful knowledge
By Steve Wallis and Bernadette Wright 02/06/2020
The basics of research are seemingly clear. Read a lot of articles, see what’s missing, and conduct research to fill the gap in the literature. Wait a minute. What is that? ‘See what’s missing?’ How can we see something that is not there?
Imagine you are videoconferencing a colleague who is showing you the results of their project. Suddenly, the screen and sound cut out for a minute. After pressing some keys, you manage to restore the link; only to have your colleague ask, ‘What do you think?’. Of course, you know that you missed something from the presentation because of the disconnection. You can see that something is missing, and you know what to ask for to get your desired results, ‘Sorry, could you repeat that last minute of your presentation, please’. It’s not so easy when we’re looking at research results, proposals, or literature reviews.
While all research is, to some extent, useful, we’ve seen a lot of research that does not have the expected impact. That means wasted time, wasted money, under-served clients, and frustration on multiple levels. A big part of that problem is that directions for research are often chosen intuitively; in a sort of ad-hoc process. While we deeply respect the intuition of experts, that kind of process is not very rigorous.
In this post, we will show you how to ‘see the invisible’: How to identify the missing pieces in any study, literature review, or program analysis. With these straight-forward techniques, you will be able to better target your research in a more cost-effective way to fill those knowledge gaps to develop more effective theories, plans, and evaluations.
The first step is to choose your source material. That can be one or more articles, reports, or other study results. Of course, you want to be sure that the material you use is of high quality . Next, you want to create a causal map of your source material.
We’re going to go a bit abstract on you here because people sometimes get lost in the ‘content’ when what we are looking at here is more about the ‘structure’. Think of it like choosing how to buy a house based on how well it is built, rather than what color it is painted. So, instead of using actual concepts, we’ll refer to them as concepts A, B, C… and so on.
So, the text might say something like: ‘Our research shows that A causes B, B causes C, and D causes less C. Oh yes, and E is also important (although we’re not sure how it’s causally connected to A, B, C, or D)’.
When we draw causal maps from the source material we’ve found, we like to have key concepts in circles, with causal connections represented by arrows.

Figure 1. Abstract example of a causal map of a theory
There are really three basic kinds of gaps for you to find: relevance/meaning, logic/structure, and data/evidence. Starting with structure, there is a gap any place where there are two circles NOT connected by a causal arrow. It is important to have at least two arrows pointing at each concept/circle for the same reason we like to have multiple independent variables for each dependent variable (although, with more complex maps, we’re learning to see these as interdependent variables).
For example, there is no arrow between A and D. Also, there is no arrow between E and any of the other concepts. Each of those is a structural gap – an opening for additional research.
You might also notice that there are two arrows pointing directly at C. Like having two independent variables and one dependent variable, it is structurally better to have at least two arrows pointing at each concept.
So, structurally , C is in good shape. This part of the map has the least need for additional research. A larger gap exists around B, because it has only one arrow pointing at it (the arrow from A to B). Larger still is the gap around A, D, and E; because they have no arrows pointing at them.
To get the greatest leverage for your research dollar, it is generally best to search for that second arrow. In short, one research question would be: What (aside from A) has a causal influence on B? Other good research questions would be (a) Is there a causal relationship between A and D? (b) Is there a causal relationship between E and any of the other concepts? (c) What else besides A helps cause B? (d) What are the causes of A, D, and E?
Now, let’s take a look at gaps in the data, evidence, or information upon which each causal arrow is established.
From structure to data
Here, we add to the drawing by making a note showing (very briefly) the kind of data supporting each causal arrow. We like to have that in a box – with a loopy line ‘typing’ the evidence to the connection. You can also use different colors to more easily differentiate between the concepts and the evidence on your map. You can also write the note along the length of the arrow.

Figure 2. Tying the data to the structure
From data to stakeholder relevance
Finally, the gap in meaning (relevance) asks if those studies were done with the ‘right’ people. By this, we mean people related to the situation or topic you are studying. Managers, line workers, clients, suppliers, those providing related services; all of those and more should be included. Similarly, you might look to a variety of academic disciplines, drawing expertise from psychology, sociology, business, economics, policy, and others.
Which participants or stakeholders are actually part of your research depends on the project. However, in general, having a broader selection of stakeholder groups results in a better map. This applies to both choosing what concepts go on the map and also who to contact for interviews and surveys.
Visualizing the gaps
All of these three gaps – gaps in structure, data, and stakeholder perspectives – can (and should) be addressed to help you choose more focused directions for your research – to generate research results that will have more impact. As a final note, remember that many gaps may be filled with secondary research; a new literature review that fills the gaps in the logic/structure, data/information, and meaning/relevance of your map so that your organisation can have a greater impact.

Figure 3. Visualizing the gaps (shown in green)
Some deeper reading on literature reviews may be found here:
- Practical Mapping for Applied Research and Program Evaluation (SAGE) provides a ‘jargon free’ explanation for every phase of research:
https://us.sagepub.com/en-us/nam/practical-mapping-for-applied-research-and-program-evaluation/book261152 (especially Chapter 3)
- This paper uses theories for addressing poverty from a range of academic disciplines and from policy centers from across the political spectrum as an example of interdisciplinary knowledge mapping and synthesis:
https://www.emerald.com/insight/content/doi/10.1108/K-03-2018-0136/full/html
- Restructuring evaluation findings into useful knowledge:
http://journals.sfu.ca/jmde/index.php/jmde_1/article/download/481/436/
This approach helps you to avoid fuzzy understandings and the dangerous ‘pretence of knowledge’ that occasionally crops up in some reports and recommendations. Everyone can see that a piece is missing and so more easily agree where more research is needed to advance our knowledge to better serve our organisational and community constituents.
Contribute Write a blog post, post a job or event, recommend a resource
Partner with Us Are you an institution looking to increase your impact?
Most Recent Posts
- Health Adviser – Ethiopia and Nigeria, FCDO – Deadline 29th July
- A guide to research evaluation frameworks
- Enhance Your Evaluation Efforts with Inclusive Communication Strategies
- Six mechanisms to strengthen citizen engagement in public service governance
- Senior Research and Learning Manager: UK Humanitarian Innovation Hub – Deadline 7th July

🌟 This week, #R2ARecommends this webinar on demystifying evaluation practice, produced by the Global Evaluation Initiative. 🌟 🔗Follow the #R2ARecommends link in our linktree to find out more! #Evaluation #Webinar #InclusiveCommunication #GEI #GlobalEval

This week #R2Arecommends this blog from AgileFacil examining the power of the 1-2-4-All structure for facilitation and effective, and inclusive, engagement. Follow the link in our bio to find this and many other recommended wisdom and resources.

"Co-production involves researchers, practitioners and the public working together and sharing power all the way through a research project." This week, #R2AImpactPractitioners spotlights this guide on co-producing a research project from the NIHR (National Institute for Health and Care Research). Follow the link in our Linktree to find this and other resources in the series.
Research To Action (R2A) is a learning platform for anyone interested in maximising the impact of research and capturing evidence of impact.
The site publishes practical resources on a range of topics including research uptake, communications, policy influence and monitoring and evaluation. It captures the experiences of practitioners and researchers working on these topics and facilitates conversations between this global community through a range of social media platforms.
R2A is produced by a small editorial team, led by CommsConsult . We welcome suggestions for and contributions to the site.
Subscribe to our newsletter!
Our contributors
Browse all authors
Friends and partners
- Global Development Network (GDN)
- Institute of Development Studies (IDS)
- International Initiative for Impact Evaluation (3ie)
- On Think Tanks
- Politics & Ideas
- Research for Development (R4D)
- Research Impact

Get science-backed answers as you write with Paperpal's Research feature
What is a Literature Review? How to Write It (with Examples)

A literature review is a critical analysis and synthesis of existing research on a particular topic. It provides an overview of the current state of knowledge, identifies gaps, and highlights key findings in the literature. 1 The purpose of a literature review is to situate your own research within the context of existing scholarship, demonstrating your understanding of the topic and showing how your work contributes to the ongoing conversation in the field. Learning how to write a literature review is a critical tool for successful research. Your ability to summarize and synthesize prior research pertaining to a certain topic demonstrates your grasp on the topic of study, and assists in the learning process.
Table of Contents
- What is the purpose of literature review?
- a. Habitat Loss and Species Extinction:
- b. Range Shifts and Phenological Changes:
- c. Ocean Acidification and Coral Reefs:
- d. Adaptive Strategies and Conservation Efforts:
How to write a good literature review
- Choose a Topic and Define the Research Question:
- Decide on the Scope of Your Review:
- Select Databases for Searches:
- Conduct Searches and Keep Track:
- Review the Literature:
- Organize and Write Your Literature Review:
- How to write a literature review faster with Paperpal?
- Frequently asked questions
What is a literature review?
A well-conducted literature review demonstrates the researcher’s familiarity with the existing literature, establishes the context for their own research, and contributes to scholarly conversations on the topic. One of the purposes of a literature review is also to help researchers avoid duplicating previous work and ensure that their research is informed by and builds upon the existing body of knowledge.

What is the purpose of literature review?
A literature review serves several important purposes within academic and research contexts. Here are some key objectives and functions of a literature review: 2
1. Contextualizing the Research Problem: The literature review provides a background and context for the research problem under investigation. It helps to situate the study within the existing body of knowledge.
2. Identifying Gaps in Knowledge: By identifying gaps, contradictions, or areas requiring further research, the researcher can shape the research question and justify the significance of the study. This is crucial for ensuring that the new research contributes something novel to the field.
Find academic papers related to your research topic faster. Try Research on Paperpal
3. Understanding Theoretical and Conceptual Frameworks: Literature reviews help researchers gain an understanding of the theoretical and conceptual frameworks used in previous studies. This aids in the development of a theoretical framework for the current research.
4. Providing Methodological Insights: Another purpose of literature reviews is that it allows researchers to learn about the methodologies employed in previous studies. This can help in choosing appropriate research methods for the current study and avoiding pitfalls that others may have encountered.
5. Establishing Credibility: A well-conducted literature review demonstrates the researcher’s familiarity with existing scholarship, establishing their credibility and expertise in the field. It also helps in building a solid foundation for the new research.
6. Informing Hypotheses or Research Questions: The literature review guides the formulation of hypotheses or research questions by highlighting relevant findings and areas of uncertainty in existing literature.
Literature review example
Let’s delve deeper with a literature review example: Let’s say your literature review is about the impact of climate change on biodiversity. You might format your literature review into sections such as the effects of climate change on habitat loss and species extinction, phenological changes, and marine biodiversity. Each section would then summarize and analyze relevant studies in those areas, highlighting key findings and identifying gaps in the research. The review would conclude by emphasizing the need for further research on specific aspects of the relationship between climate change and biodiversity. The following literature review template provides a glimpse into the recommended literature review structure and content, demonstrating how research findings are organized around specific themes within a broader topic.
Literature Review on Climate Change Impacts on Biodiversity:
Climate change is a global phenomenon with far-reaching consequences, including significant impacts on biodiversity. This literature review synthesizes key findings from various studies:
a. Habitat Loss and Species Extinction:
Climate change-induced alterations in temperature and precipitation patterns contribute to habitat loss, affecting numerous species (Thomas et al., 2004). The review discusses how these changes increase the risk of extinction, particularly for species with specific habitat requirements.
b. Range Shifts and Phenological Changes:
Observations of range shifts and changes in the timing of biological events (phenology) are documented in response to changing climatic conditions (Parmesan & Yohe, 2003). These shifts affect ecosystems and may lead to mismatches between species and their resources.
c. Ocean Acidification and Coral Reefs:
The review explores the impact of climate change on marine biodiversity, emphasizing ocean acidification’s threat to coral reefs (Hoegh-Guldberg et al., 2007). Changes in pH levels negatively affect coral calcification, disrupting the delicate balance of marine ecosystems.
d. Adaptive Strategies and Conservation Efforts:
Recognizing the urgency of the situation, the literature review discusses various adaptive strategies adopted by species and conservation efforts aimed at mitigating the impacts of climate change on biodiversity (Hannah et al., 2007). It emphasizes the importance of interdisciplinary approaches for effective conservation planning.

Strengthen your literature review with factual insights. Try Research on Paperpal for free!
Writing a literature review involves summarizing and synthesizing existing research on a particular topic. A good literature review format should include the following elements.
Introduction: The introduction sets the stage for your literature review, providing context and introducing the main focus of your review.
- Opening Statement: Begin with a general statement about the broader topic and its significance in the field.
- Scope and Purpose: Clearly define the scope of your literature review. Explain the specific research question or objective you aim to address.
- Organizational Framework: Briefly outline the structure of your literature review, indicating how you will categorize and discuss the existing research.
- Significance of the Study: Highlight why your literature review is important and how it contributes to the understanding of the chosen topic.
- Thesis Statement: Conclude the introduction with a concise thesis statement that outlines the main argument or perspective you will develop in the body of the literature review.
Body: The body of the literature review is where you provide a comprehensive analysis of existing literature, grouping studies based on themes, methodologies, or other relevant criteria.
- Organize by Theme or Concept: Group studies that share common themes, concepts, or methodologies. Discuss each theme or concept in detail, summarizing key findings and identifying gaps or areas of disagreement.
- Critical Analysis: Evaluate the strengths and weaknesses of each study. Discuss the methodologies used, the quality of evidence, and the overall contribution of each work to the understanding of the topic.
- Synthesis of Findings: Synthesize the information from different studies to highlight trends, patterns, or areas of consensus in the literature.
- Identification of Gaps: Discuss any gaps or limitations in the existing research and explain how your review contributes to filling these gaps.
- Transition between Sections: Provide smooth transitions between different themes or concepts to maintain the flow of your literature review.
Write and Cite as you go with Paperpal Research. Start now for free.
Conclusion: The conclusion of your literature review should summarize the main findings, highlight the contributions of the review, and suggest avenues for future research.
- Summary of Key Findings: Recap the main findings from the literature and restate how they contribute to your research question or objective.
- Contributions to the Field: Discuss the overall contribution of your literature review to the existing knowledge in the field.
- Implications and Applications: Explore the practical implications of the findings and suggest how they might impact future research or practice.
- Recommendations for Future Research: Identify areas that require further investigation and propose potential directions for future research in the field.
- Final Thoughts: Conclude with a final reflection on the importance of your literature review and its relevance to the broader academic community.

Conducting a literature review
Conducting a literature review is an essential step in research that involves reviewing and analyzing existing literature on a specific topic. It’s important to know how to do a literature review effectively, so here are the steps to follow: 1
Choose a Topic and Define the Research Question:
- Select a topic that is relevant to your field of study.
- Clearly define your research question or objective. Determine what specific aspect of the topic do you want to explore?
Decide on the Scope of Your Review:
- Determine the timeframe for your literature review. Are you focusing on recent developments, or do you want a historical overview?
- Consider the geographical scope. Is your review global, or are you focusing on a specific region?
- Define the inclusion and exclusion criteria. What types of sources will you include? Are there specific types of studies or publications you will exclude?
Select Databases for Searches:
- Identify relevant databases for your field. Examples include PubMed, IEEE Xplore, Scopus, Web of Science, and Google Scholar.
- Consider searching in library catalogs, institutional repositories, and specialized databases related to your topic.
Conduct Searches and Keep Track:
- Develop a systematic search strategy using keywords, Boolean operators (AND, OR, NOT), and other search techniques.
- Record and document your search strategy for transparency and replicability.
- Keep track of the articles, including publication details, abstracts, and links. Use citation management tools like EndNote, Zotero, or Mendeley to organize your references.
Review the Literature:
- Evaluate the relevance and quality of each source. Consider the methodology, sample size, and results of studies.
- Organize the literature by themes or key concepts. Identify patterns, trends, and gaps in the existing research.
- Summarize key findings and arguments from each source. Compare and contrast different perspectives.
- Identify areas where there is a consensus in the literature and where there are conflicting opinions.
- Provide critical analysis and synthesis of the literature. What are the strengths and weaknesses of existing research?
Organize and Write Your Literature Review:
- Literature review outline should be based on themes, chronological order, or methodological approaches.
- Write a clear and coherent narrative that synthesizes the information gathered.
- Use proper citations for each source and ensure consistency in your citation style (APA, MLA, Chicago, etc.).
- Conclude your literature review by summarizing key findings, identifying gaps, and suggesting areas for future research.
Whether you’re exploring a new research field or finding new angles to develop an existing topic, sifting through hundreds of papers can take more time than you have to spare. But what if you could find science-backed insights with verified citations in seconds? That’s the power of Paperpal’s new Research feature!
How to write a literature review faster with Paperpal?
Paperpal, an AI writing assistant, integrates powerful academic search capabilities within its writing platform. With the Research feature, you get 100% factual insights, with citations backed by 250M+ verified research articles, directly within your writing interface with the option to save relevant references in your Citation Library. By eliminating the need to switch tabs to find answers to all your research questions, Paperpal saves time and helps you stay focused on your writing.
Here’s how to use the Research feature:
- Ask a question: Get started with a new document on paperpal.com. Click on the “Research” feature and type your question in plain English. Paperpal will scour over 250 million research articles, including conference papers and preprints, to provide you with accurate insights and citations.
- Review and Save: Paperpal summarizes the information, while citing sources and listing relevant reads. You can quickly scan the results to identify relevant references and save these directly to your built-in citations library for later access.
- Cite with Confidence: Paperpal makes it easy to incorporate relevant citations and references into your writing, ensuring your arguments are well-supported by credible sources. This translates to a polished, well-researched literature review.
The literature review sample and detailed advice on writing and conducting a review will help you produce a well-structured report. But remember that a good literature review is an ongoing process, and it may be necessary to revisit and update it as your research progresses. By combining effortless research with an easy citation process, Paperpal Research streamlines the literature review process and empowers you to write faster and with more confidence. Try Paperpal Research now and see for yourself.
Frequently asked questions
A literature review is a critical and comprehensive analysis of existing literature (published and unpublished works) on a specific topic or research question and provides a synthesis of the current state of knowledge in a particular field. A well-conducted literature review is crucial for researchers to build upon existing knowledge, avoid duplication of efforts, and contribute to the advancement of their field. It also helps researchers situate their work within a broader context and facilitates the development of a sound theoretical and conceptual framework for their studies.
Literature review is a crucial component of research writing, providing a solid background for a research paper’s investigation. The aim is to keep professionals up to date by providing an understanding of ongoing developments within a specific field, including research methods, and experimental techniques used in that field, and present that knowledge in the form of a written report. Also, the depth and breadth of the literature review emphasizes the credibility of the scholar in his or her field.
Before writing a literature review, it’s essential to undertake several preparatory steps to ensure that your review is well-researched, organized, and focused. This includes choosing a topic of general interest to you and doing exploratory research on that topic, writing an annotated bibliography, and noting major points, especially those that relate to the position you have taken on the topic.
Literature reviews and academic research papers are essential components of scholarly work but serve different purposes within the academic realm. 3 A literature review aims to provide a foundation for understanding the current state of research on a particular topic, identify gaps or controversies, and lay the groundwork for future research. Therefore, it draws heavily from existing academic sources, including books, journal articles, and other scholarly publications. In contrast, an academic research paper aims to present new knowledge, contribute to the academic discourse, and advance the understanding of a specific research question. Therefore, it involves a mix of existing literature (in the introduction and literature review sections) and original data or findings obtained through research methods.
Literature reviews are essential components of academic and research papers, and various strategies can be employed to conduct them effectively. If you want to know how to write a literature review for a research paper, here are four common approaches that are often used by researchers. Chronological Review: This strategy involves organizing the literature based on the chronological order of publication. It helps to trace the development of a topic over time, showing how ideas, theories, and research have evolved. Thematic Review: Thematic reviews focus on identifying and analyzing themes or topics that cut across different studies. Instead of organizing the literature chronologically, it is grouped by key themes or concepts, allowing for a comprehensive exploration of various aspects of the topic. Methodological Review: This strategy involves organizing the literature based on the research methods employed in different studies. It helps to highlight the strengths and weaknesses of various methodologies and allows the reader to evaluate the reliability and validity of the research findings. Theoretical Review: A theoretical review examines the literature based on the theoretical frameworks used in different studies. This approach helps to identify the key theories that have been applied to the topic and assess their contributions to the understanding of the subject. It’s important to note that these strategies are not mutually exclusive, and a literature review may combine elements of more than one approach. The choice of strategy depends on the research question, the nature of the literature available, and the goals of the review. Additionally, other strategies, such as integrative reviews or systematic reviews, may be employed depending on the specific requirements of the research.
The literature review format can vary depending on the specific publication guidelines. However, there are some common elements and structures that are often followed. Here is a general guideline for the format of a literature review: Introduction: Provide an overview of the topic. Define the scope and purpose of the literature review. State the research question or objective. Body: Organize the literature by themes, concepts, or chronology. Critically analyze and evaluate each source. Discuss the strengths and weaknesses of the studies. Highlight any methodological limitations or biases. Identify patterns, connections, or contradictions in the existing research. Conclusion: Summarize the key points discussed in the literature review. Highlight the research gap. Address the research question or objective stated in the introduction. Highlight the contributions of the review and suggest directions for future research.
Both annotated bibliographies and literature reviews involve the examination of scholarly sources. While annotated bibliographies focus on individual sources with brief annotations, literature reviews provide a more in-depth, integrated, and comprehensive analysis of existing literature on a specific topic. The key differences are as follows:
| Annotated Bibliography | Literature Review | |
| Purpose | List of citations of books, articles, and other sources with a brief description (annotation) of each source. | Comprehensive and critical analysis of existing literature on a specific topic. |
| Focus | Summary and evaluation of each source, including its relevance, methodology, and key findings. | Provides an overview of the current state of knowledge on a particular subject and identifies gaps, trends, and patterns in existing literature. |
| Structure | Each citation is followed by a concise paragraph (annotation) that describes the source’s content, methodology, and its contribution to the topic. | The literature review is organized thematically or chronologically and involves a synthesis of the findings from different sources to build a narrative or argument. |
| Length | Typically 100-200 words | Length of literature review ranges from a few pages to several chapters |
| Independence | Each source is treated separately, with less emphasis on synthesizing the information across sources. | The writer synthesizes information from multiple sources to present a cohesive overview of the topic. |
References
- Denney, A. S., & Tewksbury, R. (2013). How to write a literature review. Journal of criminal justice education , 24 (2), 218-234.
- Pan, M. L. (2016). Preparing literature reviews: Qualitative and quantitative approaches . Taylor & Francis.
- Cantero, C. (2019). How to write a literature review. San José State University Writing Center .
Paperpal is an AI writing assistant that help academics write better, faster with real-time suggestions for in-depth language and grammar correction. Trained on millions of research manuscripts enhanced by professional academic editors, Paperpal delivers human precision at machine speed.
Try it for free or upgrade to Paperpal Prime , which unlocks unlimited access to premium features like academic translation, paraphrasing, contextual synonyms, consistency checks and more. It’s like always having a professional academic editor by your side! Go beyond limitations and experience the future of academic writing. Get Paperpal Prime now at just US$19 a month!
Related Reads:
- Empirical Research: A Comprehensive Guide for Academics
- How to Write a Scientific Paper in 10 Steps
- How Long Should a Chapter Be?
- How to Use Paperpal to Generate Emails & Cover Letters?
6 Tips for Post-Doc Researchers to Take Their Career to the Next Level
Self-plagiarism in research: what it is and how to avoid it, you may also like, five things authors need to know when using..., 7 best referencing tools and citation management software..., maintaining academic integrity with paperpal’s generative ai writing..., research funding basics: what should a grant proposal..., how to write an abstract in research papers..., how to write dissertation acknowledgements, how to structure an essay, leveraging generative ai to enhance student understanding of..., what’s the best chatgpt alternative for academic writing, how to write a good hook for essays,....
Harvey Cushing/John Hay Whitney Medical Library
- Collections
- Research Help
YSN Doctoral Programs: Steps in Conducting a Literature Review
- Biomedical Databases
- Global (Public Health) Databases
- Soc. Sci., History, and Law Databases
- Grey Literature
- Trials Registers
- Data and Statistics
- Public Policy
- Google Tips
- Recommended Books
- Steps in Conducting a Literature Review
What is a literature review?
A literature review is an integrated analysis -- not just a summary-- of scholarly writings and other relevant evidence related directly to your research question. That is, it represents a synthesis of the evidence that provides background information on your topic and shows a association between the evidence and your research question.
A literature review may be a stand alone work or the introduction to a larger research paper, depending on the assignment. Rely heavily on the guidelines your instructor has given you.
Why is it important?
A literature review is important because it:
- Explains the background of research on a topic.
- Demonstrates why a topic is significant to a subject area.
- Discovers relationships between research studies/ideas.
- Identifies major themes, concepts, and researchers on a topic.
- Identifies critical gaps and points of disagreement.
- Discusses further research questions that logically come out of the previous studies.
APA7 Style resources
APA Style Blog - for those harder to find answers
1. Choose a topic. Define your research question.
Your literature review should be guided by your central research question. The literature represents background and research developments related to a specific research question, interpreted and analyzed by you in a synthesized way.
- Make sure your research question is not too broad or too narrow. Is it manageable?
- Begin writing down terms that are related to your question. These will be useful for searches later.
- If you have the opportunity, discuss your topic with your professor and your class mates.
2. Decide on the scope of your review
How many studies do you need to look at? How comprehensive should it be? How many years should it cover?
- This may depend on your assignment. How many sources does the assignment require?
3. Select the databases you will use to conduct your searches.
Make a list of the databases you will search.
Where to find databases:
- use the tabs on this guide
- Find other databases in the Nursing Information Resources web page
- More on the Medical Library web page
- ... and more on the Yale University Library web page
4. Conduct your searches to find the evidence. Keep track of your searches.
- Use the key words in your question, as well as synonyms for those words, as terms in your search. Use the database tutorials for help.
- Save the searches in the databases. This saves time when you want to redo, or modify, the searches. It is also helpful to use as a guide is the searches are not finding any useful results.
- Review the abstracts of research studies carefully. This will save you time.
- Use the bibliographies and references of research studies you find to locate others.
- Check with your professor, or a subject expert in the field, if you are missing any key works in the field.
- Ask your librarian for help at any time.
- Use a citation manager, such as EndNote as the repository for your citations. See the EndNote tutorials for help.

