- ConscienHealth
- Advocacy Organizations
- Affiliates & Advocates
- Service Partners
- Publications
- LATEST NEWS


Discipline and the Obesity That No One Wants to See
Discipline – or the lack of it – is something that is sometimes offered up as an explanation for obesity. Public health professionals, employers, and physicians gathered at a medical forum in Baltimore last week to discuss obesity and how health plans can address this growing health concern. One physician who is medical director for a large health insurer asked at the end of a presentation on the physiology of obesity:
This is all very interesting, but isn’t obesity simply a matter of self-discipline? I mean the food might be available, but does that mean that you have to eat it all? Why do we pretend obesity is a medical issue?
As a matter of fact, complex physiology regulates how our bodies energy absorb, use, and store energy as fat. In obesity, that physiology causes the body to store fat in an unhealthy way. Obesity is no more a failure of discipline than high blood pressure is. It is a failure of physiology. It requires care, not blame.
Stereotypical thinking assumes that people with obesity are undisciplined or suffering from a number of other character flaws. It is well documented in studies of weight bias and stigma that many healthcare professionals harbour such attitudes. Such thinking is often used as an excuse for ignoring obesity and for neglecting the medical needs of people who have it.
A new editorial by Daniele Di Pauli in Eating and Weight Disorders points out that weight bias should not be overlooked:
As health professionals, and scientific societies, we cannot allow the stigma toward obesity to go unnoticed like happens to Icarus, in the painting by Pieter Bruegel the Elder, in which no one seems to notice the son of Daedalus fallen from the sky into the sea.
Unfortunately, bias against people living with obesity has been quietly overlooked for far too long. Health professionals who are inclined to blame people for their illness should reflect upon the purpose of their chosen profession.
Click here for the editorial by Di Pauli.
Order, photograph © A Not Very Creative Mind / flickr
Subscribe by email to follow the accumulating evidence and observations that shape our view of health, obesity, and policy.
Your email:
June 12, 2016
12 Responses to “Discipline and the Obesity That No One Wants to See”
June 12, 2016 at 8:45 am, M said:
I suspect part of the issue is that doctors are being told “You have to address obesity with your patients!” There’s two parts here, I think. One is the bizarre idea that fat people don’t know they’re fat. (I suspect they’re confusing people who say “I am perfectly healthy otherwise. Who cares what I weigh?” with fat people thinking they’re skinny.) The other is the too common belief that “address” means bully and shame into restrictive dieting, instead of making sure the patient is eating well and regularly exercising – just as they should be doing for their thin patients, as well.
Studies show that doctors often think that fat people are non-compliant, likely from a belief that “If they cannot control what they eat how can we expect them to follow treatment?” The frightening truth of the “death by obesity” statistic is that doctors may have a role in those deaths.
June 12, 2016 at 4:33 pm, Ted said:
Unfortunately, much of what you say has been shown to be true in research on weight bias. This is a case where the “cure” is worse than the problem. It certainly makes the problem worse.
June 12, 2016 at 9:51 am, Stephen Phillips said:
The concept of obesity resulting from willful misconduct is as old as ignorance.
Stephen Phillips American Association of Bariatric Counselors
June 12, 2016 at 10:10 am, Beth Bianca said:
Thank you for being an advocate for our community. Discipline is great if you have to lose 20 pounds. However, those of us who have tried using discipline over and over our entire lives and end up heavier are obviously dealing with something different.
I wrote an article last month that was published in the Huffington Post. It addressed the judgement against weight-loss surgery and how people do not think discipline is required for the results. Therefore, people looked at weight-loss surgery results as “not counting” as much as using “diet and exercise alone. Absolutely absurd.
June 12, 2016 at 4:30 pm, Ted said:
You are right, Beth. Thanks for speaking up!
June 13, 2016 at 5:30 am, Mary-Jo Overwater said:
I firmly believe in the importance of discipline in life. Exercising discipline to stay on task when one is distracted or wants to give up or to reign in impulsive behaviors can be character-building and really help one enjoy feelings of accomplishment and strength. People who are hard-wired to be naturally slim or self-regulators, but who have put on 10-25 lbs with age or change of lifestyle circumstances have better success when they exercise discipline because their bodies respond more efficiently to treatments and to any lifestyle changes to eat more healthfully/ balanced again and/or to exercise. Discipline is rewarded in these cases and affirms the argument for discipline.
But, when it comes to weight management in obesity, it is naïve and ignorant to assert it has a key role to solving the struggle with obesity. Most of my obese clients who struggle with their weight are, in fact, often MORE disciplined than people who don’t have the (patho)physiology of obesity. The amount and focus of self-control and dedication exhibited for long periods of time in keeping dietary intake either restricted or certainly much less than their bodies are hard-wired to ‘require’ and to sustain exercise regimes often much longer and more intense than non-obese individuals, takes incredible discipline Then, after all that effort, to see little or no change on the scale or in your clothes size, or even in your biomarkers — well, it’s soul-crushing.
So, people with obesity and people who treat obesity need the facts before any true assessments and/or decisions about courses of action can be made. In my case, as a person who is BOTH — I work with people who struggle with weight and I, myself, struggle with my weight. I know the reality that growing up obese and being obese for a good part of my early adulthood has set my body up to fight tremendous odds to get me at a certain ‘ideal’ weight. I exert tremendous discipline in pushing myself to exercise at least 5 times a week and in stopping eating when I know I’ve had enough. I am not hard-wired to stop. I do believe that discipline has kept me from being 50, maybe 100 lbs more than I am now.
But, believe me, it IS at times, soul-destroying. What makes it even worse is when other fellow-dietitians or anyone else, for that matter, make presumptive judgements. The reality of weight bias is extremely destructive. I could go for a bypass or pursue medical treatment and I may do so at some point. Right now, my labs and biomarkers are all good and I feel healthy and vital, despite being 40-50 lbs more than I have been at my lowest weight before my second pregnancy. Exercising discipline is important for me, but having a clear understanding of the limitations of discipline has been extremely uplifting and actually keeps me even more motivated to keep up with my healthier choices. 🙂
June 13, 2016 at 5:36 am, Ted said:
Beautifully well said, Mary-Jo. Thank you!
June 13, 2016 at 12:24 pm, Katherine Rivard said:
In even high-level corporate Health Coaching Companies, where boss women are heavy and at the top, the idea of a skinny subordinate is reason to limit their advancement.
So the flip side of “I am working on it” shows up in the numbers reflecting that weight is actually not managed because it is a human reason to suggest that people of managed weight don’t sit down enough to get their work done and are less devoted to the female boss. I have seen this unspoken and not addressed until the research came back showing that weight is least likely to change in the workplace neighborhood.
June 13, 2016 at 10:24 pm, ejh said:
Ted —
I find others have well described the personal dynamic of issues surrounding obesity — so I am grateful and feel no need to further discuss it.
HOWEVER — I would like to know what the response was to the physicians question about lack of discipline and blame the fat person mentality…. Did he listen? Do you think he LEARNED anything? Scares me that someone in his position would remain so ignorant. Ten years ago maybe I could see it…. so I am curious…
As always, thanks for your column.
June 14, 2016 at 4:44 am, Ted said:
Thanks for asking, Jean. The presenter responded that obesity has many causes and an undisciplined personality is not one of them. The presenter went on to describe the physiology of obesity, but my assessment was that the questioner was not listening. He left the room several times. At lunch, he tried to persuade another HCP, who was a bariatric surgery patient, that her problems with obesity since early childhood were due to emotional problems. He was not doing a lot of listening.
June 14, 2016 at 8:09 pm, John said:
The blog is a breath of fresh air. It’s so hard to find folk that understand this complex chronic disease. Yet the facts about the physiology are clear. We somehow allow this disorder of regulation to be treated differently to others like blood pressure, diabetes and cancer. It’s interesting diabetes and hypertension generate complications – obesity generates co-morbidities!
Come how this is different? Why?
But this blog is the exception. Other blogs that follow a little touch of the truth are condemned for their clear error in that “we all know it’s all about bad choices”!
But, we are not winning. Can you imagine the outcry if we just treated 1% of those with type 2 diabetes with effective care beyond lifestyle advice. I think the word is negligence.
June 15, 2016 at 5:44 am, Ted said:
Thanks, John. You make some excellent points. In particular, the comparison to the failure of regulating glucose, blood pressure, lipids, and cell growth will stick with me. Thanks!
Search this blog
- access to care
- anti-obesity medicines
- bariatric surgery
- childhood obesity
- evidence based medicine
- food industry
- food policy
- health disparities
- health economics
- health insurance
- health outcomes
- health reporting
- Obesity Action Coalition
- obesity care
- obesity causes
- obesity complications
- obesity prevention
- obesity statistics
- obesity treatment
- physical activity
- public health
- scientific integrity
- scientific rigor
- semaglutide
- weight bias
- weight discrimination
- weight loss
- weight stigma
- February 2024
- January 2024
- December 2023
- November 2023
- October 2023
- September 2023
- August 2023
- February 2023
- January 2023
- December 2022
- November 2022
- October 2022
- September 2022
- August 2022
- February 2022
- January 2022
- December 2021
- November 2021
- October 2021
- September 2021
- August 2021
- February 2021
- January 2021
- December 2020
- November 2020
- October 2020
- September 2020
- August 2020
- February 2020
- January 2020
- December 2019
- November 2019
- October 2019
- September 2019
- August 2019
- February 2019
- January 2019
- December 2018
- November 2018
- October 2018
- September 2018
- August 2018
- February 2018
- January 2018
- December 2017
- November 2017
- October 2017
- September 2017
- August 2017
- February 2017
- January 2017
- December 2016
- November 2016
- October 2016
- September 2016
- August 2016
- February 2016
- January 2016
- December 2015
- November 2015
- October 2015
- September 2015
- August 2015
- February 2015
- January 2015
- December 2014
- November 2014
- October 2014
- September 2014
- August 2014
- February 2014
- January 2014
- December 2013
- November 2013
- October 2013
- September 2013
- August 2013
- February 2013
- January 2013
- December 2012
- November 2012
- October 2012
- September 2012
- August 2012
- February 2012
- January 2012
- October 2011
- February 2011
- January 2011
- December 2010
- October 2010
- September 2010
- October 2009
- August 2009
- Consumer Trends
- Food & Nutrition
- Food Industry
- Health & Obesity
- Health Policy
- Scientific Meetings & Publications

outstanding advocacy
Recognized by The Obesity Society & Obesity Action Coalition
©2009-2013 ConscienHealth. All rights reserved. | Website Design by Mariela Antunes | Hosting by DTS
Obesity and Weight Loss Strategies Essay
- To find inspiration for your paper and overcome writer’s block
- As a source of information (ensure proper referencing)
- As a template for you assignment
Introduction
Otc product and diet.
The obesity epidemic is among the most urgent healthcare issues in the United States and worldwide. According to recent estimations, between 39% and 49% of the world’s population are overweight or obese nowadays (Powell-Wiley et al., 2021). This trend has led to many people seeking weight loss through different means, including diet, eating behavior management, and pharmacological weight loss agents (Kushner, 2018). However, over-the-counter (OTC) weight loss products have also gained popularity despite serious health risks (Rodriguez-Guerra et al., 2021). Therefore, it is essential for healthcare professionals to keep the broad public well-informed about the nature and potential adverse effects of such products.
The model client is a 40-year-old man with a family history of obesity-related cardiovascular disease. The client pursues weight loss primarily out of concerns for personal health due to recently developed hypertension. The client has considered using an OTC, non-prescription herbal weight loss supplement, AMPK Metabolic Activator. The drug is advertised as a mixture of two botanical components that supposedly help the body burn stored abdominal fat (AMPK Metabolic Activator, n. d.). The patient’s product choice was primarily driven by the desire to achieve quick weight loss using natural products instead of synthetic medications.
However, the client was strongly advised against using OTC products due to a broad range of associated health hazards. Despite advertisement, most OTC herbal weight loss drugs are adulterated with active pharmaceutical agents (Dastjerdi et al., 2018). The pharmaceutical components in such products include tramadol, caffeine, fluoxetine, rizatriptan, venlafaxine, and methadone (Dastjerdi et al., 2018). Legal in most countries, these agents present serious health risks in case of excessive consumption. Furthermore, sibutramine, associated with a high risk of cardiovascular diseases even among consumers without a known history of CVDs, remains in many herbal medications (Rodriguez-Guerra et al., 2021). Therefore, the list of potential negative side-effects of the OTC weight loss products contradicts the client’s initial expectations and desires.
A healthier and more effective weight loss strategy is changing the lifestyle. Healthcare experts agree that weight loss depends primarily on reducing total caloric intake and sufficient physical activity (Kushner, 2018). Additionally, this strategy helps prevent a broad range of cardiovascular diseases and improves the overall physical condition. Therefore, a diet based on the client’s metabolic profile and health condition is the strategy’s primary focus. Experts recommend the calorie-reduced Dietary Approaches to Stop Hypertension (DASH) diet, rich in fruits, vegetables, and low-fat dairy products, for patients with hypertension (Kushner, 2018). The proposed day 1 menu would consist of the following:
- a whole-wheat bagel with 2 tablespoons peanut butter, an orange, and a cup of fat-free milk for breakfast;
- spinach salad with reduced-sodium wheat crackers for lunch;
- baked cod with 1/2 cup brown rice pilaf with vegetables, 1/2 cup fresh green beans, and herbal tea for dinner (Sample menus for the DASH diet, 2020).
This diet corresponds to the client’s goals and is optimal for his health profile.
Intermittent fasting (IF) has become an increasingly popular approach to treating obesity. Its proponents argue that the strategy is more effective in addressing weight loss than traditional daily caloric intake reduction (Halpern & Mendes, 2021). The IF advocates claim that high insulin levels in the organism associated with high carbohydrate intake facilitate the development of obesity. Intermittent fasting addresses this issue by reducing insulin levels via specially developed fasting schedules. However, experimental models in animals and humans have repeatedly discredited the insulin-related theory (Halpern & Mendes, 2021). Nevertheless, many people still see IF as a preferable alternative, mainly due to its widely marketed supposed benefits and the absence of strict dietary limitations and excessive physical activity.
Obesity remains a significant public health hazard globally, requiring the development and broad introduction of efficient and affordable weight loss strategies and programs. While many still resort to OTC medications and other questionable weight loss strategies, public health professionals and institutions must promote evidence-based approaches. These include safe, personally developed, balanced dietary measures, prescription pharmaceutical agents, and a healthy lifestyle with sufficient physical activity and caloric intake.
AMPK Metabolic Activator (n. d.). Life Extension. Web.
Dastjerdi, A. G., Akhgari, M., Kamali, A., & Mousavi, Z. (2018). Principal component analysis of synthetic adulterants in herbal supplements advertised as weight loss drugs . Complementary Therapies in Clinical Practice, 31 , 236–241. Web.
Halpern, B., & Mendes, T. B. (2021). Intermittent fasting for obesity and related disorders: unveiling myths, facts, and presumptions. Archives of Endocrinology and Metabolism, 65 (1). Web.
Kushner, R. F. (2018). Weight Loss Strategies for Treatment of Obesity: Lifestyle Management and Pharmacotherapy . Progress in Cardiovascular Diseases. Web.
Powell-Wiley, T. M., Poirier, P., Burke, L. E., J.-P., Després, Gordon-Larsen, P., Lavie, C. J., Lear,S. A., Ndumele, C. E., Neeland, I. J., Sanders, P., & St-Onge, M.-P. (2021). Obesity and cardiovascular disease: A scientific statement from the American Heart Association . Circulation, 143 (21), 984–1010. Web.
Rodriguez-Guerra, M., Yadav, M., Bhandari, M., Sinha, A., Bella, J. N., & Sklyar, E. (2021). Sibutramine as a cause of sudden cardiac death . Case Reports in Cardiology, 2021 , 1–5. Web.
Sample menus for the DASH diet (2020). Mayo Clinic. Web.
- Nursing Analysis of Community of Heidelberg, Germany
- Disaster Recovery Plan for the Valley City
- Special Education: Clean Intermittent Catheterization
- Fasting in Contemporary Christianity
- Over-the-Counter Classes: Global Perspective and Indian Scenario
- Humanity’s Collective Health Impacted by Globalization
- Importance of Self-Care: Rhetoric and Persuasion
- Pitney Bowes Company's Approach to Employee Health
- The Limitations of Pitney Bowes’ Approach to Employee Health
- Analysis of Obesity as a Public Health Concern
- Chicago (A-D)
- Chicago (N-B)
IvyPanda. (2024, February 12). Obesity and Weight Loss Strategies. https://ivypanda.com/essays/obesity-and-weight-loss-strategies/
"Obesity and Weight Loss Strategies." IvyPanda , 12 Feb. 2024, ivypanda.com/essays/obesity-and-weight-loss-strategies/.
IvyPanda . (2024) 'Obesity and Weight Loss Strategies'. 12 February.
IvyPanda . 2024. "Obesity and Weight Loss Strategies." February 12, 2024. https://ivypanda.com/essays/obesity-and-weight-loss-strategies/.
1. IvyPanda . "Obesity and Weight Loss Strategies." February 12, 2024. https://ivypanda.com/essays/obesity-and-weight-loss-strategies/.
Bibliography
IvyPanda . "Obesity and Weight Loss Strategies." February 12, 2024. https://ivypanda.com/essays/obesity-and-weight-loss-strategies/.
Obesity Essay
Last updated on: Feb 9, 2023
Obesity Essay: A Complete Guide and Topics
By: Nova A.
11 min read
Reviewed By: Jacklyn H.
Published on: Aug 31, 2021

Are you assigned to write an essay about obesity? The first step is to define obesity.
The obesity epidemic is a major issue facing our country right now. It's complicated- it could be genetic or due to your environment, but either way, there are ways that you can fix it!
Learn all about what causes weight gain and get tips on how you can get healthy again.

On this Page
What is Obesity
What is obesity? Obesity and BMI (body mass index) are both tools of measurement that are used by doctors to assess body fat according to the height, age, and gender of a person. If the BMI is between 25 to 29.9, that means the person has excess weight and body fat.
If the BMI exceeds 30, that means the person is obese. Obesity is a condition that increases the risk of developing cardiovascular diseases, high blood pressure, and other medical conditions like metabolic syndrome, arthritis, and even some types of cancer.
Obesity Definition
Obesity is defined by the World Health Organization as an accumulation of abnormal and excess body fat that comes with several risk factors. It is measured by the body mass index BMI, body weight (in kilograms) divided by the square of a person’s height (in meters).
Obesity in America
Obesity is on the verge of becoming an epidemic as 1 in every 3 Americans can be categorized as overweight and obese. Currently, America is an obese country, and it continues to get worse.

Paper Due? Why Suffer? That's our Job!
Causes of obesity
Do you see any obese or overweight people around you?
You likely do.
This is because fast-food chains are becoming more and more common, people are less active, and fruits and vegetables are more expensive than processed foods, thus making them less available to the majority of society. These are the primary causes of obesity.
Obesity is a disease that affects all age groups, including children and elderly people.
Now that you are familiar with the topic of obesity, writing an essay won’t be that difficult for you.
How to Write an Obesity Essay
The format of an obesity essay is similar to writing any other essay. If you need help regarding how to write an obesity essay, it is the same as writing any other essay.
Obesity Essay Introduction
The trick is to start your essay with an interesting and catchy sentence. This will help attract the reader's attention and motivate them to read further. You don’t want to lose the reader’s interest in the beginning and leave a bad impression, especially if the reader is your teacher.
A hook sentence is usually used to open the introductory paragraph of an essay in order to make it interesting. When writing an essay on obesity, the hook sentence can be in the form of an interesting fact or statistic.
Head on to this detailed article on hook examples to get a better idea.
Once you have hooked the reader, the next step is to provide them with relevant background information about the topic. Don’t give away too much at this stage or bombard them with excess information that the reader ends up getting bored with. Only share information that is necessary for the reader to understand your topic.
Next, write a strong thesis statement at the end of your essay, be sure that your thesis identifies the purpose of your essay in a clear and concise manner. Also, keep in mind that the thesis statement should be easy to justify as the body of your essay will revolve around it.
Body Paragraphs
The details related to your topic are to be included in the body paragraphs of your essay. You can use statistics, facts, and figures related to obesity to reinforce your thesis throughout your essay.
If you are writing a cause-and-effect obesity essay, you can mention different causes of obesity and how it can affect a person’s overall health. The number of body paragraphs can increase depending on the parameters of the assignment as set forth by your instructor.
Start each body paragraph with a topic sentence that is the crux of its content. It is necessary to write an engaging topic sentence as it helps grab the reader’s interest. Check out this detailed blog on writing a topic sentence to further understand it.
End your essay with a conclusion by restating your research and tying it to your thesis statement. You can also propose possible solutions to control obesity in your conclusion. Make sure that your conclusion is short yet powerful.
Obesity Essay Examples
Essay about Obesity (PDF)
Childhood Obesity Essay (PDF)
Obesity in America Essay (PDF)
Essay about Obesity Cause and Effects (PDF)
Satire Essay on Obesity (PDF)
Obesity Argumentative Essay (PDF)
Obesity Essay Topics
Choosing a topic might seem an overwhelming task as you may have many ideas for your assignment. Brainstorm different ideas and narrow them down to one, quality topic.
If you need some examples to help you with your essay topic related to obesity, dive into this article and choose from the list of obesity essay topics.
Childhood Obesity
As mentioned earlier, obesity can affect any age group, including children. Obesity can cause several future health problems as children age.
Here are a few topics you can choose from and discuss for your childhood obesity essay:
- What are the causes of increasing obesity in children?
- Obese parents may be at risk for having children with obesity.
- What is the ratio of obesity between adults and children?
- What are the possible treatments for obese children?
- Are there any social programs that can help children with combating obesity?
- Has technology boosted the rate of obesity in children?
- Are children spending more time on gadgets instead of playing outside?
- Schools should encourage regular exercises and sports for children.
- How can sports and other physical activities protect children from becoming obese?
- Can childhood abuse be a cause of obesity among children?
- What is the relationship between neglect in childhood and obesity in adulthood?
- Does obesity have any effect on the psychological condition and well-being of a child?
- Are electronic medical records effective in diagnosing obesity among children?
- Obesity can affect the academic performance of your child.
- Do you believe that children who are raised by a single parent can be vulnerable to obesity?
- You can promote interesting exercises to encourage children.
- What is the main cause of obesity, and why is it increasing with every passing day?
- Schools and colleges should work harder to develop methodologies to decrease childhood obesity.
- The government should not allow schools and colleges to include sweet or fatty snacks as a part of their lunch.
- If a mother is obese, can it affect the health of the child?
- Children who gain weight frequently can develop chronic diseases.
Obesity Argumentative Essay Topics
Do you want to write an argumentative essay on the topic of obesity?
The following list can help you with that!
Here are some examples you can choose from for your argumentative essay about obesity:
- Can vegetables and fruits decrease the chances of obesity?
- Should you go for surgery to overcome obesity?
- Are there any harmful side effects?
- Can obesity be related to the mental condition of an individual?
- Are parents responsible for controlling obesity in childhood?
- What are the most effective measures to prevent the increase in the obesity rate?
- Why is the obesity rate increasing in the United States?
- Can the lifestyle of a person be a cause of obesity?
- Does the economic situation of a country affect the obesity rate?
- How is obesity considered an international health issue?
- Can technology and gadgets affect obesity rates?
- What can be the possible reasons for obesity in a school?
- How can we address the issue of obesity?
- Is obesity a chronic disease?
- Is obesity a major cause of heart attacks?
- Are the junk food chains causing an increase in obesity?
- Do nutritional programs help in reducing the obesity rate?
- How can the right type of diet help with obesity?
- Why should we encourage sports activities in schools and colleges?
- Can obesity affect a person’s behavior?
Health Related Topics for Research Paper
If you are writing a research paper, you can explain the cause and effect of obesity.
Here are a few topics that link to the cause and effects of obesity.Review the literature of previous articles related to obesity. Describe the ideas presented in the previous papers.
- Can family history cause obesity in future generations?
- Can we predict obesity through genetic testing?
- What is the cause of the increasing obesity rate?
- Do you think the increase in fast-food restaurants is a cause of the rising obesity rate?
- Is the ratio of obese women greater than obese men?
- Why are women more prone to be obese as compared to men?
- Stress can be a cause of obesity. Mention the reasons how mental health can be related to physical health.
- Is urban life a cause of the increasing obesity rate?
- People from cities are prone to be obese as compared to people from the countryside.
- How obesity affects the life expectancy of people? What are possible solutions to decrease the obesity rate?
- Do family eating habits affect or trigger obesity?
- How do eating habits affect the health of an individual?
- How can obesity affect the future of a child?
- Obese children are more prone to get bullied in high school and college.
- Why should schools encourage more sports and exercise for children?
Tough Essay Due? Hire Tough Writers!
Topics for Essay on Obesity as a Problem
Do you think a rise in obesity rate can affect the economy of a country?
Here are some topics for your assistance regarding your economics related obesity essay.
- Does socioeconomic status affect the possibility of obesity in an individual?
- Analyze the film and write a review on “Fed Up” – an obesity epidemic.
- Share your reviews on the movie “The Weight of The Nation.”
- Should we increase the prices of fast food and decrease the prices of fruits and vegetables to decrease obesity?
- Do you think healthy food prices can be a cause of obesity?
- Describe what measures other countries have taken in order to control obesity?
- The government should play an important role in controlling obesity. What precautions should they take?
- Do you think obesity can be one of the reasons children get bullied?
- Do obese people experience any sort of discrimination or inappropriate behavior due to their weight?
- Are there any legal protections for people who suffer from discrimination due to their weight?
- Which communities have a higher percentage of obesity in the United States?
- Discuss the side effects of the fast-food industry and their advertisements on children.
- Describe how the increasing obesity rate has affected the economic condition of the United States.
- What is the current percentage of obesity all over the world? Is the obesity rate increasing with every passing day?
- Why is the obesity rate higher in the United States as compared to other countries?
- Do Asians have a greater percentage of obese people as compared to Europe?
- Does the cultural difference affect the eating habits of an individual?
- Obesity and body shaming.
- Why is a skinny body considered to be ideal? Is it an effective way to reduce the obesity rate?
Obesity Solution Essay Topics
With all the developments in medicine and technology, we still don’t have exact measures to treat obesity.
Here are some insights you can discuss in your essay:
- How do obese people suffer from metabolic complications?
- Describe the fat distribution in obese people.
- Is type 2 diabetes related to obesity?
- Are obese people more prone to suffer from diabetes in the future?
- How are cardiac diseases related to obesity?
- Can obesity affect a woman’s childbearing time phase?
- Describe the digestive diseases related to obesity.
- Obesity may be genetic.
- Obesity can cause a higher risk of suffering a heart attack.
- What are the causes of obesity? What health problems can be caused if an individual suffers from obesity?
- What are the side effects of surgery to overcome obesity?
- Which drugs are effective when it comes to the treatment of obesity?
- Is there a difference between being obese and overweight?
- Can obesity affect the sociological perspective of an individual?
- Explain how an obesity treatment works.
- How can the government help people to lose weight and improve public health?
Writing an essay is a challenging yet rewarding task. All you need is to be organized and clear when it comes to academic writing.
- Choose a topic you would like to write on.
- Organize your thoughts.
- Pen down your ideas.
- Compose a perfect essay that will help you ace your subject.
- Proofread and revise your paper.
Were the topics useful for you? We hope so!
However, if you are still struggling to write your paper, you can pick any of the topics from this list, and our essay writer will help you craft a perfect essay.
Are you struggling to write an effective essay?
If writing an essay is the actual problem and not just the topic, you can always hire an essay writing service for your help. Essay experts at 5StarEssays can help compose an impressive essay within your deadline.
All you have to do is contact us. We will get started on your paper while you can sit back and relax.
Place your order now to get an A-worthy essay.