Review the literature
Some questions to help you analyze the research:
- What was the research question of the study you are reviewing? What were the authors trying to discover?
- Was the research funded by a source that could influence the findings?
- What were the research methodologies? Analyze its literature review, the samples and variables used, the results, and the conclusions.
- Does the research seem to be complete? Could it have been conducted more soundly? What further questions does it raise?
- If there are conflicting studies, why do you think that is?
- How are the authors viewed in the field? Has this study been cited? If so, how has it been analyzed?
Tips:
- Review the abstracts carefully.
- Keep careful notes so that you may track your thought processes during the research process.
- Create a matrix of the studies for easy analysis, and synthesis, across all of the studies.
- << Previous: Recommended Books
- Last Updated: Jun 20, 2024 9:08 AM
- URL: https://guides.library.yale.edu/YSNDoctoral
- Library databases
- Library website
Library Guide to Capstone Literature Reviews: Find a Research Gap
Find a research gap: tips to get started.
Finding a research gap is not an easy process and there is no one linear path. These tips and suggestions are just examples of possible ways to begin.
In Ph.D. dissertations, students identify a gap in research. In other programs, students identify a gap in practice. The literature review for a gap in practice will show the context of the problem and the current state of the research.
Research gap definition
A research gap exists when:
- a question or problem has not been answered by existing studies/research in the field
- a concept or new idea has not been studied at all
- all the existing literature on a topic is outdated
- a specific population/location/age group etc has not been studied
A research gap should be:
- grounded in the literature
- amenable to scientific study
- Litmus Test for a Doctoral-Level Research Problem (Word) This tool helps students determine if they have identified a doctoral level research problem.
Identify a research gap
To find a gap you must become very familiar with a particular field of study. This will involve a lot of research and reading, because a gap is defined by what does (and does not) surround it.
- Search the research literature and dissertations (search all university dissertations, not just Walden!).
- Understand your topic! Review background information in books and encyclopedias .
- Look for literature reviews, systematic reviews, and meta-analyses.
- Take notes on concepts, themes, and subject terms .
- Look closely at each article's limitations, conclusions, and recommendations for future research.
- Organize, analyze, and repeat!
- Quick Answer: How do I find dissertations on a topic?
Start with broad searches
Use the Library Search (formerly Thoreau) to do a broad search with just one concept at a time . Broad searches give you an idea of the academic conversation surrounding your topic.
- Try the terms you know (keywords) first.
- Look at the Subject Terms (controlled language) to brainstorm terms.
- Subject terms help you understand what terms are most used, and what other terms to try.
- No matter what your topic is, not every researcher will be using the same terms. Keep an eye open for additional ways to describe your topic.
- Guide: Subject Terms & Index Searches: Index Overview
Keep a list of terms
- Create a list of terms
- Example list of terms
This list will be a record of what terms are:
- related to or represent your topic
- synonyms or antonyms
- more or less commonly used
- keywords (natural language) or subject terms (controlled language)
- Synonyms & antonyms (database search skills)
- Turn keywords into subject terms
Term I started with:
culturally aware
Subject terms I discovered:
cultural awareness (SU)
cultural sensitivity (SU)
cultural competence (SU)
Search with different combinations of terms
- Combine search terms list
- Combine search terms table
- Video: Search by Themes
Since a research gap is defined by the absence of research on a topic, you will search for articles on everything that relates to your topic.
- List out all the themes related to your gap.
- Search different combinations of the themes as you discover them
For example, suppose your research gap is on the work-life balance of tenured and tenure-track women in engineering professions. In that case, you might try searching different combinations of concepts, such as:
- women and STEM
- STEM or science or technology or engineering or mathematics
- female engineering professors
- tenure-track women in STEM
- work-life balance and women in STEM
- work-life balance and women professors
- work-life balance and tenure
Topic adapted from one of the award winning Walden dissertations.
- Walden University Award Winning Dissertations
- Gossage, Lily Giang-Tien, "Work-Life Balance of Tenured and Tenure-Track Women Engineering Professors" (2019). Walden Dissertations and Doctoral Studies. 6435.
Break your topic into themes and try combining the terms from different themes in different ways. For example:
Theme 1 and Theme 4
Theme 2 and Theme 1
Theme 3 and Theme 4
| Theme 1 and related terms | Theme 2 and related terms | Theme 3 and related terms | Theme 4 and related terms | Theme 5 and related terms |
|---|---|---|---|---|
| women | STEM | tenure track | work life balance | professor |
| female | science or technology or engineer or mathematics | tenured | work-life-balance | faculty |
Video: Search by Themes (YouTube)
(2 min 40 sec) Recorded April 2014 Transcript
Track where more research is needed
Most research articles will identify where more research is needed. To identify research trends, use the literature review matrix to track where further research is needed.
- Download or create your own Literature Review Matrix (examples in links below).
- Do some general database searches on broad topics.
- Find an article that looks interesting.
- When you read the article, pay attention to the conclusions and limitations sections.
- Use the Literature Review Matrix to track where 'more research is needed' or 'further research needed'. NOTE: you might need to add a column to the template.
- As you fill in the matrix you should see trends where more research is needed.
There is no consistent section in research articles where the authors identify where more research is needed. Pay attention to these sections:
- limitations
- conclusions
- recommendations for future research
- Literature Review Matrix Templates: learn how to keep a record of what you have read
- Literature Review Matrix (Excel) with color coding Sample template for organizing and synthesizing your research
- Previous Page: Scope
- Next Page: Get & Stay Organized
- Office of Student Disability Services
Walden Resources
Departments.
- Academic Residencies
- Academic Skills
- Career Planning and Development
- Customer Care Team
- Field Experience
- Military Services
- Student Success Advising
- Writing Skills
Centers and Offices
- Center for Social Change
- Office of Academic Support and Instructional Services
- Office of Degree Acceleration
- Office of Research and Doctoral Services
- Office of Student Affairs
Student Resources
- Doctoral Writing Assessment
- Form & Style Review
- Quick Answers
- ScholarWorks
- SKIL Courses and Workshops
- Walden Bookstore
- Walden Catalog & Student Handbook
- Student Safety/Title IX
- Legal & Consumer Information
- Website Terms and Conditions
- Cookie Policy
- Accessibility
- Accreditation
- State Authorization
- Net Price Calculator
- Contact Walden
Walden University is a member of Adtalem Global Education, Inc. www.adtalem.com Walden University is certified to operate by SCHEV © 2024 Walden University LLC. All rights reserved.

UNE Library Services
Research Help
Gaps in the literature.
Gaps in the literature are missing pieces or insufficient information in the published research on a topic. These are areas that have opportunities for further research because they are unexplored, under-explored, or outdated.
Finding Gaps
Gaps can be missing or incomplete:
- Population or sample: size, type, location etc…
- Research methods: qualitative, quantitative, or mixed
- Data collection or analysis
- Research variables or conditions
Conduct a thorough literature search to find a broad range of research articles on your topic. Search research databases ; you can find recommended databases for your subject area in research by subject for your course or program.
Identifying Gaps
If you do not find articles in your literature search, this may indicate a gap.
If you do find articles, the goal is to find a gap for contributing new research. Authors signal that there is a gap using phrases such as:
- Has not been clarified, studied, reported, or elucidated
- Further research is required or needed
- Is not well reported
- Suggestions for further research
- Key question is or remains
- It is important to address
- Poorly understood or known
- Lack of studies
- These findings provide valuable insights into the potential benefits of mindfulness-based interventions for stress management,however, further study is needed to address several limitations and extend our understanding in this area .
- While this study provides preliminary evidence of the potential efficacy of VRET in reducing PTSD symptoms, several aspects related to its implementation and specific treatment outcomes remain inadequately clarified, highlighting the need for further research .
- Although the studies reviewed provide valuable insights into the potential effects of climate change on species composition and ecosystem functioning. The question of how climate change will interact with other anthropogenic stressors to influence the resilience and adaptive capacity of tropical rainforest ecosystems remains unanswered, highlighting the need for further research .
Questions & Help
If you have questions on this, or another, topic, contact a librarian for help!

- Classification
- Physical Education
- Travel and Tourism
- BIBLIOMETRICS
- Banking System
- Real Estate
Select Page
Types of Research Gaps in Literature Review | How to Find a Research Gap
Posted by Md. Harun Ar Rashid | Nov 30, 2022 | Research Methodology
A research gap ( which indicates a lack of prior research on a topic ) is essentially an unanswered question or unsolved issue in a certain discipline. Alternatively, when there is a good number of studies conducted but the findings reflect in multiple ways, making it difficult to draw solid conclusions, there may be a research gap. Let’s take an example; where the goal of your study is to determine the cause (or causes) of a specific disease. In the literature, there is evidence to suggest that smoking is a major contributing factor, but there is also a substantial body of data that shows no connection between smoking and the disease. In that scenario, you may find a research gap that needs further investigation. In the rest of this article, we are going to know about the different types of research gaps in literature review and how to find a research gap .
Definition of Research Gap:
A research gap is essentially an unanswered question or unresolved problem in a field, reflecting a lack of existing research ( Grad Coach ).
A research gap is a key problem or a question that has not been answered by any of the existing studies within your area of research ( Dr. Sowndarya Somasundaram ).
From the above definitions, we can say that a research gap is a topic or area where there is a lack of information or insufficient data that prevents reviewers to grasp a conclusion regarding a particular question.
Types of Research Gaps in Literature Review:
According to (Robinson, et al., (2011), Muller-Bloch, & Kranz (2015), and Miles (2017); the research gap can be classified into seven categories which are briefly being:
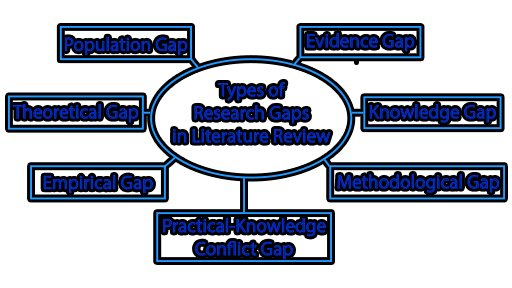
1. Evidence Gap: An evidence gap occurs with a provocative exception arising if a new research finding contradicts widely accepted conclusions. This gap involves contradictions in the findings of the prior research. It occurs if results from studies allow for conclusions in their own right, but are contradictory when examined from a more abstract point of view. The identification of contradictory evidence starts with analyzing each research stream. Subsequently, the results from these analyses need to be synthesized in order to reveal contradictory evidence.
2. Knowledge Gap: The knowledge gap is a common gap in prior research. There are two settings where a knowledge gap (knowledge void) might occur. First, knowledge may not exist in the actual field of theories and literature from related research domains. Second, it might be the case that the results of a study differ from what was expected.
3. Practical-Knowledge Conflict Gap: This kind of gap tends to be a discrepancy that can motivate new research in this direction. A practical–knowledge (action-knowledge) conflict arises when the actual behavior of professionals is different from their advocated behavior. In this case, the research could seek to determine the scope of the conflict and uncover the reasons for its existence.
4. Methodological Gap: A methodological gap is the type of gap that deals with the conflict that occurs due to the influence of methodology on research results. This gap addresses the conflicts with the research methods in the prior studies and offers a new line of research that is divergent from those research methods. It is noted that it might be useful to various research methods, especially if certain research topics have been mainly explored using a singular or common method.
5. Empirical Gap: An empirical gap is the type of gap that deals with gaps in prior research. This conflict deals with the research findings or propositions that need to be evaluated or empirically verified. For example, the empirical gap often addresses conflicts that no study to date has directly attempted to evaluate a subject or topic from an empirical approach.
6. Theoretical Gap: The theoretical gap is the type of gap that deals with the gaps in theory with prior research. For example, if one phenomenon is being explained through various theoretical models, similar to a methodological gap conflict, there might be a theoretical conflict. Researchers and scholars could examine whether one of those theories is superior in terms of the gap in the prior research. Theoretical gaps are a common occurrence in examining prior research on a phenomenon.
7. Population Gap: A population gap is a common gap recognized among researchers. There are always under-served populations that have been under-researched. This gap is the type of research regarding the population that is not adequately represented or under-researched in the evidence base or prior research (e.g., gender, race/ethnicity, age, etc).
How to Find a Research Gap:
Start with a broad topic related to your field of interest: A broad topic allows you more opportunities to find a research gap. Pick a topic that interests you and that you already know something about. As you learn more about your topic, you can narrow it down further to help you find your focus.
Conduct preliminary research to explore your topic: Begin with a simple online search to learn the basics of a topic. Read encyclopedia entries, journal articles, and recent news articles related to your topic. Then, search online databases for peer-reviewed journal articles related to your topic of study.
Compile a wide range of articles about your topic: Search for different types of articles, like informative texts, research texts, and meta-analyses. This will provide you with a broader understanding of your topic so you can more easily find a gap.
Once you’ve gathered a meaty collection of resources, the section that you really want to focus on is the one titled “further research opportunities” or “further research is needed”. In this section, the researchers will explicitly state where more studies are required – in other words, where potential research gaps may exist. You can also look at the “limitations” section of the studies, as this will often spur ideas for methodology-based research gaps.
By following this process, you’ll orient yourself with the current state of research, which will lay the foundation for you to identify potential research gaps. You can then start drawing up a shortlist of ideas and evaluating them as candidate topics. But remember, make sure you’re looking at recent articles – there’s no use going down a rabbit hole only to find that someone’s already filled the gap.
References:
- Miles, D.A. (2017). A Taxonomy of Research Gaps: Identifying and Defining the Seven Research Gaps, Doctoral Student Workshop: Finding Research Gaps – Research Methods and Strategies, Dallas, Texas, 2017.
- Müller-Bloch, C. & Kranz, J., (2014). A Framework for Rigorously Identifying Research Gaps in Qualitative Literature Reviews, The Thirty Sixth International Conference on Information Systems, Fort Worth 2015 , pp. 1–19.
- Robinson, K., Saldanha, I. & McKoy, N.A. (2011). Development of A Framework for to Identify Research Gaps Systematic Reviews, Journal of Epidemiology , 64(1), pp. 1325-1330.

Former Student at Rajshahi University
About The Author

Md. Harun Ar Rashid
Related posts.
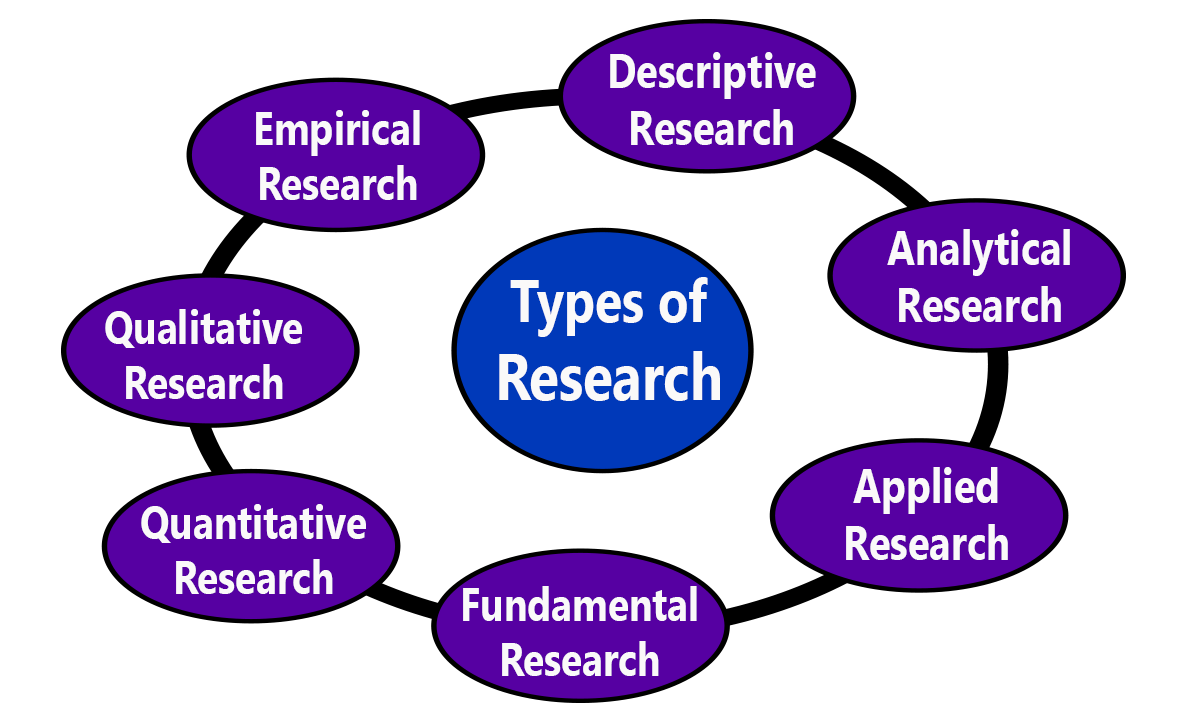
Research | Objectives of Research | Types of Research | Characteristics of Research
August 2, 2019

The Art of Descriptive Writing: Purpose, Techniques, Types, and Tips
February 1, 2024
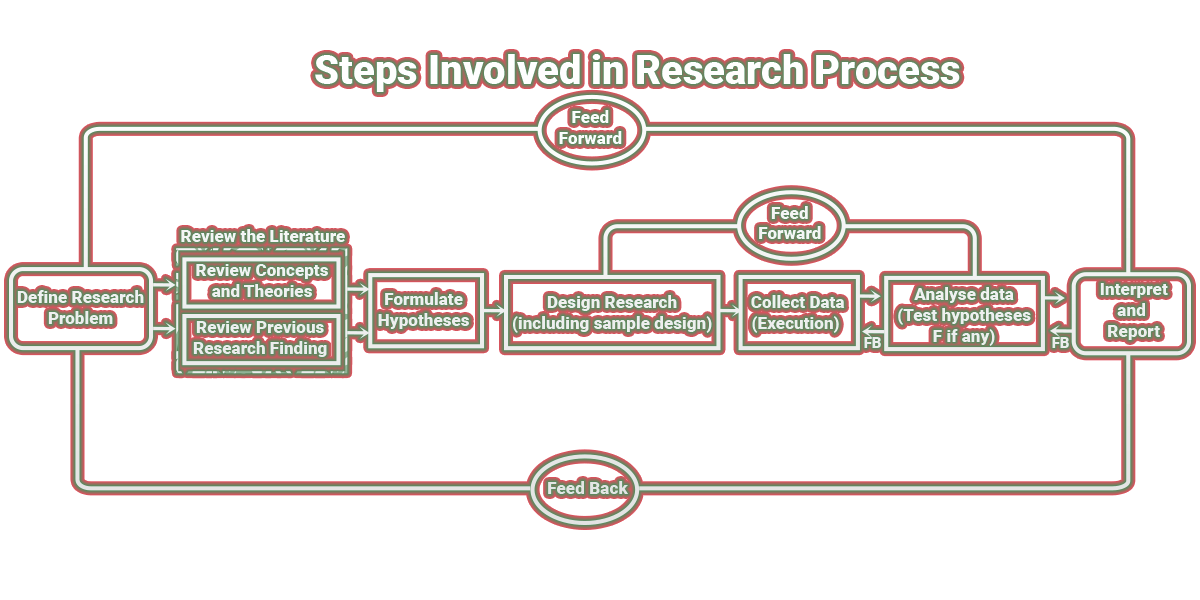
Steps Involved in Research Process
July 6, 2020

A Guide for Conducting Academic Research Using the Internet
January 10, 2024
Follow us on Facebook
Library & Information Management Community
Recent Posts

| M | T | W | T | F | S | S |
|---|---|---|---|---|---|---|
| 1 | 2 | 3 | 4 | 5 | 6 | 7 |
| 8 | 9 | 10 | 11 | 12 | 13 | 14 |
| 15 | 16 | 17 | 18 | 19 | 20 | 21 |
| 22 | 23 | 24 | 25 | 26 | 27 | 28 |
| 29 | 30 | 31 | ||||
Pin It on Pinterest
- LiveJournal
Academia.edu no longer supports Internet Explorer.
To browse Academia.edu and the wider internet faster and more securely, please take a few seconds to upgrade your browser .
Enter the email address you signed up with and we'll email you a reset link.
- We're Hiring!
- Help Center