Marketing, Thesis
As a Digital Content Strategist, Nova Allison has eight years of experience in writing both technical and scientific content. With a focus on developing online content plans that engage audiences, Nova strives to write pieces that are not only informative but captivating as well.
Was This Blog Helpful?
Keep reading.
- How to Write A Bio – Professional Tips and Examples

- Learn How to Write an Article Review with Examples

- How to Write a Poem Step-by-Step Like a Pro

- How To Write Poetry - 7 Fundamentals and Tips

- Know About Appendix Writing With the Help of Examples

- List of Social Issues Faced By the World

- How To Write A Case Study - Easy Guide

- Learn How to Avoid Plagiarism in 7 Simple Steps

- Writing Guide of Visual Analysis Essay for Beginners

- Learn How to Write a Personal Essay by Experts

- Character Analysis - A Step By Step Guide

- Thematic Statement: Writing Tips and Examples

- Expert Guide on How to Write a Summary

- How to Write an Opinion Essay - Structure, Topics & Examples

- How to Write a Synopsis - Easy Steps and Format Guide

- Learn How To Write An Editorial By Experts

- How to Get Better at Math - Easy Tips and Tricks

- How to Write a Movie Review - Steps and Examples

- Creative Writing - Easy Tips For Beginners

- Types of Plagiarism Every Student Should Know

People Also Read
- thesis statement examples
- dissertation vs thesis
- writing conventions
- improve writing skills for high school students
- transition words for essays
Burdened With Assignments?

Advertisement
- Homework Services: Essay Topics Generator
© 2024 - All rights reserved
Essay on Self Discipline for Students and Children
500+ words essay on self discipline.
Self-discipline means self-control, which gives you inner strength and a way to control yourself, actions, and reactions. It is one of the most important and useful skills to achieve success and everyone should possess this quality. Self-discipline comes naturally to some people. And some people can achieve it with some effort. The effort made is worth it as it changes life for the better. It just means exercising self- control. A person who stays in control has the ability to take charge of his/her actions and reactions.

Tips to Achieve Self-discipline
- Set your goals: – The first step towards leading a disciplined life is to set goals. Goals give you a clear idea about what needs to be achieved. One must always set a timeline for your goals. This serves as a driving force and motivates you to work hard. It is a good idea to set both short term and long term goals and create a well thought out plan to achieve them.
- Do meditation:- Meditation is one of the best ways to channel our energy in the right direction. It helps maintain focus, acquaints us with our inner self and furthers better self- control. It is the stepping stone for a disciplined life. Meditating for half an hour every day can help in inculcating self-discipline.
- Set a Routine:- Those who set a routine and follow it daily lead a more disciplined life. It is suggested to list all the tasks that you require accomplishing in a given day. Write them in the order of their priority, set a timeline for each and act accordingly. This is a good way to lead an organized and disciplined life.
- Stay away from distractions :- In this technology-driven world, there are numerous things that can distract us and take charge of our lives. Our mobile phones, television, and chatting apps are some of the new age things that are a big hindrance in practicing self-discipline. No matter how determined we are to study, work or sleep on time, we tend to get distracted at the beep of our phone. Social media platforms, chatting apps and web series are extremely addictive and hamper work. In order to practice self-discipline, it is important to stay away from these distractions. Put your phone on silent or keep it at a distance when you sit to study or work. Similarly, just put your phone away at bedtime and instead pick a book to read.
- Reward yourself :- Reward yourself for every goal you achieve. This will motivate you to work harder to achieve more. This is a good way to trick your brain to inculcate self-discipline.
- Take proper sleep :- You can inculcate self-discipline only when you are well-rested. So, it is essential to sleep for eight hours each night. Maintaining a good sleep cycle is also essential. This means that you should try sleeping and waking up at the same time each day. A power nap during the afternoon can help further.
- Stay Positive : – Many people want to inculcate self-discipline but are unable to because they somehow believe that it is difficult to achieve. They feel that it is too much to ask for and that they shall not be able to practice it. This is the wrong approach. You can achieve anything in life if you stay positive and believe in yourself. So, you should stay positive. It is a pre-requisite for inculcating self-discipline.
Get the huge list of more than 500 Essay Topics and Ideas
Self Discipline Benefits and Importance
Self-discipline helps you to overcome the bad habits by meditating regularly. It gives you the ability not to give up after failure and setbacks, develop self-control, provide the ability to resist distractions, helps you to motivate yourself until you accomplish your goals.
Achieving self-discipline may be difficult but in order to lead a healthy personal and professional life, it is very important. A self-disciplined person makes optimum use of the time. Hence, he can achieve more and do more work as compared to a person who is not self-disciplined. We should, therefore, make some efforts to achieve it.
Customize your course in 30 seconds
Which class are you in.

- Travelling Essay
- Picnic Essay
- Our Country Essay
- My Parents Essay
- Essay on Favourite Personality
- Essay on Memorable Day of My Life
- Essay on Knowledge is Power
- Essay on Gurpurab
- Essay on My Favourite Season
- Essay on Types of Sports
Leave a Reply Cancel reply
Your email address will not be published. Required fields are marked *
Download the App

- About Project
- Testimonials
Business Management Ideas

Essay on Obesity
List of essays on obesity, essay on obesity – short essay (essay 1 – 150 words), essay on obesity (essay 2 – 250 words), essay on obesity – written in english (essay 3 – 300 words), essay on obesity – for school students (class 5, 6, 7, 8, 9, 10, 11 and 12 standard) (essay 4 – 400 words), essay on obesity – for college students (essay 5 – 500 words), essay on obesity – with causes and treatment (essay 6 – 600 words), essay on obesity – for science students (essay 7 – 750 words), essay on obesity – long essay for medical students (essay 8 – 1000 words).
Obesity is a chronic health condition in which the body fat reaches abnormal level. Obesity occurs when we consume much more amount of food than our body really needs on a daily basis. In other words, when the intake of calories is greater than the calories we burn out, it gives rise to obesity.
Audience: The below given essays are exclusively written for school students (Class 5, 6, 7, 8, 9, 10, 11 and 12 Standard), college, science and medical students.
Introduction:
Obesity means being excessively fat. A person would be said to be obese if his or her body mass index is beyond 30. Such a person has a body fat rate that is disproportionate to his body mass.
Obesity and the Body Mass Index:
The body mass index is calculated considering the weight and height of a person. Thus, it is a scientific way of determining the appropriate weight of any person. When the body mass index of a person indicates that he or she is obese, it exposes the person to make health risk.
Stopping Obesity:
There are two major ways to get the body mass index of a person to a moderate rate. The first is to maintain a strict diet. The second is to engage in regular physical exercise. These two approaches are aimed at reducing the amount of fat in the body.
Conclusion:
Obesity can lead to sudden death, heart attack, diabetes and may unwanted illnesses. Stop it by making healthy choices.
Obesity has become a big concern for the youth of today’s generation. Obesity is defined as a medical condition in which an individual gains excessive body fat. When the Body Mass Index (BMI) of a person is over 30, he/ she is termed as obese.
Obesity can be a genetic problem or a disorder that is caused due to unhealthy lifestyle habits of a person. Physical inactivity and the environment in which an individual lives, are also the factors that leads to obesity. It is also seen that when some individuals are in stress or depression, they start cultivating unhealthy eating habits which eventually leads to obesity. Medications like steroids is yet another reason for obesity.
Obesity has several serious health issues associated with it. Some of the impacts of obesity are diabetes, increase of cholesterol level, high blood pressure, etc. Social impacts of obesity includes loss of confidence in an individual, lowering of self-esteem, etc.
The risks of obesity needs to be prevented. This can be done by adopting healthy eating habits, doing some physical exercise regularly, avoiding stress, etc. Individuals should work on weight reduction in order to avoid obesity.
Obesity is indeed a health concern and needs to be prioritized. The management of obesity revolves around healthy eating habits and physical activity. Obesity, if not controlled in its initial stage can cause many severe health issues. So it is wiser to exercise daily and maintain a healthy lifestyle rather than being the victim of obesity.
Obesity can be defined as the clinical condition where accumulation of excessive fat takes place in the adipose tissue leading to worsening of health condition. Usually, the fat is deposited around the trunk and also the waist of the body or even around the periphery.
Obesity is actually a disease that has been spreading far and wide. It is preventable and certain measures are to be taken to curb it to a greater extend. Both in the developing and developed countries, obesity has been growing far and wide affecting the young and the old equally.
The alarming increase in obesity has resulted in stimulated death rate and health issues among the people. There are several methods adopted to lose weight and they include different diet types, physical activity and certain changes in the current lifestyle. Many of the companies are into minting money with the concept of inviting people to fight obesity.
In patients associated with increased risk factor related to obesity, there are certain drug therapies and other procedures adopted to lose weight. There are certain cost effective ways introduced by several companies to enable clinic-based weight loss programs.
Obesity can lead to premature death and even cause Type 2 Diabetes Mellitus. Cardiovascular diseases have also become the part and parcel of obese people. It includes stroke, hypertension, gall bladder disease, coronary heart disease and even cancers like breast cancer, prostate cancer, endometrial cancer and colon cancer. Other less severe arising due to obesity includes osteoarthritis, gastro-esophageal reflux disease and even infertility.
Hence, serious measures are to be taken to fight against this dreadful phenomenon that is spreading its wings far and wide. Giving proper education on benefits of staying fit and mindful eating is as important as curbing this issue. Utmost importance must be given to healthy eating habits right from the small age so that they follow the same until the end of their life.
Obesity is majorly a lifestyle disease attributed to the extra accumulation of fat in the body leading to negative health effects on a person. Ironically, although prevalent at a large scale in many countries, including India, it is one of the most neglect health problems. It is more often ignored even if told by the doctor that the person is obese. Only when people start acquiring other health issues such as heart disease, blood pressure or diabetes, they start taking the problem of obesity seriously.
Obesity Statistics in India:
As per a report, India happens to figure as the third country in the world with the most obese people. This should be a troubling fact for India. However, we are yet to see concrete measures being adopted by the people to remain fit.
Causes of Obesity:
Sedentary lifestyle, alcohol, junk food, medications and some diseases such as hypothyroidism are considered as the factors which lead to obesity. Even children seem to be glued to televisions, laptops and video games which have taken away the urge for physical activities from them. Adding to this, the consumption of junk food has further aggravated the growing problem of obesity in children.
In the case of adults, most of the professions of today make use of computers which again makes people sit for long hours in one place. Also, the hectic lifestyle of today makes it difficult for people to spare time for physical activities and people usually remain stressed most of the times. All this has contributed significantly to the rise of obesity in India.
Obesity and BMI:
Body Mass Index (BMI) is the measure which allows a person to calculate how to fit he or she is. In other words, the BMI tells you if you are obese or not. BMI is calculated by dividing the weight of a person in kg with the square of his / her height in metres. The number thus obtained is called the BMI. A BMI of less than 25 is considered optimal. However, if a person has a BMI over 30 he/she is termed as obese.
What is a matter of concern is that with growing urbanisation there has been a rapid increase of obese people in India? It is of utmost importance to consider this health issue a serious threat to the future of our country as a healthy body is important for a healthy soul. We should all be mindful of what we eat and what effect it has on our body. It is our utmost duty to educate not just ourselves but others as well about this serious health hazard.
Obesity can be defined as a condition (medical) that is the accumulation of body fat to an extent that the excess fat begins to have a lot of negative effects on the health of the individual. Obesity is determined by examining the body mass index (BMI) of the person. The BMI is gotten by dividing the weight of the person in kilogram by the height of the person squared.
When the BMI of a person is more than 30, the person is classified as being obese, when the BMI falls between 25 and 30, the person is said to be overweight. In a few countries in East Asia, lower values for the BMI are used. Obesity has been proven to influence the likelihood and risk of many conditions and disease, most especially diabetes of type 2, cardiovascular diseases, sleeplessness that is obstructive, depression, osteoarthritis and some cancer types.
In most cases, obesity is caused through a combination of genetic susceptibility, a lack of or inadequate physical activity, excessive intake of food. Some cases of obesity are primarily caused by mental disorder, medications, endocrine disorders or genes. There is no medical data to support the fact that people suffering from obesity eat very little but gain a lot of weight because of slower metabolism. It has been discovered that an obese person usually expends much more energy than other people as a result of the required energy that is needed to maintain a body mass that is increased.
It is very possible to prevent obesity with a combination of personal choices and social changes. The major treatments are exercising and a change in diet. We can improve the quality of our diet by reducing our consumption of foods that are energy-dense like those that are high in sugars or fat and by trying to increase our dietary fibre intake.
We can also accompany the appropriate diet with the use of medications to help in reducing appetite and decreasing the absorption of fat. If medication, exercise and diet are not yielding any positive results, surgery or gastric balloon can also be carried out to decrease the volume of the stomach and also reduce the intestines’ length which leads to the feel of the person get full early or a reduction in the ability to get and absorb different nutrients from a food.
Obesity is the leading cause of ill-health and death all over the world that is preventable. The rate of obesity in children and adults has drastically increased. In 2015, a whopping 12 percent of adults which is about 600 million and about 100 million children all around the world were found to be obese.
It has also been discovered that women are more obese than men. A lot of government and private institutions and bodies have stated that obesity is top of the list of the most difficult and serious problems of public health that we have in the world today. In the world we live today, there is a lot of stigmatisation of obese people.
We all know how troubling the problem of obesity truly is. It is mainly a form of a medical condition wherein the body tends to accumulate excessive fat which in turn has negative repercussions on the health of an individual.
Given the current lifestyle and dietary style, it has become more common than ever. More and more people are being diagnosed with obesity. Such is its prevalence that it has been termed as an epidemic in the USA. Those who suffer from obesity are at a much higher risk of diabetes, heart diseases and even cancer.
In order to gain a deeper understanding of obesity, it is important to learn what the key causes of obesity are. In a layman term, if your calorie consumption exceeds what you burn because of daily activities and exercises, it is likely to lead to obesity. It is caused over a prolonged period of time when your calorie intake keeps exceeding the calories burned.
Here are some of the key causes which are known to be the driving factors for obesity.
If your diet tends to be rich in fat and contains massive calorie intake, you are all set to suffer from obesity.
Sedentary Lifestyle:
With most people sticking to their desk jobs and living a sedentary lifestyle, the body tends to get obese easily.
Of course, the genetic framework has a lot to do with obesity. If your parents are obese, the chance of you being obese is quite high.
The weight which women gain during their pregnancy can be very hard to shed and this is often one of the top causes of obesity.
Sleep Cycle:
If you are not getting an adequate amount of sleep, it can have an impact on the hormones which might trigger hunger signals. Overall, these linked events tend to make you obese.
Hormonal Disorder:
There are several hormonal changes which are known to be direct causes of obesity. The imbalance of the thyroid stimulating hormone, for instance, is one of the key factors when it comes to obesity.
Now that we know the key causes, let us look at the possible ways by which you can handle it.
Treatment for Obesity:
As strange as it may sound, the treatment for obesity is really simple. All you need to do is follow the right diet and back it with an adequate amount of exercise. If you can succeed in doing so, it will give you the perfect head-start into your journey of getting in shape and bidding goodbye to obesity.
There are a lot of different kinds and styles of diet plans for obesity which are available. You can choose the one which you deem fit. We recommend not opting for crash dieting as it is known to have several repercussions and can make your body terribly weak.
The key here is to stick to a balanced diet which can help you retain the essential nutrients, minerals, and, vitamins and shed the unwanted fat and carbs.
Just like the diet, there are several workout plans for obesity which are available. It is upon you to find out which of the workout plan seems to be apt for you. Choose cardio exercises and dance routines like Zumba to shed the unwanted body weight. Yoga is yet another method to get rid of obesity.
So, follow a blend of these and you will be able to deal with the trouble of obesity in no time. We believe that following these tips will help you get rid of obesity and stay in shape.
Obesity and overweight is a top health concern in the world due to the impact it has on the lives of individuals. Obesity is defined as a condition in which an individual has excessive body fat and is measured using the body mass index (BMI) such that, when an individual’s BMI is above 30, he or she is termed obese. The BMI is calculated using body weight and height and it is different for all individuals.
Obesity has been determined as a risk factor for many diseases. It results from dietary habits, genetics, and lifestyle habits including physical inactivity. Obesity can be prevented so that individuals do not end up having serious complications and health problems. Chronic illnesses like diabetes, heart diseases and relate to obesity in terms of causes and complications.
Factors Influencing Obesity:
Obesity is not only as a result of lifestyle habits as most people put it. There are other important factors that influence obesity. Genetics is one of those factors. A person could be born with genes that predispose them to obesity and they will also have difficulty in losing weight because it is an inborn factor.
The environment also influences obesity because the diet is similar in certain environs. In certain environments, like school, the food available is fast foods and the chances of getting healthy foods is very low, leading to obesity. Also, physical inactivity is an environmental factor for obesity because some places have no fields or tracks where people can jog or maybe the place is very unsafe and people rarely go out to exercise.
Mental health affects the eating habits of individuals. There is a habit of stress eating when a person is depressed and it could result in overweight or obesity if the person remains unhealthy for long period of time.
The overall health of individuals also matter. If a person is unwell and is prescribed with steroids, they may end up being obese. Steroidal medications enable weight gain as a side effect.
Complications of Obesity:
Obesity is a health concern because its complications are severe. Significant social and health problems are experienced by obese people. Socially, they will be bullied and their self-esteem will be low as they will perceive themselves as unworthy.
Chronic illnesses like diabetes results from obesity. Diabetes type 2 has been directly linked to obesity. This condition involves the increased blood sugars in the body and body cells are not responding to insulin as they should. The insulin in the body could also be inadequate due to decreased production. High blood sugar concentrations result in symptoms like frequent hunger, thirst and urination. The symptoms of complicated stages of diabetes type 2 include loss of vision, renal failure and heart failure and eventually death. The importance of having a normal BMI is the ability of the body to control blood sugars.
Another complication is the heightened blood pressures. Obesity has been defined as excessive body fat. The body fat accumulates in blood vessels making them narrow. Narrow blood vessels cause the blood pressures to rise. Increased blood pressure causes the heart to start failing in its physiological functions. Heart failure is the end result in this condition of increased blood pressures.
There is a significant increase in cholesterol in blood of people who are obese. High blood cholesterol levels causes the deposition of fats in various parts of the body and organs. Deposition of fats in the heart and blood vessels result in heart diseases. There are other conditions that result from hypercholesterolemia.
Other chronic illnesses like cancer can also arise from obesity because inflammation of body cells and tissues occurs in order to store fats in obese people. This could result in abnormal growths and alteration of cell morphology. The abnormal growths could be cancerous.
Management of Obesity:
For the people at risk of developing obesity, prevention methods can be implemented. Prevention included a healthy diet and physical activity. The diet and physical activity patterns should be regular and realizable to avoid strains that could result in complications.
Some risk factors for obesity are non-modifiable for example genetics. When a person in genetically predisposed, the lifestyle modifications may be have help.
For the individuals who are already obese, they can work on weight reduction through healthy diets and physical exercises.
In conclusion, obesity is indeed a major health concern because the health complications are very serious. Factors influencing obesity are both modifiable and non-modifiable. The management of obesity revolves around diet and physical activity and so it is important to remain fit.
In olden days, obesity used to affect only adults. However, in the present time, obesity has become a worldwide problem that hits the kids as well. Let’s find out the most prevalent causes of obesity.
Factors Causing Obesity:
Obesity can be due to genetic factors. If a person’s family has a history of obesity, chances are high that he/ she would also be affected by obesity, sooner or later in life.
The second reason is having a poor lifestyle. Now, there are a variety of factors that fall under the category of poor lifestyle. An excessive diet, i.e., eating more than you need is a definite way to attain the stage of obesity. Needless to say, the extra calories are changed into fat and cause obesity.
Junk foods, fried foods, refined foods with high fats and sugar are also responsible for causing obesity in both adults and kids. Lack of physical activity prevents the burning of extra calories, again, leading us all to the path of obesity.
But sometimes, there may also be some indirect causes of obesity. The secondary reasons could be related to our mental and psychological health. Depression, anxiety, stress, and emotional troubles are well-known factors of obesity.
Physical ailments such as hypothyroidism, ovarian cysts, and diabetes often complicate the physical condition and play a massive role in abnormal weight gain.
Moreover, certain medications, such as steroids, antidepressants, and contraceptive pills, have been seen interfering with the metabolic activities of the body. As a result, the long-term use of such drugs can cause obesity. Adding to that, regular consumption of alcohol and smoking are also connected to the condition of obesity.
Harmful Effects of Obesity:
On the surface, obesity may look like a single problem. But, in reality, it is the mother of several major health issues. Obesity simply means excessive fat depositing into our body including the arteries. The drastic consequence of such high cholesterol levels shows up in the form of heart attacks and other life-threatening cardiac troubles.
The fat deposition also hampers the elasticity of the arteries. That means obesity can cause havoc in our body by altering the blood pressure to an abnormal range. And this is just the tip of the iceberg. Obesity is known to create an endless list of problems.
In extreme cases, this disorder gives birth to acute diseases like diabetes and cancer. The weight gain due to obesity puts a lot of pressure on the bones of the body, especially of the legs. This, in turn, makes our bones weak and disturbs their smooth movement. A person suffering from obesity also has higher chances of developing infertility issues and sleep troubles.
Many obese people are seen to be struggling with breathing problems too. In the chronic form, the condition can grow into asthma. The psychological effects of obesity are another serious topic. You can say that obesity and depression form a loop. The more a person is obese, the worse is his/ her depression stage.
How to Control and Treat Obesity:
The simplest and most effective way, to begin with, is changing our diet. There are two factors to consider in the diet plan. First is what and what not to eat. Second is how much to eat.
If you really want to get rid of obesity, include more and more green vegetables in your diet. Spinach, beans, kale, broccoli, cauliflower, asparagus, etc., have enough vitamins and minerals and quite low calories. Other healthier options are mushrooms, pumpkin, beetroots, and sweet potatoes, etc.
Opt for fresh fruits, especially citrus fruits, and berries. Oranges, grapes, pomegranate, pineapple, cherries, strawberries, lime, and cranberries are good for the body. They have low sugar content and are also helpful in strengthening our immune system. Eating the whole fruits is a more preferable way in comparison to gulping the fruit juices. Fruits, when eaten whole, have more fibers and less sugar.
Consuming a big bowl of salad is also great for dealing with the obesity problem. A salad that includes fibrous foods such as carrots, radish, lettuce, tomatoes, works better at satiating the hunger pangs without the risk of weight gain.
A high protein diet of eggs, fish, lean meats, etc., is an excellent choice to get rid of obesity. Take enough of omega fatty acids. Remember to drink plenty of water. Keeping yourself hydrated is a smart way to avoid overeating. Water also helps in removing the toxins and excess fat from the body.
As much as possible, avoid fats, sugars, refined flours, and oily foods to keep the weight in control. Control your portion size. Replace the three heavy meals with small and frequent meals during the day. Snacking on sugarless smoothies, dry fruits, etc., is much recommended.
Regular exercise plays an indispensable role in tackling the obesity problem. Whenever possible, walk to the market, take stairs instead of a lift. Physical activity can be in any other form. It could be a favorite hobby like swimming, cycling, lawn tennis, or light jogging.
Meditation and yoga are quite powerful practices to drive away the stress, depression and thus, obesity. But in more serious cases, meeting a physician is the most appropriate strategy. Sometimes, the right medicines and surgical procedures are necessary to control the health condition.
Obesity is spreading like an epidemic, haunting both the adults and the kids. Although genetic factors and other physical ailments play a role, the problem is mostly caused by a reckless lifestyle.
By changing our way of living, we can surely take control of our health. In other words, it would be possible to eliminate the condition of obesity from our lives completely by leading a healthy lifestyle.
Health , Obesity
Get FREE Work-at-Home Job Leads Delivered Weekly!

Join more than 50,000 subscribers receiving regular updates! Plus, get a FREE copy of How to Make Money Blogging!
Message from Sophia!
Like this post? Don’t forget to share it!
Here are a few recommended articles for you to read next:
- Essay on Cleanliness
- Essay on Cancer
- Essay on AIDS
- Essay on Health and Fitness
No comments yet.
Leave a reply click here to cancel reply..
You must be logged in to post a comment.
Billionaires
- Donald Trump
- Warren Buffett
- Email Address
- Free Stock Photos
- Keyword Research Tools
- URL Shortener Tools
- WordPress Theme
Book Summaries
- How To Win Friends
- Rich Dad Poor Dad
- The Code of the Extraordinary Mind
- The Luck Factor
- The Millionaire Fastlane
- The ONE Thing
- Think and Grow Rich
- 100 Million Dollar Business
- Business Ideas
Digital Marketing
- Mobile Addiction
- Social Media Addiction
- Computer Addiction
- Drug Addiction
- Internet Addiction
- TV Addiction
- Healthy Habits
- Morning Rituals
- Wake up Early
- Cholesterol
- Reducing Cholesterol
- Fat Loss Diet Plan
- Reducing Hair Fall
- Sleep Apnea
- Weight Loss
Internet Marketing
- Email Marketing
Law of Attraction
- Subconscious Mind
- Vision Board
- Visualization
Law of Vibration
- Professional Life
Motivational Speakers
- Bob Proctor
- Robert Kiyosaki
- Vivek Bindra
- Inner Peace
Productivity
- Not To-do List
- Project Management Software
- Negative Energies
Relationship
- Getting Back Your Ex
Self-help 21 and 14 Days Course
Self-improvement.
- Body Language
- Complainers
- Emotional Intelligence
- Personality
Social Media
- Project Management
- Anik Singal
- Baba Ramdev
- Dwayne Johnson
- Jackie Chan
- Leonardo DiCaprio
- Narendra Modi
- Nikola Tesla
- Sachin Tendulkar
- Sandeep Maheshwari
- Shaqir Hussyin
Website Development
Wisdom post, worlds most.
- Expensive Cars
Our Portals: Gulf Canada USA Italy Gulf UK
Privacy Overview
| Cookie | Duration | Description |
|---|---|---|
| cookielawinfo-checkbox-analytics | 11 months | This cookie is set by GDPR Cookie Consent plugin. The cookie is used to store the user consent for the cookies in the category "Analytics". |
| cookielawinfo-checkbox-functional | 11 months | The cookie is set by GDPR cookie consent to record the user consent for the cookies in the category "Functional". |
| cookielawinfo-checkbox-necessary | 11 months | This cookie is set by GDPR Cookie Consent plugin. The cookies is used to store the user consent for the cookies in the category "Necessary". |
| cookielawinfo-checkbox-others | 11 months | This cookie is set by GDPR Cookie Consent plugin. The cookie is used to store the user consent for the cookies in the category "Other. |
| cookielawinfo-checkbox-performance | 11 months | This cookie is set by GDPR Cookie Consent plugin. The cookie is used to store the user consent for the cookies in the category "Performance". |
| viewed_cookie_policy | 11 months | The cookie is set by the GDPR Cookie Consent plugin and is used to store whether or not user has consented to the use of cookies. It does not store any personal data. |
Essay Service Examples Education Discipline
Self Discipline Essays
- Proper editing and formatting
- Free revision, title page, and bibliography
- Flexible prices and money-back guarantee

Discipline Essay 1 (100 words)
Discipline essay 2 (200 words), discipline essay 3 (300 words), discipline essay 4 (400 words), introduction, importance of discipline, discipline essay 5 (500 words), necessity of discipline, forms of discipline, discipline essay 6 (600 words), importance and types of discipline, the need for discipline, advantages of discipline, discipline essay 7 (600 words), importance and benefits, discipline in student’s life, discipline essay 8 (800 words), discipline – what we understand, importance of being self-disciplined, advantages of being disciplined, examples from history, discipline essay 9 (1100 words).
Our writers will provide you with an essay sample written from scratch: any topic, any deadline, any instructions.
Cite this paper
Related essay topics.
Get your paper done in as fast as 3 hours, 24/7.
Related articles

Most popular essays
My overall philosophy of discipline is that it should be fair, consistent, and reflect what would...
- Perspective
- Public School
I am a kindergarten teacher working at the Early Birds Kindergarten, Nursery and Childcare Centre....
- Critical Thinking
Culture of discipline is a phrase used by Jim Collins (Good to Great) in his study of great...
Self-discipline: Build mental toughness, Increase focus, Stop procrastinating and Achieve your...
- Academic Performance
Discipline is the key to attain and achieved our goal's in life. We as a future educator's,...
Do you know the difference between discipline and punishment with their Latin roots? Punishment...
- Child Abuse
Parents physically abuse their kids. It’s a practice that parents have been using for countless...
Discipline is mainly to teach and guide with love to your children — it's not to Physically punish...
As a parent, it’s their job to educate and support their child all throughout their childhood and...
Join our 150k of happy users
- Get original paper written according to your instructions
- Save time for what matters most
Fair Use Policy
EduBirdie considers academic integrity to be the essential part of the learning process and does not support any violation of the academic standards. Should you have any questions regarding our Fair Use Policy or become aware of any violations, please do not hesitate to contact us via [email protected].
We are here 24/7 to write your paper in as fast as 3 hours.
Provide your email, and we'll send you this sample!
By providing your email, you agree to our Terms & Conditions and Privacy Policy .
Say goodbye to copy-pasting!
Get custom-crafted papers for you.
Enter your email, and we'll promptly send you the full essay. No need to copy piece by piece. It's in your inbox!

Why Self-Discipline is Important (11 Key Reasons)
Have you ever wondered why self-discipline is important?
This article is going to help answer that question. I am going to go over:
- WHAT self-discipline is
- Why self-discipline can be CHALLENGING
- Why self-discipline is IMPORTANT
Including providing 11 huge reasons WHY self-discipline is IMPORTANT, and can transform your life!
What Self-Discipline Is
Here is the definition of self-discipline according to a few sources:
“The ability to make yourself do things when you should, even if you do not want to do them.” ( Cambridge Dictionary )
“Discipline and training of oneself, usually for improvement.” ( Dictionary.com )
“The ability to control one’s feelings and overcome one’s weaknesses; the ability to pursue what one thinks is right despite temptations to abandon it.” ( Oxford Dictionary )
“The ability to make yourself do things that should be done.” ( Merriam-Webster )
Common Themes Across Definitions
Although the definitions vary a bit, a few key themes emerge.
Self-discipline is about…
- Controlling yourself
- Making yourself do things
- Self-improvement
The Meaning of Self-Discipline
Here is a definition which ties all these themes together:
Self-discipline is about learning to control yourself so you can work towards your goals, even when no one is forcing you to do so.
Why Self-Discipline Can Be Challenging
Why is it that self-discipline can be challenging for a lot of people?
Controlling Yourself is the Hard Part
The “controlling yourself” aspect is the big challenge.
You often know what you need to do to achieve a goal. (Or at least you have the capacity to learn the knowledge and skills which are required).
But despite knowing what you need to get done, consistently working towards your goals without procrastinating or getting distracted can be difficult.
Imagine if you were a character in a video game, and you were controlling yourself. Self-discipline wouldn’t be an issue.
You simply would click a button and you would do whatever you needed to get done.
- Make your video game self take a programming course
- Make your video game self apply for fancy tech jobs with super high salaries
- Don’t let your video game self get discouraged and sit in pajamas all day re-watching all The Lord of the Rings movies
- Make your video game self stick to a diet
- Make your video game self exercise
- Don’t let your video game self give up and binge on Doritos and ice cream until four in the morning
Just imagine how successful your actual self would be if you treated yourself the way you would treat your video game self?
The problem is, in real life, there are a few challenges that you don’t have in the video game scenario.
Real-Life Challenges to Being Self-Disciplined
- Needing to mentally and/or physically exert yourself
- Dealing with emotions , such as worry, doubt, or fear
- Conflicting priorities that make it difficult to determine what to focus on
- Having a vague sense of what you need to do, but not knowing the specific steps involved or how to get started
- Being impacted by tough life events or going through bad ruts that make self-discipline even harder
These are enormous obstacles, but are possible to overcome.
11 Reasons Why Self-Discipline is Important
Although self-discipline can be hard, it is worth developing, because it is capable of transforming your life in monumental ways.
Here are 11 reasons why self-discipline is important to develop.
Why Self-Discipline is Important – Reason #1: Self-Discipline Helps You Achieve Your Goals
One of the biggest reasons to learn self-discipline, is that it will help you follow through with your goals.
Although there are some things you can get done without self-discipline, most goals require self-discipline to accomplish.
For most things in life, no one is going to be there to force you to follow through with those things every step of the way.
When you are a kid, you can get by without self-discipline because your parents and teachers tell you to do things.
But at some point, you need self-discipline to get things done.
The amazing thing about self-discipline, is once you build it, you can use it to accomplish any goal you want.
Whether that is:
- Getting in better shape
- Advancing your career
- Forming stronger connections with people
- Starting a business
- Learning an instrument
- Writing a book
Or whatever else you dream of doing.
Why Self-Discipline is Important – Reason #2: Self-Discipline Benefits Your Future Self
There is a theory called Present Bias which states that most of the time we do things to benefit our Present Selves, and we discount the effects our actions have on our Future Selves.
For example, you eat a cookie because it tastes good in the moment.
Even though you know that in the future too many cookies can negatively impact your health.
Self-discipline gives you the power of delayed gratification . Which means you can resist short-term rewards in favor of long-term benefits.
And the best thing about self-discipline is you don’t ALWAYS have to delay gratification.
Your Present Self matters too.
But self-discipline puts you in charge. So you have the ability to do things which are hard in the moment, but benefit your Future Self.
Why Self-Discipline is Important – Reason #3: Self-Discipline Involves Forming Good Habits
Habits can be extremely powerful.
Habits are about getting things so ingrained into your routine that you consistently do them without giving them a second thought.
A big part of self-discipline involves forming good habits that enable you to stick with your goals for the long-run.
Why Self-Discipline is Important – Reason #4: Self-Discipline Helps You Break Bad Habits
On the flip side of good habits, are bad habits.
Examples include:
- Maintaining a bad sleep schedule
- Wasting more time than you want to on the internet or social media
- Eating too much junk food
Keep in mind, some bad habits are very personal and what is bad for one person might not be bad for another.
For example, I know people who spend large periods of the day playing video games and are perfectly happy.
But there are other people who want to reduce how much time they devote to video games , so they have more time for other stuff.
Whatever you consider you bad habits, self-discipline will help you control them – by either reducing the amount of time you spend on them or eliminating them entirely.
Side note, here are a few resources on how to break bad habits you may find helpful:
- Moderating Behavior —> Using The Who What When Where Why Method : A full, in-depth guide on how to control bad habits, which you get if you signup for my newsletter (for free).
- How to Cure Your Phone Addiction : Figure out how to BREAK your phone addiction using several POWERFUL strategies which have helped me cure my own phone addiction.
Why Self-Discipline is Important – Reason #5: Self-Discipline Helps You Stop Procrastinating
Another reason why self-discipline is important, is that it helps you stop procrastinating.
Procrastination is the act of putting something off that you need or want to get done.
Self-discipline helps you reduce the amount of time you spend procrastinating, and helps you get started with the things you have been postponing.
Side note – Here is an article with more information on how to stop procrastinating .
Why Self-Discipline is Important – Reason #6: The Spillover Effect
The Spillover Effect is the idea that sometimes progress in one area (even if really small) can lead to a series of exponential breakthroughs in other areas of your life.
This effect is really strong when it comes to self-discipline.
Since as you build self-discipline in one area of your life, you often start seeing positive changes in other areas of your life as well.
For example, I used to have zero self-discipline in all aspects of life. Work, school, exercise. You name it.
But I finally had a breakthrough when it came to working out.
Not only was that amazing in its own right, but once I found out how to be disciplined when it came to working out, it started becoming easier to get disciplined in OTHER areas of my life as well.
My discipline in exercise eventually led me to be more disciplined in a ton of other areas.
- And finances
Plus, it boosted my confidence which helped my self-esteem and social life.
Sometimes all it takes is becoming self-disciplined in ONE area of your life to spark a SERIES of positive life changes.
Side note – If you are interested in more on exercise, check out my article on how to stick to a workout schedule .
Why Self-Discipline is Important – Reason #7: Self-Discipline Gives You Confidence
As you start to build self-discipline, you will start to gain confidence in yourself.
There are two reasons for this.
First, as you get more self-disciplined, you will start making progress towards your goals, which will give you a sense of accomplishment.
Second, you will start to create a positive feedback loop, which looks like this:
- Achieving more goals —> Increased confidence
- Increased confidence —> Achieving more goals
- The initial goals you accomplish increase your confidence and belief in yourself.
- Which make it easier to accomplish even more goals.
- Which then leads to even more confidence.
Why Self-Discipline is Important – Reason #8: Self-Discipline Improves Your Time Management Skills
Time management is about regulating how much time you spend on specific goals or tasks, in order to accomplish your goals in the most efficient manner possible.
Learning self-discipline and time management go hand-in-hand, as a big part of self-discipline is figuring out how to manage your time effectively.
Self-discipline involves learning how to allocate your time to different goals, and how to execute them as efficiently and productively as you can.
Why Self-Discipline is Important – Reason #9: Self-Discipline Allows You to Follow Through with Your Great Ideas
Have you ever had a brilliant idea, but then never did anything with it?
We’ve all had those ideas we regret never following through on.
Self-discipline will help you make your ideas a reality.
I’m not saying they are going to all work out. But at the very least, with self-discipline, you will give them a shot.
For instance:
- If you have a business idea, self-discipline will help you do what you need to do to start that business.
- If you have an idea for a novel, self-discipline will help you write your story.
Whatever your great idea is, self-discipline will help you execute it – and not just keep telling yourself you are going to get to it “eventually.”
Why Self-Discipline is Important – Reason #10: Self-Discipline is Important Because it is Within Your Sphere of Influence
There are so many things in life which are outside of our control:
- Where you are born
- Who your family is
- How tall or short you are
But self-discipline is one of the few things that is within your sphere of influence. And that makes it all the more important to develop.
Why Self-Discipline is Important – Reason #11: Self-Discipline Can Help You Find Your Sense of Purpose
As you build self-discipline, you will start making progress towards your goals.
And as you progress, some of those goals may send you in a direction you couldn’t have even imagined your life would go in.
You may discover a career you want to pursue. A hobby you are passionate about. Or even a person you fall in love with.
You don’t necessarily have to have one single sense of purpose.
But as self-discipline opens up new doors through a continued process of self-improvement and self-discovery, you may find layers of meaning somewhere along your journey.
Free “Why Self-Discipline is Important” Cheat Sheet
Click here to get a free PDF cheat sheet for this article when you sign up for The Disciplined Rebel Newsletter!
The newsletter is all about how to build self-discipline . You will get also get access to other great newsletter-only resources as well.
How to Build Self-Discipline
So now that you’ve learned why self-discipline is important, the next step is to figure out how to build it!
Check here to learn how to build self-discipline
This article contains some of my best resources on how to build self-discipline.
PS: You may be interested in this article/video on why self-discipline is difficult and how to make it easier.

Essay on Self Discipline
Students are often asked to write an essay on Self Discipline in their schools and colleges. And if you’re also looking for the same, we have created 100-word, 250-word, and 500-word essays on the topic.
Let’s take a look…
100 Words Essay on Self Discipline
Introduction.
Self-discipline is the ability to control one’s feelings and overcome weaknesses. It’s about making choices that lead to healthy, productive behaviors.
Importance of Self-Discipline
Self-discipline is crucial for success. It helps us focus on our goals, resist temptations, and persist in the face of adversity.
Building Self-Discipline
Building self-discipline requires practice. Start small, create routines, and gradually take on bigger challenges.
Benefits of Self-Discipline
Self-discipline leads to improved focus, better health, and achievement of goals. It also fosters resilience and self-confidence.
Also check:
250 Words Essay on Self Discipline
Self-discipline, an essential attribute for personal and professional success, refers to the ability to control one’s emotions, behavior, and desires, aligning them with set goals. It is a skill that enables individuals to overcome impulses, procrastinate less, and stay focused on their objectives.
The Importance of Self-Discipline
Self-discipline is a cornerstone of personal development and self-improvement. It fosters resilience, enabling individuals to endure hardships and persevere in the face of challenges. Furthermore, it promotes time management, allowing for the prioritization of tasks according to their importance and urgency. This leads to increased productivity and efficiency.
Self-Discipline and Success
The correlation between self-discipline and success is well-established. Those with high self-discipline tend to perform better academically and professionally. They are also more likely to maintain a healthy lifestyle, manage stress effectively, and demonstrate higher levels of happiness.
Developing Self-Discipline
Developing self-discipline requires consistent effort and practice. It starts with setting clear, achievable goals, followed by creating a plan to reach them. Regular self-reflection is crucial to assess progress and make necessary adjustments. Moreover, cultivating a positive mindset can significantly enhance one’s self-discipline.
500 Words Essay on Self Discipline
Introduction to self-discipline.
Self-discipline, an essential characteristic for personal and professional success, is the ability to control one’s feelings and overcome weaknesses. It involves acting according to what you think instead of how you feel in the moment. It’s a sign of inner strength and control of oneself and one’s actions.
Self-discipline is of paramount importance for achieving goals. It is the backbone of successful people who manage to excel in their fields. It is the driving force that compels individuals to resist negative impulses and distractions. Self-discipline is the key to consistency and continuity in any endeavor, be it academic, personal, or professional. It helps in maintaining focus, thus enabling individuals to make constructive decisions that lead to positive outcomes.
Self-Discipline and Time Management
Self-discipline and emotional control.
Building self-discipline is a gradual process that requires patience and perseverance. It begins with setting clear goals and establishing a plan to achieve them. It requires consistent practice and the willingness to step out of one’s comfort zone. Regular exercise, a healthy diet, and adequate sleep are also integral in fostering self-discipline as they enhance mental strength and focus.
Challenges and Solutions
That’s it! I hope the essay helped you.
If you’re looking for more, here are essays on other interesting topics:
Happy studying!
Leave a Reply Cancel reply
Save my name, email, and website in this browser for the next time I comment.

- Skip to main content
- Skip to secondary menu
- Skip to primary sidebar
- Skip to footer
A Plus Topper
Improve your Grades
Importance of Self Discipline Essay | Essay on Importance of Self Discipline for Students and Children in English
February 13, 2024 by Prasanna
Importance of Self Discipline Essay: Self-Discipline means having control over oneself; it provides self-control overreactions, actions, and oneself and boosts a person’s inner strength. Self- Discipline is the most important skill a person should possess. One of the main attributes of Self-Discipline is its ability to abdicate immediate pleasure and gratification.
Self-Discipline does not necessarily mean to live a controlled or restrictive lifestyle, but to have control over oneself. It gives a person the power to make the right decisions, despite temptations, and achieve goals. Furthermore, the skill manifests as inner strength leading to strong willpower and overcoming procrastination, laziness, addictions, and overeating.
Thus, Self-discipline is a skill that leads one to achieve success.
Long and Short Essays on Importance of Self Discipline in English for Students and Kids
Below we have provided a Long, descriptive Essay and a Short, brief Essay. The extended essay consists of 400-500 words and is a guideline to help students with their essay topic. The short essay contains 150-200 words to help and guide children and kids.
Long Essay On Importance of Self Discipline 500 Words in English
The long essay mentioned below is for students belonging to classes 6,7,8,9, and 10, and competitive exam aspirants. The essay is a guide to help with class assignments, comprehension, and competitive examinations.
Self-Discipline is the ability to control and avoid unhealthy habits or excess that could create a negative impact. A self-disciplined person rejects any immediate pleasure or gratifications that favors more significant pain but requires time and effort to mold the skill.
The possession of Self-Discipline enables an individual to choose the right decisions, and maintain their thoughts, behavior, and actions, to attain success and improvement. Every person needs to possess the skill of self-discipline. Self-Discipline strengthens those who acknowledge it and yet only a few put efforts to develop it.
Life throws a series of challenges on the path to attain success and achievement. To rise above the obstacles, one needs to imbibe the habit of persistence and perseverance, which can be achieved through self-discipline. Furthermore, it helps an individual overcome his/her negative habits.
Importance of Self Discipline
Habit either creates or destroys a person; Self Discipline builds a pattern through discipline. It directs a person to stay consistent in work and reach the door that opens success.
It helps a person organize his/her schedule and get things done accordingly. It makes a person remain consistent in their work and helps them achieve success.
Life is a cycle of distractions and challenges, but a self-disciplined person focuses on the goals. Self-discipline singles out your goal from the rest of the distractions and fixates him/her to achieve great things in life.
Self-discipline boosts a person’s work ethic and self-esteem simultaneously—furthermore, self-discipline molds a person to become an improved version of themselves.
Through self-discipline, a person nurtures his path with confidence, inner strength, and self-esteem, leading to satisfaction and happiness. Contrarily, a person who lacks this ability falls into the pits of loss, failure, health and relationship problems, gluttony and obesity, and other related troubles.
Steps to achieve Self-Discipline
- Set your goals: Goals give you a clear understanding of your needs for achievement. The preparation of a timeline draws you closer to your goal and is a driving force to work hard.
- Meditation: Meditation channels a person’s energy in the right path. It aids a person to better his/her self-control, maintain focus, and connects them to their inner self.
- Everyday Routine check: a self-disciplined person set a daily routine and enlists their tasks for accomplishment. Prioritize your goals and set them up in a timeline, and fulfill them accordingly. This act betters a person’s overall personality.
- Avoid Distractions: Life is encompassed with numerous day-to-day distractions. Self-Discipline allows a person to hold charge of this/her actions. For instance, mobile phones have become an essential gadget in today’s life. However, it is a hindrance, addictive, and hamper work. Instead, read a book or meditate.
- Positivity: Many people strive to achieve self-discipline. However, they fail to meet their goal. Constant negativity and lack of positivity act as a barrier and is a wrong approach. Positivity helps an individual achieve anything and molds him/her as a reliable and confident person.
In short, Self-discipline directs a person to lead a healthy professional and personal life. A self- determined person achieves great heights through his efforts and optimum use of time.

Short Essay on Importance of Self Discipline 200 Words in English
The short essay mentioned below is for kids and children up to class 6. The essay is to help with essay assignments, comprehension, and school events.
Self-discipline is the ability of a person to do what he needs, even though he is interested not to do it. However, hard a person organizes or schedules his/her work. At times when you feel low, you battle with your self-determination. This is the reason behind uncontrolled behaviors.
Self-determination is needed at all times, whether you feel encouraged or low. When you are happy and positive, you feel inspired and apply self-determination in all your works. The skill is embedded in your subconscious memory, and you do not realize it. However, when you are experiencing a bad day, you realize your self-determination.
Self-determination is an inner power that instructs you to never give up, despite challenges and failures. It enables you to harness your temptations and distractions that come your way and helps you overcome it and attain success.
We can improve our self-discipline and better ourselves to achieving our goals. It is essential to know that improvement takes time. Self-discipline helps you grow stronger. There are ample opportunities your way, take your time and practice till you perfect yourself.
Self- discipline can never be denied in our lives. Self-discipline helps us achieve our dream by directing us in the focus we need to follow.
10 Lines about Importance of Self Discipline Essay in English
- Self-discipline is the ability of an individual to act according to his or her knowledge, experience, and consciousness. It helps him/her achieve maximum potential.
- Self-discipline is an essential aspect of an individual’s life, through his journey from school, to college to work.
- A person cannot achieve success or the desired outcomes without the application of self-discipline in life.
- Self-determination aids a person in overcoming all eating disorders, addictions, smoking and drinking problems, and al other harmful habits.
- Through self-discipline, a person nurtures his/her self with inner strength, confidence, and self-esteem. It helps him/her in many ways to achieve goals.
- To achieve self-discipline in life, one needs to set goals, stay positive, meditate for focus, avoid all distractions, and reward oneself for every tiny achievement.
- Self-discipline is present when you are motivated or when demotivated. A person fails to realize self-discipline during happy times. However, when he/she is sad, self-discipline is noticed.
- Development of self-discipline leads you to avoid acting on impulse, overcome procrastination and laziness, continue your project with focus, etc.
- The skill helps a person to strategize his/her goals. Through self-discipline, a person prioritizes all the vital tasks in their lives.
- Self-discipline is a doer that helps your achieve your dreams, and the world today needs more self-determined people who make their dreams and goals.

FAQ’s on Importance of Self Discipline Essay
Question 1. Why is self-discipline highly necessary?
Answer: Self-discipline is essential because it acts as a power that instructs you never to give up, despite failures. It is a skill that enables you to harness all the distractions that come your way and helps you overcome it to reach success.
Question 2. State a few qualities a self-disciplined person posses
Answer: A self-disciplined person stays positive, avoids distractions, keeps himself/herself focused, aims to achieve the goal, quick with work, and works hard.
Question 3. How can you maintain self-discipline?
Answer: To remain a self-disciplined person, you must identify your weakness, remove all temptations, set clear goals, have a backup plan, stay healthy, and create new and straightforward habits that improve your life.
Question 4. Is self-discipline difficult to follow?
Answer: Self- discipline is not when a person is motivated. However, when people lack motivation, they lose hope and give up. So one must take up the task of creating self-discipline to create a motivating and positive way to reach your goal.
- Picture Dictionary
- English Speech
- English Slogans
- English Letter Writing
- English Essay Writing
- English Textbook Answers
- Types of Certificates
- ICSE Solutions
- Selina ICSE Solutions
- ML Aggarwal Solutions
- HSSLive Plus One
- HSSLive Plus Two
- Kerala SSLC
- Distance Education
Self-Discipline
The importance of self-discipline for success.
Is there a link between self-discipline and success? We believe there is, and here’s why.
Many, of the high-achieving individuals we’ve studied , have stated or shown, that although numerous factors have contributed to their success, most of their achievements would be impossible without self-discipline. While passion, determination, and perseverance are all keys to success, the one thing truly required for success to happen is self-discipline.
Napoleon Hill, the great success scholar commissioned by Andrew Carnegie concluded the same thing; that the importance of self-discipline for success should not be ignored.
Look, setting goals is easy. Anyone can sit down for five minutes and create a list of goals . However, turning those goals into accomplishments doesn’t happen by itself. Bridging that gap between our goals, and the accomplishment of them can only be done with self-discipline.
When you have self-discipline, it’s easier to transform your goals into accomplishments. Understanding the link between success and self-discipline is the first step to becoming self-disciplined enough to achieve lasting success.
We Are the Product of Our Decisions and Choices
And this is why self-discipline is important; because life isn’t a level playing field. Certainly, there are factors that can both ease and inhibit our chances for success, and some people start out in life with more advantages than others. However, in the 21st century, we are largely a product of our personal choices and decisions.
First of all, no matter what cards you were dealt, you have complete control over your attitude. You also have control over how you treat other people and how you treat yourself.
Self-discipline is a choice. Depending on your upbringing and personal struggles, you may have to work harder to become self-disciplined, but the good news is, self-discipline can be learned.
The Unique Qualities of People Who Are Successful
It feels great to be successful, but behind most successful people, there are years of habits, choices, and decisions that most people never suspect of existing.
Almost without exception, successful people:
- Complete tasks high in value first
- Choose to be successful
- Understand the law of attraction
- Commit to lifelong learning
- Have a growth mindset
- Are self-disciplined
The Importance of Self-Discipline

When you learn and master self-discipline, some magical things start to happen. For example:
Self-Discipline Boosts Your Work Ethic
The great thing about success is that it builds on itself. When you experience success, it’s addicting. You automatically want more success. In this way, self-discipline increases your work ethic . The late Jim Rohn, who was a leadership expert and scholar of success, often pointed out that one discipline nearly always leads to another discipline.
You Will Have a Higher Self-Esteem
There is nothing that boosts your self-esteem more than completing a goal or creating an accomplishment. When you’re self-disciplined, you will have far more accomplishments in your life and you will grow to have higher self-esteem.
It Helps You Get Stuff Done
The key to success is getting high-value things done and self-discipline is what helps you get things done. As human beings, we’re biologically engineered to look for shortcuts because shortcuts are efficient. Unfortunately, this means that most of us have to make a concerted effort to get up every day and tackle the hard things.
Self-Discipline Creates Habits
Anytime you can put some areas of your life on autopilot, you’re freeing up time and energy to do the hard things. When you create habits, you’re building self-discipline into your life.
Habits make it easy to stay on track, and self-discipline creates habits.
Being Disciplined Helps You Focus
More than ever, we live in a world that is full of distractions. When you have self-discipline, you are more likely to stay focused on your goals. No one except Mark Zuckerberg ever became successful by being on Facebook all day, and honestly, we doubt he spends all of his time watching kitten videos and posting photos of what he had for lunch.
Self-Discipline Helps You Achieve Mastery
How do you master anything? You have to spend a lot of time practicing and doing. Experts such as Malcolm Gladwell suggest that to master something, you need to spend about 10,000 hours doing it. This can only happen if you’re self-disciplined.
You Realize Your Full Potential
Do human beings have unlimited potential? In a way we do. However, we’re limited by the number of days we have on this earth and the number of hours in the day. Keep this in mind: Uber-successful people like Oprah Winfrey , Jeff Bezos, and Elon Musk all have the same number of hours in the day as the rest of us.
However, their self-discipline is what sets them apart.
Self-Discipline Can Be Taught (and Learned)
People aren’t born with self-discipline. If we’re fortunate, we were raised in homes where self-discipline was practiced and taught. However, most of us have to find our own paths to self-discipline. The good news is that there is a specific formula for learning to be more self-disciplined.
1. Begin at the Beginning
You can become self-disciplined today by deciding to do the next thing right. However, complete self-discipline and success don’t happen overnight. Start small by setting micro-goals. Once you achieve one goal, you will be motivated to keep going with it.
2. Understand Your Triggers
Are there things that trigger you into distraction or unhealthy habits? Knowing what triggers you is key to becoming self-disciplined.
3. Remove Temptations
Most people have temptations that hold them back from getting things done. In terms of distraction, TV, the internet, social media, and pleasure reading can all be easy temptations that pull us away from what we need to be accomplishing.
Are sweet treats and fad-laden snacks keeping you from achieving your weight and fitness goals? Simply remove them from your home.
4. Explore Your Key Motivators
What motivates you? Have you ever really thought about that? Take a few minutes and write down a list of things that motivate you. It’s seldom the activity itself that is our motivator. For example, few people get excited about exercising. However, the motivator is feeling more energetic and looking better.
Another example is money . You may or may not love your work, but you’re probably motivated by having money in the bank and enjoying the satisfaction of knowing your bills are paid.
5. Create Habits and Routines From Behaviors
Start small by creating some habits that are easy to work into your life. Then, create routines and habits that are in line with your goals. For example, if you want to get more done before noon every day, try going to bed early the night before. Set an early bedtime for yourself and stick to it.
Why Self-Discipline Is Important: It Leads to Success
Are you convinced that the key to success is self-discipline? Hopefully you’ve come to realize the importance of self-discipline through this post, because that was our goal; to empower you with this life-changing insight.
Now, if you don’t have as much self-discipline as you would like, that’s no problem at all. You can start where you are right now and become more self-disciplined. All you have to do is take that first step and keep putting one foot in front of the other. In fact, here are few terrific resources you can use as stepping stones to support you on your journey:
- Books to Strengthen Your Self-Discipline
- Affirmations for Self-Discipline
Quotes to Inspire Self-Discipline
- Habits to Improve Self-Discipline
Whatever mistakes and missteps you’ve made in the past, you can always make a different choice right now, today.
Till next time,
PS – If you enjoyed this post on the importance of self-discipline for success, then you’ll love this post on the real ‘secret’ to success .
Like This Post?
STOP WAITING, START DOING. ENTER YOUR EMAIL BELOW, AND HIT GO !
WHAT DOES IT MEAN TO BE SUCCESSFUL?
7 LESSONS ON HOW TO NETWORK BETTER ON LINKEDIN FROM KEITH FERRAZZI
The STRIVE is on a mission to inspire and uplift 1 billion people by 2032. Our primary aim is to help as many people as possible believe in the uncommon thought, that they can be more than they are, do more than they've done, and achieve more prosperity than they've ever dreamed possible. Let's achieve the impossible together.
You may like

35+ INSPIRATIONAL QUOTES ON PATIENCE AND SUCCESS

75+ MOTIVATING DENZEL WASHINGTON QUOTES ABOUT SUCCESS

DO AFFIRMATIONS WORK?