Gap Analysis for Literature Reviews and Advancing Useful Knowledge

2020, Research to Action: The Global Guide to Research Impact
The basics of research are seemingly clear. Read a lot of articles, see what’s missing, and conduct research to fill the gap in the literature. Wait a minute. What is that? “See what’s missing?” How can we see something that is not there? In this post, we will show you how to “see the invisible;” How to identify the missing pieces in any study, literature review, or program analysis. With these straight-forward techniques, you will be able to better target your research in a more cost-effective way to fill those knowledge gaps to develop more effective theories, plans, and evaluations.
Related Papers
ISSAH BAAKO
Various researchers have established the need for researchers to position their research problem in the research gap of the study area. This does not only indicate the relevance of the study but it demonstrates the significant contribution it would make in the field of study. The purpose of this paper is to conduct a systematic literature review on the concept of research gaps and provoke a discussion on the contemporary literature on types of research gaps. The paper discusses the various approaches for researchers to identify, align and position research problems, research design, and methodology in the research gaps to achieve relevance in their findings and study. A systematic review of the current literature on research gaps might assist beginning researchers in the justification of research problems. Given the acceptable tenet of developing a research agenda, design, and development on a research gap, many early career researchers especially (post)graduate students have difficulties in systematically identifying research gaps as a basis for conducting research work. The significance of this paper is twofold. First, it provides a systematic review of literature on the identification of research gaps to undertake research that would challenge assumptions and underlying existing theories in a significant way. Second, it provides a theoretical discussion on the importance of developing research problems on research gaps to structure their study.
Journal of Research Methods and Strategies
D. Anthony Miles
One of the most prevailing issues in the craft of research is to develop a research agenda and build the research on the development of the research gap. Most research of any endeavor is attributed to the development of the research gap, which is a primary basis in the investigation of any problem, phenomenon or scientific question. Given this accepted tenet of engagement in research, surprising in the research fraternity, we do not train researchers on how to systematically identify research gaps as basis for the investigation. This is has continued to be a common problem with novice researchers. Unfailingly, very little theory and research has been developed on identifying research gaps as a basis for a line in inquiry. The purpose of this research is threefold. First, the proposed theoretical framework builds on the five-point theoretical model of Robinson, Saldanhea, and McKoy (2011) on research gaps. Second, this study builds on the six-point theoretical model of Müller-Bloch and Franz (2014) on research gaps. Lastly, the purpose of this research is to develop and propose a theoretical model that is an amalgamation of the two preceding models and re-conceptualizes the research gap concepts and their characteristics. Thus, this researcher proposes a seven-point theoretical model. This article discusses the characteristics of each research and the situation in which its application is warranted in the literature review The significance of this article is twofold. First, this research provides theoretical significance by developing a theoretical model on research gaps. Second, this research attempts to build a solid taxonomy on the different characteristics of research gaps and establish a foundation. The implication for researchers is that research gaps should be structured and characterized based on their functionality. Thus, this provides researchers with a basic framework for identifying them in the literature investigation.
Kayode Oyediran
Problem in a research as well as human body calls for perfect diagnosis of illness. This is important to avoid treating the symptoms instead of the actual disease. A research problem could be identified through professional or/and academic efforts. This poses a lot of problems to students, both at the undergraduate and postgraduate levels, as this determines the title of their articles or research works. Many of them have to submit many topics to their supervisors before one could be reframed and approved. At times, students appealed to their supervisors to provide them with researchable topics. This to the supervisor(s) almost writing the dissertations/theses for them. The argument of this paper is to let students understand "problem identification" using an analogy from the Holy Bible. The study employed a conversation analysis methodology, which is empirically grounded, exploratory in process and inferential. This involves using every conversation between two or more parties to explore facts/lesson. It was recommended that seasoned lecturers should explain to students how to identify research problems using what are familiar to them to make them understand this important aspect of research.
Omini Akpang
Publications
Cherley C Du Plessis
The ability to conduct an explicit and robust literature review by students, scholars or scientists is critical in producing excellent journal articles, academic theses, academic dissertations or working papers. A literature review is an evaluation of existing research works on a specific academic topic, theme or subject to identify gaps and propose future research agenda. Many postgraduate students in higher education institutions lack the necessary skills and understanding to conduct in-depth literature reviews. This may lead to the presentation of incorrect, false or biased inferences in their theses or dissertations. This study offers scientific knowledge on how literature reviews in different fields of study could be conducted to mitigate against biased inferences such as unscientific analogies and baseless recommendations. The literature review is presented as a process that involves several activities including searching, identifying, reading, summarising, compiling, analysing, interpreting and referencing. We hope this article serves as reference material to improve the academic rigour in the literature review chapters of postgraduate students' theses or dissertations. This article prompts established scholars to explore more innovative ways through which scientific literature reviews can be conducted to identify gaps (empirical, knowledge, theoretical, methodological, application and population gap) and propose a future research agenda.
Management Information Systems Quarterly
Richard Watson
Journal of General Internal Medicine
Susanne Hempel
BACKGROUND: Well-defined, systematic, and transparent processes to identify health research gaps, needs, and priorities are vital to ensuring that available funds target areas with the greatest potential for impact. OBJECTIVE: The purpose of this review is to characterize methods conducted or supported by research funding organizations to identify health research gaps, needs, or priorities. METHOD: We searched MEDLINE, PsycINFO, and the Web of Science up to September 2019. Eligible studies reported on methods to identify health research gaps, needs, and priorities that had been conducted or supported by research funding organizations. Using a published protocol, we extracted data on the method, criteria, involvement of stakeholders, evaluations, and whether the method had been replicated (i.e., used in other studies). RESULTS: Among 10,832 citations, 167 studies were eligible for full data extraction. More than half of the studies employed methods to identify both needs and priorities, whereas about a quarter of studies focused singularly on identifying gaps (7%), needs (6%), or priorities (14%) only. The most frequently used methods were the convening of workshops or meetings (37%), quantitative methods (32%), and the James Lind Alliance approach, a multistakeholder research needs and priority setting process (28%). The most widely applied criteria were importance to stakeholders (72%), potential value (29%), and feasibility (18%). Stakeholder involvement was most prominent among clinicians (69%), researchers (66%), and patients and the public (59%). Stakeholders were identified through stakeholder organizations (51%) and purposive (26%) and convenience sampling (11%). Only 4% of studies evaluated the effectiveness of the methods and 37% employed methods that were reproducible and used in other studies. DISCUSSION: To ensure optimal targeting of funds to meet the greatest areas of need and maximize outcomes, a much more robust evidence base is needed to ascertain the effectiveness of methods used to identify research gaps, needs, and priorities.
UNICAF University - Zambia
Ivan Steenkamp
This section contains the four Thematic Gap Analyses and the Cross-Cutting Gap Analysis. Each of the chapters has a lead author (s) as noted on the front page of the chapter. This follows the way that the team has divided-up the responsibilities for each Thematic Area, with a disciplinary specialist (s) taking the lead on each area. The chapters have, however, been reviewed and commented by others in the project team so the analysis and suggested actions and conclusions have the general support of the full project team.
Loading Preview
Sorry, preview is currently unavailable. You can download the paper by clicking the button above.
RELATED PAPERS
Aare 2004 Doing the Public Good Positioning Educational Research International Education Research Conference Proceedings
Pat Thomson
Charles Turkelson
Rebekka Tunombili
International Journal of P R O F E S S I O N A L Business Review
Journal of Practical Studies in Education
Jenine Beekhuyzen
Notchie Angeles
Sid Ahmed KHETTAB
Global Journal of Artificial Intelligence
Oluwatobi Balogun
The Qualitative Report
Janeen T Lamb
Auxiliadora Padilha
Amanda Bolderston
Quality & Quantity, 47, 3249-3259
Raewyn Bassett
European, Mediterranean, and Middle Eastern Conference on Information Systems
Smaa Elnagar
David Nicholas
Tatam Chiway , Abdullah Ramdhani , Muhammad Ali Ramdhani
International Journal on Studies in English Language and Literature
JOSEPHINE DANIELS
David W Armstrong
Frances Slack
Journal of Asian Development
SANIAGO DAKHI
RELATED TOPICS
- We're Hiring!
- Help Center
- Find new research papers in:
- Health Sciences
- Earth Sciences
- Cognitive Science
- Mathematics
- Computer Science
- Academia ©2024
- Study Protocol
- Open access
- Published: 04 July 2024
Adherence to single inhaler triple therapy and digital inhalers in Chronic Obstructive Pulmonary Disease: a literature review and protocol for a randomized controlled trial (TRICOLON study)
- Liz J. A. Cuperus 1 , 2 , 3 ,
- Job van der Palen 4 ,
- Arnoud Aldenkamp 5 ,
- Astrid van Huisstede 6 ,
- Erik W. M. A. Bischoff 7 ,
- Job F. M. van Boven 8 ,
- Folkert Brijker 9 ,
- Stephan Dik 10 ,
- Jeroen A. J. M. van Excel 11 ,
- Martijn Goosens 12 ,
- Peter Th. W. van Hal 13 ,
- Jolanda C. Kuijvenhoven 14 ,
- Lisette I. Z. Kunz 15 ,
- Erwin C. Vasbinder 16 ,
- Huib A. M. Kerstjens 2 ,
- Johannes C. C. M. in ’t Veen 1 , 3 &
the TRICOLON study group
BMC Pulmonary Medicine volume 24 , Article number: 317 ( 2024 ) Cite this article
109 Accesses
Metrics details
Medication non-adherence is a significant problem in patients with Chronic Obstructive Pulmonary Disease (COPD). Efforts to address this issue are receiving increased attention. Simplifying treatment by prescribing single-inhaler triple therapy (SITT) as an alternative to multi-inhaler triple therapy (MITT) or with smart inhalers are often considered potential solutions. However, the actual impact of these innovations on adherence and clinical outcomes is unclear.
To address this knowledge gap we first conducted a literature review focusing on two research questions: 1) the difference in adherence between SITT and MITT users in COPD, and 2) the effect of smart inhalers on adherence in COPD. Separate searches were conducted in PubMed and two authors independently assessed the articles. In addition, we present a protocol for a study to acquire knowledge for the gaps identified.
To address the first research question, 8 trials were selected for further review. All trials were observational, i.e. randomized controlled trials were lacking. Seven of these trials showed higher adherence and/or persistence in patients on SITT compared with patients on MITT. In addition, four studies showed a positive effect of SITT on various clinical outcomes. For the second research question, 11 trials were selected for review. While most of the studies showed a positive effect of smart inhalers on adherence, there was considerable variation in the results regarding their effect on other clinical outcomes.
The TRICOLON (TRIple therapy COnvenience by the use of one or multipLe Inhalers and digital support in ChrONic Obstructive Pulmonary Disease) trial aims to improve understanding regarding the effectiveness of SITT and smart inhalers in enhancing adherence. This open-label, randomized, multi-center study will enroll COPD patients requiring triple therapy at ten participating hospitals. In total, 300 patients will be randomized into three groups: 1) MITT; 2) SITT; 3) SITT with digital support through a smart inhaler and an e-health platform. The follow-up period will be one year, during which three methods of measuring adherence will be used: smart inhaler data, self-reported data using the Test of Adherence to Inhalers (TAI) questionnaire, and drug analysis in scalp hair samples. Finally, differences in clinical outcomes between the study groups will be compared.
Our review suggests promising results concerning the effect of SITT, as opposed to MITT, and smart inhalers on adherence. However, the quality of evidence is limited due to the absence of randomized controlled trials and/or the short duration of follow-up in many studies. Moreover, its impact on clinical outcomes shows considerable variation. The TRICOLON trial aims to provide solid data on these frequently mentioned solutions to non-adherence in COPD. Collecting data in a well-designed randomized controlled trial is challenging, but the design of this trial addresses both the usefulness of SITT and smart inhalers while ensuring minimal interference in participants' daily lives.
Trial registration
NCT05495698 (Clinicaltrials.gov), registered at 08–08-2022. Protocol version: version 5, date 27–02-2023.
Peer Review reports
Introduction
Chronic obstructive pulmonary disease (COPD) is characterized by chronic respiratory symptoms due to abnormalities in the airways and/or alveoli, resulting in persistent and often progressive airflow obstruction. Inhalation medication is the primary medical treatment, with three types of inhalation medication available as maintenance therapy: 1) long-acting β2-agonist (LABA), 2) long-acting muscarinic antagonist (LAMA), and 3) inhaled corticosteroids (ICS). Triple therapy is defined as treatment with LABA, LAMA and ICS [ 1 ]. Large randomized controlled trials have shown that triple therapy provides clinical benefits compared to dual therapy in patients with moderate-to-severe COPD and a history of exacerbations, particularly when eosinophilia is present [ 2 , 3 , 4 , 5 , 6 ]. Furthermore, two trials suggest that triple therapy reduces mortality in this specific population [ 7 , 8 ]. Triple therapy can be administered through multiple devices, known as multi-inhaler-triple therapy (MITT), or combined in one inhaler, known as single-inhaler-triple therapy (SITT). Assessment of adherence to inhalation therapy is a crucial element in managing COPD patients according to the Global Initiative for Chronic Obstructive Lung Disease (GOLD) [ 1 ]. Previous studies have shown that medication adherence is poor in patients with COPD. A systematic review showed that non-adherence rates ranged from 22 to 93%, depending on the study population and method of measurement [ 9 ]. Non-adherence is associated with poor clinical and economic outcomes [ 10 , 11 ]. Simplifying treatment with smart-inhalers and prescribing single-inhaler triple therapy (SITT) as an alternative to multi-inhaler triple therapy (MITT) can be considered as potential solutions. Nowadays, the GOLD report (version 2024) acknowledges that a single inhaler may be more convenient compared to multi-inhaler therapy. [ 1 ]. The actual impact of these innovations on adherence is unclear. Therefore, we conducted a literature review to examine the current evidence on these two potential solutions. Should the evidence prove to be insufficient, we wanted to present a protocol for a study to fill this gap.
Methods for measuring adherence
Adherence is defined as the process by which patients take their medication as prescribed, while persistence refers to the duration from initiation to discontinuation of the treatment. Adherence and persistence are complex constructs, as previously described by Vrijens et al. [ 12 , 13 ]. Various methods can be used to assess medication adherence. Healthcare professionals commonly inquire directly about their patients' adherence. While this approach is straightforward, research has demonstrated its unreliability in comparison to more objective measurement methods. Unstructured self-reports often lead to an overestimation of adherence [ 14 ]. Patients can structurally self-report their adherence using questionnaires, such as the Test of Adherence to Inhalers (TAI). The TAI is developed specifically to measure adherence to inhalation medication in patients with COPD or asthma [ 15 ]. Furthermore, pharmacy data are often used to determine patient’s access to medication over time by calculating the Proportion of Days Covered (PDC). This method may be less reliable due to missing or inaccessible data (e.g. when multiple pharmacies are used) and the uncertainty about whether the patient actually used the medication [ 16 , 17 ]. Smart inhalers offer a more objective method for measuring adherence. These electronic sensors (e-devices) are attached to or integrated into inhalers. Devices range from simple dose counters to advanced devices that provide reminders, feedback, and/or analyse inhalation technique [ 18 ]. Smart inhalers are often integrated with other e-health interventions, such as telemonitoring, personalised feedback with apps, counselling, and training [ 19 , 20 , 21 ]. Finally, hair analysis can provide a bioanalytical assessment of average long-term drug exposure in the human body. This method could potentially provide an objective measure of adherence over the last few months. However, external factors can impact measurement, and only small part of medication that has been present in the systemic blood circulation is built into hair [ 22 ].
First, we present a review of the literature on two strategies to improve adherence. Second, we describe the study protocol of the TRICOLON trial (TRIple therapy COnvenience by the use of one or multipLe Inhalers and digital support in ChrONic Obstructive Pulmonary Disease).
Search strategy literature review
Separate searches were conducted in PubMed based on two research questions: 1) What is the difference in adherence between SITT and MITT users in COPD?, and 2) What is the effect of smart inhalers on adherence in COPD? The selection of articles from the second PubMed search was supplemented by four papers known to the authors or found by snowballing. Two authors independently assessed these articles to determine whether they should be included in this review (LC and JiV). In cases of disagreement, the opinion of a third author was sought (HK). Only original English-language studies were included. Details of the PubMed search and selection process can be found in the Appendix, Suppl.1.
Assessment of the evidence
The primary outcome was the adherence and/or persistence to triple therapy. Secondary outcomes were clinical outcomes, such as exacerbations, COPD Assessment Test (CAT) score, and FEV 1 . Each study underwent an evaluation across multiple criteria to assess the evidence supporting the research question. The strength of the study design was rated with stars: one star for retrospective studies, two stars for prospective observational studies or intervention studies without randomization (e.g. before-and-after designs), and three stars for randomised controlled trials. A green smiley indicates statistically significant superior results in the intervention group (either SITT or smart-inhaler group, depending on the research question) compared to the control group; a yellow neutral smiley signifies no difference between the groups, while a red sad smiley denotes statistically significant inferior results in the intervention group compared to the control group. Additionally, a thumbs-up signifies that other clinical outcomes were measured in that study, whereas a thumbs-down indicates the absence of measurements for other clinical outcomes, Tables 1 and 2 .
Literature review
Adherence to single versus multi inhaler triple therapy.
The first search yielded eighteen articles, Suppl. Figure 1. After the selection process, eight articles were included for further evaluation, Table 1 . None had a randomized controlled design. Four studies compared SITT with MITT in a prospective setting [ 23 , 27 , 28 , 30 ] and four in a retrospective analysis [ 24 , 25 , 26 , 29 ]. The retrospective studies used either anonymized data from electronic health records of patients in primary or secondary care [ 24 , 26 ], or databases of health insurance claims [ 25 , 29 ]. Seven of these studies showed that adherence and/or persistence to SITT was significantly higher compared to MITT in COPD patients [ 23 , 24 , 25 , 27 , 28 , 29 , 30 ]. Deslee et al. presented contrasting findings, showing that while persistence was higher in the SITT group (median 181 versus 135 days), adherence levels were similar in SITT and MITT (85.7% versus 86.1%) [ 26 ]. The seven trials that showed a positive effect of SITT on adherence were heterogeneous in terms of study design, and methods of measurement, type of inhaler, and molecules. Although most studies directly compared SITT with MITT, two of the prospective studies assessed adherence to SITT after switching from either dual therapy or MITT [ 27 , 28 ]. Brusselle et al. reported separate results for former MITT users: 71.9% at baseline, 74.7% three months after switching to SITT, and 83.8% at six months [ 28 ]. In contrast, Gessner et al. did not report separate results for the different treatments at baseline. Therefore, this difference between SITT and the control group should be interpreted with caution [ 27 ].
Clinical outcomes in single vs multi inhaler triple therapy
Five trials investigated the effect of SITT compared to MITT on clinical outcomes. Four of these trials showed a beneficial effect of SITT on clinical outcomes, Table 1 . SITT users had a lower risk of exacerbations compared to MITT users in two studies [ 23 , 28 ]; three studies showed lower CAT-scores and higher FEV 1 in SITT users [ 27 , 28 , 30 ]; and one study showed a reduced all-cause mortality risk in SITT users [HR: 0.475 (0.237–0.952), p = 0.036] [ 23 ]. In contrast to these studies with positive effects of SITT, Bogart et al. showed different results in two different groups of patients. In patients enrolled in Medicare Advantage with Part D (MAPD) insurance, a significant reduction in exacerbations and healthcare utilisation was seen in the SITT group. However, these differences were not statistically significant in the commercially insured patients [ 29 ].
The effect of smart inhalers on adherence
The second part of our literature review investigated the effect of smart inhalers on adherence in patients with COPD and resulted in 78 articles, from which 11 studies were selected, Table 2 . These studies were heterogenetic in terms of number of patients, study design, and type of intervention and/or smart inhaler. Additionally, length of follow-up ranged from 1 to 12 months, with the vast majority (90.9%) having a follow-up period of ≤ 6 months. Seven studies prospectively compared COPD patients who used a smart-inhalers with a control group; four of those had a randomized controlled open-label design. Six of these seven studies showed a statistically better adherence in the intervention group [ 19 , 31 , 32 , 37 , 38 , 40 ]; one prospective study showed no difference in adherence between smart inhaler users and controls [ 33 ]. Four other observational studies showed variable average adherence rates in smart-inhaler users from 44–77%; however, it should be noted that these trials did not include a control group without smart-inhaler [ 34 , 35 , 36 , 39 ].
The effect of smart inhalers on clinical outcomes
Nine studies also investigated the effect of smart inhalers on clinical outcomes [ 19 , 31 , 32 , 33 , 35 , 36 , 37 , 38 , 39 ]. These studies showed mixed results, Table 2 . A significant better inhalation technique was seen in two studies [ 31 , 33 ]. The impact of smart inhalers on other clinical outcomes, including exacerbations, disease burden, quality of life assessments, rescue medication usage, hospitalizations, and healthcare utilization, varied across different studies [ 19 , 32 , 33 , 35 , 36 , 37 , 38 , 39 ].
Conclusion of literature review
This review suggests promising results concerning the effect of SITT, as opposed to MITT, and smart inhalers on adherence. However, the quality of evidence is limited due to the absence of randomized controlled trials and/or the short duration of follow-up in many studies. Moreover, there is considerable variation in the findings of these studies regarding diverse clinical outcomes. Consequently, there is a clear need for comprehensive randomised controlled trials to evaluate the benefits of SITT versus MITT in COPD, as well as the individual and combined effects of smart inhalers, both on adherence and clinical outcomes.
Study protocol for an RCT: the TRICOLON study
The TRICOLON study was initiated to provide evidence on two previously mentioned potential solutions for the non-adherence issue in COPD patients. The primary objective is to investigate whether the adherence to SITT is superior to the adherence to MITT over 12 months of treatment and to investigate whether the adherence of SITT users with a smart inhaler and digital support is superior to the adherence of MITT and SITT users without the smart inhaler and digital support. As a secondary objective, three methods of measuring adherence will be compared: smart inhaler data, self-reported data using the Test of Adherence to Inhalers (TAI) questionnaire [ 15 ], and drug analysis of formoterol in scalp hair samples [ 41 ]. Finally, differences in clinical outcomes between the study groups will be examined.
Study design
The TRICOLON study is an investigator-initiated, prospective, open-label, randomised, real-world, multicentre study. The study will be conducted at ten hospitals in the Netherlands, Supplement 2. Patients will be recruited from the pulmonary wards or outpatient clinics of the participating hospitals. Informed consent will be obtained by a member of the research team. Participants are randomly assigned in a 1:1:1 ratio to one of three groups: 1) multi-inhaler triple therapy (Bevespi® and Qvar®), 2) single-inhaler triple therapy (Trimbow®), 3) single-inhaler triple therapy (Trimbow®) with digital support, Fig. 1 . The follow-up period will be one year, during which we aim to minimise disruption to their usual care, thus creating a (close to) real-world situation. The study outline is presented in Fig. 2 . Ethical approval for this study was granted by the United Medical Research Ethics Committees (NL79938.100.22). The trial is registered on clinicaltrials.gov (NCT05495698).
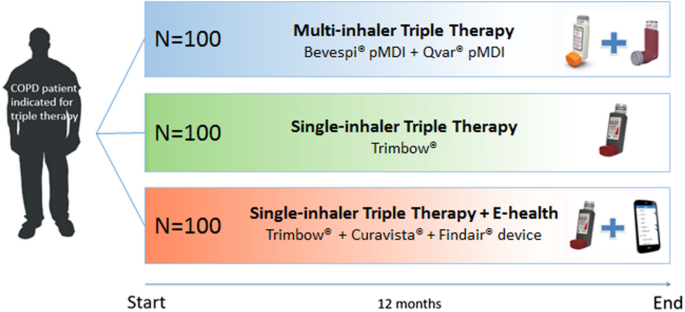
Study design. Patients are randomly assigned in a 1:1:1 ratio to one of three groups: 1) multi-inhaler triple therapy (Bevespi® and Qvar®), 2) single-inhaler triple therapy (Trimbow®), 3) single-inhaler triple therapy (Trimbow®) with e-health. The follow-up period is one year
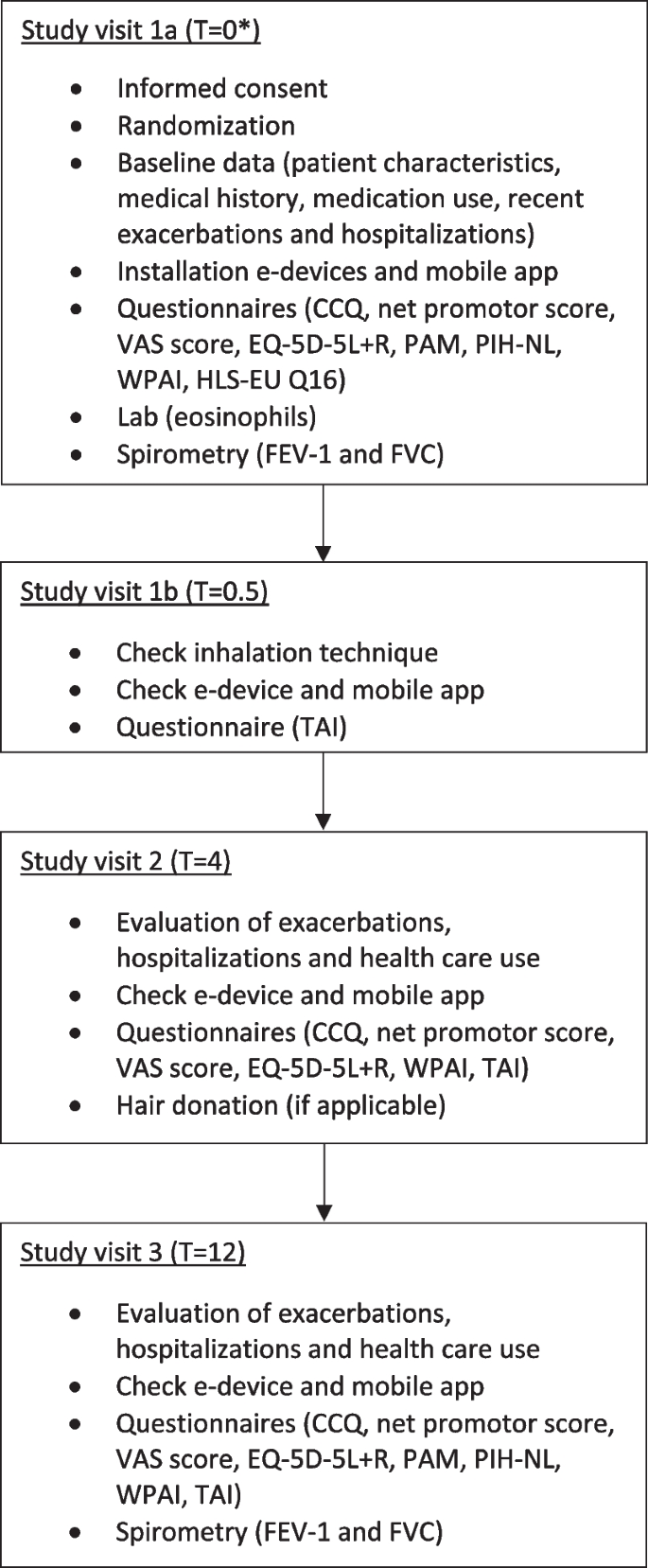
Study program
*time in months
Study participants
A total of 300 patients will be enrolled. Patients with a diagnosis of COPD and an indication for triple therapy according to their physician following the GOLD report are eligible to participate. Patients are excluded if asthma is the dominant diagnosis (asthma in the past or as a comorbidity is allowed), if patients use nebulizers or if they already use an e-health application for their COPD. The inclusion and exclusion criteria are displayed in Table 3 .
Interventions
The study groups have uniform doses, identical molecules and doses (beclomethasone 100µg, formoterol 6µg, and glycopyrronium 10µg), and the same device type (pressurised metered dose inhaler). Therefore, the only differentiating factors are the number of devices used and the use of digital support. Digital support comprises the Findair® smart-inhaler, an electronic device that is attached to the inhaler and measures the frequency and time of the actuations, and the Curavista® platform (Gezondheidsmeter PGO), a digital platform that promotes patient self-management by displaying their medication use and providing medication intake reminders [ 31 , 32 ]. Each patient is provided with smart inhalers that are attached to all their inhalers, including the potential rescue medication. This enables the measurement of actuation frequency and timing. The smart-inhalers are linked to the digital platform for data collection. However, it is important to note that only group 3 has access to an overview of the actuations with feedback in the app and reminders, along with full access to the digital platform. Groups 1 and 2 will not receive any reminders and cannot access the digital platform. Their e-health applications are solely used for data collection purposes, ensuring "silent monitoring" that should not influence their adherence.
We aim for all participants to complete the study using the original study medication. However, given the real-world nature of the study, it is possible that patients require a change in medication due to clinical reasons such as side effects or lack of effectiveness. To prevent the loss of these patients from the study, changes in medication are permitted only when absolutely necessary. Data collection will persist via the electronic devices and with the same settings of the app (silent monitoring or full access). Patients who no longer use a pressurized metered dose inhaler will be excluded, as the electronic devices are specifically tailored for this type of inhaler.
The primary outcome is the average adherence to ICS therapy (measured as the number of actuations registered by the smart-inhaler divided by the total number of doses prescribed, in %) over 12 months of treatment. As a secondary outcome, the average adherence to LABA/LAMA in study group 1 will be compared with adherence to ICS in group 1, and with adherence to LABA/LAMA/ICS in groups 2 and 3. Additional secondary outcomes include the percentage of patients with good adherence, defined as an average ICS adherence of more than 80% and less than 110% actuations measured by the smart inhaler; the Test of Adherence to Inhalers (TAI) scores; and drug levels of formoterol in scalp hair. The hair samples will be collected, stored, and prepared according to the guidelines of the Society of Hair Testing [ 42 ]. Additionally, the study will measure changes in Patient Reported Outcome Measures (PROMs), use of rescue medication, number of exacerbations and hospitalizations, healthcare consumption, and spirometry (FEV 1 ). The PROMs are displayed in Supplement 3.
Statistical analysis
The statistical software G*Power version 3.1.9.6 was used to calculate the sample size. The study aims to compare three groups: group 1 vs group 2, group 2 vs group 3, and group 1 vs group 3. The sample size calculation is based on the comparison of the average adherence in group 1 vs group 2 (so MITT vs SITT without e-health). Based on a previous study [ 19 ], we expect a 15% difference between the groups, with a standard deviation of 30%. The significance level of the test was set at (alpha) 0.0167 using the Holm-Bonferroni method to adjust for multiple testing, as we are comparing three groups (alpha 0.05/3 = 0.0167), with a power of 80%. We calculated n = 84 for each group using a two-sided T-test, and plan to include 100 patients in each group of the study, considering a potential drop-out rate of 15%. The patients will be randomized using the program Castor EDC. To prevent inequality in the study groups, at randomization patients will be stratified for their treatment before the study (dual therapy, MITT or SITT) and for inclusion during an exacerbation or during stable disease. The data will be analyzed using both the intention-to-treat (primary analysis) and per-protocol methods. The Kruskal–Wallis test or ANOVA, as appropriate, will be used to compare the average adherence between the three study groups. Post-hoc comparisons will be performed using Mann–Whitney U tests or Tukey’s HSD, as appropriate. The average baseline scores of the PROMs and baseline clinical status (FEV 1 , number of exacerbations, hospitalizations and rescue medication use) will be presented descriptively. These scores and outcomes are all continuous, unpaired data and will be compared between more than two groups. Therefore, we will use the Kruskal–Wallis or ANOVA, as appropriate, to investigate the differences between the three groups. The Net Promoter score is a binary variable, so we will use the Chi-square test. Questionnaire data will be analysed by both the difference in mean scores between groups and the percentage of patients achieving the minimally clinical important difference (MCID) when available. Furthermore, a mixed model repeated measurement analysis will be performed to assess the differences in the previously mentioned outcomes over time. The analysis will be conducted on normally distributed data, with or without transformations. The main parameter of interest is the group * time interaction. Between-group comparisons will be adjusted using the method of Sidak. If the data cannot be normalized, difference scores will be calculated (follow-up – baseline). These differences will be analysed using either the Kruskal–Wallis test or ANOVA, where appropriate. Post-hoc comparisons will be conducted using Mann–Whitney U tests or Tukey’s HSD, where appropriate.
Serious adverse events (SAEs) will be monitored and reported in accordance with the legal requirements and deadlines. The Ethics committee has granted permission for hospital admissions resulting from a COPD exacerbation not to be reported as SAE. This exemption is due to their frequent occurrence in this specific population. Instead, to monitor this fragile population, a Data and Safety Monitoring Board (DSMB) has been established. The DSMB will periodically review mortality rates, serious adverse events, and premature withdrawals from the study every six months. The application and e-health platform in use have a substantial history, spanning many years. Over the past two decades, 26 peer-reviewed scientific publications have been published. Notably, there have been no reported safety concerns, and assessments of usability, feasibility, and efficacy consistently yield positive results [ 43 ].
Non-adherence is a significant challenge in COPD patients, and addressing this issue is receiving increased attention. The first solution we investigated was simplifying the treatment by prescribing single-inhaler triple therapy (SITT) as an alternative to multi-inhaler triple therapy (MITT). The GOLD report 2023 suggested, for the first time, that single inhaler therapy may be more convenient than multi inhaler therapy [ 1 ]. However, although our literature review reveals some promising results regarding the effect of SITT on adherence, the quality of evidence is limited due to the absence of randomized controlled trials that specifically examined the difference in adherence between SITT and MITT. Due to the observational setting and design of all studies in the first part of this review, the SITT and MITT groups showed differences in their baseline characteristics, including the number of exacerbations prior to enrolment, disease severity, and FEV-1. Moreover, the quality of the observational data was occasionally limited. For example, two studies relied on administrative databases using health insurance claims [ 25 , 29 ]. Consequently, from these trials we are unable to draw conclusions on the cause-effect relationship between improved adherence and clinical outcomes. In contrast to the four studies included in our review, which all demonstrated slightly better clinical outcomes in SITT users, other literature, not incorporated into our review due to a lack of adherence as an outcome, presented contrasting results regarding the effect of SITT on clinical outcomes. Specifically, a retrospective study in Spain and an RCT showed improved clinical outcomes in SITT users [ 44 , 45 ]. However, three randomized controlled trials indicated that both SITT and MITT users exhibited similar results in terms of lung function, health status, exacerbation rate, and rescue medication usage [ 2 , 46 , 47 ].
The use of smart inhalers was the second potential solution to non-adherence that we investigated. Our review showed that while the effect on adherence was mostly positive, no consistent differences in clinical outcomes were observed. The strength of studies showing improved adherence in the absence of improved clinical outcomes is limited. These findings are consistent with other recent reviews in both COPD and asthma [ 18 , 20 , 21 ]. Demonstrating the connection between adherence and clinical outcomes has proven to be challenging. Given that COPD entails irreversible lung damage and the medication aims to stabilize rather than cure the disease, an extensive follow-up period is essential to demonstrate its impact on clinical outcomes. However, the current studies have limitations regarding the duration of follow-up. The smart inhalers used, as well as the supplementary interventions, and the extent of monitoring and/or interference varied significantly among the studies. The majority of smart inhalers used in current literature can only record the time and location of actuation. They are unable to measure whether inhalation is performed correctly. Other techniques, such as smart inhalers capable of measuring airflow or hair analysis of inhaled drugs, can assist in addressing this limitation. Further research is needed to gain a deeper understanding of the contributions of the different electronic modalities, the underlying mechanisms, clinical outcomes, and optimal implementation of these devices in clinical practice. Several challenges must be addressed before integrating smart inhalers into daily practice, including technical complexities, limited evidence concerning clinical outcomes, uncertainties about cost-effectiveness, and the issue of funding for the devices [ 18 ]. The TRICOLON study aims to offer additional evidence, potentially bringing us closer to their use in daily practice.
To the best of our knowledge, the TRICOLON trial is the first that aims to investigate whether single inhaler usage in COPD patients receiving triple therapy can improve adherence in a large-scale, randomized, controlled, real-world setting. Moreover, unlike the majority of existing studies focusing on the impact of smart inhalers, the TRICOLON trial distinguishes itself with a prolonged follow-up period of one year. We acknowledge that patients’ adherence may be influenced by their awareness of participating in a study. To minimize this interference, we have limited the number of study visits to closely resemble real-world settings. Additionally, patients are informed that the focus of this study is on the convenience of various treatment options, and adherence is not specifically mentioned in the information provided by the researchers or in the patient information letter. This has been approved by the Medical Ethical Review Board. The Tricolon study not only investigates the impacts of a single inhaler and the use of a smart inhaler on adherence but also evaluates various clinical outcomes, including exacerbation rates, hospitalizations, and disease burden. Nevertheless, the study is powered on the primary outcome adherence to inhalation therapy. Therefore, although not powered for the clinical outcomes or for the correlation between adherence and clinical outcomes, valuable information on these outcomes will be collected to inform possible follow-up studies.