TOP 100 SUCCESS AND MOTIVATIONAL BLOGS FOR 2024

50+ INSPIRATIONAL MASTER P QUOTES FOR SUCCESS

POSITIVE THINKING: THE KEY TO SUCCESS
10 WAYS TO ACHIEVE YOUR GOALS IN 2024
Setting goals is a crucial part of success. No matter what you want to achieve in life, be it in your career, relationships, or in business, identifying what you want to achieve and then making a plan to move toward that destination is one of the most important steps of all.
When you know what you want and the exact outcome you desire, you can then create a plan and take action to get there. This is why setting goals works. Extraordinary people are able to produce amazing results in life because they have a clear goal that they want to achieve in mind. They know what they want, and then they get to work on their goals, every single day.
With that being said, if you want to master yourself, achieve greater results in life, and ultimately make your dreams a reality, you’ll need to learn how to set and achieve your goals. So, here the top 10 ways to achieve your goals in 2024. Enjoy!
Top 10 Ways To Achieve Your Goals This Year

1. Always Keep Your Goals in Your Mind
One of the most common reasons why some people fail at their goals while others succeed at them, is that those who successfully achieved their goals are really adept at keeping their goals top of mind.
Of course, this is easier said than done. But, it is backed up by the one of the most well-known success phrases of all-time…“You become what you think about most of the time”. It’s a phrase that conveys the fact that your life is organized around your thoughts. Hence, your dominant thoughts will determine how you will live your life.
If you always think about having not enough money, guess what, you will not be having enough money. You will find it hard to come up with extra money and there are always more days left at the end of the money.
Your thoughts dictate your life. Tony Robbins once said, “Where you focus goes, energy flows”, thus, if you always think about your goals and focus on them, that’s what you will create in your life. So, always choose to consciously think about your goals.
This is why you need to write down your goals, review them, visualize them, and see yourself achieve them. Make a vision board for your goals if you want to.
2. Make Sure Your Goals Align With Your Inner Values
Next up on the list of top 10 ways to achieve your goals is to ensure they align with your values. Yes, you have to make sure your goals align with your inner values. You don’t want to set a goal that is not in harmony with your values.
For example, if you are someone who values security more than adventure, setting a goal like traveling alone around the world may not work for you. Even if you force yourself to do it, you will not enjoy the progress and the experience.
Here’s another example, many people set income goals. And if money isn’t their main purpose, their goals will never work. They will find it hard to come up with the drive to put themselves into action and they will find ways to sabotage their own success.
This is what happens when your goals conflict with your values. Instead, learn to set goals that align with your inner values. Set goals that make your heart sing.
Related: Goal Setting Mistakes to Avoid
3. Make Your Goals Measurable
Are your goals measurable? Most people set very general and vague goals like, “I want to become rich”, or “I want to be happy”, etc., but these goals are vague, and they are not measurable.
Let me ask you, if your goal is to live a happy life, how do you know when you have achieved it? That’s the problem. When your goal isn’t measurable, you will never know when you have reached it.
So, make your goals quantifiable. Make them measurable so that you can tell when you have reached them. Plus, when something is measurable, you can then come up with a specific action plan to achieve it.
If your goals are not measurable, you will work day and night without knowing if you have reached them.
4. Identify the Lead Measures
Lead measure is an important measure of your goals. Most people focus on their main target or the results they want, but they don’t focus on their lead measures, and this is why they fail.
Your lead measures are the measures that directly impact the results of your goals.
For instance, if your goal is to lose weight, the two main lead measures are exercise and diet. How much time do you spend to exercise each week? And do you track your diet and calorie intake?
You see, these two measures will directly impact your goal of losing weight. If you want to achieve your goal, then all you need to do is to focus on the two lead measures: exercise and diet.
And you hit your exercise and diet target, you will automatically reach your weight loss goal.
Here’s another classic example. If you want to increase your sales, what should you do? You focus on prospecting and presentation. The more prospects you present to, the higher your number of sales. Therefore, the number of prospects you approach, and sales presentation you deliver are the two lead measures you must work on.
When you achieved your lead measure goals, you will achieve your main goal, which is to increase your sales. So, focus and work on the lead measures.
5. Focus on Making Progress
Next, don’t always think about your goals and the results, when it comes to maintaining your momentum, you need to focus on making progress.
As a blogger, one of my goals is to build a huge responsive subscribers list from my blog. But if I focus on the result, the number of subscribers I get each day, I’m going to fail. Why? When I first started, my blog is new and there are no visitors and subscribers.
So, if I think about my goal of having a ton of subscribers, I will feel dejected, lose my motivation, and eventually give up on my blog. Instead, I choose to focus on making progress.
I know that if I want to grow my subscribers, I will need to publish new articles consistently. Hence, I focus on publishing content. Every time I published a new article, I celebrate and reward myself. I feel good about it and it drives me to continue publishing new content.
And so, day after day, I make progress. And slowly, the number of visitors to my blog increases, and the same goes for my number of subscribers.
Can you notice the difference? Having a goal is important, but to achieve your goal, you need to make progress. Hence, it is more important to focus on the progress than to only think about your goals and do nothing.
Let your progress motivate you and get you to your goals.

6. Work on Improving Yourself Every Day
There is no way you can achieve your goals if you don’t improve yourself. You are where you are because of what you know and what you do. If you want to get to a new place, you need to do something different, and that requires you to improve yourself.
I love to give an example of playing games. If the character in your game is at level 3 and you need to fight a level 5 enemy, you will find the enemy difficult to beat. But as you play the game, gain better experience, and level up your character, say to level 8, the same level 5 enemy will be easy to beat.
Therefore, work on improving your level. When the size of you increase, the problem will become a small problem.
It is the size of you that matters, not the size of the problem. If you think you are having a big problem right now, it is because the size of you is small. You must learn to improve yourself so that the problems become no problem for you.
Related: Motivation Journals for Self-Improvement
7. Set Goals That Are Fun and Exciting
Think about it, if something isn’t fun or exciting, will you have the motivation to achieve it? Obviously, the answer is no. But unfortunately, that’s what most people do. They set goals that are not fun or exciting to them.
You have to understand that if you want to achieve your goals, your goals must be fun and exciting so that you will want to wake up each morning and work on them. If your goals are boring and uninspiring, you will choose to continue to sleep than to wake up and chase them.
Set a goal that makes your heart sing. Be passionate about your goals and make sure you are excited when you think, talk, and work on your goals .
8. Make Your Goals Challenging
Besides making your goals fun and exciting, you must also make them challenging. Why? Because that’s the only way you can grow.
You see, Albert Einstein once said, “A ship is safe at the harbor, but that’s not why it is built for.” Your life is meant to be fun, exciting, and challenging. You want to live a remarkable life, isn’t it? Hence, make your goals challenging.
Think about it, if you are currently earning $5,000 a month, making an additional $100 isn’t going to make you jump out of your bed in the morning. What you want is to have a goal that is challenging and inspiring.
You want your goals to force you out of your comfort zone so that you can grow and become someone better, and worthy of the goals.
9. Take Baby Steps Each Day
It doesn’t matter how big your goals or how difficult they are, as long as you take baby steps and make progress each day, you will eventually get to your goals.
The key is in making progress every day. You can’t achieve your goals by thinking about them, you need to do something.
There is a saying, “If you swing the ax five times, every day, eventually the tree will fall.” Yes, no matter how big the tree, if you just swing an ax at it just five times a day, it will eventually fall.
The same principle applies to your life and your goals. As long as you take action and persist in working on your goals every day, you will eventually arrive at your destination.
Therefore, be consistent. Commit to taking at least 5 baby steps each day, and trust me, you will achieve your goals faster than you thought possible.
10. Believe in Your Goals and Trust Yourself That You Can Do It
Last up on this list of the 10 ways to achieve your goals is related to belief. You need to believe in your goals and trust yourself that you can do it. First, you must believe that your goals are possible. And second, you must trust that you can achieve them.
When you truly believe you can achieve your goals, you will do whatever it takes to reach them. Think about why people buy lottery tickets. Well, it is because they believe that they stand a chance to win, right? If you don’t believe you stand a chance to win, you will never bother buying the lottery ticket.
The same goes for your goals. When you believe that you can achieve them, you will do it with a 100% commitment rather than a half-hearted attempt.
Therefore, believe that your goals are possible and trust that you can achieve them.
There is no way you are going to achieve your goals if you all you do is sit there and do nothing. Reading this article is good because it helps you understand what you need to do to achieve the results you want, but until you implement the knowledge and take action , nothing is going to happen.
“Dream Big, Start Small, But Most Of All, Start.” – Simon Sinek –
Hence, don’t just think and daydream about your goals and the success you want. Make this year your best year ever by using these 10 ways to achieve your goals. If you need a little reminder, you can always print out or save the summarized tips for achieving your goals below:

It is true that this year has been challenging and tough, but if you keep a positive attitude , focus on your goals, and do what is necessary, you can make 2024 a life-transforming year. Use these goal achieving tips to help you.
PS – We hope you enjoyed these top 10 ways to achieve your goals, but never lose sight of this important fact: Achieving goals doesn’t just magically happen. Goal achievement requires a plan . So, if you truly want to make 2024 a life-transforming year, you’ll want to use this to make it happen.
SELF-DISCIPLINE: THE KEY TO HAPPINESS

If you want to know how discipline leads to happiness, then you’ll enjoy this article. Our research on this topic started after we came across an older, but still very relevant article that suggested the key to happiness was self-discipline.
We were struck by the article; particularly because it had brought to light a different key to happiness than we’ve been accustomed to hearing for most of our lives. The kind of secrets to happiness that we are all pretty much accustomed to hearing, you know; be more grateful, be present, get some supportive friends, have some goals to aspire to, focus on your health, or make more money , etc..
The article we read was published by the Atlantic. It was a synopsis of a study conducted in 2013 by Wilhelm Hoffman at the University of Chicago. If you are interested in digging deeper into the published research, you can do so here: Wiley Online Library .
“A Disciplined Mind Leads To Happiness, And An Undisciplined Mind Leads To Suffering.” – Dalai Lama –
Don’t Worry, Be Happy Self-Disciplined
The article spoke to us not only because it was refreshingly different from what the rest of the world typically says about acquiring happiness, but because it is something that we’ve found to be true in our own lives.
We’ve noticed through our own experiences, that when we’ve let our guard down, when we let our lack of self-control, and lack of discipline drive our life, things always seem to eventually get worse. It’s not something that happens immediately either; whenever we’ve let off the proverbial (self-discipline) pedal; it has always led to a slow process of degradation.
It typically starts with something small, like having a good habit of going to bed early morph into a bad habit of going to bed late. Having this good habit eventually turn into a bad habit, slowly leads to other good habits, like going to the gym consistently, or starting/arriving to work before schedule, in addition to other habits of our turning into bad habits all of their own. Eventually, through inertia, even our once chipper and positive attitude becomes influenced, allowing us to drift into a realm of negativity.
Unfortunately, this degradation process has led us to having less patience with friends and family, in addition to obvious signs of work motivation and productivity being impacted. Eventually, our levels of happiness and feelings of joy would take a very noticeable nose dive.
There’s no better quote to express the discipline to happiness process than the Dalai Lama’s famous quote: “A disciplined mind leads to happiness, and an undisciplined mind leads to suffering.”
Needless to say, reading the study was not only like taking a breath of fresh air, but it was also reaffirming of our own experiences and philosophy on the link between self-discipline and happiness (which always feels good).
How Discipline Leads to Happiness
Below is a great way to visualize how discipline leads to happiness. It demonstrates how the end result/happiness levels can be determined by the level of discipline applied.

Get Disciplined About Self-Discipline
We are always aiming to add value to you, our readers, so we did some serious self-reflection and research to come up with the four methods that, you can apply easily, but that will still have the biggest impact on your ability to increase your self-discipline. We intentionally left out any fluff, so you can get moving on your journey towards increased happiness.
This is going to sound like a crazy thought, but it is true. Acquiring discipline requires discipline . None of the steps that we are about to provide to you will take place without you making up your mind to take action on them.
So in essence, to get disciplined, you have to have at least a smidgen of discipline to get you moving forward on those actions. We know everyone has at least enough discipline to at a minimum, get started on these small steps towards improving our discipline.
Related: The Definition of Self-Discipline
1. Create a Compelling Reason to Be Disciplined
One of the most powerful catalysts we’ve experienced in improving our self-discipline, was in creating a compelling reason to stick to those disciplines. The best way we’ve found to do this, was to take the time to think about and outline our goals for the next 12 months.
The most important aspect of setting these goals was to ensure that they were goals that really brought excitement into our lives. We wanted to ensure they were goals that excited us, goals that if (and when) reached, would add a level of amazingness to our lives.
Needless to say, the goals you need to create should be so enticing, so exciting, that you will be compelled to take action on them.
When you do this, you will have effectively set the stage to stick to your disciplines a little bit better. Dare we say, that after you do this, you may experience (as we did) an almost magical-like tug on you, to take action on your ideas and plans (when needed) until that compelling reason/goal you set up for yourself is realized.
Check out these resources to help you create your compelling reason:
- A basic how-to outline for goal setting from Psychology Today .
- 4 steps for setting powerful goals from Success.com .
- An effective goal setting template that spans 10 years .
2. Sleep Your Way To Stronger Self-Discipline
We pride ourselves on being Spartan-like, and often force ourselves to work late into the night, instead of sleeping.

Of course, facts are facts, and apparently even Spartans have to sleep too. As such, this step should be an easy one to execute.
The next simple way you can get started on improving your self-discipline is through getting enough sleep. It sounds simple, but when we deprive ourselves of sufficient amounts of sleep, it can significantly impact our ability to focus, it can affect our mood, our judgement, and even our general sense of well-being.
On top of this, when we are not well rested, even the simplest of tasks can become difficult to accomplish. So in short, getting sufficient levels of sleep is directly linked with our ability to be self-disciplined.
Last we checked, most people crave sleep, so why not allow yourself the luxury of indulging in at least this one thing?
If you want to go into more depth on sleep deprivation and the impact it can have on your cognitive performance, here are two helpful studies to dig into: Study One & Study Two .
Use these tips to help you get more sleep.
- Start taking naps .
- Stop using a digital device one hour before falling asleep (this one is so hard, but you can do it).
- Sleep no more or no less than 8 hours.
- Have a bed-time routine.
Our next actionable step, like sleep, requires you to keep your eyes shut. However, this step takes quite a bit more effort.
3. Meditate Your Way to Self-Discipline
Our third tip to strengthen your self-discipline is to meditate . Mediation is a practice of quieting our minds. When done correctly, it can help put our minds at ease, and drown out our hyperactive thoughts. In essence, meditation is actually a practice in disciplining your attention.
Before reading further, if you find that mediation is just too ‘new-age’ a topic for you to even consider, take a look at any of these scientific reviews from the National Institute of Health , webmd.com , and PyschologyToday.com to help you become a believer.
Once done, come on back and I’ll share with you the powerful benefits that mediation can provide to help you improve your self-discipline.
Self-Discipline Benefit 1
The first benefit, is that your mind will gradually become less noisy, allowing for improved focus and clarity. With an improvement in these two areas, you will have a higher tendency to pay attention to the things in your life that really matter.
So, remove the mental distractions from your life. The more the merrier. And by doing this, you will get more done. And this will in turn, contribute greatly to your ability to become more self-disciplined.
Self-Discipline Benefit 2
The second benefit is that through the practice of meditation itself, you will be simultaneously improving your mental self-discipline. We say this, because meditation is a practice, and it requires you to make and take the time to do it. The great thing is, when you make time to do something as simple as this, on a consistent basis, you are in effect training your ‘self-discipline muscles’.
Self-discipline, like a muscle, can become stronger the more you use it. Similar to how we mentioned earlier, that being too casual with our self-disciplines can create a downward spiraling effect in our lives (where all other disciplines start to be negatively affected), the same cascading process can occur, but in the opposite direction when the smallest of disciplines (such as mediation) are practiced.
When you start your sessions they don’t have to take up much of your time either. A quality session can take anywhere from 10 minutes to 20 minutes. Of course, the duration is up to you.
Lastly, if you start this habit, there is a good chance you will also experience other great life enhancing benefits. For instance, people who regularly meditate, have reduced levels of negative emotions, reduced levels of stress, improved immune responses, and an increase in overall mental and physical health. Gaim.com has a terrific beginner’s guide to meditation , so if you are really curious about the ins and outs of this practice, we recommend checking it out.
4. Read Your Way to Self-Discipline
This last step is simple, but powerful. So don’t let it’s simplicity mislead you. So here it is… reading. That’s right, you can read your way to improved self-discipline. Here’s how.

You see, for almost any area in our lives that we want to improve we must first become students of that subject. And as students we must be open to learning as much about those subjects we wish to master. And in this case, you want to master self-discipline.
As such, you should strive to get your hands on as many self-discipline books as you can. Then become a student of those books. Devour them, pick them apart, and put the self-discipline wisdom you find in each book to work for you.
Like we said, simple….but powerful!
If you’re looking for a good place to start, give this list of popular books on discipline a shot.
Self-discipline can Lead to Happiness
One of our favorite mentor’s once stated that the key to getting all we want in life is through self-discipline. He stressed that for every disciplined effort, there are multiple rewards.
We’ve taken this advice to mean, that every discipline affects all other disciplines. When we show discipline, even in the slightest thing, like waking up early, or eating less food, we build our ‘discipline muscles’. These muscles, or rather, habits, start to carry over into other disciplines.
Before we know it, we find ourselves making our bed every morning, making it to meetings on time, actually finishing personal/professional projects we’ve been meaning to wrap up, doing more to help around the house, exercising more , etc., the list will go on and on.
Here’s a shocker, self-disciplined are happier because they eventually get their lives in order.
Related: The Link Between Self-Control and Success
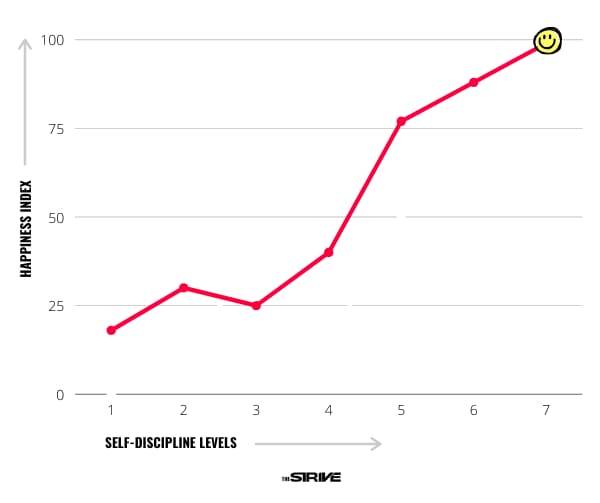
Final Thoughts
The great news is this, you can start working on your increased happiness today . You have a starting point. The four steps we’ve included are not the end-all-be-all of habits to hone to improve your self-discipline. These four steps are simply an ideal place to kick off your new journey towards becoming more self-disciplined.
We’ve given you these bite-sized steps to improve your discipline for a reason. Our hope is that they will increase the likelihood that you will actually start following some of these steps. The goal is that you find it easy to begin your new self-discipline project.
Put these four simple disciplines into action, and you’ll be effortlessly doing the bigger disciplines in no time at all. Employ the disciplines that truly lead to significant life change, and consequently, significant happiness.
Thus, our last and final takeaway for you is this, that people with high self-discipline are happier than those without. Self-discipline can be your key to happiness .
So, if you are seeking ways to become happier, and if you are open to improving just about every aspect of your life in the process, it appears that there is no faster way to do both, than through the practice of self-discipline.
Till you reach your aims,
PS – Self-discipline is the key to happiness, and we have the key to self-discipline. So, if you want to be more self-disciplined then you may want to take a look at this tool.
100+ SELF-DISCIPLINE QUOTES TO HELP YOU ACHIEVE UNLIMITED SUCCESS

Self-discipline is one of the world’s best kept secrets when it comes to success. Countless people who have accomplished many of their goals or have achieved meaningful success across a variety of different areas typically give credit to their self-discipline when asked, ‘how did they do it?’ As such, we’ve decided to pull together some of the absolute best self-discipline quotes of all-time.
“Discipline Is The Bridge Between Goals And Accomplishment.”
Our hope is that these discipline quotes will permeate your mind with one of the best kept secrets of some of the world’s highest achievers. We also hope that they’ll inspire you to believe, that with enough self-discipline, you too can achieve the impossible. So, if you’re ready for one of the most comprehensive lists of self-discipline quotes, then let’s dive in:
BEST 100+ SELF-DISCIPLINE QUOTES

1. “The great master key to riches is nothing more or less than the self-discipline necessary to help you take full and complete possession of your own mind.” – Napoleon Hill
2. “With self-discipline, most anything is possible.” – Theodore Roosevelt
3. “We do today what they won’t, so tomorrow we can accomplish what they can’t.” – Dwayne ‘The Rock’ Johnson
4. “Winners embrace hard work. They love the discipline of it, the trade-off they’re making to win. Losers, on the other hand, see it as a punishment. And that’s the difference.” – Lou Holtz
5. “A disciplined mind leads to happiness, and an undisciplined mind leads to suffering.” – Dalai Lama
6. “Discipline is the soul of an army. It makes small numbers formidable; procures success to the weak, and esteem to all.” – George Washington
7. “The successful person has the habit of doing the things failures don’t like to do. They don’t like doing them either necessarily. But their disliking is subordinated to the strength of their purpose.” – E.M. Gray
8. “The only discipline that lasts is self-discipline.” – Bum Philips
9. “Success is a result of daily disciplines compounded over time.” – Darren Hardy
10. “Discipline is the bridge between goals and accomplishment.” – Jim Rohn

11. “There is no easy way. There is only hard work, late nights, early mornings, practice, rehearsal, repetition, study, sweat, blood, toil, frustration, and discipline.” – Jocko Willink
12. “We must all suffer one of two things: the pain of discipline or the pain of regret and disappointment.” – Jim Rohn
13. “I could only achieve success in my life through self-discipline, and I applied it until my wish and my will became one.” – Nikola Tesla
14. “Self-command is the main discipline.” – Ralph Waldo Emerson
15. “Without self-discipline, success is impossible, period.” – Lou Holtz
16. “One discipline always leads to another discipline.” – Jim Rohn
17. “He who lives without discipline dies without honor.” Icelandic Proverb
18. “The price of excellence is discipline. The cost of mediocrity is disappointment.” – William Arthur Ward
19. “You have power over your mind, not outside events. Realize this, and you will find strength.” – Marcus Aurelius
20. “Discipline is choosing between what you want now and what you want most.” – Abraham Lincoln

21. “Confidence comes from discipline and training.” – Robert Kiyosaki
22. “Success is a matter of understanding and religiouly practicing specific simple habits that always lead to success.” – Robert J. Ringer
23. “No man is fit to command another that cannot command himself.” – William Penn
24. “Most talk about ‘super-geniuses’ is nonsense. I have found that when ‘stars’ drop out, successors are usually at hand to fill their places, and the successors are merely men who have learned by application and self-discipline to get full production from an average, normal brain.”- Charles M. Schwab
25. “Success doesn’t just happen. You have to be intentional about it, and that takes discipline.” – John C. Maxwell
26. “Discipline is the foundation of a successful and happy life.” – Anonymous
27. “True freedom is impossible without a mind made free by discipline.” – Mortimer J. Adler
28. “Self-control is the chief element in self-respect, and self-respect is the chief element in courage.” – Thucydides
29. “You will never have a greater or lesser dominion than that over yourself…the height of a man’s success is gauged by his self-mastery; the depth of his failure by his self-abandonment. …And this law is the expression of eternal justice. He who cannot establish dominion over himself will have no dominion over others.” – Leonardo da Vinci
30. “The first and greatest victory is to conquer self.” – Plato

31. “We must do our work for its own sake, not for fortune or attention or applause.” – Steven Pressfield
32. “One painful duty fulfilled makes the next plainer and easier.” – Hellen Keller
33. “Self-respect is the fruit of discipline; the sense of dignity grows with the ability to say no to oneself.” – Abraham J. Heschel
34. “Do not consider painful what is good for you.” – Euripides
35. “Success is nothing more than a few simple disciplines, practiced every day.” – Jim Rohn
36. “Those who have nothing have only their discipline.” – Alain Badiou
37. “It is time to reverse this prejudice against conscious effort and to see the powers we gain through practice and discipline as eminently inspiring and even miraculous.” – Robert Greene
38. “With this magic ingredient, you can accomplish anything and everything you want to, and it is called self-discipline.” – Brian Tracy
39. “Do not bite at the bait of pleasure till you know there is no hook beneath it.” – Thomas Jefferson
40. “Great leaders always have self-discipline — without exception.” – John C. Maxwell

41. “Mental toughness is many things and rather difficult to explain. Its qualities are sacrifice and self-denial. Also, most importantly, it is combined with a perfectly disciplined will that refuses to give in. It’s a state of mind-you could call it character in action.” – Vince Lombardi
42. “Respect your efforts, respect yourself. Self-respect leads to self-discipline. When you have both firmly under your belt, that’s real power.” – Clint Eastwood
43. “Success is actually a short race – a sprint fueled by discipline just long enough for habit to kick in and take over.” – Gary Keller
44. “By constant self-discipline and self-control you can develop greatness of character.” – Grenville Kleiser
45. “Most powerful is he who has himself in his own power.” – Seneca
46. “He who cannot obey himself will be commanded. That is the nature of living creatures.” – Friedrich Nietzsche
47. “It is not enough to have great qualities; We should also have the management of them.” – La Rochefoucauld
48. “Discipline really means our ability to get ourselves to do things when we don’t want to.” – Arden Mahlberg
49. “Your level of success is determined by your level of discipline and perseverance.” – Anonymous
50. “That aim in life is highest which requires the highest and finest discipline.” – Henry David Thoreau

Ready To Go Out and Conquer The World Yet?
We don’t know about you, but after reading through these first 50 discipline quotes, we are about ready to go out and conquer the world. But don’t stop reading just yet on our account.
By all means, continue pounding your mind with these last 50 self-discipline quotes. Let them saturate your mind so you can go forth and be victorious with your renewed levels of self-discipline !
51. “Self-discipline is about controlling your desires and impulses while staying focused on what needs to get done to achieve your goal.” – Adam Sicinski
52. “Discipline yourself to do the things you need to do when you need to do them, and the day will come when you will be able to do the things you want to do when you want to do them.” – Zig Ziglar
53. “All successes begin with self-discipline. It starts with you.” – Dwayne “The Rock” Johnson
54. “Self-discipline is that which, next to virtue, truly and essentially raises one man above another.” – Joseph Addison
55. “The more disciplined you become, the easier life gets.” – Steve Pavlina
56. “The center of bringing any dream into fruition, is self-discipline.” – Will Smith
57. “Self-discipline is the ability to make yourself do what you should do, when you should do it, whether you feel like it or not.” – Elbert Hubbard
58. “In reading the lives of great men, I found that the first victory they won was over themselves…self-discipline with all of them came first.” – Harry S. Truman
59. “If it were easy to walk the path of self-discipline, we wouldn’t gain much from it.” – Glenn C. Stewart
60. “Discipline is built by consistently performing small acts of courage.” – Robin Sharma

61. “Discipline is the ability to control our conduct by principle rather than by social pressure.” – Glenn C. Stewart
62. “Self-respect is the fruit of discipline; the sense of dignity grows with the ability to say no to oneself.” – Abraham J. Heschel
63. “We all have dreams. But in order to make dreams come into reality, it takes an awful lot of determination, dedication, self-discipline, and effort.” – Jesse Owens
64. “Discipline is the silent force at work that breeds success. It requires only one thing; that you sacrifice time in things you enjoy.” – Anonymous
65. “We don’t have to be smarter than the rest; we have to be more disciplined than the rest.” – Warren Buffett
66. “Never believe a promise from a man or woman who has no discipline. They have broken a thousand promises to themselves, and they break their promise for you.” – Matthew Kelly
67. “If the self-discipline of the free cannot match the iron discipline of the mailed fist-in economic, political, scientific and all other kinds of struggles as well as the military-then the peril to freedom will continue to rise.” – John F. Kennedy
68. “Self-discipline is the root quality that will improve every aspect of your life.” – Jocko Willink
69. “Success is measured by your discipline and inner peace.” – Mike Ditka
70. “ Self-control is strength, right thought is mastery, calmness is power.” – James Allen

71. “Motivation gets you going, but discipline keeps you growing.” – John C. Maxwell
72. “Discipline without freedom is tyranny. Freedom without discipline is chaos.” – Cullen Hightower
73. “By constant self-discipline and self-control you can develop greatness of character.” – Grenville Kleiser
74. “Self-discipline is a self-enlarging process.” – M. Scott Peck
75. “Self control is the key to self esteem and self confidence.” – Laurance McGraw V
76. “Not being able to govern events, I govern myself.” – Michel De Montaigne
77. “Small disciplines repeated with consistency every day lead to great achievements gained slowly over time.” – John C. Maxwell
78. “Talent without discipline is like an octopus on roller skates.” – H. Jackson Brown, Jr.
79. “If you wish to be out front, then act as if you were behind.” – Lao Tzu
80. “Self-discipline creates a brighter tomorrow.” – Anonymous

81. “Success is created through the performance of a few small daily disciplines that stack up over time to produce achievements far beyond anything you could of ever planned for. Failure, on the other hand, is just as easy to slip into. Failure’s is nothing more than the inevitable outcome of a few small acts of daily neglect performed consistently over time so that they take you past the point of no return.” – Robin Sharma
82. “Self-discipline is an act of cultivation. It requires you to connect today’s actions to tomorrow’s results. There’s a season for sowing a season for reaping . Self-discipline helps you know which is which.” – Gary Ryan Blair
83. “ Self-discipline begins with the mastery of thought. If you do not control your thoughts, you cannot control your needs. Self-discipline calls for a balancing of the emotions of your heart with the reasoning faculty of your head.” – Napoleon Hill
84. “Trophies should go to the winners. Self-esteem does not lead to success in life. Self-discipline and self-control do, and sports can help teach those.” – Roy Baumeister
85. “It’s all right letting yourself go, as long as you can get yourself back.” – Mick Jagger
86. “The individual who wants to reach the top in business must appreciate the might and force of habit. He must be quick to break those habits that can break him—and hasten to adopt those practices that will become the habits that help him achieve the success he desires.” – J. Paul Getty
87. “It is better to conquer self than to win a thousand battles.” – Buddha
88. “The good Lord gave you a body that can stand most anything. It’s your mind you have to convince.” – Vince Lombardi
89. “Talent without discipline is like an octopus on roller skates.” – H. Jackson Brown, Jr.
90. “If we don’t discipline ourselves, the world will do it for us.” – William Feather

91. “When a man is sufficiently motivated, discipline will take care of itself.” – Albert Einstein
92. “No life ever grows great until it is focused, dedicated, disciplined.” – Harry Emerson Fosdick
93. “It’s never crowded along the extra mile.” – Wayne Dyer
94. “I think self-discipline is something, it’s like a muscle. The more you exercise it, the stronger it gets.” Daniel Goldstein
95. “Self-discipline is the magic power that makes you virtually unstoppable.” – Dan Kennedy
96. “He conquers twice who conquers himself in victory.” – Jyrus
97. “It doesn’t matter whether you are pursuing success in business, sports, the arts, or life in general: The bridge between wishing and accomplishing is discipline.” – Harvey Mackay
98. “I don’t count my sit-ups, I only start counting when it starts hurting, when I feel pain, that’s when I start counting, cause that’s when it really counts.” – Muhammad Ali
99. “What it lies in our power to do, it lies in our power not do.” – Aristotle
100. “Mastering others is strength. Mastering yourself is true power.” – Lao Tzu

101. “I count him braver who overcomes his desires than him who conquers his enemies; for the hardest victory is over self.” – Aristotle
102. “Rule your mind or it will rule you.” – Horace
103 . “Self-discipline is the center of all material success. You can’t win the war against the world if you can’t win the war against your own mind.” – Will Smith
104. “In this life there are countless trails to self-realization, though most demand intense discipline, so very few take them.” – David Goggins
105. “If I want to be great I have to win the victory over myself…self-discipline.” – Harry S. Truman
106. “What we do upon some great occasion will probably depend on what we already are: and what we are will be the result of previous years of self-discipline.” – H.P. Liddon
107. “The pain of discipline weighs ounces, but the pain of regret weighs tons.” – Darren Hardy
108. “Discipline is the refining fire by which talent becomes ability.” – Roy L. Smith
109. “Self-discipline is when your conscience tells you to do something and you don’t talk back.” – W.K. Hope
110. “Discipline is doing what you hate to do, but nonetheless doing it like you love it.” – Mike Tyson

111. “There is no magic wand that can resolve our problems. The solution rests with our work and discipline.” – Jose Eduardo Dos Santos
112. “There is no luck except where there is discipline.” – Irish Proverb
113. “Discipline is consistency of action.” – James C. Collins
114. “Discipline is wisdom and vice versa.” – M. Scott Peck
115. “Self-discipline is the No.1 delineating factor between the rich, the middle class, and the poor.” – Robert Kiyosaki
116. “Self-Discipline means living your life the hard way: resisting temptations and instant gratification, in order to receive bigger and better rewards in the future.” – Martin Meadows
117. “The obstacle in the path becomes the path. Never forget, within every obstacle is an opportunity to improve our condition.” – Ryan Holiday
118. “Self-discipline is easy when you have a vision that pulls you.” – Nathan Lee Morales
119. “There are two disciplines in life. There is the pain of discipline and the pain of disappointment. If you can handle the pain of discipline, then you’ll never have to deal with the pain of disappointment.” – Nick Saban
120. “Self-discipline is the architect of accomplishment.” – The STRIVE

121. “The first step to getting rich requires discipline. If you really want to be rich, you need to find the discipline.” – Mark Cuban
122. “The habit of self-discipline virtually guarantees your success in life.” – Brian Tracy
Bonus Discipline Quote
Bonus: Alright, here is our last and final discipline quote which we decided to include as a bonus because it does such a good job hitting the nail on the head when it comes to self-discipline. Enjoy!
“Discipline Equals Freedom.” – Jocko Willink –
There you have it, some of the best discipline quotes of all time. We hope these quotes serve you in creating the habit of self-discipline. Let them guide you towards becoming your very best so you can achieve the success you’re striving for.
PS – If you enjoyed this page and its self-discipline quotes, please consider helping us reach our goal if inspiring and uplifting a billion people by sharing our page or one of these discipline quotes with your inner circle. Lastly, i f you enjoyed these quotes, we have a hunch you’ll love these Quotes on Effort , and you may even enjoy these Affirmations For Discipline .
15+ BEST BOOKS TO BUILD SELF-DISCIPLINE AND MASTER SELF-CONTROL (2024)
Ahhh, self-discipline, that pain-in-the-butt success attribute that most of us wish were easier to wield. If I told you there was a pill you could take to increase your self-discipline, would you want one?
Hahaha, so would I.
Unfortunately, there is no pill.
But, I do have something for you that is far better than some easy peasy pill. In fact, I have 15 or so of them for you.
And I am confident you could benefit from them.
How can I be so sure?
Statistics. Statistically speaking, 92% of people who set goals at the beginning of each year, don’t achieve them (University of Scranton.) That stat alone, says so much about the state of our collective self-discipline.
“92 % of people who set goals at the beginning of each year, don’t achieve them.” – University of Scranton
It reveals that most people can’t stick to a simple goal they set out to achieve.
How is it that so many people fail to achieve what they really want?
I mean, nobody sets a goal they don’t think they can achieve.
Nobody sets a goal around something they don’t sincerely want either.
Yet, so many still fail to reach the simple goals they set for themselves, year after year.
And what about the big goals? Let’s not even go there.
Here’s the most likely culprit. When the results we go after don’t come fast enough, and we realize what we’re chasing seems like more of a hassle than we first imagined, we second-guess ourselves. And as we continue to pursue our goals, we slowly begin making up our minds that the pain of consistent self-discipline is a cost we aren’t willing to pay. The pain bests us.
So, what do we do?
We stop striving for our goal.
If that scenario sounds familiar, then you’ve had your own struggles with self-discipline. In short, self-discipline is likely hard for you.
But, you don’t have to feel too bad about it (just a little bad), because you are not alone. Self-discipline is painful for just about everyone. But just because it’s painful, doesn’t mean we shouldn’t strive to find more of it.
Truth is, self-discipline is a pain that is good for you. It’s so good for you that it really shouldn’t be seen as pain at all.
Like Euripides said…. “Do not consider painful what is good for you.”
NO PAIN NO GAIN
My friend, self-discipline is a worthy characteristic to improve. It’s worthy because it has the power to lead you from where you are now, to where you want to be, faster than any other human quality.
Self-discipline is a force to be reckoned with. When it is strong, it will keep you moving forward, progressing towards your goals till you hit them.
On the flip side, self-discipline is also something everyone struggles with at some point in their lives. And when it’s weak your achievements will be meek.
So go big, keep going for those big goals, but make sure your self-discipline is strong before you do so.
Why? Because trying to achieve a goal without self-discipline, is like trying to ride a bicycle across a hilly countryside and expecting to get up the harder, steeper hills without peddling.
It’s just not going to happen. Which is why goal achievement without self-discipline is impossible.
Fortunately, you can build and craft your self-discipline to your liking. And you can do it in a short amount of time.
The more you build it, the more and more achievements you’re likely to see in your life.
And I have just the thing to help you begin building your self-discipline.
Here are 14 self-discipline books you should read to help you fortify your self-discipline.
You’ll strengthen your discipline just by reading them, because it takes discipline to read books.
But, you’ll also gain powerful self-discipline mindset insights, insights that will help you become the master over your very own.
So here you go my friends, a handful of stepping stones to higher and better levels of self-discipline.
BEST BOOKS ON DISCIPLINE

Note: We’re reader-supported. When you buy through links on our site, we may earn an affiliate commission.
1. The Compound Effect
‘ The Compound Effect’ is like a manifesto for self-discipline. The author of this book is Darren Hardy, who is the former publisher of SUCCESS Magazine, a serial entrepreneur, mutli-millionaire, and the author of a few other books. And you know what? This guy knows a thing or two about success and self-discipline.
Darren sums it up well in his book when he gives the formula for how to create radical change in our lives. The formula is this: “Small smart choices + Consistency + Time = RADICAL DIFFERENCE”
Small smart choices come down to small daily self-disciplines.
This book is worth the read because it will help you realize that it is the small everyday choices you make, not the big disciplines, that determine the size of your achievements.
After reading this, self-discipline will seem less daunting, more manageable, and perhaps even a bit attractive. Get this book, and let Darren sell you on the power of self-discipline and it can do to transform the outcome of your life.

‘ Mastery ’ is a masterpiece. This book was authored by Robert Greene, and it covers a wide spectrum of ideas that coalesces around what it takes to become a master. A master of your craft, your profession, a master of your life.
Much of the material in the book is pulled from the author’s vast knowledge of historical and modern masters to help you realize what it takes to become a master, the likes of Mozart, Leonardo Da Vinci, Goethe, John Coltrane, Marcel Proust, and many others.
He demonstrates that Mastery is a simple process that is accessible to anyone who is willing to put in the time, effort, dedication and sacrifice to create masterful work.
His reference to Leonardo Da Vinci’s motto, Ostinato Rigore , meaning stubborn rigor sums up what kind of self-discipline is required to achieve your life’s task (your purpose).
To strengthen your self-discipline and learn what it takes to become the master of your fate, this is definitely book you should digest.

3. The Willpower Instinct
‘ The Willpower Instinct ‘ approaches self-discipline and self-control from a more academic stand point. It’s a good self discipline book, but if I am honest, it’s quite boring to read.
If you are true student of self-discipline and self-control though, it will be worth it.
It’s worth your time because it will help you gain clarity on why self-discipline seems so challenging to master for so many people. The clarity gained from this book can lead to better decisions, and better decisions always leads to better results.

4. The Master Key to Riches
This book is a powerful book for building self-discpline. Every chapter provides insight upon insight on the habits and types of efforts that are required for you to achieve more in life.
The most important chapter though, is chapter 12, because it deals solely with self-discipline. Chapter 12 makes a strong case for why you should work on becoming self-disciplined, especially if wealth, success, and riches are things you are striving for.
And let’s be honest, money, success, and power are things we’re all striving for. So give this one a read, and learn why self-discipline is the master key to riches . Then put what you learn to use, and build the rich and abundant life you deserve for yourself.

5. The War of Art
In my opinion, out of all of the best books on discipline, this one is the best. However, this book is listed and #5 because it was primarily written for creative types who know the self-sabotaging challenges that come with trying to create great work consistently.
Even if you are not an artist, author, or entrepreneur, this book will help you realize the struggle to create is real, but that it can be conquered.
I believe this book is for everyone because we are all creators, creators and designers of our own lives.
Now the author doesn’t call out self-discipline directly through the book, rather, he positions it as “Resistance”. But, through his concept of “Resistance” clearly communicates how you must commit to your work, to becoming a pro, and how when you do, you’ll be applying the self-discipline you’ve needed to do what you’ve always wanted.
It’s a good kick in the pants that will help you deal with your self-discipline challenges in an effective way. So give it read .

6. The Practicing Mind
If you are looking for a new perspective on how to build your self-discipline, then this book is for you. Thomas M. Sterner makes a strong case for the importance mindset plays on how self-disciplined we are. He does a good job relating his personal experiences with mastering golf, piano lessons, and book writing, using the practicing mind process.
You’ll learn that with the right awareness and mindset, you can better master just about anything. His biggest urging is to learn to love the process of whatever it is you are seeking to accomplish, to do so, is to develop a practicing mind.
And when you’ve developed a practicing mind, the self-discipline and focus we all struggle with, becomes easier to wield.
A slow read, but it has some gems in it for sure.

7. Willpower: Rediscovering The Greatest Human Strength
Roy Baumeister is highly admired psychologists who teamed up with the renowned New York Times science writer, John Tierney, to create what is in a sense a self-control manifesto . Both authors do a great job of taking their vast knowledge of people and human psychology, to effectively sum up the power of willpower.
They give great examples of how we can refuel our willpower, and create effective habits that can actually make it easier for us to control ourselves. In short, you’ll learn the science behind self-control and many new and unique methods to help you master yours.
All in all, it’s a great book to read and an excellent building block to help you level up your self-discipline.

8. Think and Grow Rich
This book belongs in almost every self-improvement category, but it really shines when it comes to self-discipline.
When you read this book, you’ll gain a new awareness to success, gaining riches, and all that other achievement jazz. But most importantly, it will drill the point home, that no success, no great riches, no high achievements can be made if you have not mastered your thoughts.
And sure enough, the mastery of your thoughts comes down to your ability to discipline your mind on how to think, what to allow into your mind, and what kind of thoughts you should consistently be focusing on to achieve your goals.
This book is a must-read for the true seeker of success and self-discipline.

9. No Excuses: The Power of Self-Discipline
Brian Tracy has been around for a very long time, but his book on discipline, ‘ No Excuses ’ is still a great starting place if you are ambitious, just finishing up your schooling, or about to get started in the working world.
He’s a pretty much a ‘self-development guru’, since he’s been at this for so long. He covers many success maxims you’ve probably already heard, but he does a good job of tying them all together around the subject of self-discipline.
Reading this book will help you realize the value self-discipline plays in just about every area of our life.

10. The Power of Habit
Charles Duhigg does a great job illuminating the complexity of the science behind our habits and breaking it down into digestible insights.
You’ll learn that the bulk of what we does is governed by our habits, and how with a little bit of disciplined awareness, you can master the art of turning bad habits into good ones.
So, if you are have some bad habits you need to change, or some new habits you need to create, and want to ensure you have the discipline to see them through, get this book , it is the ultimate cheat sheet for mastering your habits.

11. The Warrior Ethos
This book not your typical book on discipline. It’s about an approach to life, it’s about an ethos.
It’s about an ethos that has become less and less apart of modern-day culture, yet, is the exact ethos most fit to help you embrace the struggles and toil of your every aspiration.
The tenets of the Warrior Ethos, directed inward, can inspire you to fight against and conquer the enemies that can be found within our own hearts and minds.
I highly recommend this book. It’s not a book 100% dedicated to self-discipline, so don’t expect a bunch of science and data. But, you can expect to be inspired and fired up to gain the discipline of a Spartan.
Read this book and gain the mental toughness you’ll need, if you want to have the self-discipline of a champion.

12. Self-Discipline
Coming in at number 12 on our list of books for building self-discipline is aptly named… ‘Self-Discipline’. This is a newer self-discipline book, but it deserves mentioning as it is jam packed with powerful principles that can help you build the mental toughness and tightened mental focus that lead to achievement. It is truly a simple and easy read, and gets right to the point on what self-discipline is and how anyone can get more of it.
Out of all of our best books on self-discipline, this book has been listed because it does a phenomenal job helping the reader learn that self-discipline is more than just a skillset, it is a lifestyle. And in my opinion, once you’ve accepted this fact and truly understand it… your ability to become the master of yourself and by extension, your fate will be transformed .

13. Make Your Bed
Make Your Bed is by far one of the more popular books on self-discipline and life improvement in general. It’s has garnered the prestigious title of a NY Times Best Seller, which we believe is a well deserved title. The author of Make Your Bed is Admiral William H. McRaven. And he wrote this book after giving a commencement speech that went viral. The message he conveyed it that commencement speech, and what he lays forth in this book, is about how the little things make a big difference in how our life turns out.
It’s is certainly not an academic book as it contains various short stories and anecdotes for life. However, it is a book that will at the very least inspire you to do the little things a little bit better and a little more consistently. And this will ultimately help you change your life. After all, that’s what self-discipline is all about, isn’t it? Consistently doing the little things.

14. The Science of Self-Discipline
Best-selling author and human psychology researcher Peter Hollins has created a one-of-a-kind resource with his book The Science of Self-Discipline. As someone who has studied high performance individuals for over a decade, Hollins really nails the psychology and science behind behind self-discipline in this book.
His book provides an 11 chapter road map that will help you understand everything from how your biology, habits, mindset, and environment can and will impact your discipline levels. As such, this discipline book comes highly recommended and should be added to your reading list as well, if you have yet to read it .

15. The Marshmallow Test
Walter Mischel is one of the world’s leading experts on self-control. His groundbreaking work on self-control (a.k.a. the famous marshmallow test) has helped him get cited more than any other psychologist when it comes to self-control, as he’s shown better than anybody else, the direct link that exists between delayed gratification and one’s ability to create a successful life for themselves.
With that said, this is a great book to study if you’re looking to master self-discipline and self-control, as Mischel provides countless antidotes and strategies that just about anyone can implement to gain mastery of both .

16. The Power of Self-Discipline
In 2021 Peter Hollins published The Power of Self-Discipline . And while it’s not one of the most popular books on discipline, it is one of the most effective.
Why? Because it helps you get right to the heart of what deteriorates discipline, and it provides tangible methods to overcome those things. In fact, The Power of Self-Discipline is one of the few books that actually gives you small exercises that you can use to slowly and methodically build your self-discipline, habits, and self-control.
So if you’re looking for effective tools to reshape how well you can stay focused, disciplined, and get more more done with less effort, then this book is for you.

Bonus Self-Discipline Book: Discipline Equals Freedom
Sometimes, what we all really need to get the discipline we want is the cold hard truth. And that is exactly what Jocko Willink lays down for us in his book Discipline Equals Freedom . Hands down this is one of the best books on discipline.
This book is a must have for every discipline seeking individual, because Jocko speaks truth. No doubt, you may find what he has to say abrasive, maybe even a bit too straight-forward. But if you are truly seeking discipline, then you should be okay with his methods. Why? Because the ends justify the means.
This is a self-help book we all need to read in this day and age. And at the moment out of all of these books on discipline, this one is currently my favorite. It’s a book that will help you discipline your thoughts, which will then help you discipline your actions. So, if you’re ready to learn the simple truths about self-discipline, truths that will lead to disciplined action, then this book is for you .

“With self-discipline, most anything is possible.” – Theodore Roosevelt
GO FORTH AND BUILD YOUR SELF-DISCIPLINE
There you have it friends, the 15 best books on self-discipline that can help you improve your self-discipline and self-control. But don’t just let your learning lead to knowledge, let your learning lead to action. And for some bonus methods to discipline your thoughts, be sure to check out these highly effective discipline affirmations , and our highly popular discipline quotes .
Remember, all successful people are highly disciplined people. All unsuccessful people are usually un disciplined and unable to control their actions and appetites.
So, read these self discipline books, leverage your resources, and put what you learn into action, so when they talk about the 8% of people who follow through on their goals, they’ll be talking about you.
PS – These are the best books on discipline, no doubt about it! But if you’re looking for something to truly help you BE self-disciplined NOW, self-disciplined enough to actually achieve the big harry audacious goals you’ve set for yourself, then this is for you .
THE ONE THING EVERY AMBITIOUS PERSON NEEDS: A MOTIVATION JOURNAL

If you’re seeking out motivational journals then this article is for you. We provide the reasons every person needs a motivation journal, along with a few of the top journals to use. However, before we reveal everything, here is what you need to know about motivation.
Every obstacle seems to move aside for the person who is truly motivated. For the truly ambitious and highly motivated, just about every goal is conquerable.
Yet, motivation can also be extremely elusive, even for the most ambitious among us.
“Ambition Without The Motivation to Act, is Called Day-Dreaming.”
Truth is, there are times when motivation seems to avoid even the best of us, appearing as something slippery, difficult to grasp, and hard to maintain. Unfortunately, when our motivation eludes us, we can feel trapped in a vicious cycle of procrastination and idleness.
But you know what? It doesn’t have to be this way. Motivation and goal achievement don’t have to be such a challenge for us. In fact, you can kill your procrastination woes forever and it’s simpler than you think.
If you consider yourself ambitious, or you’d like to… and the idea of “staying motivated” 24/7/365 interests you, then keep reading.
The Truth About Motivation and Achievement
They say motivation is the driving force by which humans achieve their goals. But oddly, way too many people struggle these days to find the motivation needed to reach their aims.
Why do they struggle? They struggle because they sit around and wait for motivation to come to them. If they’re not feeling “motivated”, they don’t act.
Sure, they act to get started on a big goal or dream when it’s new and the passion to achieve it is red hot. But, most people stop taking action on their goals when the fire and newness surrounding them fizzles out.
When most people have a bad day, or a day where they feel less than inspired to take action on their goals, they tend to not do much towards accomplishing them.
They let themselves get distracted or decide to consciously do everything except what they originally committed themselves to doing.

No doubt this is a problem, and it’s one we’ve all faced before. Unfortunately, less motivation leads to less action, and less action leads to less achievement.
But, there is a solution! And believe it or not, is this….
Believe it or not, ritual is the little known secret that most accomplished achievers in the world use to motivate themselves.
Study any high performer closely and you’ll notice they don’t depend on motivation to strike before they get their work done.
Nope, they do the work they set out to do, motivated or not. Why? Because they’ve ritualized the process of motivation. Some create early morning routines , and others late night rituals . But it really doesn’t matter what time of day it occurs, so longs as they have a ritual to move their needle forward.
You see, what high achievers have figured out, is that goal accomplishment is easier to come by when habits have been created that force them to take action daily.
High achievers know that motivation never lasts, and so they find a way to ritualize their motivation.
And can you guess what one of the best ways to ritualize motivation is?
Use a Motivation Journal
If you guessed journaling, you’re right. Every ambitious person needs a motivation journal to help them create a ritual that motivates.
Create a ritual that motivates, and you’ll end up conquering goals like you never thought you could. Why?
Because when you discover a way to improve your motivation simultaneously increase your chances of taking more action. And more action leads to better results and more achievement.

So if you can get in the habit of using a journal, you may just end up conquering goals like some of the greats.
In fact, here are a some of those great people who have used the ritual of journaling to propel themselves to achieve some pretty extraordinary things.
Notable Journal Users
Check them out:
- The well-known productivity expert, author, and entrepreneur, Tim Ferriss is known to have a daily journaling ritual that he does every morning. He spends at least five to ten minutes jotting down his ideas and plans, which he states helps him “push the ball forward”.
- Jim Rohn , the world-renowned business philosopher journaled constantly. In fact, keeping a journal was one of his best recommendations for life change and getting on the right track for goal achievement. If you’ve ever studied or listened to any of Jim Rohn’s famous lectures, you’d hear him zealously encourage everyone to get into the habit of keeping a journal.
- Benjamin Franklin , one of America’s most famous founding fathers was a consummate journal keeper. He was known to keep methodical records of his ideas and musings on life, politics, his ideas, and business. But, most importantly, he would use his journals for the habitual learning, reflection, and accountability that lead him to become the highly accomplished renaissance man we’ve come to revere.
- One of the most talented individuals to have ever lived, Leonardo Da Vinci , was known to have filled tens of thousands of pages with note taking and planning. And look what that did for him, it helped him become one of the best innovators and artists the world has ever known. Journaling has something truly magical about it, especially when you use it as a mechanism to make progress on your ideas and goals.
- Albert Einstein wrote more than 80,000 pages in his journals. And well, he was one of the most accomplished physicists to have ever lived. Was it the journals that lead him to his great achievements? Probably not 100%, but, the journaling certainly helped him gain clarity around his ideas and improved his thinking; two things that did lead to many of his greatest theoretical accomplishments.
There’s a good reason so many others have also documented why many of the world’s most successful people kept journals.
The reason is because journals are a great way to create a ritual around planning your day, brainstorming your big ideas, visualizing your success, and recording your gratitude… all things some of the most successful people do on the daily.
So, now you know what many of the greats have done to stay motivated to achieve. They used a journal.
Now, all you have to do is get out there and get yourself a journal, and then get to work.
If you don’t know where to start don’t worry. We will take care of you. We know a thing or two about motivational journals, as such, we’ll be listing our top rated motivational journals below.
Whichever journal you choose, we believe you can’t go wrong with any of the choices below.
Don’t Know Where to Start? Try These Motivational Journals

Note: We’re reader-supported. When you buy through links on our site, we may earn an affiliate commission.
1. The Freedom Journal
Our first recommendation is The Freedom Journal. John Lee Dumas of the hit Podcast ‘Entrepreneur On Fire’ created the high-quality product known as The Freedom Journal.
This motivational journal acts as a personal accountability partner, and does a good job helping people stay motivated to accomplish their #1 goal in 100 days.
With that said, we think you’ll like the product. And if you don’t, they have a 100% money-back, 1-year guarantee. So, if you’ve yet to employ this journal, give it a look.