The implementation of an e-health application may present challenges, whether due to technical issues or the potential unfamiliarity among patients and healthcare professionals [ 48 ]. To proactively address these concerns, we dedicated time to thoroughly test the application before the start of the study. This involved multiple stakeholders, including the researchers, the app producer, and patients. Moreover, the application's design is intentionally kept simple and clear, ensuring that individuals of all ages, educational backgrounds, and health literacy levels can easily comprehend and use it. This was confirmed in a previous study where an older, and thus more digitally challenged, population of patients with Idiopathic Pulmonary Fibrosis (IPF) used this app for daily spirometry. The study found that 80% of the participants found the app easy to use, and 90% did not perceive it as burdensome [ 49 ].
Beyond addressing the primary research questions, this TRICOLON study creates an opportunity for a direct comparison between three methods to measure adherence: digital data from the smart inhaler, self-reported data collected through the TAI questionnaire, and drug deposition data in hair. The use of this final technique is relatively uncommon in studies concerning inhalation medication, although it has been used in previous research related to cortisol and in forensic studies [ 22 , 50 ]. In a specific study involving asthma and COPD patients, the measurement of inhalation medication demonstrated a clear dose–response relationship among those using formoterol [ 41 ].
Our identification of a lack of high-quality data on the improvement of adherence of SITT over MITT therapy in COPD and limited data for smart inhalers highlights the need for further research. The multi-centre, randomized controlled, three-arm, real-world TRICOLON trial aims to increase insight in the value of SITT and the added value of electronic adherence monitoring.
Availability of data and materials
All data relevant to the study are included in the article or uploaded as supplementary information. The datasets used and/or analyzed during the current study are available from the corresponding author on reasonable request.
Global Initiative for Chronic Obstructive Lung Disease. 2023 Report: global strategy for prevention, diagnosis and management of COPD [Available from: https://goldcopd.org/2023-gold-report-2/ .
Vestbo J, Papi A, Corradi M, Blazhko V, Montagna I, Francisco C, et al. Single inhaler extrafine triple therapy versus long-acting muscarinic antagonist therapy for chronic obstructive pulmonary disease (TRINITY): a double-blind, parallel group, randomised controlled trial. Lancet. 2017;389(10082):1919–29.
Article CAS PubMed Google Scholar
Lipson DA, Barnhart F, Brealey N, Brooks J, Criner GJ, Day NC, et al. Once-Daily Single-Inhaler Triple versus Dual Therapy in Patients with COPD. N Engl J Med. 2018;378(18):1671–80.
Papi A, Vestbo J, Fabbri L, Corradi M, Prunier H, Cohuet G, et al. Extrafine inhaled triple therapy versus dual bronchodilator therapy in chronic obstructive pulmonary disease (TRIBUTE): a double-blind, parallel group, randomised controlled trial. Lancet. 2018;391(10125):1076–84.
Singh D, Papi A, Corradi M, Pavlisova I, Montagna I, Francisco C, et al. Single inhaler triple therapy versus inhaled corticosteroid plus long-acting beta2-agonist therapy for chronic obstructive pulmonary disease (TRILOGY): a double-blind, parallel group, randomised controlled trial. Lancet. 2016;388(10048):963–73.
Ferguson GT, Rabe KF, Martinez FJ, Fabbri LM, Wang C, Ichinose M, et al. Triple therapy with budesonide/glycopyrrolate/formoterol fumarate with co-suspension delivery technology versus dual therapies in chronic obstructive pulmonary disease (KRONOS): a double-blind, parallel-group, multicentre, phase 3 randomised controlled trial. Lancet Respir Med. 2018;6(10):747–58.
Lipson DA, Crim C, Criner GJ, Day NC, Dransfield MT, Halpin DMG, et al. Reduction in All-Cause Mortality with Fluticasone Furoate/Umeclidinium/Vilanterol in Patients with Chronic Obstructive Pulmonary Disease. Am J Respir Crit Care Med. 2020;201(12):1508–16.
Article PubMed PubMed Central Google Scholar
Rabe KF, Martinez FJ, Ferguson GT, Wang C, Singh D, Wedzicha JA, et al. Triple Inhaled Therapy at Two Glucocorticoid Doses in Moderate-to-Very-Severe COPD. N Engl J Med. 2020;383(1):35–48.
Bhattarai B, Walpola R, Mey A, Anoopkumar-Dukie S, Khan S. Barriers and strategies for improving medication adherence among people living with COPD: a systematic review. Respir Care. 2020;65(11):1738–50.
Article PubMed Google Scholar
van Boven JF, Chavannes NH, van der Molen T, Rutten-van Molken MP, Postma MJ, Vegter S. Clinical and economic impact of non-adherence in COPD: a systematic review. Respir Med. 2014;108(1):103–13.
Cushen B, Sulaiman I, Greene G, MacHale E, Mokoka M, Reilly RB, et al. The clinical impact of different adherence behaviors in patients with severe chronic obstructive pulmonary disease. Am J Respir Crit Care Med. 2018;197(12):1630–3.
Vrijens B, De Geest S, Hughes DA, Przemyslaw K, Demonceau J, Ruppar T, et al. A new taxonomy for describing and defining adherence to medications. Br J Clin Pharmacol. 2012;73(5):691–705.
Vrijens B, Dima AL, Van Ganse E, van Boven JF, Eakin MN, Foster JM, et al. What we mean when we talk about adherence in respiratory medicine. J Allergy Clin Immunol Pract. 2016;4(5):802–12.
George J, Kong DC, Stewart K. Adherence to disease management programs in patients with COPD. Int J Chron Obstruct Pulmon Dis. 2007;2(3):253–62.
PubMed PubMed Central Google Scholar
Plaza V, Fernandez-Rodriguez C, Melero C, Cosio BG, Entrenas LM, de Llano LP, et al. Validation of the “Test of the Adherence to Inhalers” (TAI) for Asthma and COPD Patients. J Aerosol Med Pulm Drug Deliv. 2016;29(2):142–52.
Rogliani P, Ora J, Puxeddu E, Matera MG, Cazzola M. Adherence to COPD treatment: Myth and reality. Respir Med. 2017;129:117–23.
Loucks J, Zuckerman AD, Berni A, Saulles A, Thomas G, Alonzo A. Proportion of days covered as a measure of medication adherence. Am J Health Syst Pharm. 2022;79(6):492–6.
Jansen EM, van de Hei SJ, Dierick BJH, Kerstjens HAM, Kocks JWH, van Boven JFM. Global burden of medication non-adherence in chronic obstructive pulmonary disease (COPD) and asthma: a narrative review of the clinical and economic case for smart inhalers. J Thorac Dis. 2021;13(6):3846–64.
O’Dwyer S, Greene G, MacHale E, Cushen B, Sulaiman I, Boland F, et al. Personalized biofeedback on inhaler adherence and technique by community pharmacists: a cluster randomized clinical trial. J Allergy Clin Immunol Pract. 2020;8(2):635–44.
Garin N, Zarate-Tamames B, Gras-Martin L, Milà R, Crespo-Lessmann A, Curto E, Hernandez M, Mestres C, Plaza V. Clinical Impact of Electronic Monitoring Devices of Inhalers in Adults with Asthma or COPD: A Systematic Review and Meta-Analysis. Pharmaceuticals (Basel). 2023;16(3):414. https://doi.org/10.3390/ph16030414 .
Schulte MHJ, Aardoom JJ, Loheide-Niesmann L, Verstraete LLL, Ossebaard HC, Riper H. Effectiveness of eHealth Interventions in Improving Medication Adherence for Patients With Chronic Obstructive Pulmonary Disease or Asthma: Systematic Review. J Med Internet Res. 2021;23(7):e29475.
Rygaard K, Linnet K, Johansen SS. A Systematic Review of Metabolite-to-Drug Ratios of Pharmaceuticals in Hair for Forensic Investigations. Metabolites. 2021;11(10):686. https://doi.org/10.3390/metabo11100686 .
Lin L, Liu C, Cheng W, Song Q, Zeng Y, Li X, et al. Comparison of treatment persistence, adherence, and risk of exacerbation in patients with COPD treated with single-inhaler versus multiple-inhaler triple therapy: A prospective observational study in China. Front Pharmacol. 2023;14:1147985.
Article CAS PubMed PubMed Central Google Scholar
Halpin DMG, Rothnie KJ, Banks V, Czira A, Compton C, Wood R, et al. Comparative Adherence and Persistence of Single- and Multiple-Inhaler Triple Therapies Among Patients with Chronic Obstructive Pulmonary Disease in an English Real-World Primary Care Setting. Int J Chron Obstruct Pulmon Dis. 2022;17:2417–29.
Mannino D, Bogart M, Wu B, Germain G, Laliberte F, MacKnight SD, et al. Adherence and persistence to once-daily single-inhaler versus multiple-inhaler triple therapy among patients with chronic obstructive pulmonary disease in the USA: A real-world study. Respir Med. 2022;197:106807.
Deslee G, Fabry-Vendrand C, Poccardi N, Thabut G, Eteve Pitsaer C, Coriat A, Renaudat C, Maguire A, Pinto T. Use and persistence of single and multiple inhaler triple therapy prescribed for patients with COPD in France: a retrospective study on THIN database (OPTI study). BMJ Open Respir Res. 2023;10(1):e001585. https://doi.org/10.1136/bmjresp-2022-001585 .
Gessner C, Trinkmann F, Bahari Javan S, Hovelmann R, Bogoevska V, Georges G, et al. Effectiveness of Extrafine Single Inhaler Triple Therapy in Chronic Obstructive Pulmonary Disease (COPD) in Germany - The TriOptimize Study. Int J Chron Obstruct Pulmon Dis. 2022;17:3019–31.
Brusselle G, Himpe U, Fievez P, Leys M, Perez Bogerd S, Peche R, et al. Evolving to a single inhaler extrafine LABA/LAMA/ICS - Inhalation technique and adherence at the heart of COPD patient care (TRIVOLVE). Respir Med. 2023;218:107368.
Bogart M, Bengtson LGS, Johnson MG, Bunner SH, Gronroos NN, DiRocco KK. Outcomes Following Initiation of Triple Therapy with Fluticasone Furoate/Umeclidinium/Vilanterol versus Multiple-Inhaler Triple Therapy Among Medicare Advantage with Part D Beneficiaries and Those Commercially Enrolled for Health Care Insurance in the United States. Int J Chron Obstruct Pulmon Dis. 2024;19:97–110.
Beeh KM, Scheithe K, Schmutzler H, Kruger S. Real-World Effectiveness of Fluticasone Furoate/Umeclidinium/Vilanterol Once-Daily Single-Inhaler Triple Therapy for Symptomatic COPD: The ELLITHE Non-Interventional Trial. Int J Chron Obstruct Pulmon Dis. 2024;19:205–16.
Hesso I, Nabhani-Gebara S, Kayyali R. Objective Assessment of Adherence and Inhaler Technique among Asthma and COPD Patients in London: A Study in Community Pharmacies Using an Electronic Monitoring Device. Pharmacy (Basel). 2023;11(3):94. https://doi.org/10.3390/pharmacy11030094 .
Criner GJ, Cole T, Hahn KA, Kastango K, Eudicone J, Gilbert I. The Impact of Budesonide/Formoterol pMDI Medication Reminders on Adherence in Chronic Obstructive Pulmonary Disease (COPD) Patients: Results of a Randomized, Phase 4, Clinical Study. Int J Chron Obstruct Pulmon Dis. 2021;16:563–77.
Dierick BJH, Been-Buck S, Klemmeier T, Hagedoorn P, van de Hei SJ, Kerstjens HAM, et al. Digital spacer data driven COPD inhaler adherence education: The OUTERSPACE proof-of-concept study. Respir Med. 2022;201:106940.
Kaye L, Gondalia R, Thompson A, Stempel DA, Barrett MA. The relationship between objective app engagement and medication adherence in asthma and COPD: a retrospective analysis. Sci Rep. 2021;11(1):24343.
Yawn BP, McCreary GM, Linnell JA, Pasquale CB, Malanga E, Choate R, et al. Pilot Study of a Patient Experience with an ELLIPTA Inhaler electronic medication monitor and associated integrated system: a prospective observational study using the COPD Patient-Powered Research Network. Chronic Obstr Pulm Dis. 2021;8(4):488–501.
Kaye L, Gondalia R, Barrett MA, Williams M, Stempel DA. Concurrent improvement observed in patient-reported burden and sensor-collected medication use among patients enrolled in a COPD Digital Health Program. Front Digit Health. 2021;3:624261.
Gregoriano C, Dieterle T, Breitenstein AL, Durr S, Baum A, Giezendanner S, et al. Does a tailored intervention to promote adherence in patients with chronic lung disease affect exacerbations? A randomized controlled trial. Respir Res. 2019;20(1):273.
Broadbent E, Garrett J, Jepsen N, Li Ogilvie V, Ahn HS, Robinson H, et al. Using Robots at Home to Support Patients With Chronic Obstructive Pulmonary Disease: Pilot Randomized Controlled Trial. J Med Internet Res. 2018;20(2):e45.
Alshabani K, Attaway AA, Smith MJ, Majumdar U, Rice R, Han X, et al. Electronic inhaler monitoring and healthcare utilization in chronic obstructive pulmonary disease. J Telemed Telecare. 2020;26(7–8):495–503.
Nides MA, Tashkin DP, Simmons MS, Wise RA, Li VC, Rand CS. Improving inhaler adherence in a clinical trial through the use of the nebulizer chronolog. Chest. 1993;104(2):501–7.
Hassall D, Brealey N, Wright W, Hughes S, West A, Ravindranath R, et al. Hair analysis to monitor adherence to prescribed chronic inhaler drug therapy in patients with asthma or COPD. Pulm Pharmacol Ther. 2018;51:59–64.
Cooper GA, Kronstrand R, Kintz P, Society of Hair T. Society of Hair Testing guidelines for drug testing in hair. Forensic Sci Int. 2012;218(1–3):20–4.
https://www.gezondheidsmeter.nl/site/index.php [
Alcazar-Navarrete B, Jamart L, Sanchez-Covisa J, Juarez M, Graefenhain R, Sicras-Mainar A. Clinical Characteristics, Treatment Persistence, and Outcomes Among Patients With COPD Treated With Single- or Multiple-Inhaler Triple Therapy: A Retrospective Analysis in Spain. Chest. 2022;162(5):1017–29.
Halpin DMG, Worsley S, Ismaila AS, Beeh KM, Midwinter D, Kocks JWH, Irving E, Marin JM, Martin N, Tabberer M, Snowise NG, Compton C. INTREPID: single- versus multiple-inhaler triple therapy for COPD in usual clinical practice. ERJ Open Res. 2021;7(2):00950–2020. https://doi.org/10.1183/23120541.00950-2020 .
Ferguson GT, Brown N, Compton C, Corbridge TC, Dorais K, Fogarty C, et al. Once-daily single-inhaler versus twice-daily multiple-inhaler triple therapy in patients with COPD: lung function and health status results from two replicate randomized controlled trials. Respir Res. 2020;21(1):131.
Bremner PR, Birk R, Brealey N, Ismaila AS, Zhu CQ, Lipson DA. Single-inhaler fluticasone furoate/umeclidinium/vilanterol versus fluticasone furoate/vilanterol plus umeclidinium using two inhalers for chronic obstructive pulmonary disease: a randomized non-inferiority study. Respir Res. 2018;19(1):19.
Pinnock H, Hui CY, van Boven JFM. Implementation of digital home monitoring and management of respiratory disease. Curr Opin Pulm Med. 2023;29(4):302–12.
Moor CC, Wapenaar M, Miedema JR, Geelhoed JJM, Chandoesing PP, Wijsenbeek MS. A home monitoring program including real-time wireless home spirometry in idiopathic pulmonary fibrosis: a pilot study on experiences and barriers. Respir Res. 2018;19(1):105.
Greff MJE, Levine JM, Abuzgaia AM, Elzagallaai AA, Rieder MJ, van Uum SHM. Hair cortisol analysis: An update on methodological considerations and clinical applications. Clin Biochem. 2019;63:1–9.
Download references
Acknowledgements
We appreciate the assistance of Carmen van der Heijden, librarian at the Medical Library in the Franciscus Gasthuis & Vlietland hospital, in conducting the PubMed searches. We would like to thank the members of the investigational teams across all participating hospitals for their dedicated time and effort in conducting this study.
TRICOLON study group
The TRICOLON Study Group consortium consists of the individuals listed below:
Liz J.A. Cuperus MD 1,2,3 , Job van der Palen PhD 4 , Arnoud Aldenkamp MD 5 , Astrid van Huisstede MD PhD 6 , Erik W.M.A. Bischoff MD PhD 7 , Job F.M. van Boven PharmD PhD 8 , Folkert Brijker MD 9 , Stephan Dik MD 10 , Jeroen A.J.M. van Excel MD 11 , Martijn Goosens MD 12 , Peter Th.W. van Hal MD PhD 13 , Jolanda C. Kuijvenhoven MD PhD 14 , Lisette I.Z. Kunz MD PhD 15 , Erwin C. Vasbinder PhD 16 , Huib A.M. Kerstjens MD PhD 2 , Johannes C.C.M. in ’t Veen MD PhD 1,3 , Marjo van der Poel 17 , Marijke Amelink 9 , Anke Rol 18 , Jennifer de Graaf 18 , Petra Hirmann 19 , Fleur van Tour 20 , Elly Jordens 13 , Lydia Alfing 13 , Gerda Lenderink 21 , Thecla Rupert 21 , Truus Rietveld 21 , Jasmijn van Campen 15 , Jantine de Bruijn 15 , Janice van ter Burg 15 , Walter van Litsenburg 5 , Len Knoops 22 , Margot Eggermont-Schilt 23 , Manon de Waard-Heijligers 23 , Ilonka Paalvast-Schouten 23 , Sarah van Oord 11
1 Pulmonology Department, Franciscus Gasthuis and Vlietland, Rotterdam, the Netherlands
2 Pulmonology Department, University of Groningen, University Medical Center Groningen, and Groningen Research Institute for Asthma and COPD, Groningen, the Netherlands
3 Pulmonology Department, Erasmus Medical Centre, Rotterdam, the Netherlands
4 Department of Epidemiology, Medisch Spectrum Twente, Enschede, The Netherlands
5 Department of Pulmonary Medicine, Catharina Hospital, Eindhoven, The Netherlands
6 Department of Pulmonology, Northwest Clinics, Alkmaar, the Netherlands
7 Department of Primary and Community Care, Radboud University Medical Center, Nijmegen, Netherlands
8 Department of Clinical Pharmacy & Pharmacology Groningen Research Institute for Asthma and COPD (GRIAC), University Medical Center Groningen, University of Groningen, Groningen, The Netherlands
9 Department of Pulmonary Medicine, Spaarne Gasthuis, Haarlem, The Netherlands
10 Department of Pulmonary Medicine, Albert Schweitzer ziekenhuis, Dordrecht, The Netherlands
11 Department of Pulmonary Medicine, HagaZiekenhuis, The Hague, The Netherlands
12 Department of Pulmonary Medicine, Gelre Ziekenhuizen, Zutphen, The Netherlands
13 Department of Respiratory Medicine, Van Weel-Bethesda Hospital, Dirksland, the Netherlands
14 Department of Respiratory Medicine, Medical Centre Leeuwarden, Leeuwarden, the Netherlands
15 Department of Pulmonology, Haaglanden Medical Centre, The Hague, the Netherlands
16 Department of Clinical Pharmacy, Franciscus Gasthuis, Rotterdam, the Netherlands
17 Spaarne Gasthuis, Haarlem, The Netherlands
18 Northwest Clinics, Alkmaar, the Netherlands
19 Medical Centre Leeuwarden, Leeuwarden, the Netherlands
20 Albert Schweitzer ziekenhuis, Dordrecht, The Netherlands
21 Gelre Ziekenhuizen, Zutphen, The Netherlands
22 Catharina Hospital, Eindhoven, The Netherlands
23 HagaZiekenhuis, The Hague, The Netherlands
The faculty received an unrestricted grant from Chiesi Pharmaceuticals B.V. Furthermore, the funding includes contributions from the research group in the Franciscus Gasthuis & Vlietland hospital and transformation funds from health insurance companies.
Author information
Authors and affiliations.
Pulmonology Department, Franciscus Gasthuis and Vlietland, Rotterdam, the Netherlands
Liz J. A. Cuperus & Johannes C. C. M. in ’t Veen
Pulmonology Department, University of Groningen, University Medical Center Groningen, and Groningen Research Institute for Asthma and COPD, Groningen, the Netherlands
Liz J. A. Cuperus & Huib A. M. Kerstjens
Pulmonology Department, Erasmus Medical Centre, Rotterdam, the Netherlands
Department of Epidemiology, Medisch Spectrum Twente, Enschede, The Netherlands
Job van der Palen
Department of Pulmonary Medicine, Catharina Hospital, Eindhoven, The Netherlands
Arnoud Aldenkamp
Department of Pulmonology, Northwest Clinics, Alkmaar, the Netherlands
Astrid van Huisstede
Department of Primary and Community Care, Radboud University Medical Center, Nijmegen, The Netherlands
Erik W. M. A. Bischoff
Department of Clinical Pharmacy & Pharmacology Groningen Research Institute for Asthma and COPD (GRIAC), University Medical Center Groningen, University of Groningen, Groningen, The Netherlands
Job F. M. van Boven
Department of Pulmonary Medicine, Spaarne Gasthuis, Haarlem, The Netherlands
Folkert Brijker
Department of Pulmonary Medicine, Albert Schweitzer Ziekenhuis, Dordrecht, The Netherlands
Stephan Dik
Department of Pulmonary Medicine, HagaZiekenhuis, The Hague, The Netherlands
Jeroen A. J. M. van Excel
Department of Pulmonary Medicine, Gelre Ziekenhuizen, Zutphen, The Netherlands
Martijn Goosens
Department of Respiratory Medicine, Van Weel-Bethesda Hospital, Dirksland, The Netherlands
Peter Th. W. van Hal
Department of Respiratory Medicine, Medical Centre Leeuwarden, Leeuwarden, The Netherlands
Jolanda C. Kuijvenhoven
Department of Pulmonology, Haaglanden Medical Centre, The Hague, The Netherlands
Lisette I. Z. Kunz
Department of Clinical Pharmacy, Franciscus Gasthuis, Rotterdam, The Netherlands
Erwin C. Vasbinder
You can also search for this author in PubMed Google Scholar
- Liz J. A. Cuperus
- , Job van der Palen
- , Arnoud Aldenkamp
- , Astrid van Huisstede
- , Erik W. M. A. Bischoff
- , Job F. M. van Boven
- , Folkert Brijker
- , Stephan Dik
- , Jeroen A. J. M. van Excel
- , Martijn Goosens
- , Peter Th. W. van Hal
- , Jolanda C. Kuijvenhoven
- , Lisette I. Z. Kunz
- , Erwin C. Vasbinder
- , Huib A. M. Kerstjens
- , Johannes C. C. M. in ’t Veen
- , Marjo van der Poel
- , Marijke Amelink
- , Jennifer de Graaf
- , Petra Hirmann
- , Fleur van Tour
- , Elly Jordens
- , Lydia Alfing
- , Gerda Lenderink
- , Thecla Rupert
- , Truus Rietveld
- , Jasmijn van Campen
- , Jantine de Bruijn
- , Janice ter Burg
- , Walter van Litsenburg
- , Len Knoops
- , Margot Eggermont-Schilt
- , Manon de Waard-Heijligers
- , Ilonka Paalvast-Schouten
- & Sarah van Oord
Contributions
LC and JV conducted the assessment and selection of articles from the PubMed searches, HK was consulted in case of author disagreements. JV initiated the Tricolon trial and acquired the funding. LC, JV, HK, JvdP, EB, JvB were involved in the study design and protocol. LC is the coordinating investigator, JV is the principal investigator. LC, JV and HK wrote the main manuscript text. All authors have thoroughly read, critically revised, and approved the submitted version of the final manuscript.
Corresponding author
Correspondence to Liz J. A. Cuperus .
Ethics declarations
Ethics approval and consent to participate.
Ethics approval for the Tricolon study was waived by the Medical research Ethics Committees United (NL79938.100.22). This study is performed after approval by the Institutional Research Board and Board of Directors of the participating hospitals. The study is registered at clinicaltrials.gov (NCT05495698). Informed consent was obtained from all subjects.
Consent for publication
Not Applicable.
Competing interests
JvdP: none.
EB: unrestricted grants and speaking fees received from Chiesi Pharmaceuticals B.V., Boehringer Ingelheim bv, GlaxoSmithKline.
JvB: received unrestricted research grants from Aardex, AstraZeneca, Chiesi, European Commission COST Action 19132 (ENABLE), European Respiratory Society CRC “CONNECT”, Novartis, Pfizer, Pill Connect, Trudell Medical and consultancy/speaker fees from AstraZeneca, Chiesi, GSK, Novartis, Teva and Vertex. All payments were unrelated to this manuscript and all paid to his institution (UMCG).
LK: received speaker fees from AZ.
EV: received unrestricted research grants from AstraZeneca and Pfizer.
HK: reports grants and consultancy/advisory board participation from/for AstraZeneca, Boehringer Ingelheim, Chiesi, GlaxoSmithKline, and Novartis, all outside the submitted work. All were paid to his institution.
JiV: received unrestricted faculty research grants from GSK, Teva, AZ, Chiesi, Sanofi, and speaker fees from AZ, GSK, Sanofi, Chiesi, Stichting RoLeX and Health Investment.
Additional information
Publisher’s note.
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Suuplementary material 1., rights and permissions.
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/ . The Creative Commons Public Domain Dedication waiver ( http://creativecommons.org/publicdomain/zero/1.0/ ) applies to the data made available in this article, unless otherwise stated in a credit line to the data.
Reprints and permissions
About this article
Cite this article.
Cuperus, L.J.A., van der Palen, J., Aldenkamp, A. et al. Adherence to single inhaler triple therapy and digital inhalers in Chronic Obstructive Pulmonary Disease: a literature review and protocol for a randomized controlled trial (TRICOLON study). BMC Pulm Med 24 , 317 (2024). https://doi.org/10.1186/s12890-024-03044-3
Download citation
Received : 16 February 2024
Accepted : 02 May 2024
Published : 04 July 2024
DOI : https://doi.org/10.1186/s12890-024-03044-3
Share this article
Anyone you share the following link with will be able to read this content:
Sorry, a shareable link is not currently available for this article.
Provided by the Springer Nature SharedIt content-sharing initiative
- Triple therapy
- Single inhaler
- Smart inhaler
- Telemonitoring
- Digital adherence technology
BMC Pulmonary Medicine
ISSN: 1471-2466
- Submission enquiries: [email protected]
- General enquiries: [email protected]
- Open access
- Published: 03 July 2024
Healthcare leaders navigating complexity: a scoping review of key trends in future roles and competencies
- Samantha Spanos ORCID: orcid.org/0000-0003-3734-3907 1 ,
- Elle Leask ORCID: orcid.org/0000-0003-1698-9151 1 ,
- Romika Patel ORCID: orcid.org/0009-0000-6523-8798 1 ,
- Michael Datyner 1 ,
- Erwin Loh ORCID: orcid.org/0000-0001-7157-0826 2 &
- Jeffrey Braithwaite ORCID: orcid.org/0000-0003-0296-4957 1
BMC Medical Education volume 24 , Article number: 720 ( 2024 ) Cite this article
213 Accesses
Metrics details
As healthcare systems rapidly become more complex, healthcare leaders are navigating expanding role scopes and increasingly varied tasks to ensure the provision of high-quality patient care. Despite a range of leadership theories, models, and training curricula to guide leadership development, the roles and competencies required by leaders in the context of emerging healthcare challenges (e.g., disruptive technologies, ageing populations, and burnt-out workforces) have not been sufficiently well conceptualized. This scoping review aimed to examine these roles and competencies through a deep dive into the contemporary academic and targeted gray literature on future trends in healthcare leadership roles and competencies.
Three electronic databases (Business Source Premier, Medline, and Embase) were searched from January 2018 to February 2023 for peer-reviewed literature on key future trends in leadership roles and competencies. Websites of reputable healthcare- and leadership-focused organizations were also searched. Data were analyzed using descriptive statistics and thematic analysis to explore both the range and depth of literature and the key concepts underlying leadership roles and competencies.
From an initial 348 articles identified in the literature and screened for relevance, 39 articles were included in data synthesis. Future leadership roles and competencies were related to four key themes: innovation and adaptation (e.g., flexibility and vision setting), collaboration and communication (e.g., relationship and trust building), self-development and self-awareness (e.g., experiential learning and self-examination), and consumer and community focus (e.g., public health messaging). In each of these areas, a broad range of strategies and approaches contributed to effective leadership under conditions of growing complexity, and a diverse array of contexts and situations for which these roles and competencies are applicable.
Conclusions
This research highlights the inherent interdependence of leadership requirements and health system complexity. Rather than as sets of roles and competencies, effective healthcare leadership might be better conceptualized as a set of broad goals to pursue that include fostering collaboration amongst stakeholders, building cultures of capacity, and continuously innovating for improved quality of care.
Peer Review reports
Healthcare leadership has grown in scope and importance in response to the increasing complexity of healthcare delivery [ 1 ]. Healthcare systems have become increasingly multifaceted, delivering a vast array of services across multiple levels, from preventative and primary care to acute, specialized care, and long-term care, to address the care needs of a changing population [ 1 ]. As populations age, chronic diseases rise, and the epidemiology and demographics of disease shift, new models of care rapidly emerge to address the ever-expanding spectrum of patient needs [ 2 ]. Advancements in technologies, tests and treatments and personalized medicine come with regulatory and ethical implications, and a growth in workforce specializations [ 3 , 4 ]. Healthcare leaders are navigating evermore complex webs of actors in the system – doctors, nurses, technicians, administrators, insurers, and patients – striving to balance priorities, foster collaboration, and provide strategic direction toward high-quality and safe patient care [ 5 ]. At the same time as running complex services, healthcare leaders need to continually assess, implement, and govern new technologies and services, adhere to the latest regulations and guidelines, operate within the confines of budgetary allocations, and meet growing consumer expectations for affordable and accessible care [ 6 , 7 ].
Competent healthcare leadership is widely considered to be critical for improving patient safety, system performance, and the effectiveness of healthcare teams [ 8 , 9 , 10 ]. Leadership has been identified as a key shaping influence on organizational culture [ 11 ], including workplace commitment to safety [ 12 ], and on preventing workforce burnout [ 13 , 14 ]. The increased need for multidisciplinary and integrated care models has shed growing light on the leadership roles of clinicians, including physicians, nurses, and allied health practitioners [ 15 , 16 , 17 ]. Individuals with both clinical and leadership expertise have been considered vital in complex healthcare landscapes because of their ability to balance administrative needs while prioritizing safety and high-quality care provision [ 18 , 19 , 20 , 21 , 22 ]. For example, physician leaders, through their deep understanding of clinical care and their credibility and influence, have been considered best able to devise strategies that improve patient care amidst stringent financial conditions [ 23 , 24 , 25 , 26 ]. Clinical leaders, particularly physician leaders, might also be of key importance for facilitating the success of collaborative care and care integration [ 27 ].
The formalization of healthcare leadership emerged as the importance of specialized healthcare leadership skills became increasingly needed, recognized and understood [ 1 , 28 , 29 ]. Leadership in healthcare has been conceptualized in several different ways, and a multitude of theories, frameworks, and models have been proposed to explain leadership roles and responsibilities [ 30 , 31 , 32 , 33 ]. For example, the CanMEDS Framework describes the Leader Role of physicians, which is comprised of key and enabling competencies, tasks, and abilities [ 34 , 35 ], and adaptations to this Framework emphasize the varying roles that leadership comprises and the competencies that fulfill them [ 36 ]. Although these frameworks present a good starting point for articulating leadership role scopes and their associated competencies, many fall short in explaining how leaders navigate complex, dynamic, multi-dimensional, and highly variable healthcare systems [ 37 ]. This is becoming increasingly recognized; CanMEDS is due to be updated in 2025 to incorporate competencies related to complexity [ 38 ]. Meanwhile, on the front lines, lack of role clarity and ambiguity about tasks and responsibilities presents a significant barrier for healthcare leaders [ 1 , 15 ]. In complex and unpredictable systems like healthcare, leaders spend substantial time ‘sense-making’, understanding, prioritizing and responding adaptively according to the needs of the situation [ 39 , 40 ]. The latest research on future healthcare trends tells us that increasing complexity associated with digital innovation, healthcare costs, regulatory compliance, sustainability concerns and equitable resource distribution will pose challenges to all actors in health systems [ 41 , 42 , 43 , 44 , 45 ]. In the face of these emerging challenges, it is vital to understand the range and type of roles and competencies that leaders will need to fulfil in the imminent future.
The aim of this scoping review is to examine the literature on the key trends in roles and competencies required for healthcare leaders in the future. We conceptualized ‘competencies’ as the attributes, skills, and abilities that comprise the fulfilment of varying leadership roles, as informed by the CanMEDS Framework [ 34 , 36 ]. Scoping review methodology was utilized to capture a broad range of literature types and identify key themes or groupings of future trends in leadership roles and competencies. Rather than focusing on answering specific questions (as per previous systematic reviews on leadership [ 46 , 47 ]) or developing theory (by utilizing a theoretical review approach to leadership literature [ 48 , 49 ]), we sought to map and identify patterns and trends within the leadership literature [ 50 ]. To investigate trends in leadership roles and competencies, we targeted emerging perspectives from key reputable thought leaders to supplement academic research [ 51 , 52 ].
The conduct and reporting of this review followed the Preferred Reporting Items for Systematic Reviews and Meta-Analyses Extension for Scoping Reviews (PRISMA-ScR) guidelines [ 53 ].
Search strategy
Comprehensive search strategies were developed, adapting search strategies utilized in a previous systematic review on physician leadership [ 26 ], and receiving input and expertise from two clinical librarians at Macquarie University (see supplementary file 1 for database search strategies). Medline, Embase, and Business Source Premier were searched from January 2018 to February 2023 to enable meaningful inferences to be made about future trends based on current perspectives. To capture key trends, patterns, shifts, and forecast changes to healthcare leadership, the Medline database search was limited to the ‘Trends’ subheading, “ used for the manner in which a subject changes, qualitatively or quantitatively, with time, whether past, present, or future. Includes “forecasting” & “futurology" ” (see supplementary file 1 ) [ 54 ]. For Embase and Business Source Premier, the ‘Trends’ subheading was not available, and instead key search terms were included to capture future trends, including “predict*”, “forecast*”, “shift*” and “transform*”. Efforts were made to locate texts that could not be retrieved, by searching Macquarie University’s digital library records and contacting authors to request the full text.
To complement the database searches, targeted searches of the Faculty of Medical Leadership and Management (FMLM; UK) website and The King’s Fund (UK) website were undertaken to identify emerging perspectives on the future roles and requirements of healthcare leaders. Targeted website searches can aid in uncovering unpublished yet relevant research identified by advocacy organizations or subject specialists, and research potentially missed by database searches [ 52 , 55 ]. Key search terms entered into the websites included ‘future healthcare’, ‘medical leader’, ‘clinical leader’, ‘medical manager’, ‘physician executive’, and ‘education and training’. We included articles that focused on leaders with a clinical background and leaders without a clinical background, to provide a comprehensive overview of leadership roles and requirements of reference to health systems [ 26 ].
Article selection
Database literature search.
References were uploaded into online data management software Rayyan [ 56 ], and duplicate records were identified and removed. Titles and abstracts of results were screened by three team members (SS, EL, RP) according to the inclusion and exclusion criteria (Table 1 ). Articles were included if they focused on future trends in the roles, competencies, attributes, or requirements of healthcare leaders, and if they reported on countries within the Organization for Economic Co-operation and Development (OECD). We limited our search to OECD countries to maximize the generalizability of findings within a developed context and enable meaningful trends to be identified. A subset of the articles was screened by all three team members to ensure that decisions were being made in a standardized manner. After this article subset was screened, the three team members discussed screening decisions, and disagreements were resolved by consensus or through discussion with JB [ 57 ]. During this process, two further exclusion criteria (#4 and #5, Table 1 ) were added to ensure that the screening process adhered to the aim of the current review. We excluded articles that focused on theories and definitions of leadership (e.g., for the purpose of developing educational or professional frameworks) without highlighting trends or changes in roles and competencies for future leadership. We also excluded articles that focused on healthcare interventions in which leaders may have been participants, but their roles or competencies were not the focus. Articles included at title and abstract screening were independently read in full and assessed for eligibility. Disagreements about inclusion were resolved through discussion, with JB available for arbitration if necessary. It was determined at this stage that if articles were conference abstracts in which the full presentation could not be accessed, the article of focus was sought and included in the analysis.
Targeted gray literature search
References were screened according to the inclusion and exclusion criteria (Table 1 ), except that articles only needed to report (rather than focus) on future leadership roles and requirements. This is because we wanted to ensure that our analysis broadly captured the most recent sources of information on healthcare leadership requirements, even if these sources did not focus exclusively on leadership.
Data charting process
Data from all records were appraised and charted simultaneously using a purpose-designed Excel data charting form designed by SS (and subsequently reviewed and endorsed by RP and EL). Multimedia records arising from targeted gray literature searches were listened to and transcribed by RP and checked by SS. Extracted data included article details (authors, year, country, text type), leadership focus (training or educational approaches, styles of leadership), and major and minor themes. Database literature were extracted first to identify and develop themes, and the targeted gray literature were extracted second to extend and embellish those themes.
Synthesis of results
Data from included articles were synthesized according to the Arksey and O’Malley framework for scoping reviews, selected for its detailed guidance on data collation, synthesis, and presentation [ 58 ]. The breadth, range, and type of data were analyzed using descriptive statistics, and underlying groups of leadership roles and competencies were analyzed using thematic analysis. First, the authorship team familiarized themselves with the articles to gain a broad overview of contexts in which leadership was discussed. An inductive approach was used to identify emerging themes of leadership roles and competencies in the database literature, where common concepts were identified, coded, and grouped together to form themes. Team discussion facilitated the final set of themes that were interpreted from the data. During this process, the extracted data were compared to the codes, groups, and resultant themes to examine the degree of consistency between the data and the interpreted findings. Where inconsistencies were identified, suggested changes (e.g., to code labels or groupings) were compared, and the most appropriate changes adopted. Targeted gray literature sources were deductively analyzed according to the identified themes.
Selection of sources of evidence
Figure 1 displays the process of identification and screening of included studies. Database searches yielded 160 records, from which 11 duplicates were removed. The remaining 149 database records were screened by title and abstract, after which a further 114 records were excluded. Of the remaining 35 that were assessed for eligibility, 22 were excluded, and 13 were included in the current review. Targeted gray literature searches yielded an additional 188 records, from which 146 were identified as duplicates and removed. The remaining 42 records were read in full and assessed for eligibility, from which a further 16 were excluded, and 26 were included in the current review. In total, 39 records were retained and synthesized.

PRISMA flowchart displaying the process of identification and selection of included articles
Characteristics of sources of evidence
The characteristics of the included records are displayed in Tables 2 and 3 . Of the database literature, most articles were published in the USA ( n = 11), and the remaining two articles were published in Canada and Australia. Seven articles were empirical; three studies employed qualitative methods [ 59 , 60 , 61 ], three were quantitative [ 62 , 63 , 64 ], and one mixed methods [ 65 ]. Six articles were non-empirical; three were perspective pieces [ 66 , 67 , 68 ], and three were reports on training or organizational interventions [ 69 , 70 , 71 ]. Of the targeted literature, blog-type articles were most common ( n = 11) [ 72 , 73 , 74 , 75 , 76 , 77 , 78 , 79 , 80 , 81 , 82 ], followed by news articles ( n = 5) [ 83 , 84 , 85 , 86 , 87 ], reports ( n = 4) [ 88 , 89 , 90 , 91 ], editorials ( n = 2) [ 92 , 93 ], podcasts ( n = 2) [ 94 , 95 ], and video and interview transcripts ( n = 2) [ 96 , 97 ]. As targeted gray sources selected were The King’s Fund website and the FMLM website, the records from these websites were published in the UK.
Leadership roles and competencies
All 13 articles derived from the database searches focused on innovation and adaptation in future leadership. Two empirical articles reported on the ways in which clinical and non-clinical leaders innovated during the COVID-19 pandemic, rapidly designing new models of hospital care [ 61 ] and extending their roles to encompass the implementation of virtual leadership [ 64 ]. Qualitative investigations explored the importance of entrepreneurial leadership for implementing clinical genomics [ 59 ] and key leadership attributes for practice-level innovation and sustainability [ 60 ]. Four articles examined leadership training approaches that build physicians’ capacity to understand, adapt to, and manage change, overcome resistance, and think entrepreneurially [ 62 , 63 , 65 , 70 ]. Two reports described the necessity for healthcare leaders to be able to create a shared vision for an organization; one highlighted the importance of leaders being confident and “self-propelled to intervene” [ 69 ], and one emphasized physician leaders’ credibility as a catalyst for change management among healthcare providers [ 71 ]. The latter report also identified that visible and committed leadership that is sensitive to workplace cultures is critical for the success of change management activities [ 71 ]. Three perspective pieces discussed increasing opportunities for medical and other clinical leaders to create positive change in increasingly complex healthcare landscapes and fulfill the demands of the industry and public [ 66 , 67 , 68 ].
In the targeted gray literature, 19 of 26 records (73%) focused on innovative and adaptive leadership. Records primarily explored adaptive leadership behaviors during COVID-19, such as service redesign, introducing improved flexibility, learning mechanisms, and support platforms [ 73 , 76 , 77 , 97 ], and future innovation to manage climate change impacts [ 81 ], growing inequities [ 89 ], and emerging technologies [ 75 , 83 , 94 , 96 ]. Comfort with change, vision setting, and a desire to innovate were emphasized as key leadership attributes for future healthcare [ 82 , 83 , 88 , 96 ]. Records also explored how to best train and develop leaders for transforming health systems, including the National Health Service (NHS) [ 84 , 90 , 96 ]. New leadership training structures were proposed that foster innovation and adaptability in leaders [ 80 , 90 , 96 ] and encourage flexibility for cross-disciplinary learning.
Collaboration and communication was a second theme that emerged across all 13 database articles. Three studies explored how collaborative leadership can foster innovation with regards to implementing genomics testing [ 59 ], creating new work models during COVID-19 [ 61 ] and developing new leadership styles via telecommunications [ 64 ]. Six articles focused on the importance of collaborating to build relationships across organisations [ 67 , 68 , 71 ] and within teams [ 65 , 69 , 70 ]. Three articles highlighted that effective communication contributes to organizational success, through fostering psychologically safe cultures [ 60 , 66 ] and generating the trust and rapport necessary for implementing technological innovations [ 71 ]. Two studies examined the impact of leadership training on physicians’ communication competencies [ 62 , 63 ].
In the targeted gray literature, 17 of 26 records (65%) focused on collaboration and communication. Records discussed specific initiatives to improve communication in clinical teams, such as staff surveys, daily huddles, and dedicated days for networking [ 75 , 77 , 80 , 95 ]. Cross-boundary collaboration and collective leadership (e.g., between clinicians and managers) [ 83 ] were advocated as a means to solve challenges [ 81 , 90 ], help build public trust [ 79 , 83 ], and improve quality of care [ 78 , 83 , 85 , 94 ]. Twelve records focused on the importance of team and leadership collaboration to create positive workplace cultures and improve staff wellbeing, through communication strategies such as openness and honesty [ 78 , 80 , 95 ], active listening and empathy [ 73 , 78 , 86 , 88 , 90 ], transparency [ 88 , 94 , 95 ], and inclusivity [ 85 , 94 ]. Three articles emphasized that encouraging staff autonomy, building trust, and demonstrating compassion facilitate better quality care than demanding and punitive leadership actions [ 73 , 74 , 88 ].
Nine of 13 database articles (69%) focused on a third theme, self-development and self-awareness in leadership. Four articles examined approaches to leadership development that incorporated self-development and self-awareness (e.g., personality testing) [ 63 , 65 , 69 , 70 ], with two articles describing these competencies as enablers for the development of other more advanced competencies (e.g., execution) [ 69 , 70 ]. Similar competencies explored included landscape awareness [ 60 ], self-organisation [ 60 ], emotional intelligence [ 64 ], and self-examination, the last of which was described as essential to gain skills beyond clinical roles [ 68 ], facilitate positive perceptions of others [ 66 ], and to remain relevant and effective in a changing healthcare environment [ 67 ]. One article also proposed strategies such as journaling, mindfulness, and feedback to encourage ongoing reflection on leadership decisions and biases [ 67 ].
In the targeted gray literature, seven of 26 records (27%) focused on self-development and self-awareness. Records examinedd the importance of continual personal leadership development, including mentoring and experiential learning, to facilitate understanding of one’s own skills [ 78 , 80 , 97 ]. Tools to facilitate self-reflection in physician leaders were advocated including the FMLM smartphone app [ 92 ] and leadership longitudinal assessments [ 91 ]. Self-care and resilience practices (e.g., meditation, social support) were also advocated for physician leaders as a means to manage “greater levels of stress and responsibility” [ 94 ].
Consumer engagement and advocacy was a fourth theme and a focus of nine targeted gray literature records (35%). Records discussed patient and community engagement as essential for health system improvement, and examples included involving patients in health service design [ 74 , 77 ], creating channels of ongoing dialogue [ 79 , 83 ] and building stronger health system-community relationships [ 79 , 88 ]. Two records described the importance of public health messaging in improving health literacy [ 83 ] and countering misinformation [ 86 ], and two focused on the role of leaders in advocating for social justice and striving to improve equitable outcomes [ 75 , 93 ].
This scoping review identified 39 key resources that explored future trends in healthcare leadership roles and competencies. These records were derived from a combination of academic and targeted gray literature searches, juxtaposed and synthesized to build understanding of leadership to improve health systems into the future. Four themes of competencies emerged from the findings – innovation and adaptation, communication and collaboration, self-development and self-awareness, and consumer engagement and advocacy.
The competencies of healthcare leaders given the most attention in the literature over the last five years relate to innovation and adaptability . Both the academic and targeted gray literature focused on how leaders, clinical and non-clinical, demonstrated innovativeness and adapted to the demands of COVID-19, including rethinking and redesigning systems to support staff and patients [ 64 , 77 ]. The second focus of the literature on innovation and adaptability was geared toward the development of these capacities in leaders through education and training, as well as through opportunities for leaders to actualize their skills [ 70 , 90 ]. The literature indicated that as the complexity of healthcare is accelerating, leaders must both understand, and have opportunities to demonstrate, innovation amidst dynamic, variable, and demanding environments [ 59 , 60 , 71 ]. This aligns with prior research demonstrating that innovation uptake requires strong change management, and the ability to rapidly assess, understand, and apply innovative changes (e.g., medical technologies) [ 1 , 98 ]. While innovations might improve the system’s ability to deal with complex challenges in the long-term, their implementation can be challenged by a number of moving parts – including workforce changes, new rules and regulations, fluctuating resources and new patient groups – which leaders must consider and appropriately plan for [ 99 , 100 ]. Perhaps an even greater challenge for leaders to overcome when embracing innovation is the tendency for growing complexity to lock the organization into suboptimal conditions (i.e., inertia) [ 101 ]. Building awareness of the interacting components of complex systems and the flexibility required for adaptation and resilience should be a key focus of healthcare leadership education and training [ 102 ].
Competencies associated with communication and collaboration have also been a focus of the healthcare leadership literature. Academic literature dealt primarily with how collaborative structures and behaviors can help leaders innovate and build organizational cultures geared for success [ 59 , 61 , 71 ]. Targeted gray literature focused on how leaders can foster communication within teams, and the positive impacts of an open and accountable culture on staff wellbeing and productivity [ 73 , 74 ]. These findings echo research on resilient health systems emphasizing that ‘over-managing’ restricts the adaptive capacities needed by teams within dynamic healthcare environments [ 100 , 103 ]. The literature pointed to the need for leaders to strengthen communication and collaboration at varying levels – environmental, team, and organizational – to enable more efficient and better-quality healthcare delivery, and during this process they should endeavor to model the balance between autonomy and accountability [ 104 ]. Implementing regular touchpoints that engage multiple stakeholders, such as communities of practice, can help to create positive feedback loops that enable systems change [ 105 ], and overcome organizational barriers to collaboration and information sharing, such as weak relationships and inadequate communication [ 106 , 107 ].
Self-development and self-awareness also emerged as an important aspect of leadership. Academic literature focused primarily on how these capacities are developed in leaders through structured education and training, including self-assessments and targeted educational modules [ 65 , 69 ]. Targeted gray literature discussed a range of activities outside of structured training (e.g., experiential learning) that can support leaders’ self-reflection and development, for physician leaders in particular to assess their performance and improve their leadership approaches [ 91 , 92 ]. These findings suggest that personal leadership development must go beyond formal curriculum requirements to incorporate everyday learning inputs [ 78 ], and align with other recent literature suggesting that self-regulation in leaders can be fostered through practicing self-discipline, boundary-setting, and managing disruptions, particularly in the digital age [ 108 , 109 ]. Practicing self-awareness can help leaders not only to sense-make in complex systems – to adapt to new situations and make appropriate trade-offs – but also to sense-give – to articulate and express the organization’s vision [ 40 ]. A minor theme, observed only in the targeted gray literature, was related to leaders’ roles and competencies in consumer engagement and advocacy . The importance of increasing consumer engagement in healthcare was emphasized, as well as the structures that are needed to facilitate these changes [ 79 ]. Working alongside consumers was highlighted as critical during times of changing care and need, such as during COVID-19 [ 77 , 86 ]. Although the involvement of consumers and the public in the co-production of care is increasing [ 110 ], there is limited academic literature focused on the roles of leaders in creating optimal environments for co-production. Consumer and community involvement in change efforts helps to improve care processes and outcomes [ 111 ], but leaders might face challenges understanding and operationalizing local engagement mechanisms [ 112 ]. Identifying the organizational and system levers that enable greater consumer involvement, and how leaders can advocate for these levers in their local context, is a fruitful area for future investigation.
The findings of the current review have implications for professional organizations that train healthcare leaders, such as the Australian College of Health Services Management (ACHSM) in Australia, and train clinicians to be leaders, including the UK’s FMLM. Creating a future-focused curriculum addressing the competencies related to the themes identified, in particular innovation and adaptability, is essential to prepare healthcare leaders for growing and changing scopes of responsibility. Such competencies are less amenable to formal theoretical teaching solely and require carefully crafted experiential learning programs in health settings, with supervision by experienced and effective healthcare leaders.
Strengths and limitations
A notable strength of this scoping review was the inclusion of a broad range of sources and perspectives on the future of healthcare leadership. We captured empirical studies, theoretical academic contributions (e.g., commentaries from healthcare leaders), and targeted grey literature, which is often a more useful source of information on emerging topics [ 52 ]. As a result, our findings identified key future trends in the roles and competencies of leaders, both clinical and non-clinical, across a wide range of contexts and situations. Another strength of this review was its specific focus on contemporary literature that examined future trends in leadership, to inform how leaders can prepare for upcoming challenges, rather than focusing on leadership that was effective in the past.
There are limitations to this review. Our search strategies may not have adequately captured other leadership trends applicable across contemporary healthcare settings or those faced by leaders and teams on the front lines of care [ 113 ]. Incorporating search terms related to specific settings, as well as complex systems concepts, may have enabled greater inferences to be made about how unique future challenges require new approaches to the development of healthcare leaders. To scope future-focused research and perspectives, database searches were narrowly restricted, and it is likely that key articles were missed. Targeted gray literature searches represent key thought leaders in healthcare and leadership, and while this enabled relevant information to be efficiently collected, undertaking highly focused searches may have introduced bias associated with geographical area (i.e., the UK) and particular stakeholder groups (e.g., policy-makers) [ 55 ]. Our choice to limit the current review to studies reporting in OECD countries further limited generalizability to other settings including in low-income and middle-income countries (LMICs) [ 1 ].
The roles and competencies of leaders are deeply enmeshed in, and reflective of, a complex and continuously transforming healthcare system. This research highlights the types of roles and competencies important for leaders facing a myriad of challenges, and the range of contexts and situations in which these types of roles and competencies can be applied. The ways in which roles and competencies manifest is highly contextual, dependent on both role responsibilities and the situational demands of healthcare environments.
Data availability
Data supporting these research findings are available upon reasonable request. Further inquiries can be directed to the corresponding author.
Abbreviations
Faculty of Medical Leadership and Management
National Health Service
Preferred Reporting Items for Systematic Reviews and Meta-Analyses Extension for Scoping Reviews
Royal Australasian College of Medical Administrators
United States of America
United Kingdom
Figueroa CA, Harrison R, Chauhan A, et al. Priorities and challenges for health leadership and workforce management globally: a rapid review. BMC Health Serv Res. 2019;19:1–11. https://doi.org/10.1186/s12913-019-4080-7
Article Google Scholar
Braithwaite J, Mannion R, Matsuyama Y, et al. The future of health systems to 2030: a roadmap for global progress and sustainability. Int J Qual Health Care. 2018;30(10):823–31. https://doi.org/10.1093/intqhc/mzy242
Anklam E, Bahl MI, Ball R, et al. Emerging technologies and their impact on regulatory science. Exp Biol Med. 2022;247(1):1–75. https://doi.org/10.1177/15353702211052280
Maeda A, Socha-Dietrich K. Skills for the future health workforce: preparing health professionals for people-centred care. OECD Health Working Papers. Paris: OECD Publishing,; 2021.
Reich MR, Javadi D, Ghaffar A. Introduction to the special issue on effective leadership for health systems. Health Syst Reform. 2016;2(3):171–5. https://doi.org/10.1080/23288604.2016.1223978
Shaw J, Brewer LC, Veinot T. Recommendations for health equity and virtual care arising from the COVID-19 pandemic: narrative review. JMIR Form Res. 2021;5(4):e23233. https://doi.org/10.2196/23233
Graham R, Woodhead T. Leadership for continuous improvement in healthcare during the time of COVID-19. Clin Radiol. 2021;76(1):67–72. https://doi.org/10.1016/j.crad.2020.08.008
Parr JM, Teo S, Koziol-McLain J. A quest for quality care: exploration of a model of leadership relationships, work engagement, and patient outcomes. J Adv Nurs. 2021;77(1):207–20. https://doi.org/10.1111/jan.14583
Ree E, Wiig S. Linking transformational leadership, patient safety culture and work engagement in home care services. Nurs Open. 2020;7(1):256–64. https://doi.org/10.1002/nop2.386
Wu X, Hayter M, Lee AJ, et al. Positive spiritual climate supports transformational leadership as means to reduce nursing burnout and intent to leave. J Nurs Manag. 2020;28(4):804–13. https://doi.org/10.1111/jonm.12994
West M, Armit K, Loewenthal L, et al. Leadership and leadership development in health care: the evidence base. London: The King’s Fund; 2015.
Google Scholar
Churruca K, Ellis LA, Pomare C, et al. Dimensions of safety culture: a systematic review of quantitative, qualitative and mixed methods for assessing safety culture in hospitals. BMJ Open. 2021;11(7):e043982. https://doi.org/10.1136/bmjopen-2020-043982
Smallwood N, Bismark M, Willis K. Burn-out in the health workforce during the COVID-19 pandemic: opportunities for workplace and leadership approaches to improve well-being. BMJ Lead. 2023;leader–2022. https://doi.org/10.1136/leader-2022-000687
Kelly RJ, Hearld LR. Burnout and leadership style in behavioral health care: a literature review. J Behav Health Serv Res. 2020;47(4):581–600. https://doi.org/10.1007/s11414-019-09679-z
Hutchinson K, Ryder T, Coleman H, et al. Determining the role and responsibilities of the community epilepsy nurse in the management of epilepsy. J Clin Nurs. 2023;32(13–14):3730–45. https://doi.org/10.1111/jocn.16582
Mianda S, Voce A. Developing and evaluating clinical leadership interventions for frontline healthcare providers: a review of the literature. BMC Health Serv Res. 2018;18(1):1–15. https://doi.org/10.1186/s12913-018-3561-4
Veronesi G, Kirkpatrick I, Vallascas F. Clinicians on the board: what difference does it make? Soc Sci Med. 2013;77:147–55. https://doi.org/10.1016/j.socscimed.2012.11.019
Ferreira TDM, de Mesquita GR, de Melo GC, et al. The influence of nursing leadership styles on the outcomes of patients, professionals and institutions: an integrative review. J Nurs Manag. 2022;30(4):936–53. https://doi.org/10.1111/jonm.13592
Boamah SA. Emergence of informal clinical leadership as a catalyst for improving patient care quality and job satisfaction. J Adv Nurs. 2019;75(5):1000–9. https://doi.org/10.1111/jan.13895
Dickinson H, Ham C. Engaging doctors in leadership: review of the literature. Birmingham: University of Birmingham; 2008.
Hershkovich O, Gilad D, Zimlichman E, et al. Effective medical leadership in times of emergency: a perspective. Disaster Mil Med. 2016;2:1–5. https://doi.org/10.1186/s40696-016-0013-8
Stoller JK. Developing physician-leaders: a call to action. J Gen Intern Med. 2009;24:876–8. https://doi.org/10.1007/s11606-009-1007-8
Warren OJ, Carnall R. Medical leadership: why it’s important, what is required, and how we develop it. Postgrad Med J. 2011;87(1023):27–32. https://doi.org/10.1136/pgmj.2009.093807
Griffith R. NHS management inquiry: report to the secretary of state for social services. London: Department of Health and Social Security; 1983.
Braithwaite J. Changing how we think about healthcare improvement. BMJ. 2018;361. https://doi.org/10.1136/bmj.k2014
Clay-Williams R, Ludlow K, Testa L, et al. Medical leadership, a systematic narrative review: do hospitals and healthcare organisations perform better when led by doctors? BMJ Open. 2017;7(9):e014474. https://doi.org/10.1136/bmjopen-2016-014474
Nieuwboer MS, van der Sande R, van der Marck MA, et al. Clinical leadership and integrated primary care: a systematic literature review. Eur J Gen Pract. 2019;25(1):7–18. https://doi.org/10.1080/13814788.2018.1515907
Dwyer AJ. Roles, attributes and career paths of medical administrators in public hospitals: survey of victorian metropolitan directors of Medical services. Aust Health Rev. 2010;34(4):506–13. https://doi.org/10.1071/AH09750
Dwyer AJ. Medical managers in contemporary healthcare organisations: a consideration of the literature. Aust Health Rev. 2010;34(4):514–22. https://doi.org/10.1071/AH09736
Health Workforce Australia. Health LEADS Australia: the Australian health leadership framework. Adelaide: Health Workforce Australia; 2013.
NHS Institute for Innovation and Improvement and Academy of Medical Royal Colleges. Medical leadership competency framework: enhancing engagement in medical leadership. Coventry: NHS Institute for Innovation and Improvement; 2010.
National Centre for Healthcare Leadership. NCHL Health Leadership Competency Model 3.0. National Centre for Healthcare Leadership. 2022. https://www.nchl.org/research/ . Accessed 28 December, 2023.
NHS Leadership Academy. Healthcare Leadership Model: the nine dimensions of leadership behaviour. Leeds: NHS Leadership Academy; 2013.
Frank JR, Snell L, Sherbino J, et al. CanMEDS 2015 Physician Competency Framework. Royal College of Physicians and Surgeons of Canada; 2015.
Dath DCM-K, Anderson G, Burke A, Razack S, Lieff S, Moineau G, Chiu A, Ellison P. Leader. In: Frank JRSL, Sherbino J, editors. CanMEDS 2015 Physician Competency Framework. Royal College of Physicians and Surgeons of Canada; 2015.
Royal Australasian College of Medical Administrators. Medical Leadership and Management Curriculum Framework. Malvern, Victoria: Royal Australasian College of Medical Administrators; 2011.
Best S, Stark Z, Brown H, et al. The leadership behaviors needed to implement clinical genomics at scale: a qualitative study. Genet Med. 2020;22(8):1384–90. https://doi.org/10.1038/s41436-020-0818-1
Thoma B, Karwowska A, Samson L, et al. Emerging concepts in the CanMEDS physician competency framework. Can Med Educ J. 2023;14(1):4–12. https://doi.org/10.36834/cmej.75591
Ahern S, Loh E. Leadership during the COVID-19 pandemic: building and sustaining trust in times of uncertainty. BMJ Lead. 2020;leader–2020. https://doi.org/10.1136/leader-2020-000271
Braithwaite J, Churruca K, Hibbert P, et al. At the heart of getting things done in complex healthcare ecosystems: leadership, strategy, sensemaking and sensegiving. In: Chambers N, editor. Research Handbook on Leadership in Healthcare. Edward Elgar Publishing; 2023. pp. 775–92.
Braithwaite J, Fisher G. Beyond the aspirational: creating the future of health care in Australia. Int Med J. 2024;54(2):342–7. https://doi.org/10.1111/imj.16286
Cernega A, Nicolescu DN, Meleșcanu Imre M, et al. Volatility, uncertainty, complexity, and ambiguity (VUCA) in healthcare. Healthc. 2024;12(7):773. https://doi.org/10.3390/healthcare12070773
Kasula BY. Revolutionizing healthcare delivery: innovations and challenges in supply chain management for improved patient care. Trans Latest Trends Health Sect. 2023;15(15).
Niaz M, Nwagwu U. Managing healthcare product demand effectively in the post-covid-19 environment: navigating demand variability and forecasting complexities. Am J Econ Manag Bus. 2023;2(8):316–30. https://doi.org/10.58631/ajemb.v2i8.55
Thirumalai S, Devaraj S. Mitigating the curse of complexity: the role of focus and the implications for costs of care. J Oper Manag. 2024;70(1):157–79. https://doi.org/10.1002/joom.1278
Savage M, Savage C, Brommels M, et al. Medical leadership: boon or barrier to organisational performance? A thematic synthesis of the literature. BMJ Open. 2020;10(7):e035542. https://doi.org/10.1136/bmjopen-2019-035542
Ahti M, Taipale-Walsh L, Kuha S, et al. Health-care leaders’ experiences of the competencies required for crisis management during COVID-19: a systematic review of qualitative studies. Leadersh Health Serv. 2023. https://doi.org/10.1108/LHS-10-2022-0104
Krasikova DV, Green SG, LeBreton JM. Destructive leadership: a theoretical review, integration, and future research agenda. J Manag. 2013;39(5):1308–38. https://doi.org/10.1177/0149206312471388
Pellegrini MM, Ciampi F, Marzi G, et al. The relationship between knowledge management and leadership: mapping the field and providing future research avenues. J Knowl Manag. 2020;24(6):1445–92. https://doi.org/10.1108/JKM-01-2020-0034
Paré G, Trudel M-C, Jaana M, et al. Synthesizing information systems knowledge: a typology of literature reviews. Inf Manag. 2015;52(2):183–99. https://doi.org/10.1016/j.im.2014.08.008
Heath A, Levay P, Tuvey D. Literature searching methods or guidance and their application to public health topics: a narrative review. Health Info Libr J. 2022;39(1):6–21. https://doi.org/10.1111/hir.12414
Adams J, Hillier-Brown FC, Moore HJ, et al. Searching and synthesising ‘grey literature’and ‘grey information’in public health: critical reflections on three case studies. Syst Rev. 2016;5(1):1–11. https://doi.org/10.1186/s13643-016-0337-y
Tricco AC, Lillie E, Zarin W, et al. PRISMA extension for scoping reviews (PRISMA-ScR): checklist and explanation. Ann Intern Med. 2018;169(7):467–73. https://doi.org/10.7326/M18-0850
Wolters Kluwer Health I. Get to know the advantages of Ovid MEDLINE ® . 2024. https://tools.ovid.com/ovidtools/medline.html . Accessed.
Stansfield C, Dickson K, Bangpan M. Exploring issues in the conduct of website searching and other online sources for systematic reviews: how can we be systematic? Syst Rev. 2016;5:1–9. https://doi.org/10.1186/s13643-016-0371-9
Ouzzani M, Hammady H, Fedorowicz Z, et al. Rayyan—a web and mobile app for systematic reviews. Syst Rev. 2016;5:1–10. https://doi.org/10.1186/s13643-016-0384-4
Peters MD, Marnie C, Tricco AC, et al. Updated methodological guidance for the conduct of scoping reviews. JBI Evid Synth. 2020;18(10):2119–26. https://doi.org/10.11124/JBIES-20-00167
Arksey H, O’Malley L. Scoping studies: towards a methodological framework. Int J Soc Res Methodol. 2005;8(1):19–32. https://doi.org/10.1080/1364557032000119616
Best S, Long J, Stark Z, et al. Clinical leadership and genomics - what works? Twin Res Hum Genet. 2019;22(5):350. 43rd Annual Scientific Meeting of the Human Genetics Society of Australasia, HGSA 2019. Wellington New Zealand.
Crabtree BF, Howard J, Miller WL, et al. Leading innovative practice: leadership attributes in LEAP practices. Milbank Q. 2020;98(2):399–445. https://doi.org/10.1111/1468-0009.12456
Woiceshyn J, Huq JL, Kannappan S, et al. We need to work differently in a crisis: peer-professional leadership to redesign physicians’ work. BMJ Lead. 2022;6(2):98–103. https://doi.org/10.1136/leader-2021-000490
Appelbaum NP, Liang C, Whitney SE, et al. What business competencies are needed for the modern physician leader and when. Physician Leadersh J. 2022;9(2):39–45.
Hopkins J, Fassiotto M, Ku MC, et al. Designing a physician leadership development program based on effective models of physician education. Health Care Manage Rev. 2018;43(4):293–302. https://doi.org/10.1097/HMR.0000000000000146
Sandberg DS, Pennington CM, Lindquist MA. Virtual leadership: CEOs and C-Level executives of healthcare organizations in the United States reimagined new roles as virtual leaders. J Leadersh Stud. 2022;16(3):61–9. https://doi.org/10.1002/jls.21827
Satiani B, Dawson K, Mehta LS, et al. Lessons learned after implementing an academic faculty leadership program over seven years. Physician Leadersh J. 2022;9(2):30–8.
Angood PB. Transitions and transformations — our choice? Physician Leadersh J. 2022;9(5):6–8.
Brace R, James D. Adapting to changing roles. J Healthc Manag. 2020;35(3):46–7.
Wright C, Pister K. New thinking leads to better transitions. Physician Leadersh J. 2018;5(1):38–40.
Ramirez B, West DJ Jr, Ramirez CL. Healthcare and leadership competencies, training methods, and venues. J Leadersh Acc Ethics. 2021;18(4):93–9.
Wain MJ, Handel DA, Williford K, et al. Transitioning from physician to hospital leader: a competency-based model. Physician Leadersh J. 2020;7(2):32–3.
Borgwardt HL, Botz CT, Doppler JM, et al. Electronic health record implementation: the people side of change. Manage Healthc. 2019;4(1):7–20.
Anandaciva S. The biggest hospital in England. The King’s Fund . 2020. https://www.kingsfund.org.uk/blog/2020/09/biggest-hospital-england . Accessed 25 February, 2023.
Bailey S, West M. Learning from staff experiences of Covid-19: let the light come streaming in. The King’s Fund . 2020. https://www.kingsfund.org.uk/blog/2020/06/learning-staff-experiences-covid-19 . Accessed 26 February, 2023.
Bailey S, West M. Naming the issue: chronic excessive workload in the NHS. The King’s Fund . 2021. https://www.kingsfund.org.uk/blog/2021/06/naming-issue-chronic-excessive-workload-nhs . Accessed 26 February, 2023.
Bhopal A, Hood G. From disaster preparedness to digital disruption: A whistle-stop tour through public health. Faculty of Medical Leadership and Management. 2018. https://www.fmlm.ac.uk/news-opinion/from-disaster-preparedness-to-digital-disruption-a-whistle-stop-tour-through-public . Accessed 27 February, 2023.
Cheetham J. How Leaders in Healthcare 2020 gave an enlightened spotlight to junior doctor leadership. Faculty of Medical Leadership and Management. 2021. https://www.fmlm.ac.uk/news-opinion/how-leaders-in-healthcare-2020-gave-an-enlightened-spotlight-to-junior-doctor . Accessed 27 February, 2023.
Collins B. Leadership and innovation during Covid-19: lessons from the Cardiff and Vale Health System. The King’s Fund . 2021. https://www.kingsfund.org.uk/blog/2021/05/leadership-innovation-covid-19-cardiff-vale . Accessed 27 February, 2023.
Cottey L. The trainee and the team. Faculty of Medical Leadership and Management. 2018. https://www.fmlm.ac.uk/news-opinion/the-trainee-and-the-team . Accessed 28 February, 2023.
Dixon M. Engaging the public in designing the future for the NHS. The King’s Fund . 2018. https://www.kingsfund.org.uk/blog/2018/01/engaging-public-designing-future-nhs . Accessed 28 February, 2023.
Leveson D. Developing clinical leaders through innovation. The King’s Fund . 2021. https://www.kingsfund.org.uk/blog/2021/03/developing-clinical-leaders-through-innovation . Accessed 25 February, 2023.
Naylor C. Getting to grips with climate change: how can the NHS get to net zero? The King’s Fund . 2020. https://www.kingsfund.org.uk/blog/2020/01/climate-change-nhs-net-zero . Accessed 19 February, 2023.
Tweedie J. Leadership - so what is it anyway? February, 2018. https://www.fmlm.ac.uk/news-opinion/blog/leadership-so-what-is-it-anyway
Faculty of Medical Leadership and Management. FMLM response to HEE’s Call for Evidence on the Future Doctor. Faculty of Medical Leadership and Management. 2019. https://www.fmlm.ac.uk/news-opinion/fmlm-response-to-hees-call-for-evidence-on-the-future-doctor . Accessed 23 February, 2023.
Faculty of Medical Leadership and Management. Supporting and developing a leading resource for the future. Faculty of Medical Leadership and Management. 2021. https://www.fmlm.ac.uk/news-opinion/supporting-and-developing-a-leading-resource-for-the-future . Accessed 27 February, 2023.
Faculty of Medical Leadership and Management. Support, wellbeing and leadership. Faculty of Medical Leadership and Management. 2021. https://www.fmlm.ac.uk/news-opinion/support-wellbeing-and-leadership . Accessed 27 February, 2023.
Faculty of Medical Leadership and Management. Reflections from the International Healthcare Leadership Conference. 2022. Faculty of Medical Leadership and Management. 2022. https://www.fmlm.ac.uk/news-opinion/reflections-from-the-international-healthcare-leadership-conference-2022 . Accessed 27 February, 2023.
Lakhani M, Osuji N, Lees P et al. FMLM statement: racism and good leadership are incompatible. Faculty of Medical Leadership and Management. 2020. https://www.fmlm.ac.uk/news-opinion/fmlm-statement-racism-and-good-leadership-are-incompatible . Accessed 28 February, 2023.
Dougall D, Ross S. Transformational change in health and care: reports from the field. 2018. Accessed February, 2023. The King’s Fund.
Fogden R, Buck D, Franklin B et al. Poverty and the health and care system: the role of data and partnership in bringing change. The King’s Fund . 2022. https://www.kingsfund.org.uk/publications/poverty-health-care-system-data-partnership . Accessed 27 February, 2023.
Ham C, Murray R. The NHS 10-year plan: how should the extra funding be spent. The King’s Fund . 2018. https://www.kingsfund.org.uk/publications/nhs-10-year-plan . Accessed 28 February, 2023.
Swanwick T, McKimm J. The assessment of leadership development in the medical undergraduate curriculum: a consensus statement. Faculty of Medical Leadership and Management. 2020. https://www.fmlm.ac.uk/resources/the-assessment-of-leadership-development-in-the-medical-undergraduate-curriculum-a . Accessed 22 February, 2023.
Evans P. A radical upward shift to benefit members and fellows. Faculty of Medical Leadership and Management. 2020. https://www.fmlm.ac.uk/news-opinion/a-radical-upward-shift-to-benefit-members-and-fellows . Accessed 22 February, 2023.
Lakhani M. Black History Month and why it matters. Faculty of Medical Leadership and Management. 2021. https://www.fmlm.ac.uk/news-opinion/black-history-month-and-why-it-matters . Accessed 28 February, 2023.
Moralee S, Exworthy M, Rajasingam D et al. What next for medical leaders? Faculty of Medical Leadership and Management. 2018. https://www.fmlm.ac.uk/resources/what-next-for-medical-leaders . Accessed 25 February, 2023.
Warren S, Laverty A. Leading with compassion: supporting the health and wellbeing of NHS staff. The King’s Fund . 2022. https://www.kingsfund.org.uk/audio-video/podcast/leading-compassion-health-wellbeing-nhs-staff . Accessed 22 February, 2023.
Hancock M. Matt Hancock at The King’s Fund annual conference 2018. 2018. https://www.kingsfund.org.uk/audio-video/matt-hancock-kings-fund-annual-conference-2018 . Accessed.
Olsson-Brown A, Interview with Dr Anna Olsson-Brown - Chair of the Academy of Medical Royal Colleges Trainee Group. Faculty of Medical Leadership and Management. 2020. https://www.fmlm.ac.uk/news-opinion/interview-with-dr-anna-olsson-brown-chair-of-the-academy-of-medical-royal-colleges . Accessed 19 February, 2023.
Denicolai S, Previtali P. Innovation strategy and digital transformation execution in healthcare: the role of the general manager. Technovation. 2023;121:102555. https://doi.org/10.1016/j.technovation.2022.102555
Borges do Nascimento IJ, Abdulazeem H, Vasanthan LT, et al. Barriers and facilitators to utilizing digital health technologies by healthcare professionals. NPJ Digit Med. 2023;6(1):161. https://doi.org/10.1038/s41746-023-00899-4
Braithwaite J, Churruca K, Ellis LA, et al. Complexity science in healthcare: aspirations, approaches, applications, and accomplishments. A white paper. Sydney: Australian Institute of Health Innovation, Macquarie University; 2017.
Coiera E. Why system inertia makes health reform so difficult. BMJ. 2011;342 https://doi.org/10.1136/bmj.d3693
Clay-Williams R, Travaglia J, Hibbert P, et al. Clinical Governance Framework. A Report prepared for the Royal Australasian College of Medical Administrators (RACMA). Melbourne: RACMA; 2017.
Plsek PE, Wilson T. Complexity, leadership, and management in healthcare organisations. BMJ. 2001;323(7315):746–9. https://doi.org/10.1136/bmj.323.7315.746
van Diggele C, Burgess A, Roberts C, et al. Leadership in healthcare education. BMC Med Educ. 2020;20:1–6. https://doi.org/10.1186/s12909-020-02288-x
Golden RE, Klap R, Carney DV, et al. Promoting learning health system feedback loops: experience with a VA practice-based research network card study. Healthc. 2021;8:100484. https://doi.org/10.1016/j.hjdsi.2020.100484
Smith CL, Fisher G, Dharmayani PNA, et al. Progress with the Learning Health System 2.0: a rapid review of Learning Health Systems’ responses to pandemics and climate change. BMC Med. 2024;22(1):131. https://doi.org/10.1186/s12916-024-03345-8
Hunt RC, Struminger BB, Redd JT, et al. Virtual peer-to-peer learning to enhance and accelerate the health system response to COVID-19: the HHS ASPR Project ECHO COVID-19 Clinical rounds Initiative. Ann Emerg Med. 2021;78(2):223–8. https://doi.org/10.1016/j.annemergmed.2021.03.035
Mander R, Hellert U, Antoni CH. Self-leadership strategies for coping with flexibility requirements of digital work with a high degree of latitude for time, place and scope for action—a qualitative study. Gr Interakt Org. 2021;52:163–71. https://doi.org/10.1007/s11612-021-00560-2
Vay C, Steinherr V. Leadership in a digitalized and crisis-ridden world: towards a comprehensive overview of relevant competencies for leaders. University of Hawaiʻi at Mānoa; 2023.
Churruca K, Pomare C, Ellis LA, et al. Patient-reported outcome measures (PROMs): a review of generic and condition‐specific measures and a discussion of trends and issues. Health Expect. 2021;24(4):1015–24. https://doi.org/10.1111/hex.13254
Best A, Greenhalgh T, Lewis S, et al. Large-system transformation in health care: a realist review. Milbank Q. 2012;90(3):421–56. https://doi.org/10.1111/j.1468-0009.2012.00670.x
Bolden R, Kars-Unluoglu S, Jarvis C, et al. Paradoxes of multi-level leadership: insights from an integrated care system. J Change Manag. 2023;23(4):337–57. https://doi.org/10.1080/14697017.2023.2234388
Braithwaite J, Dammery G, Spanos S, et al. Learning health systems 2.0: future-proofing healthcare against pandemics and climate change. A White Paper. Sydney: Australian Institute of Health Innovation, Macquarie University; 2023.
Download references
Acknowledgements
The authors thank Mary Simons and Jeremy Cullis for their specialist guidance on database searches.
This work was funded in part by RACMA. RACMA contributed to the conceptualization and design of the research. JB is funded and supported by an NHMRC Leadership Investigator Award (1176620).
Author information
Authors and affiliations.
Centre for Healthcare Resilience and Implementation Science, Australian Institute of Health Innovation, Macquarie University, 75 Talavera Rd, North Ryde, Sydney, NSW, 2109, Australia
Samantha Spanos, Elle Leask, Romika Patel, Michael Datyner & Jeffrey Braithwaite
Royal Australasian College of Medical Administrators, Melbourne, VIC, Australia
You can also search for this author in PubMed Google Scholar
Contributions
JB and SS led the research conception and design. SS, ELe, and RP executed the research, and acquired, and analyzed the data. JB, SS, and MD significantly contributed to the interpretation of the data. SS wrote the original manuscript draft which was critically reviewed by JB, ELe, RP, MD and ELo. SS led the manuscript revisions with significant contribution from JB, and input from ELe, RP, MD, and ELo. All authors agree on the journal to which the article will be submitted, have reviewed, and approved the manuscript, and agree to be personally accountable for its contents.
Corresponding author
Correspondence to Samantha Spanos .
Ethics declarations
Ethics approval and consent to participate.
Not applicable.
Consent for publication
Competing interests.
The authors declare no competing interests.
Additional information
Publisher’s note.
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Supplementary Material 1
Rights and permissions.
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/ . The Creative Commons Public Domain Dedication waiver ( http://creativecommons.org/publicdomain/zero/1.0/ ) applies to the data made available in this article, unless otherwise stated in a credit line to the data.
Reprints and permissions
About this article
Cite this article.
Spanos, S., Leask, E., Patel, R. et al. Healthcare leaders navigating complexity: a scoping review of key trends in future roles and competencies. BMC Med Educ 24 , 720 (2024). https://doi.org/10.1186/s12909-024-05689-4
Download citation
Received : 13 February 2024
Accepted : 21 June 2024
Published : 03 July 2024
DOI : https://doi.org/10.1186/s12909-024-05689-4
Share this article
Anyone you share the following link with will be able to read this content:
Sorry, a shareable link is not currently available for this article.
Provided by the Springer Nature SharedIt content-sharing initiative
- Physician leadership
- Future health care
- Future healthcare
- Complex systems
BMC Medical Education
ISSN: 1472-6920
- Submission enquiries: [email protected]
- General enquiries: [email protected]
Rule of Law Enhancement, Innovation Incentives, and Business Performance: Evidence from China’s IPCs
- Published: 08 July 2024
Cite this article