2. Best Self Motivational Journal
Our next suggestion is the Best Life journal. This journal is both a week life planner and a motivational journal tied into one. The Best Life Journal has a daily progress tracker to help you outperform your prior goals.
It also includes a section for cultivating daily gratitude and improving your positivity levels. This is important, because we are more inclined to take action on our goals when we feel good about our lives and about ourselves.
No doubt, it is a motivational journal worthy of your consideration.

3. The Strive Journal
In case you didn’t already know, one of the best journals designed specifically to help you stay motivated long enough to achieve your goals is The Strive Journal. The Strive Journal is a motivation journal that helps you persist long enough on your goals to see them through.
The components of the journal have been pulled together based off years of journaling and accomplishing goals, and it includes various aspects which are effective for creating feelings of accomplishment, which in turn can motivate you to keep making progress towards goals.
By and large, this motivational journal is terrific for helping you make move forward on your goals and not quit too soon. So, give it a try if you’re struggle with persistence.

“Set goals for the day, the week, the month, the year, and my life. Just as the rain must fall before the wheat will crack its shell and sprout, so must I have objectives before my life will crystallize. – Og Mandino
There you have it, if you you’re looking to journal for motivation, then you can’t go wrong with the motivational journals recommended.
With that being said, the only thing standing between you and the achievement of your goals is the consistent and motivated action needed to bridge the gap.
So, go get yourself a journal and bridge that gap!
That said, if you enjoyed this page on motivation journals, then you may also find value in the following resources:
Best Motivational Books | Top Motivational Videos | Motivational Audiobooks
Obviously, there are other standard journals and even other motivation journals out there for you to use to help you ritualize your motivation. So by all means, do further research if you need to, and choose whatever works best for you.
SELF-DISCIPLINE TIPS: THE BEST 7 WAYS TO IMPROVE SELF-DISCIPLINE

Just about every single person on earth has in some way, shape, or form struggled with self-discipline. Most people wish there was an easy pill, or wish there was some type of shortcut that would allow them to bypass the discipline required to achieve their goals, but, there isn’t one. Goals, and by extension, success, requires self-discipline. So, while there’s no shortcuts to success, the next best thing is a handful of highly effective self-discipline tips.
“Discipline Is The Bridge Between Goals And Accomplishment.”
That said, the more self-discipline you have, the more success you’ll have. It’s that simple. The hard part of course, is in the becoming. Becoming self-discipline is a challenge. But, challenges are meant to be overcome, and it’s why we’ve decided to pull together this list of the top 7 ways to improve self-discipline.
Our hope is that you’ll learn a thing or two from this short but powerful collection of self-discipline tips, and find more success in your life as you put them to work for you. So, if you’re ready to discover some of the absolute best way to improve your self-discipline levels, then let’s dive right in:
BEST 7 WAYS TO IMPROVE SELF-DISCIPLINE

1. Set Realistic Goals
Believe it or not, setting a goal is one of the most powerful self-discipline tips you could employ. [1] A goal well set can get even the most sluggish person among us moving, grooving, and on track.
However, you can’t just set any goal, it has to be a realistic one.
Certainly, when we have a critical mission it seems wise to take care of the larger tasks first. However, larger goals are harder to reach, which makes self-discipline more challenging.
For instance, you may want to lose a significant amount of weight; however, after training hard for a few weeks and seeing meager results, you may want to give up.
Therefore, it’s far better to commit to an intermediary goal like dropping a few inches a month, rather than choosing one that overwhelms you and causes you to throw in the towel too soon. Sure you can aim high, but aim for realistic intermediary goals first.
And as you reach those goals, then simply raise the bar a little higher. This one self-discipline tip alone will level-up just about anyone’s self-discipline.
Related: Keys to Accomplishing Your Goals
2. Avoid Temptation
When it comes to self-discipline, it’s best that we stay away from things that can take us away from our goal. If we are trying to quit something, like smoking for instance. Then it’s important to stay away from people who regularly smoke cigarettes.
By doing this, we won’t be tempted to partake in the temptation.
Similarly, if you’re trying to lose weight, get the junk food out of your pantry. Having easy access to the things that will get you off course will weaken your resolve faster than almost any other thing.
Of course, this tip can be one of the hardest tips to improve your self discipline if you don’t proactively remove those temptations first. So, be sure to keep those vices out of reach and out of sight.
Just remember, that when our vices are out of our reach, it’s so much easier to focus on other things, like our goals.
3. Do a Countdown
We’ve all had those pesky “I’ll do it later” moments; A.K.A. procrastination . Now, believe it or not, procrastinating is one of self-discipline’s greatest rivals. In a sense, they are antithetical to each other, meaning they are each other’s opposites.
Fortunately, there is a way to defeat self-discipline’s arch nemesis. Jus do this; when you’re feeling lazy or hesitant to follow through with your goal, conduct a simple countdown. Seriously, doing a simple count can help defeat procrastination.
Counting down from ten can get you out of bed for a jog or to get you off of the couch to cook dinner for your family. The countdown provides a bumper before springing into action. If necessary, you can yourself as much as a minute and work our way down, or you can go with just five seconds like motivational coach Mel Robbins suggests.
4. Reward Good Behavior
Unfortunately, we’re usually better at punishing ourselves for poor behavior than rewarding good behavior. From now on, we need to start giving ourselves praise when we stay on track to meet our goals.
Now, the rewards don’t have to be large or extravagant. In fact, your reward can be as simple as allowing yourself a cheat dessert after eating healthy six days of the week.
In some cases, rewards can be a break. it’s possible to overextend ourselves with little to no rest, especially with physical goals. Keep in mind, we don’t want to go overboard with rewards. Rewarding ourselves with every minor goal we meet, we can become counterproductive and even stagnant in our ability to self-regulate.
5. Recruit Someone to Help with Accountability
Having someone to support our efforts is great for a number of reasons. For one, there’s someone there to encourage and motivate us to move forward. It’s also great to have someone there to hold us accountable when we begin to slack.
Say we’re trying to go into business for ourselves. There’s a lot of work that goes into entrepreneurship, and procrastination can make or break our chances of success. If a friend or partner helps us stay focused, we’ll have an easier time getting to the finish line. [2]
Even when times are hard, they can give us the motivation we need as opposed to giving up.
6. Understand Your Weaknesses
Before you start your self-discipline journey, it’s important that you are honest about your shortcomings prior to setting any goals. Once you identify what you struggle with, you can work on overcoming and moving closer to what it is you are trying to achieve.
For example, you may have a hard time saying no to people you love, even if it gets in the way of accomplishing your personal goals. Or you may have enjoy having a few drinks every weekend to relieve stress; which is okay, but if you love doing it, and it gets in the way of your goals, then making a mental not of this weakness is key.
When you improve your clarity, you’ll improve your results. Overtime, you’ll learn how to turn your weaknesses into strengths.
Related: Self-Discipline Affirmations
7. Prioritize Wellness
This is easily one of the most important tips to improve self discipline. All of the hard work is irrelevant if we’re not taking care of our physical, mental, and emotional health.
When it comes to discipline, to get optimal results, we need to maintain healthy diets, get enough rest, and keep our stress levels at bay. Once we start prioritize wellness and our well-being, we’ll have an easier time and more energy to actionize our goals.
As a result, our ability to be more disciplined with improve across the board and almost effortlessly.
Bonus Self-Discipline Tip
Here’s our final self-discipline tip, and it’s one that all too many people over look. Most people likely overlook this tip because most people don’t like to read or study. But, learning and seeking mastery over any topic, is the best to ensure you become good at a thing.
When people want to get good at managing their money, they study money. When people want to improve their cooking skills, they research cooking techniques. And striving to improve your self-discipline is no different. It’s why you are on this page.
So, if you really want to improve your self-discipline, and take it to the next level by giving serious effort and time towards studying the various self-discipline books that are out there, and then practicing what you learned. Do this, and there’s no way you can’t but improve your discipline.
Repetition is the mother of skill, so here’s a final recap of the 7 best ways to improve self-discipline to find more success in everything you do:
- Set Realistic Goals
- Avoid/Remove Temptations
- Do A Countdown
- Reward Good Behavior
- Recruit An Accountability Partner
- Understand Your Weaknesses
- Prioritize Your Wellness
- Study Self-Discipline
We all can benefit from perfecting our self discipline. Using these tips for self-discipline will not only help with productivity, it will also benefit your overall wellness, your ability to connect with others, and most importantly, they’ll help you become more successful.
Best of all, you don’t have to do it alone. By reaching out to others, we can help each other fortify our levels of self-discipline, reach our goals, and avoid giving up on our dreams .
PS – If you enjoyed these self-discipline tips, then you’ll love this article on how to build self-discipline as well.
HOW TO DEVELOP DISCIPLINE THE EASY WAY

Discipline is one of the most important factors for achieving success. Many people already know this, but unfortunately many of them perceive the consistent application of discipline to be too hard. As a result, many people never take those first steps towards their big goals.
They assume they don’t have what it takes to succeed, so never try. But we are here to tell you that being disciplined doesn’t have to be hard. In fact, there is an easy way to develop discipline. So, if you want to know how to develop discipline the easy way, then this article is for you.
We aim to share with you one of the easiest, yet effective ways to develop the discipline you’ll need to start achieving more of what you truly want in life. That being said, if you’re ready to learn about the easiest and most effective ways to develop discipline, let’s get started.
HOW TO DEVELOP DISCIPLINE

1. Start With Little Disciplines
One of the most simple ways to develop your self-discipline muscles is to start small. When you start executing on those seemingly small disciplines, you’ll begin noticing that you are in fact slowly progressing on a larger discipline.
Large disciplines are basically the accumulation of many smaller disciplines. And after you’ve tackled enough of those small disciplines, to your amazement, you’ll have executed on a big one.
On top of this, every discipline executed, regardless of size, impacts your ability to execute on other disciplines. And the more you practice exercising your discipline, the stronger it will become over time.
So start small, and never forget that inch by inch everything is a cinch.
“Inch by inch everything is a cinch.” – Robert Schuller –
2. Create a Goal That Inspires
A person who has a strong enough “WHY” never has to worry about the “HOW”. Too many people shrug off the power of goal-setting , but when it’s done correctly, a person can anoint themselves with seemingly god-like levels of discipline.
By creating a goal that inspires, and by reviewing that goal daily, you position yourself to be pulled by your goals. This “pulling effect”, will lead to you taking action day in and day out towards your goals, even on days when you’re not 100% up to putting in the work.
So, be extra vigilant in your goal-setting, and you’ll cultivate the extreme self-discipline needed to accomplish great things.
“People are not lazy. They simply have impotent goals – that is, goals that do not inspire them.” – Anthony Robbins –
3. Toss Out The Temptations
Getting off-track is so easy to do. One slight slip up typically leads to another one, and then another, until we get so off track that we choose to throw in the towel on our goals.
But it doesn’t have to be this way. You can take control of the situation and set yourself up for success by outsmarting your environment. And all it requires of you, is a little pre-emptive work to rid your environment of the distractions and temptations that will get you off your game.
If your goal requires losing weight, toss out the junk food in your cupboard. If your goal requires less distractions like binge watching YouTube or FB scrolling, remove those apps from your phone.
You get the picture, if there is a temptation or distraction that can potentially hinder taking the actions necessary to reach your goals, toss them.
“Temptation usually comes in through a door that has deliberately been left open.” – Arnold H. Glasow –
4. Hold Yourself Accountable
Self-discipline is all about self-regulation, self-direction, and getting yourself to do what you said you were going to do. As such, you also need to hold yourself accountable.
By holding yourself accountable, you’ll be able to get yourself to do more. You’ll remember, that if you don’t do what you said you were going to do, there will be a consequence.
So, to hold yourself accountable, all you have to do is choose a consequence for yourself, if you don’t follow through. Yes, this will be hard. And it should be.
The consequence you set for yourself, will help drive you to act when you are suppose. And it can be something simple, like saying to yourself, ‘Okay, if don’t go to the gym at least 4 times this week, then I don’t get to have any ice cream this weekend.’
It’s simple accountability, but it’s effective.
“If we don’t discipline ourselves, the world will do it for us.” – william feather –
Final Thoughts Developing Discipline The Easy Way
Anyone can develop discipline, and it is especially easy if the steps outlined are followed. Remember, discipline is not as difficult as it seems, and once you master it, your whole world will change. You’ll achieve more goals, and in so doing, you’ll begin getting more of what you want in life.
Once again, the easy way for you to develop discipline is to practice these three simple steps:
- Start With Small Disciplines
- Create a Goal That Pulls You Into Action
- Toss Out Temptations
- Hold Yourself Accountable
Lastly, if you enjoyed this article and tips mentioned above, then you’ll love these handful of articles created to support you in developing the discipline needed to achieve all your goals:
Books for Building Self-Discipline
How to Build Self-Discipline
Discipline Affirmations That Actually Work
Self-Discipline: The Key to Happiness
Follow the simple steps outlined in this article, use the recommended resources above, and then leverage your new found discipline to create the life you want. Easy peasy.
PS – If you enjoyed this article on how to develop self-discipline, then you’ll likely enjoy this article on why discipline is the key to success .

100+ DAVID GOGGINS QUOTES TO HELP YOU GET AND STAY INSPIRED

35+ KEEP MOVING FORWARD QUOTES TO HELP YOU GO THE DISTANCE

25+INSPIRING SYLVESTER STALLONE QUOTES FOR SUCCESS

RUDY RUETTIGER NET WORTH

25 AFFIRMATIONS FOR CONFIDENCE THAT ACTUALLY WORK

RYAN PINEDA NET WORTH AND HOW HE GOT SO RICH

ANDREW CARNEGIE’S NET WORTH + MIND-BLOWING EARNING POWER

100+ INSPIRING EFFORT QUOTES TO HELP YOU ACHIEVE YOUR POTENTIAL

100+ HARD WORK QUOTES TO HELP YOU OUTWORK EVERYONE

100+ INSPIRING QUOTES ABOUT FOLLOWING YOUR DREAMS

100+ MOTIVATIONAL QUOTES TO HELP YOU NEVER GIVE UP
Home — Essay Samples — Life — Discipline — Importance of Self Discipline
Importance of Self Discipline
- Categories: Discipline
About this sample

Words: 623 |
Published: Jun 13, 2024
Words: 623 | Page: 1 | 4 min read
Table of contents
Personal development, academic success, professional achievement.

Cite this Essay
Let us write you an essay from scratch
- 450+ experts on 30 subjects ready to help
- Custom essay delivered in as few as 3 hours
Get high-quality help

Verified writer
- Expert in: Life

+ 120 experts online
By clicking “Check Writers’ Offers”, you agree to our terms of service and privacy policy . We’ll occasionally send you promo and account related email
No need to pay just yet!
Related Essays
4 pages / 2008 words
4 pages / 1908 words
2 pages / 1087 words
2 pages / 1011 words
Remember! This is just a sample.
You can get your custom paper by one of our expert writers.
121 writers online
Still can’t find what you need?
Browse our vast selection of original essay samples, each expertly formatted and styled
Related Essays on Discipline
Tracy, Brian. 'The Psychology of Success: Develop a Winning Mindset for Achieving Your Goals.' AMACOM, 2019.Covey, Stephen R. 'The 7 Habits of Highly Effective People: Powerful Lessons in Personal Change.' Simon & Schuster, [...]
The topic of corporal punishment in schools has sparked intense debate among educators, parents, and policymakers for decades. This practice, which involves the physical disciplining of students, often through methods such as [...]
Overcoming laziness is a journey that requires self-awareness, discipline, and a willingness to adapt. By understanding the triggers of laziness and employing effective strategies, individuals can regain control over their [...]
In conclusion, the pros and cons of spanking present a complex and multifaceted issue. While proponents argue that spanking can be an effective disciplinary tool, critics highlight the potential for harm and negative [...]
We all have goals for many areas of our lives. Some of us want successful relationships, some like to get more money, others want simply happiness in their lives and others seek better health with less weight. These are common [...]
Discipline is a staple of a competent force and the predominant contributing factor to an effective military. The importance of discipline in the army cannot be overstated, as individual outside stressors and personal issues [...]
Related Topics
By clicking “Send”, you agree to our Terms of service and Privacy statement . We will occasionally send you account related emails.
Where do you want us to send this sample?
By clicking “Continue”, you agree to our terms of service and privacy policy.
Be careful. This essay is not unique
This essay was donated by a student and is likely to have been used and submitted before
Download this Sample
Free samples may contain mistakes and not unique parts
Sorry, we could not paraphrase this essay. Our professional writers can rewrite it and get you a unique paper.
Please check your inbox.
We can write you a custom essay that will follow your exact instructions and meet the deadlines. Let's fix your grades together!
Get Your Personalized Essay in 3 Hours or Less!
We use cookies to personalyze your web-site experience. By continuing we’ll assume you board with our cookie policy .
- Instructions Followed To The Letter
- Deadlines Met At Every Stage
- Unique And Plagiarism Free
More From Forbes
9 powerful ways to cultivate extreme self-discipline.
- Share to Facebook
- Share to Twitter
- Share to Linkedin
“The first and best victory is to conquer self.” ~ PLATO
Learning to effectively lead yourself and others all comes down to discipline. Happiness, success, and fulfillment stem from focus and self-control. It may be hard to believe when you’re facing an all-you-can-eat buffet, the prospect of making a quick buck, or the lazy lure of sleeping in versus getting on the Peloton, but studies show that people with self-discipline are happier. Why? Because with discipline and self-control we actually accomplish more of the goals we truly care about. Self-discipline is the bridge between goals defined and goals accomplished .
Chapter Eight of my new book - Embrace the Suck: The Navy SEAL Way To An Extraordinary Life - is titled ‘Win More Through Discipline And Accountability.’ People with a higher degree of self-control spend less time debating whether to indulge in behaviors and activities that don’t align with their values or goals. They are more decisive. They don’t let impulses or feelings dictate their choices. They are the architects of their own beliefs and the actions they take to achieve a desired outcome. As a result, they aren’t as easily distracted by temptation and tend to feel more satisfied with their lives.
“You have power over your mind—not outside events. Realize this, and you will find strength.” ~ MARCUS AURELIUS
There are specific strategies you can execute to learn self-discipline and gain the willpower to live a happier, more fulfilling life. If you are looking to take control of your habits and choices, here are the eight most powerful things you can do to master self-discipline—which is imperative for life beyond your comfort zone—and maybe even redefining “extraordinary.”
STEP ONE: Know your strengths and weaknesses.
We all have weaknesses. Whether they’re the desire for alcohol, tobacco, unhealthy food, obsession over social media, or the video game Fortnite (what the heck is with this game by the way?!), they have a similar effect on us. Weaknesses don’t just come in the form of areas where we lack self-control either. We all have our strong suits and the stuff we kind of stink at. For example, I don’t care for having difficult conversations, lengthy paperwork that involves digging up old documents I never saved in the first place, holding my temper when someone is shooting at me, or calling into automated phone systems. And therefore, I used to actively (or purposefully) avoid these activities. Now, I strive to tackle them head-on—or I delegate them to others. (Never forget about the subtle art of delegation!)
Self-awareness is a powerful tool for comfort zone expansion, but it requires constant focus and acknowledging your shortcomings, whatever they may be. I suffered from bad allergies and asthma growing up and had terrible eyesight. Those were some significant weaknesses when considering becoming a Navy SEAL. But so what? I trained hard to improve my lung function and used money I’d saved for LASIK eye surgery. Too often people either try to pretend their vulnerabilities don’t exist or they succumb to them with a fixed mindset, throwing their hands up in defeat and saying, “Oh well.” Know your strengths, but more importantly, own up to your flaws. You can’t overcome them until you do.
Best High-Yield Savings Accounts Of 2024
Best 5% interest savings accounts of 2024.
STEP TWO: Remove temptations.
“I can resist anything except temptation.” ~ OSCAR WILDE
Like the saying goes, “out of sight, out of mind.” It may seem silly, but this phrase offers powerful advice. By simply removing the biggest temptations from your environment, you will greatly improve your self-discipline. When I decided I was going to pursue the lofty goal of becoming a SEAL, everything in my life had to change. If you want to eat healthier, toss the junk food in the trash. Want to drink less? Throw out the booze. If you want to enhance your productivity at work, improve the management of your To-Do’s, turn off social media notifications and silence your cell phone. Prioritize and execute.
The fewer distractions you have, the more focused you will be on accomplishing your goals. Set yourself up for success by ditching bad influences.
STEP THREE: Set clear goals and have an execution plan.
If you hope to achieve greater degrees of self-discipline, you must have a clear vision of what you hope to accomplish, just like any goal. You must also have an understanding of what success means to you. After all, if you don’t know where you are going, it’s easy to lose your way or get sidetracked. Remember to prioritize. At TakingPoint Leadership, when we work with our corporate clients on strategic planning, execution, and organizational transformation, we remind them that having ten priorities translates to no priorities.
A clear plan outlines each time-bound step you must take to reach your goals. Create a mantra to keep yourself focused. Successful people use this technique to stay on track, emotionally connect to their mission, and establish a clear finish line.
STEP FOUR: Practice daily diligence.
We aren’t born with self-discipline; it’s a learned behavior. And just like any other skill you want to master, it requires daily practice and repetition. It must become habitual. But the effort and focus that self-discipline requires can be draining. As time passes, it can become more and more difficult to keep your willpower in check. The bigger the temptation or decision, the more challenging it can feel to tackle other tasks that also require self-control.
So, work on building your self-discipline through daily diligence in a given area associated with a goal. This goes back to step three. In order to practice daily diligence, you must have a plan. Put it on your calendar, your to-do list, tattoo it on the back of your eyelids - whatever works best for you. With practice, anyone can push the boundaries of their comfort zone every day.
STEP FIVE: Create new habits and rituals.
Acquiring self-discipline and working to instill a new habit can feel daunting at first, especially if you focus on the entire task at hand. To avoid feeling intimidated, keep it simple. Break your goal into small, doable steps. Instead of trying to change everything at once, focus on doing one thing consistently and master self-discipline with that goal in mind.
As we say in the SEAL Teams, “ Eat the elephant one bite at a time.”
If you’re trying to get in shape but don’t exercise regularly (or ever), start by working out ten or fifteen minutes a day. If you’re trying to achieve better sleep habits, start by going to bed thirty minutes earlier each night. If you want to eat healthier, change your grocery shopping habits and prep meals ahead of time. Take baby steps. Eventually, when your mindset and behavior starts to shift, you can add more goals to your list.
STEP SIX: Change your perception about willpower.
If you believe you have a limited amount of willpower, you probably won’t surpass those limits. As I mentioned previously, studies show that willpower can deplete over time. But what about changing that perception? The SEAL candidate who believes they probably won’t make it through training won’t succeed. Why assume our will to win can only take us so far?
When we embrace the mindset of unlimited willpower, we continue to grow, achieve more, and develop mental toughness. It’s the same philosophy as setting “stretch” goals. In short, our internal conceptions about willpower and self-control can determine how disciplined we are. If you can remove these subconscious obstacles and truly believe you can do it, then you will give yourself an extra boost of motivation toward making those goals a reality.
STEP SEVEN: Give yourself a backup plan.
In the SEAL Teams, we always have contingency plans. Psychologists use a technique to boost willpower called “implementation intention.” That’s when you give yourself a plan to deal with a potentially difficult situation you know you will likely face. To be clear, I am not referring to a backup plan under the auspices that you’ll probably fail at Plan A.
Let’s say you aspire to become a trapeze expert, but tell yourself, “Well, I’m probably not going to excel at this, so chances are I’ll be sticking with miniature golf.” That’s a lame backup plan wrapped in mediocrity. We are talking about contingencies for intentional course correction, not planning for failure. So be bold and keep moving forward. Going in with a plan will help give you the mindset and self-control necessary for the situation. You will also save energy by not having to make a sudden decision based on your emotional state.
STEP EIGHT: Find trusted coaches or mentors.
The development of expertise requires coaches who are capable of giving constructive, even painful, feedback. Real experts are extremely motivated students who seek out such feedback. They’re also skilled at understanding when and if a coach or mentor’s advice doesn’t work for them.
The elite performers I’ve known and worked with always knew what they were doing right while concentrating on what they were doing wrong. They deliberately picked unsentimental coaches who would challenge them and drive them to higher levels of performance. The best coaches also identify aspects of your performance that will need to be improved at your next level of skill and aid you in preparation.
STEP NINE: Forgive yourself and move forward.
Even with all our best intentions and well laid plans, we sometimes fall short. It happens. You will have ups and downs, great successes and dismal failures. The key is to keep going. A very close SEAL buddy of mine has had a lifelong dream of not just serving in the SEAL Teams but also making it to our tier one special missions unit. He has every qualification this unit could possibly want, but for some reason they didn’t select him on his first application attempt. Did he wallow in sorrow? Not for one second. He immediately developed a plan to request even more “schools,” train even harder, and he transferred to a different SEAL Team for a better chance to get picked up next time. Easy day.
If you stumble, find the root cause by asking the five WHY’s and move on. Don’t let yourself get wrapped up in guilt, anger, or frustration, because these emotions will only drag you further down and impede future progress.
Learn from your missteps and forgive yourself. Then get your head back in the game and violently execute. Good luck!

- Editorial Standards
- Reprints & Permissions
Information
- Author Services
Initiatives
You are accessing a machine-readable page. In order to be human-readable, please install an RSS reader.
All articles published by MDPI are made immediately available worldwide under an open access license. No special permission is required to reuse all or part of the article published by MDPI, including figures and tables. For articles published under an open access Creative Common CC BY license, any part of the article may be reused without permission provided that the original article is clearly cited. For more information, please refer to https://www.mdpi.com/openaccess .
Feature papers represent the most advanced research with significant potential for high impact in the field. A Feature Paper should be a substantial original Article that involves several techniques or approaches, provides an outlook for future research directions and describes possible research applications.
Feature papers are submitted upon individual invitation or recommendation by the scientific editors and must receive positive feedback from the reviewers.
Editor’s Choice articles are based on recommendations by the scientific editors of MDPI journals from around the world. Editors select a small number of articles recently published in the journal that they believe will be particularly interesting to readers, or important in the respective research area. The aim is to provide a snapshot of some of the most exciting work published in the various research areas of the journal.
Original Submission Date Received: .
- Active Journals
- Find a Journal
- Proceedings Series
- For Authors
- For Reviewers
- For Editors
- For Librarians
- For Publishers
- For Societies
- For Conference Organizers
- Open Access Policy
- Institutional Open Access Program
- Special Issues Guidelines
- Editorial Process
- Research and Publication Ethics
- Article Processing Charges
- Testimonials
- Preprints.org
- SciProfiles
- Encyclopedia

Article Menu

- Subscribe SciFeed
- Recommended Articles
- Google Scholar
- on Google Scholar
- Table of Contents
Find support for a specific problem in the support section of our website.
Please let us know what you think of our products and services.
Visit our dedicated information section to learn more about MDPI.
JSmol Viewer
Barriers to care for pediatric patients with obesity.