- Wang Hao 1 ,
- Liu Chengkui 1 ,
- Yu Yue 1 &
- Lin Xiaodan 1
This study aims to determine the relationship between judicial protection of intellectual property rights (IPRs), innovation, and firm performance. Using the establishment of intellectual property courts (IPCs) by the Chinese government in Beijing, Shanghai, and Guangzhou in 2014 as a quasi-natural experiment, we build a difference in differences model to assess the impact of legal regulation on firm performance from a judicial perspective. The results show that the IPC reform significantly promotes the growth of firm performance, and this incentive effect is realized through the innovation quality mechanism. For different enterprises, the effect of IPC policy is more evident among firms with strong external funding dependence, large enterprise size, large spillover effects, and state ownership. In addition, we calculated sustainability indicators for firms and found that IPCs increased firms’ total factor productivity through quality-based innovation mechanisms. The important contribution of this study is that it fills a research gap in examining the impact of legal regulation on firms from a judicial perspective by identifying the relationship between judicial protection of IPRs, innovation, and business performance. This paper has implications for the promotion of judicial reform in countries with weak IPR systems, for developing countries like China, the judicial protection of IPRs should be increased to provide an institutional environment more conducive to enterprise development.
This is a preview of subscription content, log in via an institution to check access.
Access this article
Subscribe and save.
- Get 10 units per month
- Download Article/Chapter or Ebook
- 1 Unit = 1 Article or 1 Chapter
- Cancel anytime
Price excludes VAT (USA) Tax calculation will be finalised during checkout.
Instant access to the full article PDF.
Rent this article via DeepDyve
Institutional subscriptions

Data Availability
The data that support the findings of this study are available from the corresponding author upon reasonable request.
According to the Global Innovation Index Report 2021 released by the World Intellectual Property Organization (WIPO), China ranks 12th in the world in terms of the innovation index and has achieved a steady increase in innovation performance for nine consecutive years beginning in 2013, with the number of patents and trademark applications at the world’s leading level.
Abdallah, A. B., & Al-Ghwayeen, W. S. (2020). Green supply chain management and business performance: The mediating roles of environmental and operational performances. Business Process Management Journal, 26 (2), 489–512. https://doi.org/10.1108/BPMJ-03-2018-0091
Article Google Scholar
Aghion, P., & Howitt, P. (1992). A model of growth through creative destruction. Econometrica, 60 (2), 323–351. https://doi.org/10.2307/2951599
Aghion, P., Reenen, J. V., & Zingales, L. (2013). Innovation and institutional ownership. American Economic Review, 103 (1), 277. https://doi.org/10.1257/aer.103.1.277
Ahmed, E. M. (2017). ICT and human capital spillover effects in achieving sustainable East Asian knowledge-based economies: Erratum. Journal of the Knowldege Economy, 8 (3), 1113. https://doi.org/10.1007/s13132-017-0474-0
Ahmed, E. M. (2020). Modelling green productivity spillover effects on sustainability. World Journal of Science Technology and Sustainable Development, 17 (3), 257–267. https://doi.org/10.1108/WJSTSD-01-2020-0009
Ahmed, E. M. (2021). Modelling information and communications technology cyber security externalities spillover effects on sustainable economic growth. Journal of the Knowldege Economy, 12 (1), 412–430. https://doi.org/10.1007/s13132-020-00627-3
Ahmed, E. M., & Kialashaki, R. (2023). FDI inflows spillover effect implications on the Asian-Pacific labour productivity. International Journal of Finance and Economics, 28 (1), 575–588. https://doi.org/10.1002/ijfe.2437
Akcigit, U., Baslandze, S., & Stantcheva, S. (2016). Taxation and the international mobility of inventors. American Economic Review, 106 (10), 2930–2981. https://doi.org/10.1257/aer.20150237
Allred, B. B., & Park, W. G. (2007). Patent rights and innovative activity: Evidence from national and firm-level data. Journal of International Business Studies, 38 (6), 878–900. https://doi.org/10.1057/palgrave.jibs.8400306
Amore, M. D., Schneider, C., & Žaldokas, A. (2013). Credit supply and corporate innovation. Journal of Financial Economics, 109 (3), 835–855. https://doi.org/10.1016/j.jfineco.2013.04.006
Andries, P., & Faems, D. (2013). Patenting activities and firm performance: Does firm size matter? Journal of Product Innovation Management, 30 (6), 1089–1098. https://doi.org/10.1111/jpim.12047
Ang, J. S., Cheng, Y., & Wu, C. (2014). Does enforcement of intellectual property rights matter in China? Evidence from financing and investment choices in the high-tech industry. Review of Economics and Statistics, 96 (2), 332–348. https://doi.org/10.2139/ssrn.1357045
Anton, J., Greene, H., & Yao, D. A. (2006). Policy implications of weak patent rights. Innovation Policy and the Economy, 6 , 1–26. https://doi.org/10.1086/ipe.6.25056178
Ardito, L., D’Adda, D., & Petruzzelli, A. M. (2018). Mapping innovation dynamics in the Internet of Things domain: Evidence from patent analysis. Technological Forecasting and Social Change, 136 , 317–330. https://doi.org/10.1016/j.techfore.2017.04.022
Barber, B. M., & Lyon, J. D. (1996). Detecting abnormal operating performance: The empirical power and specification of test statistics. Journal of Financial Economics, 41 (3), 359–399. https://doi.org/10.1016/0304-405X(96)84701-5
Baum, L. (2009). Probing the effects of judicial specialization. Duke Law Journal, 58 (7), 1668–1684.
Google Scholar
Bennouri, M., Chtioui, T., Nagati, H., & Nekhili, M. (2018). Female board directorship and firm performance: What really matters? Journal of Banking and Finance, 88 , 267–291. https://doi.org/10.1016/j.jbankfin.2017.12.010
Bhaumik, S. K., & Selarka, E. (2012). Does ownership concentration improve M&A outcomes in emerging markets: Evidence from India. Journal of Corporate Finance, 18 (4), 717–726.
Bouet, D. (2015). A study of intellectual property protection policies and innovation in the Indian pharmaceutical industry and beyond. Technovation, 38 , 31–41. https://doi.org/10.1016/j.technovation.2014.10.007
Boulton, T. J. (2023). Property rights and access to equity capital in China. Global Finance Journal, 55 , 100797. https://doi.org/10.1016/j.gfj.2022.100797
Brem, A., Nylund, P. A., & Hitchen, E. (2017). Open innovation and intellectual property rights: How do SMEs benefit from patents, industrial designs, trademarks and copyrights? Management Decision, 55 (6), 1285–1306. https://doi.org/10.1108/md-04-2016-0223
Chen, L., Ping, L., & Song, F. (2010). Property rights protection and corporate R&D: Evidence from China. Journal of Development Economics, 93 (1), 49–62. https://doi.org/10.1016/j.jdeveco.2009.04.006
Ciftci, M., & Cready, W. M. (2011). Scale effects of R&D as reflected in earnings and returns. Journal of Accounting & Economics, 52 (1), 62–80. https://doi.org/10.1016/j.jacceco.2011.02.003
Claessens, S., & Laeven, L. (2003). Financial development, property rights, and growth. Journal of Finance, 58 (6), 2401–2436. https://doi.org/10.1046/j.1540-6261.2003.00610.x
Cremers, K., Ernicke, M., Gaessler, F., Harhoff, D., Helmers, C., & McDonagh, L. (2017). Patent litigation in Europe. European Journal of Law and Economics, 44 (1), 1–44. https://doi.org/10.1007/s10657-016-9529-0
Cui, W., Hicks, J., & Xing, J. (2022). Cash on the table? Imperfect take-up of tax incentives and firm investment behavior. Journal of Public Economics, 208 , 104632. https://doi.org/10.1016/j.jpubeco.2022.104632
De Chaisemartin, C., & D’Haultfoeuille, X. (2020). Two-way fixed effects estimators with heterogeneous treatment effects. American Economic Review, 110 (9), 2964–2996. https://doi.org/10.1257/aer.20181169
De Chaisemartin, C., & D’Haultfoeuille, X. (2024). Difference-in-differences estimators of intertemporal treatment effects. Review of Economics and Statistics , 1–45. https://doi.org/10.1162/rest_a_01414
Desyllas, P., Salter, A., & Alexy, O. (2022). The breadth of business model reconfiguration and firm performance. Strategic Organization, 20 (2), 231–269. https://doi.org/10.1177/1476127020955138
Elfaki, K. E., & Ahmed, E. M. (2024). Digital technology adoption and globalization innovation implications on Asian Pacific green sustainable economic growth. Journal of Open Innovation: Technology, Market, and Complexity, 10 (1), 100221. https://doi.org/10.1016/j.joitmc.2024.100221
Evangelista, A., Ardito, L., Boccaccio, A., Fiorentino, M., Petruzzelli, A. M., & Uva, A. E. (2020). Unveiling the technological trends of augmented reality: A patent analysis. Computers in Industry, 118 , 1–15. https://doi.org/10.1016/j.compind.2020.103221
Fang, L. H., Lerner, J., & Wu, C. (2017). Intellectual property rights protection, ownership, and innovation: Evidence from China. Review of Financial Studies, 30 (7), 2446–2477. https://doi.org/10.1093/rfs/hhx023
Feng, G. (2005). Innovation, future earnings, and market efficiency. Journal of Accounting, Auditing & Finance, 20 , 385–418. https://doi.org/10.1177/0148558X0502000405
Foo, C. T. (2012). Leadership, strategy and culture. Chinese Management Studies, 6 (4), 536–538. https://doi.org/10.1108/cms.2012.32306daa.001
Fu, T., & Jian, Z. (2021). Corruption pays off: How environmental regulations promote corporate innovation in a developing country. Ecological Economics, 183 (5), 106969. https://doi.org/10.1016/j.ecolecon.2021.106969
Galasso, A., & Hong, L. (2017). Tort reform and innovation. Journal of Law and Economics, 60 (3), 385–412. https://doi.org/10.1086/694337
Ginarte, J. C., & Park, W. G. (1997). Determinants of patent rights: A cross-national study. Research Policy, 26 (3), 283–301. https://doi.org/10.1016/s0048-7333(97)00022-x
Greenhalgh, C., & Rogers, M. (2007). The value of intellectual property rights to firms and society. Oxford Review of Economic Policy, 23 (4), 541–567. https://doi.org/10.1093/oxrep/grm035
Guo, F., Bo, Q. W., Tong, X., & Zhang, X. F. (2020). A paradoxical view of speed and quality on operational outcome: An empirical investigation of innovation in high-tech small and medium-sized enterprises. International Journal of Production Economics, 229 , 107780. https://doi.org/10.1016/j.ijpe.2020.107780
Gyedu, S., Tang, H., Menyah, M. V., & Kissi, G. D. (2024). The relationship between intellectual property rights, innovation, and economic development in the G20 and selected developing countries. Journal of the Knowledge Economy https://doi.org/10.1007/s13132-024-01859-3
Habib, M., Abbas, J., & Noman, R. (2019). Are human capital, intellectual property rights, and research and development expenditures really important for total factor productivity? An empirical analysis. International Journal of Social Economics, 46 (6), 756–774. https://doi.org/10.1108/IJSE-09-2018-0472
Hameed, W. U., Nisar, Q. A., & Wu, H. C. (2021). Relationships between external knowledge, internal innovation, firms’ open innovation performance, service innovation and business performance in the Pakistani hotel industry. International Journal of Hospitality Management, 92 , 102745. https://doi.org/10.1016/j.ijhm.2020.102745
Hanel, P. (2008). The use of intellectual property rights and innovation by manufacturing firms in Canada. Economics of Innovation & New Technology, 17 (4), 285–309. https://doi.org/10.1080/10438590701581481
He, S., Liu, J., & Ying, Q. (2023). Externalities of government-oriented support for innovation: Evidence from the national innovative city pilot policy in China. Economic Modelling, 128 , 106503. https://doi.org/10.1016/j.econmod.2023.106503
Hirshleifer, D., Hsu, P. H., & Li, D. (2018). Innovative originality, profitability, and stock returns. Review of Financial Studies, 31 (7), 2553–2605. https://doi.org/10.1093/rfs/hhx101
Hochberg, Y. V., & Lindsey, L. (2010). Incentives, targeting, and firm performance: An analysis of non-executive stock options. Review of Financial Studies, 23 (11), 4148–4186. https://doi.org/10.1093/rfs/hhq093
Holland, L. C., & Elder, E. M. (2006). Employee stock options in compensation agreements: A financing explanation. Journal of Corporate Finance, 12 (2), 367–379. https://doi.org/10.1016/j.jcorpfin.2005.06.002
Hu, M. (2018). Literature review on imitation innovation strategy. American Journal of Industrial and Business Management, 8 (8), 1777–1788. https://doi.org/10.4236/ajibm.2018.88120
Keller, W. (2004). International technology diffusion. Journal of Economic Literature, 42 (3), 752–782. https://doi.org/10.1257/0022051042177685
Kesan, J. P., & Ball, G. G. (2011). Judicial experience and the efficiency and accuracy of patent adjudication: An Empirical analysis of the case for a specialized patent trial court. Harvard Journal of Law & Technology , 24.
Kim, Y. K., Lee, K., Park, W. G., & Choo, K. (2012). Appropriate intellectual property protection and economic growth in countries at different levels of development. Research Policy, 41 (2), 358–375. https://doi.org/10.1016/j.respol.2011.09.003
Kong, D. M., Yang, Y. W., & Wang, Q. (2023). Innovative efficiency and firm value: Evidence from China. Finance Research Letters, 52 , 103557. https://doi.org/10.1016/j.frl.2022.103557
Liang, R., Wen, X., & Zhu, S. (2023). The impact of emission charges on the quality of corporate innovation: Based on the perspective of breakthrough technological innovation. Journal of Cleaner Production, 404 , 136830. https://doi.org/10.1016/j.jclepro.2023.136830
Lin, K. (2023). The impact of intellectual property protection on business performance of high-tech enterprises: The mediating effect of political-business relations. Finance Research Letters, 54 , 103718. https://doi.org/10.1016/j.frl.2023.103718
Liu, S., Du, J., Zhang, W., Tian, X., & Kou, G. (2021). Innovation quantity or quality? The role of political connections. Emerging Markets Review, 48 , 100819. https://doi.org/10.1016/j.ememar.2021.100819
Lu, Y., & Yu, L. (2015). Trade liberalization and markup dispersion: Evidence from China’s WTO accession. American Economic Journal: Applied Economics, 7 (4), 221–253. https://doi.org/10.1257/app.20140350
Mann, R. J., & Sager, T. W. (2007). Patents, venture capital, and software start-ups. Research Policy, 36 (2), 193–208. https://doi.org/10.1016/j.respol.2006.10.002
Moser, P. (2005). How do patent laws influence innovation? Evidence from nineteenth-century world’s fair. American Economic Review, 95 (4), 1214–1236. https://doi.org/10.1257/0002828054825501
Naghavi, A., & Strozzi, C. (2015). Intellectual property rights, diasporas, and domestic innovation. Journal of International Economics, 96 (1), 150–161. https://doi.org/10.1016/j.jinteco.2015.01.007
Nanda, R., & Rhodes-Kropf, M. (2013). Investment cycles and startup innovation. Journal of Financial Economics, 110 (2), 403–418. https://doi.org/10.1016/j.jfineco.2013.07.001
Neves, P. C., Afonso, O., Silva, D., & Sochirca, E. (2021). The link between intellectual property rights, innovation, and growth: A meta-analysis. Economic Modelling, 97 , 196–209. https://doi.org/10.1016/j.econmod.2021.01.019
Pandit, S., Wasley, C. E., & Zach, T. (2011). The effect of research and development (R&D) inputs and outputs on the relation between the uncertainty of future operating performance and R&D expenditures. Journal of Accounting, Auditing and Finance, 26 (1), 121–144. https://doi.org/10.1177/0148558X11400583
Pandit, S., Wasley, C. E., & Zach, T. (2015). The effect of research and development (R&D) inputs and outputs on the relation between the uncertainty of future operating performance and R&D expenditures. Journal of Accounting, Auditing & Finance, 26 (1), 121–144. https://doi.org/10.1177/0148558X11400583
Parra, A. (2019). Sequential innovation, patent policy, and the dynamics of the replacement effect. The RAND Journal of Economics, 50 (3), 568–590. https://doi.org/10.1111/1756-2171.12287
Porta, R. L., Lopez-De-Silanes, F., Shleifer, A., & Vishny, R. W. (1998). Law and finance. Journal of Political Economy, 106 (6), 1113–1155. https://doi.org/10.1086/250042
Prud’homme, D. (2019). Re-conceptualizing intellectual property regimes in international business research: Foreign-friendliness paradoxes facing MNCs in China. Journal of World Business, 54 (4), 399–419. https://doi.org/10.1016/j.jwb.2019.02.002
Rehman, Z. U., Khan, A., & Rahman, A. (2020). Corporate social responsibility’s influence on firm risk and firm performance: The mediating role of firm reputation. Corporate Social Responsibility & Environmental Management, 27 (6), 2991–3005. https://doi.org/10.1002/csr.2018
Sampat, B., & Williams, H. L. (2019). How do patents affect follow-on innovation? Evidence from the human genome. American Economic Review, 109 (1), 203–236. https://doi.org/10.1257/aer.20151398
Somaya, D., & McDaniel, C. A. (2012). Tribunal specialization and institutional targeting in patent enforcement. Organization Science, 23 (3), 869–887. https://doi.org/10.1287/orsc.1110.0669
Tang, Z. (2019). Judicial enforcement of intellectual property rights in China -from technical improvement to institutional reform. Asia Pacific Law Review, 27 (2), 176–197. https://doi.org/10.1080/10192557.2020.1718351
Tong, T. W., He, W., He, Z. L., & Lu, J. (2014). Patent regime shift and firm innovation: Evidence from the second amendment to China’s patent law. Academy of Management Annual Meeting Proceedings, 2014 (1), 14174–14174. https://doi.org/10.5465/ambpp.2014.14174abstract
Visnjic, I., Wiengarten, F., & Neely, A. (2016). Only the brave: Product innovation, service business model innovation, and their impact on performance. Journal of Product Innovation Management, 33 (1), 36–52. https://doi.org/10.1111/jpim.12254
Wang, C. X., Guo, F., & Zhang, Q. P. (2023). How does disruptive innovation influence firm performance? A moderated mediation model. European Journal of Innovation Management, 26 (3), 798–820. https://doi.org/10.1108/EJIM-07-2021-0369
Wang, H. D., Cho, C. C., & Lin, C. J. (2019). Related party transactions, business relatedness, and firm performance. Journal of Business Research, 101 , 411–425. https://doi.org/10.1016/j.jbusres.2019.01.066
Wang, J. Y., Fan, W. L., & Wang, Z. X. (2024). Tax incentives and earnings management: A study based on accelerated depreciation policy in China. Economic Analysis and Policy, 81 , 281–296. https://doi.org/10.1016/j.eap.2023.11.036
Wang, Z. N., Cai, S. H., Liang, H. G., Wang, N. X., & Xiang, E. W. (2021). Intellectual capital and firm performance: The mediating role of innovation speed and quality. International Journal of Human Resource Management, 32 (6), 1222–1250. https://doi.org/10.1080/09585192.2018.1511611
Weatherall, K., & Webster, E. (2014). Patent enforcement: A review of the literature. Journal of Economic Surveys, 28 (2), 312–343. https://doi.org/10.1111/joes.12009
Wyzycka, N., & Hasmath, R. (2017). The impact of the European union’s policy towards China’s intellectual property regime. International Political Science Review, 38 (5), 549–562. https://doi.org/10.1177/0192512116641320
Yao, L., & Rao, Y. (2009). IPRs protection measure and regional differences in China. International Business Research , 2(3). https://doi.org/10.5539/ibr.v2n3p108
Yao, S., Pan, Y., Sensoy, A., Uddin, G. S., & Cheng, F. (2021). Green credit policy and firm performance: What we learn from China. Energy Economics, 101 , 105415. https://doi.org/10.1016/j.eneco.2021.105415
Yu, L., & Zhao, C. (2023). Promote or inhibit? The effect of the whole chain development of intellectual property on manufacturing firm performance. Frontiers in Psychology, 14 , 1100865. https://doi.org/10.3389/fpsyg.2023.1100865
Zhang, L. G., & Lee, N. (2018). Institutional reforms and governance of intellectual property rights in China - The case of specialized intellectual property courts. Queen Mary Journal of Intellectual Property, 8 (1), 59–67. https://doi.org/10.4337/qmjip.2018.01.06
Zhang, Y. F., Li, L. M., & Xu, K. (2022). Do specialized intellectual property courts show a pro-patent propensity? Evidence from China. International Review of Law and Economics, 70 , 106065. https://doi.org/10.1016/j.irle.2022.106065
Zhang, Y., Ma, X., Pang, J., Xing, H., & Wang, J. (2023a). The impact of digital transformation of manufacturing on corporate performance - The mediating effect of business model innovation and the moderating effect of innovation capability. Research in International Business and Finance, 64 , 101890. https://doi.org/10.1016/j.ribaf.2023.101890
Zhang, Y., Wang, J., Chen, J. K., & Liu, W. Z. (2023b). Does environmental regulation policy help improve business performance of manufacturing enterprises? Evidence from China. Environment, Development and Sustainability, 25 (5), 4335–4364. https://doi.org/10.1007/s10668-022-02245-2
Zheng, P. P., Li, Z., & Zhuang, Z. Y. (2023). The impact of judicial protection of intellectual property on digital innovation: Evidence from China. Finance Research Letters, 58 , 104257. https://doi.org/10.1016/j.frl.2023.104257
Zhou, W. C., & Wang, R. (2020). Intellectual property, institutional dynamics, and firm innovation. Science & Public Policy (SPP), 47 (3), 299–312. https://doi.org/10.1093/scipol/scaa004
Download references
National Social Science Fund of China, Grant/Award Number: 18BJY213.
Author information
Authors and affiliations.
School of Economics and Management, Wuhan University, No. 16, Luojiashan Road, Wuchang District, Wuhan City, 430072, China
Wang Hao, Liu Chengkui, Yu Yue & Lin Xiaodan
You can also search for this author in PubMed Google Scholar
Corresponding author
Correspondence to Liu Chengkui .
Additional information
Publisher's note.
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
Reprints and permissions
About this article
Hao, W., Chengkui, L., Yue, Y. et al. Rule of Law Enhancement, Innovation Incentives, and Business Performance: Evidence from China’s IPCs. J Knowl Econ (2024). https://doi.org/10.1007/s13132-024-02195-2
Download citation
Received : 11 December 2023
Accepted : 07 June 2024
Published : 08 July 2024
DOI : https://doi.org/10.1007/s13132-024-02195-2
Share this article
Anyone you share the following link with will be able to read this content:
Sorry, a shareable link is not currently available for this article.
Provided by the Springer Nature SharedIt content-sharing initiative
- Intellectual property
- Judicial protection
- Innovation-driven
- Business performance
JEL Classification
- Find a journal
- Publish with us
- Track your research
Information
- Author Services
Initiatives
You are accessing a machine-readable page. In order to be human-readable, please install an RSS reader.
All articles published by MDPI are made immediately available worldwide under an open access license. No special permission is required to reuse all or part of the article published by MDPI, including figures and tables. For articles published under an open access Creative Common CC BY license, any part of the article may be reused without permission provided that the original article is clearly cited. For more information, please refer to https://www.mdpi.com/openaccess .
Feature papers represent the most advanced research with significant potential for high impact in the field. A Feature Paper should be a substantial original Article that involves several techniques or approaches, provides an outlook for future research directions and describes possible research applications.
Feature papers are submitted upon individual invitation or recommendation by the scientific editors and must receive positive feedback from the reviewers.
Editor’s Choice articles are based on recommendations by the scientific editors of MDPI journals from around the world. Editors select a small number of articles recently published in the journal that they believe will be particularly interesting to readers, or important in the respective research area. The aim is to provide a snapshot of some of the most exciting work published in the various research areas of the journal.
Original Submission Date Received: .
- Active Journals
- Find a Journal
- Proceedings Series
- For Authors
- For Reviewers
- For Editors
- For Librarians
- For Publishers
- For Societies
- For Conference Organizers
- Open Access Policy
- Institutional Open Access Program
- Special Issues Guidelines
- Editorial Process
- Research and Publication Ethics
- Article Processing Charges
- Testimonials
- Preprints.org
- SciProfiles
- Encyclopedia

Article Menu

- Subscribe SciFeed
- Recommended Articles
- Google Scholar
- on Google Scholar
- Table of Contents
Find support for a specific problem in the support section of our website.
Please let us know what you think of our products and services.
Visit our dedicated information section to learn more about MDPI.
JSmol Viewer
Evaluating the spatial heterogeneity and driving factors of sustainable development level in chengdu with point of interest data and geographic detector model.