1. Introduction
1.1. stigma, 1.2. limited care providers, 1.3. barriers to lifestyle changes, 1.4. social determinants of health, 1.5. nutritional, 1.6. exercise, 1.8. psychological and familial support, 1.9. limited treatment options, 1.10. continuity of care, 2. conclusions, conflicts of interest.
- Childhood Obesity Facts. Available online: https://www.cdc.gov/obesity/php/data-research/childhood-obesity-facts.html (accessed on 3 March 2024).
- Child Obesity. Available online: https://www.hsph.harvard.edu/obesity-prevention-source/obesity-trends-original/global-obesity-trends-in-children/ (accessed on 3 March 2024).
- Haqq, A.M.; Kebbe, M.; Tan, Q.; Manco, M.; Salas, X.R. Complexity and Stigma of Pediatric Obesity. Child. Obes. 2021 , 17 , 229–240. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- Pont, S.J.; Puhl, R.; Cook, S.R.; Slusser, W.; Section on Obesity; The Obesity Society. Stigma Experienced by Children and Adolescents with Obesity. Pediatrics 2017 , 140 , e20173034. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- Palad, C.J.; Yarlagadda, S.; Stanford, F.C. Weight stigma and its impact on paediatric care. Curr. Opin. Endocrinol. Diabetes 2019 , 26 , 19–24. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- Braddock, A.; Browne, N.T.; Houser, M.; Blair, G.; Williams, D.R. Weight stigma and bias: A guide for pediatric clinicians. Obes. Pillars 2023 , 6 , 100058. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- Maffeis, C.; Busetto, L.; Wasniewska, M.; Di Pauli, D.; Maccora, C.; Lenzi, A. Perceptions, attitudes, and behaviors among adolescents living with obesity, caregivers, and healthcare professionals in Italy: The ACTION Teens study. Eat. Weight Disord. Stud. Anorex. Bulim. Obes. 2024 , 29 , 35. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- Body Mass Index (BMI). 2024. Available online: https://www.cdc.gov/healthyweight/assessing/bmi/index.html (accessed on 3 March 2024).
- Rubino, F.; Puhl, R.M.; Cummings, D.E.; Eckel, R.H.; Ryan, D.H.; Mechanick, J.I.; Nadglowski, J.; Ramos Salas, X.; Schauer, P.R.; Twenefour, D.; et al. Joint international consensus statement for ending stigma of obesity. Nat. Med. 2020 , 26 , 485–497. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- Roberts, K.J.; Polfuss, M.L. Weight stigma in children and adolescents: Recommendations for practice and policy. Nursing 2022 , 52 , 17–24. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- Arrieta, F.; Pedro-Botet, J. Recognizing obesity as a disease: A true challenge. Rev. Clin. Esp. 2021 , 221 , 544–546. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- Kyle, T.K.; Dhurandhar, E.J.; Allison, D.B. Regarding Obesity as a Disease: Evolving Policies and Their Implications. Endocrinol. Metab. Clin. N. Am. 2016 , 45 , 511–520. [ Google Scholar ] [ CrossRef ]
- Gomez, G.; Stanford, F.C. US health policy and prescription drug coverage of FDA-approved medications for the treatment of obesity. Int. J. Obes. 2018 , 42 , 495–500. [ Google Scholar ] [ CrossRef ]
- Hinton, E.; Elizabeth, W.; Raphael, J.; Mudumala, A.; Rudowitz, R.; Gifford, K. Amid Unwinding of Pandemic-Era Policies, Medicaid Programs Continue to Focus on Delivery Systems, Benefits, and Reimbursement Rates: Results from an Annual Medicaid Budget Survey for State Fiscal Years 2023 and 2024. Available online: https://www.kff.org/report-section/50-state-medicaid-budget-survey-fy-2023-2024-pharmacy/ (accessed on 10 April 2024).
- Satti, K.F.; Tanski, S.E.; Jiang, Y.; McClure, A. Improving Care for Childhood Obesity: A Quality Improvement Initiative. Pediatr. Qual. Saf. 2021 , 6 , e412. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- Rhee, K.E.; Kessl, S.; Lindback, S.; Littman, M.; El-Kareh, R.E. Provider views on childhood obesity management in primary care settings: A mixed methods analysis. BMC Health Serv. Res. 2018 , 18 , 55. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- Lowenstein, L.M.; Perrin, E.M.; Campbell, M.K.; Tate, D.F.; Cai, J.; Ammerman, A.S. Primary care providers’ self-efficacy and outcome expectations for childhood obesity counseling. Child. Obes. 2013 , 9 , 208–215. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- Silberberg, M.; Carter-Edwards, L.; Murphy, G.; Mayhew, M.; Kolasa, K.; Perrin, E.M.; Armstrong, S.; Graham, C.; Menon, N. Treating pediatric obesity in the primary care setting to prevent chronic disease: Perceptions and knowledge of providers and staff. N. C. Med. J. 2012 , 73 , 9–14. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- Thomas, L.N.; Donadio, A.; Carnevale, T.; Neal, P. Improved management of pediatric obesity in the primary care setting through implementation of the healthy care for healthy kids obesity toolkit. J. Pediatr. Nurs. 2022 , 65 , e115–e125. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- Haemer, M.; Cluett, S.; Hassink, S.G.; Liu, L.; Mangarelli, C.; Peterson, T.; Pomietto, M.; Young, K.L.; Weill, B. Building capacity for childhood obesity prevention and treatment in the medical community: Call to action. Pediatrics 2011 , 128 (Suppl. S2), S71–S77. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- Lenders, C.M.; Manders, A.J.; Perdomo, J.E.; Ireland, K.A.; Barlow, S.E. Addressing Pediatric Obesity in Ambulatory Care: Where Are We and Where Are We Going? Curr. Obes. Rep. 2016 , 5 , 214–240. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- Measuring Obesity. Available online: https://www.hsph.harvard.edu/obesity-prevention-source/obesity-definition/how-to-measure-body-fatness/ (accessed on 13 June 2024).
- Kebbe, M.; Perez, A.; Buchholz, A.; McHugh, T.F.; Scott, S.S.; Richard, C.; Mohipp, C.; Dyson, M.P.; Ball, G.D.C. Barriers and enablers for adopting lifestyle behavior changes in adolescents with obesity: A multi-centre, qualitative study. PLoS ONE 2018 , 13 , e0209219. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- Muha, J.; Schumacher, A.; Campisi, S.C.; Korczak, D.J. Depression and emotional eating in children and adolescents: A systematic review and meta-analysis. Appetite 2024 , 200 , 107511. [ Google Scholar ] [ CrossRef ]
- Hahn, R.A. What is a social determinant of health? Back to basics. J. Public Health Res. 2021 , 10 , jphr-2021. [ Google Scholar ] [ CrossRef ]
- Javed, Z.; Valero-Elizondo, J.; Maqsood, M.H.; Mahajan, S.; Taha, M.B.; Patel, K.V.; Sharma, G.; Hagan, K.; Blaha, M.J.; Blankstein, R.; et al. Social determinants of health and obesity: Findings from a national study of US adults. Obesity 2022 , 30 , 491–502. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- Thompson, H.R.; Linchey, J.; Madsen, K.A. Are physical education policies working? A snapshot from San Francisco, 2011. Prev. Chronic Dis. 2013 , 10 , E142. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- Pate, R.R.; Flynn, J.I.; Dowda, M. Policies for promotion of physical activity and prevention of obesity in adolescence. J. Exerc. Sci. Fit. 2016 , 14 , 47–53. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- Nowicka, P.; Ek, A.; Grafstrom, E.; Johansson, T.; Nordin, K.; Neuman, N.; Reijs Richards, H.; Eli, K. How Do Interpersonal Relationships Affect Children’s Weight Management? A Qualitative Analysis of Parents’ Long-Term Perceptions after Obesity Treatment. Child. Obes. 2022 , 18 , 274–280. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- O’Hara, V.; Cuda, S.; Kharofa, R.; Censani, M.; Conroy, R.; Browne, N.T. Clinical review: Guide to pharmacological management in pediatric obesity medicine. Obes. Pillars 2023 , 6 , 100066. [ Google Scholar ] [ CrossRef ]
- Samuels, R.C.; Ward, V.L.; Melvin, P.; Macht-Greenberg, M.; Wenren, L.M.; Yi, J.; Massey, G.; Cox, J.E. Missed Appointments: Factors Contributing to High No-Show Rates in an Urban Pediatrics Primary Care Clinic. Clin. Pediatr. 2015 , 54 , 976–982. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- Robinson, T.N.; Banda, J.A.; Hale, L.; Lu, A.S.; Fleming-Milici, F.; Calvert, S.L.; Wartella, E. Screen Media Exposure and Obesity in Children and Adolescents. Pediatrics 2017 , 140 , S97–S101. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- Westbury, S.; Oyebode, O.; van Rens, T.; Barber, T.M. Obesity Stigma: Causes, Consequences, and Potential Solutions. Curr. Obes. Rep. 2023 , 12 , 10–23. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- Hong, P.K.W.; Santana, J.P.; Larson, S.D.; Berger, A.M.; Indelicato, L.A.; Taylor, J.A.; Mustafa, M.M.; Islam, S.; Neal, D.; Petroze, R.T. Social determinants of health in pediatric scald burns: Is food access an issue? Surgery 2022 , 172 , 1510–1515. [ Google Scholar ] [ CrossRef ]
- Tester, J.M.; Rosas, L.G.; Leung, C.W. Food Insecurity and Pediatric Obesity: A Double Whammy in the Era of COVID-19. Curr. Obes. Rep. 2020 , 9 , 442–450. [ Google Scholar ] [ CrossRef ]
- Cerceo, E.; Sharma, E.; Boguslavsky, A.; Rachoin, J.S. Impact of Food Environments on Obesity Rates: A State-Level Analysis. J. Obes. 2023 , 2023 , 5052613. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- Pope, K.J.; Whitcomb, C.; Vu, M.; Harrison, L.M.; Gittelsohn, J.; Ward, D.; Erinosho, T. Barriers, facilitators, and opportunities to promote healthy weight behaviors among preschool-aged children in two rural U.S communities. BMC Public Health 2023 , 23 , 53. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- Hardy, R.; Boch, S.; Keedy, H.; Chisolm, D. Social Determinants of Health Needs and Pediatric Health Care Use. J. Pediatr. 2021 , 238 , 275–281.e1. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- Yusuf, Z.I.; Dongarwar, D.; Yusuf, R.A.; Bell, M.; Harris, T.; Salihu, H.M. Social Determinants of Overweight and Obesity among Children in the United States. Int. J. Matern. Child Heal. AIDS (IJMA) 2019 , 9 , 22–33. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- Motevalli, M.; Drenowatz, C.; Tanous, D.R.; Khan, N.A.; Wirnitzer, K. Management of Childhood Obesity—Time to Shift from Generalized to Personalized Intervention Strategies. Nutrients 2021 , 13 , 1200. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- Ardeshirlarijani, E.; Namazi, N.; Jabbari, M.; Zeinali, M.; Gerami, H.; Jalili, R.B.; Larijani, B.; Azadbakht, L. The link between breakfast skipping and overweigh/obesity in children and adolescents: A meta-analysis of observational studies. J. Diabetes Metab. Disord. 2019 , 18 , 657–664. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- McCormick, D.P.; Reyna, L.; Reifsnider, E. Calories, Caffeine and the Onset of Obesity in Young Children. Acad. Pediatr. 2020 , 20 , 801–808. [ Google Scholar ] [ CrossRef ]
- Calcaterra, V.; Cena, H.; Magenes, V.C.; Vincenti, A.; Comola, G.; Beretta, A.; Di Napoli, I.; Zuccotti, G. Sugar-Sweetened Beverages and Metabolic Risk in Children and Adolescents with Obesity: A Narrative Review. Nutrients 2023 , 15 , 702. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- Abbasalizad Farhangi, M.; Mohammadi Tofigh, A.; Jahangiri, L.; Nikniaz, Z.; Nikniaz, L. Sugar-sweetened beverages intake and the risk of obesity in children: An updated systematic review and dose-response meta-analysis. Pediatr. Obes. 2022 , 17 , e12914. [ Google Scholar ] [ CrossRef ]
- Monteiro, C.A.; Moubarac, J.C.; Cannon, G.; Ng, S.W.; Popkin, B. Ultra-processed products are becoming dominant in the global food system. Obes. Rev. 2013 , 14 (Suppl. S2), 21–28. [ Google Scholar ] [ CrossRef ]
- Hall, K.D.; Ayuketah, A.; Brychta, R.; Cai, H.; Cassimatis, T.; Chen, K.Y.; Chung, S.T.; Costa, E.; Courville, A.; Darcey, V.; et al. Ultra-Processed Diets Cause Excess Calorie Intake and Weight Gain: An Inpatient Randomized Controlled Trial of Ad Libitum Food Intake. Cell Metab. 2019 , 30 , 67–77.e3. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- Harb, A.A.; Shechter, A.; Koch, P.A.; St-Onge, M.P. Ultra-processed foods and the development of obesity in adults. Eur. J. Clin. Nutr. 2023 , 77 , 619–627. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- Valicente, V.M.; Peng, C.H.; Pacheco, K.N.; Lin, L.; Kielb, E.I.; Dawoodani, E.; Abdollahi, A.; Mattes, R.D. Ultraprocessed Foods and Obesity Risk: A Critical Review of Reported Mechanisms. Adv. Nutr. 2023 , 14 , 718–738. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- Ricotti, R.; Caputo, M.; Monzani, A.; Pigni, S.; Antoniotti, V.; Bellone, S.; Prodam, F. Breakfast Skipping, Weight, Cardiometabolic Risk, and Nutrition Quality in Children and Adolescents: A Systematic Review of Randomized Controlled and Intervention Longitudinal Trials. Nutrients 2021 , 13 , 3331. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- Gearan, E.C.; Fox, M.K. Updated Nutrition Standards Have Significantly Improved the Nutritional Quality of School Lunches and Breakfasts. J. Acad. Nutr. Diet 2020 , 120 , 363–370. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- Hecht, A.A.; Olarte, D.A.; McLoughlin, G.M.; Cohen, J.F.W. Strategies to Increase Student Participation in School Meals in the United States: A Systematic Review. J. Acad. Nutr. Diet 2023 , 123 , 1075–1096.e1. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- Brown, C.L.; Perrin, E.M. Obesity Prevention and Treatment in Primary Care. Acad. Pediatr. 2018 , 18 , 736–745. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- Gato-Moreno, M.; Martos-Lirio, M.F.; Leiva-Gea, I.; Bernal-López, M.R.; Vegas-Toro, F.; Fernández-Tenreiro, M.C.; López-Siguero, J.P. Early Nutritional Education in the Prevention of Childhood Obesity. Int. J. Environ. Res. Public Health 2021 , 18 , 6569. [ Google Scholar ] [ CrossRef ]
- Romanos-Nanclares, A.; Zazpe, I.; Santiago, S.; Marín, L.; Rico-Campà, A.; Martín-Calvo, N. Influence of Parental Healthy-Eating Attitudes and Nutritional Knowledge on Nutritional Adequacy and Diet Quality among Preschoolers: The SENDO Project. Nutrients 2018 , 10 , 1875. [ Google Scholar ] [ CrossRef ]
- Kim, H.S.; Park, J.; Ma, Y.; Im, M. What Are the Barriers at Home and School to Healthy Eating? Overweight/Obese Child and Parent Perspectives. J. Nurs. Res. 2019 , 27 , e48. [ Google Scholar ] [ CrossRef ]
- Chatham, R.E.; Mixer, S.J. Cultural Influences on Childhood Obesity in Ethnic Minorities: A Qualitative Systematic Review. J. Transcult. Nurs. 2020 , 31 , 87–99. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- Baran, J.; Weres, A.; Czenczek-Lewandowska, E.; Łuszczki, E.; Sobek, G.; Pitucha, G.; Leszczak, J.; Mazur, A. Early Eating Patterns and Overweight and Obesity in a Sample of Preschool Children in South-East Poland. Int. J. Environ. Res. Public Health 2019 , 16 , 3064. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- Hall, W.J.; Schneider, M.; Thompson, D.; Volpe, S.L.; Steckler, A.; Hall, J.M.; Fisher, M.R.; Group, H.S. School factors as barriers to and facilitators of a preventive intervention for pediatric type 2 diabetes. Transl. Behav. Med. 2014 , 4 , 131–140. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- Mc Carthy, C.M.; de Vries, R.; Mackenbach, J.D. The influence of unhealthy food and beverage marketing through social media and advergaming on diet-related outcomes in children—A systematic review. Obes. Rev. 2022 , 23 , e13441. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- Smith, R.; Kelly, B.; Yeatman, H.; Boyland, E. Food Marketing Influences Children’s Attitudes, Preferences and Consumption: A Systematic Critical Review. Nutrients 2019 , 11 , 875. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- Libuy, N.; Church, D.; Ploubidis, G.; Fitzsimons, E. Fast food proximity and weight gain in childhood and adolescence: Evidence from Great Britain. Health Econ. 2024 , 33 , 449–465. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- St Pierre, C.; Ver Ploeg, M.; Dietz, W.H.; Pryor, S.; Jakazi, C.S.; Layman, E.; Noymer, D.; Coughtrey-Davenport, T.; Sacheck, J.M. Food Insecurity and Childhood Obesity: A Systematic Review. Pediatrics 2022 , 150 , e2021055571. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- Brownell, K.D.; Kersh, R.; Ludwig, D.S.; Post, R.C.; Puhl, R.M.; Schwartz, M.B.; Willett, W.C. Personal responsibility and obesity: A constructive approach to a controversial issue. Health Aff. 2010 , 29 , 379–387. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- Sonntag, D.; Schneider, S.; Mdege, N.; Ali, S.; Schmidt, B. Beyond Food Promotion: A Systematic Review on the Influence of the Food Industry on Obesity-Related Dietary Behaviour among Children. Nutrients 2015 , 7 , 8565–8576. [ Google Scholar ] [ CrossRef ]
- Zabinski, M.F.; Saelens, B.E.; Stein, R.I.; Hayden-Wade, H.A.; Wilfley, D.E. Overweight children’s barriers to and support for physical activity. Obes. Res. 2003 , 11 , 238–246. [ Google Scholar ] [ CrossRef ]
- Hu, J.; Li, Z.; Li, S.; Li, H.; Wang, S.; Wang, S.; Xu, L.; Yang, D.; Ruan, T.; Li, H.; et al. Skipping breakfast and physical fitness among school-aged adolescents. Clinics 2020 , 75 , e1599. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- Fromel, K.; Groffik, D.; Mitas, J.; Madarasova Geckova, A.; Csanyi, T. Physical Activity Recommendations for Segments of School Days in Adolescents: Support for Health Behavior in Secondary Schools. Front. Public Health 2020 , 8 , 527442. [ Google Scholar ] [ CrossRef ]
- An, R.; Yang, Y.; Hoschke, A.; Xue, H.; Wang, Y. Influence of neighbourhood safety on childhood obesity: A systematic review and meta-analysis of longitudinal studies. Obes. Rev. 2017 , 18 , 1289–1309. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- [Anon]. Federal Policy Opportunities to Increase Physical Activity. Available online: https://www.aap.org/en/patient-care/institute-for-healthy-childhood-weight/obesity-prevention-policy-opportunities-tool/federal-advocacy-strategies-to-increase-physical-activity/ (accessed on 18 April 2024).
- Kanellopoulou, A.; Notara, V.; Magriplis, E.; Antonogeorgos, G.; Rojas-Gil, A.P.; Kornilaki, E.N.; Lagiou, A.; Yannakoulia, M.; Panagiotakos, D.B. Sleeping patterns and childhood obesity: An epidemiological study in 1728 children in Greece. J. Clin. Sleep Med. 2021 , 17 , 1093–1101. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- Paruthi, S.; Brooks, L.J.; D’Ambrosio, C.; Hall, W.A.; Kotagal, S.; Lloyd, R.M.; Malow, B.A.; Maski, K.; Nichols, C.; Quan, S.F.; et al. Recommended Amount of Sleep for Pediatric Populations: A Consensus Statement of the American Academy of Sleep Medicine. J. Clin. Sleep Med. 2016 , 12 , 785–786. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- Guo, Y.; Miller, M.A.; Cappuccio, F.P. Short duration of sleep and incidence of overweight or obesity in Chinese children and adolescents: A systematic review and meta-analysis of prospective studies. Nutr. Metab. Cardiovasc. Dis. 2021 , 31 , 363–371. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- Kuki, A.; Terui, A.; Sakamoto, Y.; Osato, A.; Mikami, T.; Nakamura, K.; Saito, M. Prevalence and factors of sleep problems among Japanese children: A population-based study. Front. Pediatr. 2024 , 12 , 1332723. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- Chaput, J.P.; Dutil, C. Lack of sleep as a contributor to obesity in adolescents: Impacts on eating and activity behaviors. Int. J. Behav. Nutr. Phys. Act. 2016 , 13 , 103. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- Fatima, Y.; Doi, S.A.R.; Al Mamun, A. Sleep problems in adolescence and overweight/obesity in young adults: Is there a causal link? Sleep Health 2018 , 4 , 154–159. [ Google Scholar ] [ CrossRef ]
- Fatima, Y.; Doi, S.A.; Mamun, A.A. Sleep quality and obesity in young subjects: A meta-analysis. Obes. Rev. 2016 , 17 , 1154–1166. [ Google Scholar ] [ CrossRef ]
- Wu, Y.; Gong, Q.; Zou, Z.; Li, H.; Zhang, X. Short sleep duration and obesity among children: A systematic review and meta-analysis of prospective studies. Obes. Res. Clin. Pract. 2017 , 11 , 140–150. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- Miller, A.L.; Lumeng, J.C.; LeBourgeois, M.K. Sleep patterns and obesity in childhood. Curr. Opin. Endocrinol. Diabetes 2015 , 22 , 41–47. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- Skjakodegard, H.F.; Danielsen, Y.S.; Frisk, B.; Hystad, S.W.; Roelants, M.; Pallesen, S.; Conlon, R.P.K.; Wilfley, D.E.; Juliusson, P.B. Beyond sleep duration: Sleep timing as a risk factor for childhood obesity. Pediatr. Obes. 2021 , 16 , e12698. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- Caliendo, C.; Femiano, R.; Umano, G.R.; Martina, S.; Nucci, L.; Perillo, L.; Grassia, V. Effect of Obesity on the Respiratory Parameters in Children with Obstructive Sleep Apnea Syndrome. Children 2023 , 10 , 1874. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- Feldman, M.A.; Yardley, H.L.; Bulan, A.; Kamboj, M.K. Role of Psychologists in Pediatric Endocrinology. Pediatr. Clin. N. Am. 2022 , 69 , 905–916. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- Smith, K.E.; Goldschmidt, A.B. Treatment of Binge-Eating Disorder Across the Lifespan: An Updated Review of the Literature and Considerations for Future Research. Curr. Obes. Rep. 2024 , 13 , 195–202. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- Counts, N.Z.; Vasan, A. Advancing mental health parity to ensure children’s access to care. Npj Ment. Health Res. 2024 , 3 , 28. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- Chai, L.K.; Collins, C.; May, C.; Brain, K.; Wong See, D.; Burrows, T. Effectiveness of family-based weight management interventions for children with overweight and obesity: An umbrella review. JBI Evid. Synth. 2019 , 17 , 1341–1427. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- Eli, K.; Howell, K.; Fisher, P.A.; Nowicka, P. A question of balance: Explaining differences between parental and grandparental perspectives on preschoolers’ feeding and physical activity. Soc. Sci. Med. 2016 , 154 , 28–35. [ Google Scholar ] [ CrossRef ]
- Eli, K.; Hornell, A.; Etminan Malek, M.; Nowicka, P. Water, juice, or soda? Mothers and grandmothers of preschoolers discuss the acceptability and accessibility of beverages. Appetite 2017 , 112 , 133–142. [ Google Scholar ] [ CrossRef ]
- Perez, A.; Holt, N.; Gokiert, R.; Chanoine, J.P.; Legault, L.; Morrison, K.; Sharma, A.; Ball, G. Why don’t families initiate treatment? A qualitative multicentre study investigating parents’ reasons for declining paediatric weight management. Paediatr. Child Health 2015 , 20 , 179–184. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- Dhaliwal, J.; Perez, A.J.; Holt, N.L.; Gokiert, R.; Chanoine, J.P.; Morrison, K.M.; Legault, L.; Sharma, A.M.; Ball, G.D.C. Why do parents discontinue health services for managing paediatric obesity? A multi-centre, qualitative study. Obes. Res. Clin. Pract. 2017 , 11 , 335–343. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- Hampl, S.E.; Hassink, S.G.; Skinner, A.C.; Armstrong, S.C.; Barlow, S.E.; Bolling, C.F.; Avila Edwards, K.C.; Eneli, I.; Hamre, R.; Joseph, M.M.; et al. Clinical Practice Guideline for the Evaluation and Treatment of Children and Adolescents with Obesity. Pediatrics 2023 , 151 , e2022060640. [ Google Scholar ] [ CrossRef ]
- A Study to Evaluate Tirzepatide (LY3298176) in Pediatric and Adolescent Participants with Type 2 Diabetes Mellitus Inadequately Controlled with Metformin or Basal Insulin or Both (SURPASS-PEDS). Available online: https://classic.clinicaltrials.gov/ct2/show/NCT05260021 (accessed on 1 April 2024).
- A Research Study on How Well Semaglutide Helps Children and Teenagers with Excess Body Weight Lose Weight (STEP Young). Available online: https://classic.clinicaltrials.gov/ct2/show/NCT05726227 (accessed on 1 April 2024).
- Mital, S.; Nguyen, H.V. Cost-Effectiveness of Antiobesity Drugs for Adolescents with Severe Obesity. JAMA Netw. Open 2023 , 6 , e2336400. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- Whitley, H.P.; Trujillo, J.M.; Neumiller, J.J. Special Report: Potential Strategies for Addressing GLP-1 and Dual GLP-1/GIP Receptor Agonist Shortages. Clin. Diabetes 2023 , 41 , 467–473. [ Google Scholar ] [ CrossRef ]
- Putka, S. Weight-Loss Drug Zepbound Faces Supply Issues. Available online: https://www.medpagetoday.com/special-reports/features/109471 (accessed on 8 April 2024).
- Shapiro, W.L.; Kunani, P.; Sidell, M.A.; Li, X.; Anderson, S.R.; Slezak, J.M.; Koebnick, C.; Schwimmer, J.B. Prevalence of Adolescents Meeting Criteria for Metabolic and Bariatric Surgery. Pediatrics 2024 , 153 , e2023063916. [ Google Scholar ] [ CrossRef ]
- Griggs, C. Bariatric Endoscopy and Surgery in the Pediatric Patient. In Proceedings of the Blackburn Course in Obesity Medicine Treating Obesity 2024, Virtual, 12 June 2024. [ Google Scholar ]
| The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
Share and Cite
Bodepudi, S.; Hinds, M.; Northam, K.; Reilly-Harrington, N.A.; Stanford, F.C. Barriers to Care for Pediatric Patients with Obesity. Life 2024 , 14 , 884. https://doi.org/10.3390/life14070884
Bodepudi S, Hinds M, Northam K, Reilly-Harrington NA, Stanford FC. Barriers to Care for Pediatric Patients with Obesity. Life . 2024; 14(7):884. https://doi.org/10.3390/life14070884
Bodepudi, Sreevidya, Malikiya Hinds, Kayla Northam, Noreen A. Reilly-Harrington, and Fatima Cody Stanford. 2024. "Barriers to Care for Pediatric Patients with Obesity" Life 14, no. 7: 884. https://doi.org/10.3390/life14070884
Article Metrics
Article access statistics, further information, mdpi initiatives, follow mdpi.