1. Introduction
2. literature review, 2.1. spatial and temporal evolution of urban land function, 2.2. functional division of land based on administrative space and its defects, 3. methodology, 3.1. case study, 3.2. methods, 3.2.1. evaluation index system of urban sustainable development, 3.2.2. entropy weight method, 3.2.3. k-means algorithm and urban edge identification, 3.2.4. poi and urban functional area division, 3.2.5. geodetector model and driving forces analysis, 4. results and discussion, 4.1. spatial-temporal patterns of urban sustainable development, 4.1.1. temporal perspective analysis, 4.1.2. spatial perspective analysis, 4.1.3. spatiotemporal perspective analysis, 4.2. urban edge identification and urban expansion trend, 4.2.1. threshold determination for urban night light data based on the k-means algorithm, 4.2.2. identification of urban boundaries based on night light data, 4.2.3. urban expansion trend analysis based on land data, 4.3. poi and identification of urban functional zones, 4.4. driving factor analysis, 5. discussion, 6. conclusions, author contributions, data availability statement, conflicts of interest.
- Antrop, M. Landscape change and the urbanization process in Europe. Landsc. Urban Plan. 2004 , 67 , 9–26. [ Google Scholar ] [ CrossRef ]
- Feng, Z.; Peng, J.; Wu, J. Using DMSP/OLS nighttime light data and K–means method to identify urban–rural fringe of megacities. Habitat Int. 2020 , 103 , 102227. [ Google Scholar ] [ CrossRef ]
- Liu, Z.; Robinson, G.M. Residential development in the peri-urban fringe: The example of Adelaide, South Australia. Land Use Policy 2016 , 57 , 179–192. [ Google Scholar ] [ CrossRef ]
- Achillopoulou, D.V.; Mitoulis, S.A.; Argyroudis, S.A.; Wang, Y. Monitoring of transport infrastructure exposed to multiple hazards: A roadmap for building resilience. Sci. Total Environ. 2020 , 746 , 141001. [ Google Scholar ] [ CrossRef ]
- Kundu, S.; Rana, N.K.; Mahato, S. Unravelling blue landscape fragmentation effects on ecosystem services in urban agglomerations. Sustain. Cities Soc. 2024 , 102 , 105192. [ Google Scholar ] [ CrossRef ]
- Wang, X.; Hu, P.; Zhu, Y. Location choice of Chinese urban fringe residents on employment, housing, and urban services: A case study of Nanjing. Front. Archit. Res. 2016 , 5 , 27–38. [ Google Scholar ] [ CrossRef ]
- Mikhaeil, E.; Okulicz-Kozaryn, A.; Valente, R.R. Subjective well-being and urbanization in Egypt. Cities 2024 , 147 , 104804. [ Google Scholar ] [ CrossRef ]
- Li, H.; Chen, K.; Yan, L.; Yu, L.; Zhu, Y. Citizenization of rural migrants in China’s new urbanization: The roles of hukou system reform and rural land marketization. Cities 2023 , 132 , 103968. [ Google Scholar ] [ CrossRef ]
- Zhang, Y.; Wang, J.; Liu, Y.; Yue, W. Quantifying multiple effects of land finance on urban sprawl: Empirical study on 284 prefectural-level cities in China. Environ. Impact Assess. Rev. 2023 , 101 , 107156. [ Google Scholar ] [ CrossRef ]
- Yang, G.; Xu, R.; Chen, Y.; Wu, Z.; Du, Y.; Liu, S.; Qu, Z.; Guo, K.; Peng, C.; Chang, J.; et al. Identifying the greenhouses by Google Earth Engine to promote the reuse of fragmented land in urban fringe. Sustain. Cities Soc. 2021 , 67 , 102743. [ Google Scholar ] [ CrossRef ]
- China Sustainable Cities Report 2016: Measuring Ecological Input and Human Development. Available online: https://www.cn.undp.org/content/china/en/home/library/democratic_governance/china-sustainable-cities-report-2016--measuring-ecological-input.html (accessed on 30 November 2016).
- Zhang, X.; Xie, Y.; Jiao, J.; Zhu, W.; Guo, Z.; Cao, X.; Liu, J.; Xi, G.; Wei, W. How to accurately assess the spatial distribution of energy CO 2 emissions? Based on POI and NPP-VIIRS comparison. J. Clean. Prod. 2023 , 402 , 136656. [ Google Scholar ] [ CrossRef ]
- Lu, T.; Lansing, J.; Zhang, W.; Bechle, M.J.; Hankey, S. Land Use Regression models for 60 volatile organic compounds: Comparing Google Point of Interest (POI) and city permit data. Sci. Total Environ. 2019 , 677 , 131–141. [ Google Scholar ] [ CrossRef ]
- Cang, J.; Wu, P.; Lin, S. Redefining the boundaries of Chinese cities—Analysis based on multisource geographical big data. Cities 2024 , 149 , 104984. [ Google Scholar ] [ CrossRef ]
- Tampekis, S.; Samara, F.; Sakellariou, S.; Sfougaris, A.; Christopoulou, O. An eco-efficient and economical optimum evaluation technique for the forest road networks: The case of the mountainous forest of Metsovo, Greece. Environ. Monit. Assess. 2018 , 190 , 1–15. [ Google Scholar ] [ CrossRef ]
- Argyroudis, S.A.; Mitoulis, S.A.; Hofer, L.; Zanini, M.A.; Tubaldi, E.; Frangopol, D.M. Resilience assessment framework for critical infrastructure in a multi-hazard environment: Case study on transport assets. Sci. Total Environ. 2020 , 714 , 136854. [ Google Scholar ] [ CrossRef ]
- Sakellariou, S.; Sfoungaris, G.; Christopoulou, O. Territorial resilience through visibility analysis for immediate detection of wildfires integrating fire susceptibility, geographical features, and optimization methods. Int. J. Disaster Risk Sci. 2022 , 13 , 621–635. [ Google Scholar ] [ CrossRef ]
- He, Q.; Yan, M.; Zheng, L.; Wang, B. Spatial stratified heterogeneity and driving mechanism of urban development level in China under different urban growth patterns with optimal parameter-based geographic detector model mining. Comput. Environ. Urban Syst. 2023 , 105 , 102023. [ Google Scholar ] [ CrossRef ]
- Cui, L.; Wang, J.; Sun, L.; Lv, C. Construction and optimization of green space ecological networks in urban fringe areas: A case study with the urban fringe area of Tongzhou district in Beijing. J. Clean. Prod. 2020 , 276 , 124266. [ Google Scholar ] [ CrossRef ]
- Pacione, M. Private profit, public interest and land use planning—A conflict interpretation of residential development pressure in Glasgow’s rural–urban fringe. Land Use Policy 2013 , 32 , 61–77. [ Google Scholar ] [ CrossRef ]
- Yin, G.; Lin, Z.; Jiang, X.; Qiu, M.; Sun, J. How do the industrial land use intensity and dominant industries guide the urban land use? Evidences from 19 industrial land categories in ten cities of China. Sustain. Cities Soc. 2020 , 53 , 101978. [ Google Scholar ] [ CrossRef ]
- Qiao, W.; Hu, B.; Guo, Z.; Huang, X. Evaluating the sustainability of land use integrating SDGs and its driving factors: A case study of the Yangtze River Delta urban agglomeration, China. Cities 2023 , 143 , 104569. [ Google Scholar ] [ CrossRef ]
- Zeng, C.; Yin, Y.; Guo, L.; Liu, C.; Zhang, Y.; Huang, Z. Integrating the administrative spillover effect into the spatial governance system to revisit land development: A study in urban-rural fringe areas of Wuhan and neighboring cities, China. Land Use Policy 2024 , 139 , 107060. [ Google Scholar ] [ CrossRef ]
- Cattivelli, V. The methods used to identify urban, rural, and intermediate territories at European level: A comparison of the methods developed in the framework of TERCET and ESPON. Cities 2023 , 143 , 104556. [ Google Scholar ] [ CrossRef ]
- Vizzari, M.; Sigura, M. Landscape sequences along the urban–rural–natural gradient: A novel geospatial approach for identification and analysis. Landsc. Urban Plan. 2015 , 140 , 42–55. [ Google Scholar ] [ CrossRef ]
- Chen, W.; Xu, Q.; Zhao, K.; Hao, L.; Pu, C.; Yuan, S.; Chui, S.; Zhao, H.; Yang, K. Spatiotemporal expansion modes of urban areas on the Loess Plateau from 1992 to 2021 based on nighttime light images. Int. J. Appl. Earth Obs. Geoinf. 2023 , 118 , 103262. [ Google Scholar ] [ CrossRef ]
- Gao, Y.; Wang, Z.; Xu, F. Geospatial characteristics and the application of land use functions in the Yangtze River Economic Belt, China: Perspectives on provinces and urban agglomerations. Ecol. Indic. 2023 , 155 , 110969. [ Google Scholar ] [ CrossRef ]
- Liu, C.; Xu, Y.; Lu, X.; Han, J. Trade-offs and driving forces of land use functions in ecologically fragile areas of northern Hebei Province: Spatiotemporal analysis. Land Use Policy 2021 , 104 , 105387. [ Google Scholar ] [ CrossRef ]
- Tian, G.; Wu, J.; Yang, Z. Spatial pattern of urban functions in the Beijing metropolitan region. Habitat Int. 2010 , 34 , 249–255. [ Google Scholar ] [ CrossRef ]
- Du, J.; Thill, J.-C.; Peiser, R.B. Land pricing and its impact on land use efficiency in post-land-reform China: A case study of Beijing. Cities 2016 , 50 , 68–74. [ Google Scholar ] [ CrossRef ]
- Liu, X.; Li, Y.; Zhang, S.; Niu, Q. Spatiotemporal patterns, driving mechanism, and multi-scenario simulation of urban expansion in Min Delta Region, China. Ecol. Indic. 2024 , 158 , 111312. [ Google Scholar ] [ CrossRef ]
- Dong, T.; Jiao, L.; Xu, G.; Yang, L.; Liu, J. Towards sustainability? Analyzing changing urban form patterns in the United States, Europe, and China. Sci. Total Environ. 2019 , 671 , 632–643. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- Shi, H.; Li, Q.; Zhang, S.; Chen, W. How does urban innovation affect construction land use change in China? An analysis based on the network linkage perspective. Expert Syst. Appl. 2024 , 249 , 123676. [ Google Scholar ] [ CrossRef ]
- Kuang, W.; Chi, W.; Lu, D.; Dou, Y. A comparative analysis of megacity expansions in China and the U.S.: Patterns, rates and driving forces. Landsc. Urban Plan. 2014 , 132 , 121–135. [ Google Scholar ] [ CrossRef ]
- Li, C.; Zhao, J.; Xu, Y. Examining spatiotemporally varying effects of urban expansion and the underlying driving factors. Sustain. Cities Soc. 2017 , 28 , 307–320. [ Google Scholar ] [ CrossRef ]
- Mitchell, A. Making sense of counterurbanization. J. Rural. Stud. 2004 , 20 , 15–34. [ Google Scholar ] [ CrossRef ]
- Chakraborty, S.; Dadashpoor, H.; Novotný, J.; Maity, I.; Follmann, A.; Patel, P.P.; Roy, U.; Pramanik, S. In pursuit of sustainability–Spatio-temporal pathways of urban growth patterns in the world’s largest megacities. Cities 2022 , 131 , 103919. [ Google Scholar ] [ CrossRef ]
- Zhou, G.; Li, C.; Li, M.; Zhang, J.; Liu, Y. Agglomeration and diffusion of urban functions: An approach based on urban land use conversion. Habitat Int. 2016 , 56 , 20–30. [ Google Scholar ] [ CrossRef ]
- Jiao, J.; Jin, Y.; Yang, R. An approach to exploring the spatial distribution and influencing factors of urban problems based on Land use types. Sustain. Cities Soc. 2024 , 104 , 105321. [ Google Scholar ] [ CrossRef ]
- Lin, J.; Zhang, W.; Wen, Y.; Qiu, S. Evaluating the association between morphological characteristics of urban land and pluvial floods using machine learning methods. Sustain. Cities Soc. 2023 , 99 , 104891. [ Google Scholar ] [ CrossRef ]
- Brown, D.G.; Page, S.; Riolo, R.; Zellner, M.; Rand, W. Path dependence and the validation of agent-based spatial models of land use. Int. J. Geogr. Inf. Sci. 2005 , 19 , 153–174. [ Google Scholar ] [ CrossRef ]
- Jedwab, R.; Kerby, E.; Moradi, A. History, Path Dependence and Development: Evidence from Colonial Railways, Settlers and Cities In Kenya. Econ. J. 2017 , 127 , 1467–1494. [ Google Scholar ] [ CrossRef ]
- Alumäe, H.; Printsmann, A.; Palang, H. Cultural and Historical Values in Landscape Planning: Locals’ Perception. In Landscape Interfaces: Cultural Heritage in Changing Landscapes ; Palang, H., Fry, G., Eds.; Springer: Dordrecht, The Netherlands, 2003; pp. 125–145. [ Google Scholar ]
- Ren, J.; Ma, R.; Huang, Y.; Wang, Q.; Guo, J.; Li, C.; Zhou, W. Identifying the trade-offs and synergies of land use functions and their influencing factors of Lanzhou-Xining urban agglomeration in the upper reaches of Yellow River Basin, China. Ecol. Indic. 2024 , 158 , 111279. [ Google Scholar ] [ CrossRef ]
- Chen, M.; Lu, Y.; Ling, L.; Wan, Y.; Luo, Z.; Huang, H. Drivers of changes in ecosystem service values in Ganjiang upstream watershed. Land Use Policy 2015 , 47 , 247–252. [ Google Scholar ] [ CrossRef ]
- Meybeck, M.; Green, P.; Vörösmarty, C. A new typology for mountains and other relief classes: An application to global continental water resources and population distribution. Mt. Res. Dev. 2001 , 21 , 34–45. [ Google Scholar ] [ CrossRef ]
- Boone, R.B.; Conant, R.T.; Sircely, J.; Thornton, P.K.; Herrero, M. Climate change impacts on selected global rangeland ecosystem services. Glob. Change Biol. 2018 , 24 , 1382–1393. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- Hunsberger, C.; Work, C.; Herre, R. Linking climate change strategies and land conflicts in Cambodia: Evidence from the Greater Aural region. World Dev. 2018 , 108 , 309–320. [ Google Scholar ] [ CrossRef ]
- Ng, C.N.; Xie, Y.J.; Yu, X.J. Measuring the spatio-temporal variation of habitat isolation due to rapid urbanization: A case study of the Shenzhen River cross-boundary catchment, China. Landsc. Urban Plan. 2011 , 103 , 44–54. [ Google Scholar ] [ CrossRef ]
- Nayak, D.; Shukla, A.K.; Devi, N.R. Decadal changes in land use and land cover: Impacts and their influence on urban ecosystem services. Aqua Water Infrastruct. Ecosyst. Soc. 2024 , 73 , 57–72. [ Google Scholar ] [ CrossRef ]
- Xun, B.; Yu, D.; Liu, Y.; Hao, R.; Sun, Y. Quantifying isolation effect of urban growth on key ecological areas. Ecol. Eng. 2014 , 69 , 46–54. [ Google Scholar ] [ CrossRef ]
- Hernik, J.; Gawroński, K.; Dixon-Gough, R. Social and economic conflicts between cultural landscapes and rural communities in the English and Polish systems. Land Use Policy 2013 , 30 , 800–813. [ Google Scholar ] [ CrossRef ]
- Zhu, C.; Zhang, X.; Zhou, M.; He, S.; Gan, M.; Yang, L.; Wang, K. Impacts of urbanization and landscape pattern on habitat quality using OLS and GWR models in Hangzhou, China. Ecol. Indic. 2020 , 117 , 106654. [ Google Scholar ] [ CrossRef ]
- Foley, J.A.; DeFries, R.; Asner, G.P.; Barford, C.; Bonan, G.; Carpenter, S.R.; Chapin, F.S.; Coe, M.T.; Daily, G.C.; Gibbs, H.K.; et al. Global Consequences of Land Use. Science 2005 , 309 , 570–574. [ Google Scholar ] [ CrossRef ]
- Marchesani, F.; Masciarelli, F.; Doan, H.Q. Innovation in cities a driving force for knowledge flows: Exploring the relationship between high-tech firms, student mobility, and the role of youth entrepreneurship. Cities 2022 , 130 , 103852. [ Google Scholar ] [ CrossRef ]
- Antipova, A. City Structure and Spatial Patterns. In Urban Environment, Travel Behavior, Health, and Resident Satisfaction ; Springer International Publishing: Cham, Switzerland, 2018; pp. 153–204. [ Google Scholar ]
- Luo, T.; Zhang, T.; Wang, Z.; Gan, Y. Driving forces of landscape fragmentation due to urban transportation networks: Lessons from Fujian, China. J. Urban Plan. Dev. 2016 , 142 , 04015013. [ Google Scholar ] [ CrossRef ]
- Hu, T.; Yang, J.; Li, X.; Gong, P. Mapping Urban Land Use by Using Landsat Images and Open Social Data. Remote Sens. 2016 , 8 , 151. [ Google Scholar ] [ CrossRef ]
- Oruonye, E.D. An assessment of the impact of road construction on land use pattern in urban centres in nigeria, a case study of Jalingo LGA, Taraba State Nigeria. Mediterr. J. Soc. Sci. 2014 , 5 , 82–88. [ Google Scholar ] [ CrossRef ]
- Peng, J.; Chen, X.; Liu, Y.; Lü, H.; Hu, X. Spatial identification of multifunctional landscapes and associated influencing factors in the Beijing-Tianjin-Hebei region, China. Appl. Geogr. 2016 , 74 , 170–181. [ Google Scholar ] [ CrossRef ]
- Coisnon, T.; Musson, A.; Pene, S.D.; Rousselière, D. Disentangling public urban green space satisfaction: Exploring individual and contextual factors across European cities. Cities 2024 , 152 , 105154. [ Google Scholar ] [ CrossRef ]
- Tobler, W.R. A Computer Movie Simulating Urban Growth in the Detroit Region. Econ. Geogr. 1970 , 46 , 234–240. [ Google Scholar ] [ CrossRef ]
- Xiao, R.; Liu, Y.; Huang, X.; Shi, R.; Yu, W.; Zhang, T. Exploring the driving forces of farmland loss under rapidurbanization using binary logistic regression and spatial regression: A case study of Shanghai and Hangzhou Bay. Ecol. Indic. 2018 , 95 , 455–467. [ Google Scholar ] [ CrossRef ]
- Kubacka, M.; Piniarski, W. Searching for optimal solutions in a landscape fragmentation assessment: A case study from Poland–Identification of spatial data and methods. Ecol. Indic. 2024 , 163 , 112118. [ Google Scholar ] [ CrossRef ]
- Ou, Y.; Kim, E.; Liu, X.; Nam, K.-M. Delineating functional regions from road networks: The case of South Korea. Environ. Plan. B Urban Anal. City Sci. 2023 , 50 , 1677–1694. [ Google Scholar ] [ CrossRef ]
- Farmer, C.J.Q.; Fotheringham, A.S. Network-Based Functional Regions. Environ. Plan. A Econ. Space 2011 , 43 , 2723–2741. [ Google Scholar ] [ CrossRef ]
- Pérez-Soba, M.; Petit, S.; Jones, L.; Bertrand, N.; Briquel, V.; Omodei-Zorini, L.; Contini, C.; Helming, K.; Farrington, J.H.; Mossello, M.T.; et al. Land Use Functions—A Multifunctionality Approach to Assess the Impact of Land Use Changes on Land Use Sustainability ; Springer: Berlin/Heidelberg, Germany, 2008; pp. 375–404. [ Google Scholar ]
- Zhang, Y.; Long, H.; Tu, S.; Ge, D.; Ma, L.; Wang, L. Spatial identification of land use functions and their tradeoffs/synergies in China: Implications for sustainable land management. Ecol. Indic. 2019 , 107 , 105550. [ Google Scholar ] [ CrossRef ]
- Song, X.; Huang, Y.; Wu, Z.; Ouyang, Z. Does cultivated land function transition occur in China? J. Geogr. Sci. 2015 , 25 , 817–835. [ Google Scholar ] [ CrossRef ]
- Fan, Y.; Jin, X.; Gan, L.; Jessup, L.H.; Pijanowski, B.C.; Yang, X.; Xiang, X.; Zhou, Y. Spatial identification and dynamic analysis of land use functions reveals distinct zones of multiple functions in eastern China. Sci. Total Environ. 2018 , 642 , 33–44. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- Liu, C.; Xu, Y.; Huang, A.; Liu, Y.; Wang, H.; Lu, L.; Sun, P.; Zheng, W. Spatial identification of land use multifunctionality at grid scale in farming-pastoral area: A case study of Zhangjiakou City, China. Habitat Int. 2018 , 76 , 48–61. [ Google Scholar ] [ CrossRef ]
- Luo, Y.; Lü, Y.; Liu, L.; Liang, H.; Li, T.; Ren, Y. Spatiotemporal scale and integrative methods matter for quantifying the driving forces of land cover change. Sci. Total Environ. 2020 , 739 , 139622. [ Google Scholar ] [ CrossRef ]
- Zeng, C.; Song, Y.; He, Q.; Liu, Y. Urban–rural income change: Influences of landscape pattern and administrative spatial spillover effect. Appl. Geogr. 2018 , 97 , 248–262. [ Google Scholar ] [ CrossRef ]
- Menezes, T.; Roth, C. Natural Scales in Geographical Patterns. Sci. Rep. 2017 , 7 , 45823. [ Google Scholar ] [ CrossRef ]
- Hu, Y.; Han, Y. Identification of Urban Functional Areas Based on POI Data: A Case Study of the Guangzhou Economic and Technological Development Zone. Sustainability 2019 , 11 , 1385. [ Google Scholar ] [ CrossRef ]
- Dijkstra, L.; Florczyk, A.J.; Freire, S.; Kemper, T.; Melchiorri, M.; Pesaresi, M.; Schiavina, M. Applying the Degree of Urbanisation to the globe: A new harmonised definition reveals a different picture of global urbanisation. J. Urban Econ. 2021 , 125 , 103312. [ Google Scholar ] [ CrossRef ]
- Storper, M. Governing the Large Metropolis. Territ. Politics Gov. 2014 , 2 , 115–134. [ Google Scholar ] [ CrossRef ]
- Brenner, N. Standortpolitik, State Rescaling and the New Metropolitan Governance in Western Europe. Disp—Plan. Rev. 2003 , 39 , 15–25. [ Google Scholar ] [ CrossRef ]
- Yi, P.; Li, W.; Zhang, D. Sustainability assessment and key factors identification of first-tier cities in China. J. Clean. Prod. 2021 , 281 , 125369. [ Google Scholar ] [ CrossRef ]
- Avtar, R.; Aggarwal, R.; Kharrazi, A.; Kumar, P.; Kurniawan, T.A. Utilizing geospatial information to implement SDGs and monitor their Progress. Environ. Monit. Assess. 2019 , 192 , 35. [ Google Scholar ] [ CrossRef ]
- Giles-Corti, B.; Moudon, A.V.; Lowe, M.; Cerin, E.; Boeing, G.; Frumkin, H.; Salvo, D.; Foster, S.; Kleeman, A.; Bekessy, S.; et al. What next? Expanding our view of city planning and global health, and implementing and monitoring evidence-informed policy. Lancet Glob. Health 2022 , 10 , e919–e926. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- Zitti, M.; Ferrara, C.; Perini, L.; Carlucci, M.; Salvati, L. Long-Term Urban Growth and Land Use Efficiency in Southern Europe: Implications for Sustainable Land Management. Sustainability 2015 , 7 , 3359–3385. [ Google Scholar ] [ CrossRef ]
- Fulman, N.; Grinblat, Y.; Benenson, I. A project-based view of urban dynamics: Analyzing ‘leapfrogging’ and fringe development in Israel. Cities 2024 , 148 , 104908. [ Google Scholar ] [ CrossRef ]
- Fu, B.; Xue, B. Temporal and Spatial Evolution Analysis and Correlation Measurement of Urban–Rural Fringes Based on Nighttime Light Data. Remote Sens. 2024 , 16 , 88. [ Google Scholar ] [ CrossRef ]
- Wu, R.; Wang, J.; Zhang, D.; Wang, S. Identifying different types of urban land use dynamics using Point-of-interest (POI) and Random Forest algorithm: The case of Huizhou, China. Cities 2021 , 114 , 103202. [ Google Scholar ] [ CrossRef ]
- Qian, J.; Liu, Z.; Du, Y.; Liang, F.; Yi, J.; Ma, T.; Pei, T. Quantify city-level dynamic functions across China using social media and POIs data. Comput. Environ. Urban Syst. 2021 , 85 , 101552. [ Google Scholar ] [ CrossRef ]
- Zhang, J.; Zhao, X. Using POI and multisource satellite datasets for mainland China’s population spatialization and spatiotemporal changes based on regional heterogeneity. Sci. Total Environ. 2024 , 912 , 169499. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- Decoding “Happy Chengdu” in the “Happiness Report”. Available online: http://www.sc.xinhuanet.com/20231201/0948be5504514d7db98575a783f56cb4/c.html (accessed on 1 December 2023).
Click here to enlarge figure
| Primary Index | Secondary Index | Quantification Method | Unit | Abbreviation |
|---|---|---|---|---|
| Resources utilization | Air quality index | Composite air quality index | - | AQI |
| Proportion of cultivated land | Cultivated land area/land area | % | PCL | |
| Water resource | Total water resources per capita | 10 m /10 person | WR | |
| Per capita output of grain | Total food production/total population | kg/person | OG | |
| Annual output value per unit area | Gross value of agricultural, forestry and fisheries production/land area | yuan/km | AOV | |
| Happiness index | Public budget | Public budget expenditure per capita | million yuan/person | PB |
| Student | Number of students/million | person/million person | STU | |
| Number of beds per 1000 person | Number of beds/thousand persons | number/thousand person | BED | |
| Scenic Spots | Number of A-listed attractions per district/area of district | number/hectares unit/hectare | SS | |
| Economic potential | GDP per unit area | Gross district product/land area | 10 thousand yuan/km | GDPA |
| Urbanization rate | Urbanisation rate of resident population | % | UR | |
| Number of industrial enterprises above designated size | Number of industrial enterprises above designated size | unit | NIE | |
| Average property price | Average annual housing price | yuan | APP | |
| Scientific research strength | Percentage of soft science scores for district colleges and universities | % | SRE | |
| Incremental effective invention | 12-month cumulative valid inventions | Number | IE | |
| Number of listed companies | Number of listed companies | numer | NLC |
| Functional Categorization | Medium Categories | POI |
|---|---|---|
| Happiness index | Public facilities | Public telephone, newspaper and magazine stand service area, public toilet, and shelter et al. |
| Science, Education, and Culture | School, training center, research institution, library and cultural palace et al. | |
| Medical and Healthcare | Clinic, general hospital, emergency center, and specialist hospital et al. | |
| Tourist Attractions | Park, scenic spot, temple, square, zoo, and botanical garden et al. | |
| Economic potential | Companies and Enterprises | Company, factory and agriculture, forestry, animal husbandry, and fishery base et al. |
| Shopping and Services | Home furnishing, specialty store, shop, comprehensive market, sporting goods store et al. | |
| Financial Institutions | Bank, insurance agency, security company et al. | |
| Business and Residential Areas | Residential area, building and industrial park et al. | |
| Resources utilization | Blank area of POI | - |
| Mixed functional area | All | All |
| Resources Utilization | Economic Potential | Happiness Index | |||
|---|---|---|---|---|---|
| Indicators | q-Statistic | Indicators | q-Statistic | Indicators | q-Statistic |
| AQI | 0.17 | GDPA | 0.60 | PB | 0.10 |
| PCL * | 0.28 | UR * | 0.24 | STU | 0.008 |
| WR * | 0.26 | NIE | 0.12 | BED * | 0.48 |
| OG * | 0.24 | APP * | 0.50 | SS * | 0.61 |
| AOV * | 0.32 | SRE * | 0.55 | - | - |
| - | - | IE | 0.74 | - | - |
| - | - | NLC * | 0.66 | - | - |
| Mean | 0.253 | 0.489 | 0.317 | ||
| Variance | 0.002 | 0.044 | 0.054 | ||
| Coefficient of variation | 0.193 | 0.43 | 0.733 | ||
| The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
Share and Cite
Ling, Y.; Zhao, Y.; Ren, Q.; Qiu, Y.; Zhang, Y.; Zhai, K. Evaluating the Spatial Heterogeneity and Driving Factors of Sustainable Development Level in Chengdu with Point of Interest Data and Geographic Detector Model. Land 2024 , 13 , 1018. https://doi.org/10.3390/land13071018
Ling Y, Zhao Y, Ren Q, Qiu Y, Zhang Y, Zhai K. Evaluating the Spatial Heterogeneity and Driving Factors of Sustainable Development Level in Chengdu with Point of Interest Data and Geographic Detector Model. Land . 2024; 13(7):1018. https://doi.org/10.3390/land13071018
Ling, Yantao, Yilang Zhao, Qingzhong Ren, Yue Qiu, Yuerong Zhang, and Keyu Zhai. 2024. "Evaluating the Spatial Heterogeneity and Driving Factors of Sustainable Development Level in Chengdu with Point of Interest Data and Geographic Detector Model" Land 13, no. 7: 1018. https://doi.org/10.3390/land13071018
Article Metrics
Further information, mdpi initiatives, follow mdpi.

Subscribe to receive issue release notifications and newsletters from MDPI journals

IMAGES
VIDEO
COMMENTS
1. The Classic Literature Gap. First up is the classic literature gap. This type of research gap emerges when there's a new concept or phenomenon that hasn't been studied much, or at all. For example, when a social media platform is launched, there's an opportunity to explore its impacts on users, how it could be leveraged for marketing, its impact on society, and so on.
Show how your research addresses a gap or contributes to a debate; Evaluate the current state of research and demonstrate your knowledge of the scholarly debates around your topic. Writing literature reviews is a particularly important skill if you want to apply for graduate school or pursue a career in research. We've written a step-by-step ...
A literature gap, or research gap, is an unexplored topic revealed during a literature search that has scope for research or further exploration. To identify literature gaps, you need to do a thorough review of existing literature in both the broad and specific areas of your topic. You could go through both the Introduction and Discussion ...
Here are some examples of research gaps that researchers might identify: Theoretical Gap Example: In the field of psychology, there might be a theoretical gap related to the lack of understanding of the relationship between social media use and mental health. Although there is existing research on the topic, there might be a lack of consensus ...
1 Answer to this question. Specifically in the context of doing and writing the literature review, you can identify a gap in any/all of the following ways: Look up papers that build on previous papers, be it by the same author/s or others. Find out what gaps the later papers have addressed, and if there are still any.
Through systematic processes, these reviews offer suggestions to synthesize literature to identify research gaps and indicate research directions. Lastly, this article serves as a guide for researchers and academics in conducting an extensive literature review.
Gap Analysis for Literature Reviews and Advancing Useful Knowledge 1. Figure 1: Abstract example of a causal map of a theory. There are really three basic kinds of gaps for you to find: relevance ...
Mapping the gap. The purpose of the literature review section of a manuscript is not to report what is known about your topic. The purpose is to identify what remains unknown—what academic writing scholar Janet Giltrow has called the 'knowledge deficit'—thus establishing the need for your research study [].In an earlier Writer's Craft instalment, the Problem-Gap-Hook heuristic was ...
As mentioned previously, there are a number of existing guidelines for literature reviews. Depending on the methodology needed to achieve the purpose of the review, all types can be helpful and appropriate to reach a specific goal (for examples, please see Table 1).These approaches can be qualitative, quantitative, or have a mixed design depending on the phase of the review.
Literature Review is a comprehensive survey of the works published in a particular field of study or line of research, usually over a specific period of time, in the form of an in-depth, critical bibliographic essay or annotated list in which attention is drawn to the most significant works. Also, we can define a literature review as the ...
An essential aspect of reviewing the literature is to identify research gaps (Webster and Watson 2002). While reviews oug ht to be conducted rigorously (e.g., Fink 2010), there has been a lack of ...
The identification of gaps from systematic reviews is essential to the practice of "evidence-based research." Health care research should begin and end with a systematic review.1-3 A comprehensive and explicit consideration of the existing evidence is necessary for the identification and development of an unanswered and answerable question, for the design of a study most likely to answer ...
What is a 'gap in the literature'? The gap, also considered the missing piece or pieces in the research literature, is the area that has not yet been explored or is under-explored. This could be a population or sample (size, type, location, etc.), research method, data collection and/or analysis, or other research variables or conditions.
As a final note, remember that many gaps may be filled with secondary research; a new literature review that fills the gaps in the logic/structure, data/information, and meaning/relevance of your map so that your organisation can have a greater impact. Figure 3. Visualizing the gaps (shown in green)
A literature review is a critical analysis and synthesis of existing research on a particular topic. It provides an overview of the current state of knowledge, identifies gaps, and highlights key findings in the literature. 1 The purpose of a literature review is to situate your own research within the context of existing scholarship ...
A literature review is important because it: Explains the background of research on a topic. Demonstrates why a topic is significant to a subject area. Discovers relationships between research studies/ideas. Identifies major themes, concepts, and researchers on a topic. Identifies critical gaps and points of disagreement.
Most literature reviews in information systems (IS) research use the framework proposed by Webster and Watson's (2002). However, their framework includes little information about how to rigorously identify research gaps when conducting literature reviews. As Webster and Watson note, "a review should identify critical knowledge gaps and thus ...
The literature review for a gap in practice will show the context of the problem and the current state of the research. Research gap definition. A research gap exists when: ... To identify research trends, use the literature review matrix to track where further research is needed. Download or create your own Literature Review Matrix (examples ...
How to Write a Literature Review in 6 Steps. Published on July 2, 2024 by Paige Pfeifer, BA. The usual purpose of a literature review is to show a gap in existing research or to show a field's overall view of a topic. A "literature review" is a summary of what previous studies have demonstrated or argued about a topic.
This research question was derived based on the analysis of the existing literature and the gaps identified. Published research provides limited evidence on how the tasks and tools of management accountants are (expected to be) impacted by digitization. Recent studies focus on limited aspects.
Identifying Gaps. If you do not find articles in your literature search, this may indicate a gap. If you do find articles, the goal is to find a gap for contributing new research. Authors signal that there is a gap using phrases such as: Has not been clarified, studied, reported, or elucidated. Further research is required or needed.
1. Evidence Gap: An evidence gap occurs with a provocative exception arising if a new research finding contradicts widely accepted conclusions. This gap involves contradictions in the findings of the prior research. It occurs if results from studies allow for conclusions in their own right, but are contradictory when examined from a more abstract point of view.
The purpose of this paper is to conduct a systematic literature review on the concept of research gaps and provoke a discussion on the contemporary literature on types of research gaps. The paper discusses the various approaches for researchers to identify, align and position research problems, research design, and methodology in the research ...
Section 7 shows research gaps and possible directions for closing them. ... These factors help ensure the 3D packing literature review is efficient, reliable, and suitable. This methodology ensures the literature review is up-to-date and allows obtaining the main body of robotic 3D packing. After applying this methodology, 46 studies were left.
To address this knowledge gap we first conducted a literature review focusing on two research questions: 1) the difference in adherence between SITT and MITT users in COPD, and 2) the effect of smart inhalers on adherence in COPD. Separate searches were conducted in PubMed and two authors independently assessed the articles.
To address this gap, our systematic literature review examined existing literature to further explore and understand visual pollution. We systematically reviewed research articles published between 2008 and 2023, utilizing three journal databases: Web of Science, Scopus, and Google Scholar.
Targeted gray literature search. References were screened according to the inclusion and exclusion criteria (Table 1), except that articles only needed to report (rather than focus) on future leadership roles and requirements.This is because we wanted to ensure that our analysis broadly captured the most recent sources of information on healthcare leadership requirements, even if these sources ...
Literature. A country's IPR regime profoundly affects the ability of firms to function as agents of social innovation. A weak IPR environment reduces firms' access to external finance and forces them to suboptimally allocate resources, thus hindering firm growth (Claessens & Laeven, 2003).Further, although a firm's competitive advantage in the marketplace relies heavily on technological ...
Over the past few decades, China has undergone the largest and fastest urbanization process in world history. By 2023, Chengdu's urbanization rate had reached 80.5%, significantly higher than the national average of 66.16%. Studying the urbanization experience of Chengdu is of great significance for optimizing urban planning policies in Chengdu and other cities in China. Although much ...