Subscribe to receive issue release notifications and newsletters from MDPI journals
11 Simple Ways to Start Building Self-Discipline Right Now

Self-discipline is difficult to master. It can be discouraging when you have the best of intentions but tend to fall short of what you set out to do. Research shows that some conditions make it harder to be self-disciplined. For example, if you’re constantly faced with temptation, you might give in and find it hard to stay on track. [ 1 ] Other conditions make it easier to be self-disciplined. For instance, being well-organized will help you make progress toward your goals. [ 2 ]
In this article, we are going to help you build self-discipline, even if you start from scratch. We will guide you in what to do and what to avoid when you’re striving toward a personal goal or trying to pick up a new habit. We’ll also give you a definition of self-discipline and tell you more about how being self-disciplined can benefit your life. Finally, we’ll throw in some quotes and a reading list to inspire you on your journey toward becoming more self-disciplined.
What is self-discipline?
How to build self-discipline.
Self-discipline represents the qualities that enable people to accomplish goals or adopt new habits, no matter what obstacles arise along the way. [ 3 ] There are three key qualities that make self-discipline possible: the ability to pay attention, self-control, and persistence. [ 4 ]
Let’s look at an example to show how these qualities come together to make self-discipline happen.
Charlie dreams of becoming a web designer. He loves the creative, practical side of web design but he hates learning the theory behind it. To get a qualification in web design, he’d need to study and pass theoretical exams. Since he hates theory, he’d have to practice some serious self-discipline to study and get through his exams.
He’d need to:
- Pay attention . He’d have to focus hard enough and long enough when studying material he finds boring or challenging in order to pass his exams.
- Maintain self-control. He’d have to control his urges to do something more appealing, like watching TV or going out with his friends.
- Persist. He’d have to consistently choose behaviors that will help him pass his exams. He’d have to keep working hard to focus and maintain self-control when things get tough.
As you can see, self-discipline is about consistently choosing behaviors that will help you reach your goal while inhibiting behaviors that will deter you from it.
Self-discipline comes more naturally to some people than to others. However, that doesn’t mean that you can’t learn and get better at self-discipline if you struggle with it. [ 5 ]
Here are 11 tips to build self-discipline:
1. Conduct a self-assessment
If you’ve been thinking about starting to be more self-disciplined, then there’s a good chance you’ve identified one or two areas in your life that need improvement. If you can’t pinpoint where you need to strengthen your self-discipline, take stock of a typical day in your life to identify areas where your self-discipline is lacking.
Get a piece of scrap paper and draw two columns, one with the heading “What I did well today” and another with the heading, “What I could have done better.” As you reflect on your day, fill in the columns. Maybe you managed your time well and completed the tasks you needed to do. However, this came at the cost of sticking to your healthy meal plan because you ordered fast food to save time.
You might also like this article on improving self-awareness .
2. Turn weaknesses into goals
Once you’ve identified what your weak spots are when it comes to self-discipline, try coming up with some goals aimed at improvement. The SMART method of goal setting can help you muster the self-discipline needed to reach your goal. [ 6 ] When you set smart goals, you make your goals specific, measurable, attainable, realistic, and time-bound. [ 6 ]
Here’s an example. Say your weakness is your exercise regime—which is non-existent at the moment. Instead of setting the goal “I want to exercise more,” your SMART goal would be the following: “I want to run for 30 minutes, two times a week from 18h30-19h00 on Mondays and Fridays.” Be careful not to make your goal too difficult and keep it as specific as possible for the best chance at success.
3. Determine your why
When you’re working toward a goal, it’s easy to become weary and lose motivation along the way. Remembering why you set the goal to begin with and why it’s important to you can help you stay strong and disciplined. [ 7 ]
The next time you feel your energy and your drive waning, take a moment to reflect. Ask yourself what the purpose is for doing what you’re doing. What is the long-term reward? Then, write the answer down and keep it somewhere you’ll see it often.
For example, if you’re working late on weekends to start up a new business, stick a post-it note with some encouraging words on your laptop. The post-it note can act as a reminder of why you’re putting in the long yards when you’d rather be out enjoying yourself with everyone else!
4. Track your progress
When you’re working toward a goal, it’s normal to feel discouraged at some point. Tracking your progress can help you stay disciplined because it’s a reminder of how far you’ve come and what you’re capable of. [ 8 ]
You can track progress toward your goal by coming up with milestones and ticking them off as you get closer to achieving your end goal. For example, say your goal was to be ready to run a half marathon within 12 weeks. You may start out with an initial goal to run 10 to 15 miles a week, then build up to 25 to 30 miles a week or more.
5. Use visualization
When you visualize yourself performing an action, an impulse is created in your brain that tells your brain cells (neurons) to carry it out. [ 9 ] So, visualizing can support self-discipline by increasing the likelihood that you’ll take action and do what’s needed to attain your goals.
When people visualize the future, they tend to focus far ahead—on the end goal. Yet visualizing the process is just as important, if not more important. [ 10 ] Visualizing the steps you need to take each day to reach your goal prompts you to act on what you can do to attain your goal in the present.
Set aside 10 minutes each morning to visualize the steps you need to take that day. For the best results, engage all five of your senses as you visualize your day: think about what you can see, hear, touch, taste, and smell. Imagine how you feel as you achieve what you need to.
6. Create a morning ritual
One reason people find it hard to stay disciplined relates to the time it takes to develop a habit. Habits take time to form, and they usually form automatically—not much thought is required to do something you’ve done for weeks, months, or years!
People usually perform rituals or a series of actions when they’re about to engage in a familiar habit. [ 11 ]
For example, if you go swimming at 5 am each morning, you might pack a kit bag and prepare coffee the evening before. These rituals usually develop organically, but you can be intentional about them. Think about a ritual you can try to help you become more disciplined with a new habit or behavior you’re trying to adopt.
7. Do challenging work at your mental best
Doing challenging work requires a lot of mental focus and energy. So, if you want to succeed in being disciplined when it comes to doing challenging work, you should be strategic about when you work.

Depending on your natural sleep and wake cycles, you’ll be more alert at certain times of the day than others. [ 12 ] If you’re a night owl, you’ll probably be more alert later in the day, whereas if you’re an early bird, you’ll probably be at your mental best earlier in the day.
Think about what time of the day you’re most energized. Plan to do your most challenging work then, when you feel mentally strong .
8. Take care of yourself
Self-discipline is easier when you’re taking care of yourself properly. If you’re getting enough sleep, eating a healthy diet, and managing stress with exercise and recreational activities, it will be much easier to stay alert, focused, and engaged when it matters. [ 13 ]
Here are some general self-care guidelines:
- Get enough sleep each night. Healthy adults need at least 7-9 hours of sleep. [ 14 ]
- Exercise regularly. You only need to do 150-300 minutes of moderate exercise per week. [ 15 ] That could look like three 50-minute walks per week.
- Eat a healthy diet containing lots of fresh fruits and vegetables. [ 16 ]
- Make time for activities that bring you joy and help you relax. [ 17 ]
9. Resist temptations
Temptations can act as obstacles when you’re working toward an important goal or trying to make a new habit stick. Research studies have shown that the environment can have a big influence on behavior. [ 18 ]
It’s important that you make your environment as conducive to success as possible by removing anything that could lead you astray. For example, if you’re trying to eat healthily, don’t keep junk food at home. That way, if you’re craving something unhealthy, it won’t even be an option. If you’re racing against time to meet a work deadline and you know you get distracted by your phone, then remove it from your sight. Put it on silent in another room until you’ve completed your work.
10. Find an accountability buddy
It’s harder to be self-disciplined when you only have to be accountable to yourself. If you rely on your own willpower and motivation alone, you may struggle to keep pushing yourself when the going gets tough. [ 19 ]
Tell a friend or family member who you know has your best interests at heart about the goal or habit you’re working toward. Ask them if they’d be willing to hold you accountable and check in with you regularly.
Having someone hold you accountable makes it easier to stay disciplined because it feels like it’s not just you who you’re letting down if you don’t do as you say. It forces you to take responsibility. [ 20 ]
11. Limit all-or-nothing thinking
Thinking in an all-or-nothing way is where you judge yourself or your behavior negatively because of a minor mishap. [ 21 ]
For example, say you’re trying to give up smoking, and you usually smoke ten cigarettes a day. You would be thinking in all-or-nothing terms if, on your first day of quitting, you caved and had one cigarette and started telling yourself you’re a failure.
Thinking in all-or-nothing terms is unhealthy because it discourages you, makes you feel bad about yourself, and can cause you to lose motivation. Instead of thinking in a narrow way when things go wrong, try to see things from a wider and more positive perspective . Failing means that you tried! Pat yourself on the back for trying, and remember that you can start afresh tomorrow.
The benefits of being self-disciplined
If you’re looking for reasons to start training your self-discipline, then you can begin by looking at the benefits of being self-disciplined. You can gain many positive life changes from practicing self-discipline. Here are 5 strong benefits of self-discipline.
1. The achievement of long-term goals
Motivation and willpower can only take you so far when it comes to habit formation and goal accomplishment. [ 19 ] While good to have, some research suggests that we may experience less or more willpower from one day to the next. [ 22 ] Self-discipline, on the other hand, is less about how you feel and more about how you act. And consistent action counts more than feelings or mindset for achievement. In the words of psychologist Angela Duckworth, “Achievement of difficult goals entails the sustained and focused application of talent over time.” [ 23 ]
2. Reduced stress and anxiety
A lack of self-discipline can lead to procrastination and an inability to reach important goals. These behaviors have consequences of their own.
If you tend to procrastinate, you may find yourself constantly working under pressure and struggling to meet deadlines. If you’re unable to reach important goals, it can cause stress and anxiety about the future and chip away at your self-esteem . [ 24 ]
If you can learn self-discipline, you’ll find that you’re less stressed and anxious because you’re living up to your expectations and doing what you set out to do. This will boost positive emotions and make you feel good about yourself.
3. Increased self-worth and happiness
Self-discipline enhances self-worth because when you achieve the goals you set for yourself, you build belief and confidence in yourself . [ 25 ] Self-discipline increases happiness , too.
Studies show that the more productive people are, the happier they feel. [ 25 ] [ 26 ]
4. Better relationships and interpersonal skills
Learning self-discipline is great for relationships, too. A self-disciplined person is better able to manage their emotions intelligently . Being able to pause and reflect before acting on how you feel is an important interpersonal skill. It helps you handle conflict effectively without becoming defensive or exploding and lashing out in anger. [ 27 ]
5. Improved physical health
If you’re self-disciplined, you’ll be better able to resist urges to engage in unhealthy behaviors like overeating, excessive drinking, and smoking. [ 28 ] You’ll also be better able to commit to making behavioral changes that promote good health, such as exercising regularly and maintaining a healthy diet and lifestyle. [ 29 ]
7 self-discipline quotes to inspire you
If you’re looking for some motivation and encouragement in your journey toward better self-discipline, you may find the following quotes helpful:
- “I think self-discipline is something, it’s like a muscle. The more you exercise it, the stronger it gets.” —Daniel Goldstein
- “In reading the lives of great men, I found that the first victory they won was over themselves…self-discipline with all of them came first.” —Harry S Truman
- “Respect your efforts, respect yourself. Self-respect leads to self-discipline. When you have both firmly under your belt, that’s real power.” —Clint Eastwood
- “It’s a lot more than mind over matter. It takes relentless self-discipline to schedule suffering into your day, every day.” ―David Goggins
- “Self-discipline is often disguised as short-term pain, which often leads to long-term gains. The mistake many of us make is the need and want for short-term gains (immediate gratification), which often leads to long-term pain.”―Charles F. Glassman
- “Discipline is the bridge between goals and accomplishment.” —Jim Rohn
- “We must all suffer one of two things: the pain of discipline or the pain of regret & disappointment.” —Jim Rohn
Self-discipline reading list
Since so many people struggle with self-discipline and want to learn how to cultivate it, several self-help books have been written on the topic. Here are 4 of the best-selling books that can teach you how to be more self-disciplined:
- No Excuses!: The Power Of Self Discipline by Brian Tracy
- Atomic Habits: An Easy and Proven Way to Build Good Habits and Break Bad Ones by James Clear
- The Little Book of Big Change: The No Willpower Approach to Breaking Any Habit by Amy Johnson
- The 7 Habits of Highly Effective People by Stephen Covey
- Kalkstein, D. A., & Fujita, K. (2020). Temptation. In K. Sweeny, M.L. Robbins, & Lee M. Cohen (Eds.), The Wiley encyclopedia of health psychology (pp.733-40). Wiley-Blackwell.
- Galla, B. M., & Duckworth, A. L. (2015). More than resisting temptation: Beneficial habits mediate the relationship between self-control and positive life outcomes. Journal of Personality and Social Psychology , 109 (3), 508–525. https://doi.org/10.1037/pspp0000026
- Collins Dictionary. (2019, December 31). Definition of self-discipline. https://www.collinsdictionary.com/dictionary/english/self-discipline
- Taylor, A. F., Kuo, F. E., & Sullivan, W. C. (2002). Views Of Nature and Self-Discipline: Evidence from Inner City Children. Journal of Environmental Psychology , 22 (1-2), 49–63. https://doi.org/10.1006/jevp.2001.0241
- Tao, T., Wang, L., Fan, C., & Gao, W. (2014). Development of self-control in children aged 3 to 9 years: Perspective from a dual-systems model. Scientific Reports , 4 (1). https://doi.org/10.1038/srep07272
- Doran, G. T. (1981, November). There’s a S.M.A.R.T. way to write management’s goals and objectives . https://community.mis.temple.edu/mis0855002fall2015/files/2015/10/S.M.A.R.T-Way-Management-Review.pdf
- Milyavskaya, M., Nadolny, D., & Koestner, R. (2014). Where Do Self-Concordant Goals Come From? The Role of Domain-Specific Psychological Need Satisfaction. Personality and Social Psychology Bulletin , 40 (6), 700–711. https://doi.org/10.1177/0146167214524445
- Harkin, B., Webb, T. L., Chang, B. P. I., Prestwich, A., Conner, M., Kellar, I., Benn, Y., & Sheeran, P. (2016). Does monitoring goal progress promote goal attainment? A meta-analysis of the experimental evidence. Psychological Bulletin, 142 (2), 198–229. https://doi.org/10.1037/bul0000025
- Alavi, A. (2016, November 15). The power of visualization . The Optometry Center for Vision Therapy. https://ocvt.info/the-power-of-visualization
- Taylor, S. E., Pham, L. B., Rivkin, I. D., & Armor, D. A. (1998). Harnessing the Imagination. Mental simulation, self-regulation, and coping. The American Psychologist , 53 (4), 429–439. https://doi.org/10.1037//0003-066x.53.4.429
- Razzetti, G. (2020, February 11). The Power of Rituals: How to Build Meaningful Habits. https://www.fearlessculture.design/blog-posts/the-power-of-rituals-how-to-build-meaningful-habits
- Facer-Childs, E. R., Boiling, S., & Balanos, G. M. (2018). The effects of time of day and chronotype on cognitive and physical performance in healthy volunteers. Sports Medicine – Open , 4 (47). https://doi.org/10.1186/s40798-018-0162-z
- Bui, T., Zackula, R., Dugan, K., & Ablah, E. (2021). Workplace Stress and Productivity: A Cross-Sectional Study. Kansas Journal of Medicine , 14 . https://doi.org/10.17161/kjm.vol1413424
- Suni, E. (2020, July 31). How Much Sleep Do We Really Need? Sleep Foundation. https://www.sleepfoundation.org/how-sleep-works/how-much-sleep-do-we-really-need
- U.S. Department of Health and Human Services. (2018). Physical Activity Guidelines for Americans 2nd edition . https://health.gov/sites/default/files/2019-09/Physical_Activity_Guidelines_2nd_edition.pdf
- Lee, S. H. (2022). Adults Meeting Fruit and Vegetable Intake Recommendations— United States, 2019. MMWR. Morbidity and Mortality Weekly Report , 71 . https://doi.org/10.15585/mmwr.mm7101a1
- Australian Government Department of Health. (2019, July 11). Purposeful activity—Hobbies . https://www.headtohealth.gov.au/meaningful-life/purposeful-activity/hobbies
- Laverl Z. Williamson, Benjamin M. Wilkowski. Nipping Temptation in the Bud: Examining Strategic Self-Control in Daily Life. Personality and Social Psychology Bulletin , 2019 http://dx.doi.org/10.1177/0146167219883606
- Duckworth, A. L., Milkman, K. L., & Laibson, D. (2018). Beyond willpower: Strategies for reducing failures of self-control. Psychological Science in the Public Interest , 19 (3), 102–129. https://doi.org/10.1177/1529100618821893
- Matthews, G. (2007). The impact of commitment, accountability, and written goals on goal achievement. Psychology Faculty Presentations . https://scholar.dominican.edu/psychology-faculty-conference-presentations/3
- Carucci, A. (2022, August 22). All-or-nothing thinking: Examples, effects, and how to manage . https://psychcentral.com/health/all-or-nothing-thinking-examples
- APA (2021). Is willpower a limited resource? https://www.apa.org/topics/willpower-limited.pdf
- Duc kworth, A. L., Peterson, C., Matthews, M. D., & Kelly, D. R. (2007). Grit: Perseverance and passion for long-term goals. Journal of Personality and Social Psychology , 92 (6), 1087–1101. https://doi.org/10.1037/0022-3514.92.6.1087
- Höpfner, J., & Keith, N. (2021). Goal missed, self hit: Goal-setting, goal-failure, and their affective, motivational, and behavioral consequences. Frontiers in Psychology , 12 . https://doi.org/10.3389/fpsyg.2021.704790
- Locke, E. A., & Latham, G. P. (2006). New directions in goal-setting theory. Current Directions in Psychological Science, 15 (5), 265-268. https://doi.org/10.1111/j.1467-8721.2006.00449.x
- Tóth, Á., Wisse, B., & Faragó, K. (2018). The impact of goal attainment and goal importance on satisfaction with life—a polynomial regression and response surface analysis. Mentálhigiéné És Pszichoszomatika , 19 (1), 80–101. https://doi.org/10.1556/0406.19.2018.004
- Mao, T., Pan, W., Zhu, Y., Yang, J., Dong, Q., & Zhou, G. (2018). Self-control mediates the relationship between personality traits and impulsivity. Personality and Individual Differences , 129 , 70–75. https://doi.org/10.1016/j.paid.2018.03.013
- Friese, M., & Hofmann, W. (2009). Control me or I will control you: Impulses, trait self-control, and the guidance of behavior. Journal of Research in Personality , 43 (5), 795–805. https://doi.org/10.1016/j.jrp.2009.07.004
- Hagger, M. S., Gucciardi, D. F., Turrell, A. S., & Hamilton, K. (2019). Self-control and health-related behaviour: The role of implicit self-control, trait self-control, and lay beliefs in self-control. British Journal of Health Psychology . https://doi.org/10.1111/bjhp.12378
Kirsty Britz has a Master’s degree in Psychology from the University of New York in Prague, Training in Person-Centered Counselling, and a Career Coaching Certification. Read more .

Should you acknowledge your weaknesses and flaws?

How to deal with hate comments and criticism
Leave a comment cancel reply.
Notify me when someone responds to my comment.
What statement best describes you?
How motivated are you to find like-minded friends, do you agree with this statement “i want to be more likable”, do you agree with this statement “i want to be more interesting to talk to”, do you agree with this statement “i want to be less awkward”, what best describes you, responses successfully analyzed, where should we send your personalized tips.
24/7 writing help on your phone
To install StudyMoose App tap and then “Add to Home Screen”
Preventing Obesity: Simple Steps for a Healthy Lifestyle
Save to my list
Remove from my list

- On the subjective acceptance during cardiovascular magnetic resonance imaging at 7.0 Tesla
- Weight loss
- Obesity and overweight
Preventing Obesity: Simple Steps for a Healthy Lifestyle. (2016, Dec 28). Retrieved from https://studymoose.com/how-to-prevent-obesity-essay
"Preventing Obesity: Simple Steps for a Healthy Lifestyle." StudyMoose , 28 Dec 2016, https://studymoose.com/how-to-prevent-obesity-essay
StudyMoose. (2016). Preventing Obesity: Simple Steps for a Healthy Lifestyle . [Online]. Available at: https://studymoose.com/how-to-prevent-obesity-essay [Accessed: 27 Jul. 2024]
"Preventing Obesity: Simple Steps for a Healthy Lifestyle." StudyMoose, Dec 28, 2016. Accessed July 27, 2024. https://studymoose.com/how-to-prevent-obesity-essay
"Preventing Obesity: Simple Steps for a Healthy Lifestyle," StudyMoose , 28-Dec-2016. [Online]. Available: https://studymoose.com/how-to-prevent-obesity-essay. [Accessed: 27-Jul-2024]
StudyMoose. (2016). Preventing Obesity: Simple Steps for a Healthy Lifestyle . [Online]. Available at: https://studymoose.com/how-to-prevent-obesity-essay [Accessed: 27-Jul-2024]
- An Analysis of Walking in Simple Exercises for Maintaining a Healthy Lifestyle Pages: 2 (355 words)
- The Importance of Healthy Behaviors to a Healthy Lifestyle Pages: 4 (956 words)
- Preventing Childhood Obesity in Argentina: Nutrition for Health and Social Care Pages: 2 (575 words)
- The Simple Answer to the Problems of Obesity in America Pages: 6 (1523 words)
- Obesity As An Unhealthy Lifestyle And Not A Disease Pages: 7 (2059 words)
- Stress Management Is Important to a Healthy Lifestyle Pages: 2 (429 words)
- The Benefits Of a Healthy Lifestyle and Clean Eating Pages: 7 (2098 words)
- Ways on Living a Happy Healthy Lifestyle Pages: 2 (448 words)
- Dialogue "Healthy Lifestyle" Pages: 5 (1288 words)
- The Importance of Healthy Lifestyle Pages: 5 (1401 words)

👋 Hi! I’m your smart assistant Amy!
Don’t know where to start? Type your requirements and I’ll connect you to an academic expert within 3 minutes.

IMAGES
VIDEO
COMMENTS
Discipline - or the lack of it - is something that is sometimes offered up as an explanation for obesity. Public health professionals, employers, and physicians gathered at a medical forum in Baltimore last week to discuss obesity and how health plans can address this growing health concern. One physician who is medical director for a large ...
Besides health complications, obesity causes an array of psychological effects, including inferiority complex among victims. Obese people suffer from depression, emanating from negative self-esteem and societal rejection. In some cases, people who become obese lose their friends and may get disapproval from teachers and other personalities ...
Intermittent fasting (IF) has become an increasingly popular approach to treating obesity. Its proponents argue that the strategy is more effective in addressing weight loss than traditional daily caloric intake reduction (Halpern & Mendes, 2021). The IF advocates claim that high insulin levels in the organism associated with high carbohydrate ...
Obesity and BMI (body mass index) are both tools of measurement that are used by doctors to assess body fat according to the height, age, and gender of a person. If the BMI is between 25 to 29.9, that means the person has excess weight and body fat. If the BMI exceeds 30, that means the person is obese. Obesity is a condition that increases the ...
Self Discipline Benefits and Importance. Self-discipline helps you to overcome the bad habits by meditating regularly. It gives you the ability not to give up after failure and setbacks, develop self-control, provide the ability to resist distractions, helps you to motivate yourself until you accomplish your goals. Conclusion.
This prevalence has tripled since the 1970s. Childhood obesity is associated with several negative health consequences, including diabetes, heart disease, and high blood pressure, as well as emotional and psychological impacts, such as low self-esteem and bullying. This essay will explore the causes of child obesity, its effects, and possible ...
Obesity in childhood can have significant long-term effects on a child's physical health, increasing the risk of developing chronic conditions such as type 2 diabetes, heart disease, and hypertension. Furthermore, obesity can have a profound impact on a child's psychological well-being, leading to low self-esteem, depression, and social isolation.
Essay on obesity! Find high quality essays on 'Obesity' especially written for school, college, science and medical students. These essays will also guide you to learn about the causes, factors, treatment, management and complications related to obesity. Obesity is a chronic health condition in which the body fat reaches abnormal level.
Discipline is the invisible glue that binds our actions toward achieving our goals. It is not just about obeying rules or following a regimented routine; it is the ability to control our behavior and actions for personal improvement and societal good. This discipline essay aims to elaborate on this central theme.
Conclusion: In conclusion, the consequences of obesity are far-reaching and demand urgent attention. From the individual health implications to the societal and economic burdens, the impact of this epidemic cannot be ignored. However, by understanding the root causes, implementing prevention strategies, and advocating for policy changes, we can ...
Why Self-Discipline is Important - Reason #11: Self-Discipline Can Help You Find Your Sense of Purpose. As you build self-discipline, you will start making progress towards your goals. And as you progress, some of those goals may send you in a direction you couldn't have even imagined your life would go in.
Self-discipline, an essential characteristic for personal and professional success, is the ability to control one's feelings and overcome weaknesses. It involves acting according to what you think instead of how you feel in the moment. It's a sign of inner strength and control of oneself and one's actions.
There are many causes for obesity in the world such as having an inactive lifestyle or consuming too much processed food. On the contrary, there are many solutions on how to overcome this problem for people such as having motivation and discipline, a well - balanced diet and also exercising. Firstly, exercise is one of the main focuses for ...
Importance of Self Discipline Essay: Self-Discipline means having control over oneself; it provides self-control overreactions, actions, and oneself and boosts a person's inner strength. Self- Discipline is the most important skill a person should possess. One of the main attributes of Self-Discipline is its ability to abdicate immediate pleasure and gratification. Self-Discipline does not ...
Previously, obesity was considered a sign of overweight which means looking bad but now it is a disease which brings lot of medical complication that can become a life threat. This complication can be overcome by proper dieting, exercise and self-discipline. There is a notion that obesity is only related to your weight.
16. The Power of Self-Discipline. In 2021 Peter Hollins published The Power of Self-Discipline. And while it's not one of the most popular books on discipline, it is one of the most effective. Why? Because it helps you get right to the heart of what deteriorates discipline, and it provides tangible methods to overcome those things.
Importance of Self Discipline. Self-discipline is a crucial attribute that enables individuals to achieve personal and professional goals. It involves the ability to control one's emotions, behaviors, and desires in the face of external demands, to stay focused and productive. Self-discipline is not just about self-control but also about ...
Set yourself up for success by ditching bad influences. STEP THREE: Set clear goals and have an execution plan. If you hope to achieve greater degrees of self-discipline, you must have a clear ...
Childhood obesity is a rapidly developing problem on a global scale. In the years of 2017-2020, 19.7% of children and adolescents were affected by obesity, which accounts for 14.7 million children [].Obesity rates are especially high among Hispanic children (26.2%) and non-Hispanic Black children (24.8%) [].If obesity continues to expand at this rate, 9% of all preschoolers will develop ...
Obesity in adults may cause problems such as: heart disease, type 2 diabetes, stroke, several types of cancer, and osteoarthritis. One study exposed that children as early as age two were likely to be obese adults. Obesity can also lead to some very serious cancers including cancer of the breast, colon, endometrium, esophagus, kidney, pancreas ...
8. Take care of yourself. Self-discipline is easier when you're taking care of yourself properly. If you're getting enough sleep, eating a healthy diet, and managing stress with exercise and recreational activities, it will be much easier to stay alert, focused, and engaged when it matters.
Obesity not only affect adults, but it also affects children as well. In order to overcome obesity, one must go through rigorous diet and exercise. Obesity swells a person when their calories intake (food) is more than their output (exercise of some sort) to burn off the calories.…. 1085 Words.
31618. We must stay active. This is an important step in preventing obesity. Join a gym or yoga class to stay slim and trim. Take the stairs or walk to do your chores. Simple steps like these can go a long way in preventing overweight and obesity. Joining a gym or yoga class will help you mingle with like-minded people who can give you valuable ...